
- •Contents
- •Preface
- •Contributors
- •1 Vessels
- •1.1 Aorta, Vena Cava, and Peripheral Vessels
- •Aorta, Arteries
- •Anomalies and Variant Positions
- •Dilatation
- •Stenosis
- •Wall Thickening
- •Intraluminal Mass
- •Perivascular Mass
- •Vena Cava, Veins
- •Anomalies
- •Dilatation
- •Intraluminal Mass
- •Compression, Infiltration
- •1.2 Portal Vein and Its Tributaries
- •Enlarged Lumen Diameter
- •Portal Hypertension
- •Intraluminal Mass
- •Thrombosis
- •Tumor
- •2 Liver
- •Enlarged Liver
- •Small Liver
- •Homogeneous Hypoechoic Texture
- •Homogeneous Hyperechoic Texture
- •Regionally Inhomogeneous Texture
- •Diffuse Inhomogeneous Texture
- •Anechoic Masses
- •Hypoechoic Masses
- •Isoechoic Masses
- •Hyperechoic Masses
- •Echogenic Masses
- •Irregular Masses
- •Differential Diagnosis of Focal Lesions
- •Diagnostic Methods
- •Suspected Diagnosis
- •3 Biliary Tree and Gallbladder
- •3.1 Biliary Tree
- •Thickening of the Bile Duct Wall
- •Localized and Diffuse
- •Bile Duct Rarefaction
- •Localized and Diffuse
- •Bile Duct Dilatation and Intraductal Pressure
- •Intrahepatic
- •Hilar and Prepancreatic
- •Intrapancreatic
- •Papillary
- •Abnormal Intraluminal Bile Duct Findings
- •Foreign Body
- •The Seven Most Important Questions
- •3.2 Gallbladder
- •Changes in Size
- •Large Gallbladder
- •Small/Missing Gallbladder
- •Wall Changes
- •General Hypoechogenicity
- •General Hyperechogenicity
- •General Tumor
- •Focal Tumor
- •Intraluminal Changes
- •Hyperechoic
- •Hypoechoic
- •Nonvisualized Gallbladder
- •Missing Gallbladder
- •Obscured Gallbladder
- •4 Pancreas
- •Diffuse Pancreatic Change
- •Large Pancreas
- •Small Pancreas
- •Hypoechoic Texture
- •Hyperechoic Texture
- •Focal Changes
- •Anechoic Lesion
- •Hypoechoic Lesion
- •Isoechoic Lesion
- •Hyperechoic Lesion
- •Irregular (Complex Structured) Lesion
- •Dilatation of the Pancreatic Duct
- •Marginal/Mild Dilatation
- •Marked Dilatation
- •5 Spleen
- •Nonfocal Changes of the Spleen
- •Diffuse Parenchymal Changes
- •Large Spleen
- •Small Spleen
- •Focal Changes of the Spleen
- •Anechoic Mass
- •Hypoechoic Mass
- •Hyperechoic Mass
- •Splenic Calcification
- •6 Lymph Nodes
- •Peripheral Lymph Nodes
- •Head/Neck
- •Extremities (Axilla, Groin)
- •Abdominal Lymph Nodes
- •Porta Hepatis
- •Splenic Hilum
- •Mesentery (Celiac, Upper and Lower Mesenteric Station)
- •Stomach
- •Focal Wall Changes
- •Extended Wall Changes
- •Dilated Lumen
- •Narrowed Lumen
- •Small/Large Intestine
- •Focal Wall Changes
- •Extended Wall Changes
- •Dilated Lumen
- •Narrowed Lumen
- •8 Peritoneal Cavity
- •Anechoic Structure
- •Hypoechoic Structure
- •Hyperechoic Structure
- •Anechoic Structure
- •Hypoechoic Structure
- •Hyperechoic Structure
- •Wall Structures
- •Smooth Margin
- •Irregular Margin
- •Intragastric Processes
- •Intraintestinal Processes
- •9 Kidneys
- •Anomalies, Malformations
- •Aplasia, Hypoplasia
- •Cystic Malformation
- •Anomalies of Number, Position, or Rotation
- •Fusion Anomaly
- •Anomalies of the Renal Calices
- •Vascular Anomaly
- •Diffuse Changes
- •Large Kidneys
- •Small Kidneys
- •Hypoechoic Structure
- •Hyperechoic Structure
- •Irregular Structure
- •Circumscribed Changes
- •Anechoic Structure
- •Hypoechoic or Isoechoic Structure
- •Complex Structure
- •Hyperechoic Structure
- •10 Adrenal Glands
- •Enlargement
- •Anechoic Structure
- •Hypoechoic Structure
- •Complex Echo Structure
- •Hyperechoic Structure
- •11 Urinary Tract
- •Malformations
- •Duplication Anomalies
- •Dilatations and Stenoses
- •Dilated Renal Pelvis and Ureter
- •Anechoic
- •Hypoechoic
- •Hypoechoic
- •Hyperechoic
- •Large Bladder
- •Small Bladder
- •Altered Bladder Shape
- •Intracavitary Mass
- •Hypoechoic
- •Hyperechoic
- •Echogenic
- •Wall Changes
- •Diffuse Wall Thickening
- •Circumscribed Wall Thickening
- •Concavities and Convexities
- •12.1 The Prostate
- •Enlarged Prostate
- •Regular
- •Irregular
- •Small Prostate
- •Regular
- •Echogenic
- •Circumscribed Lesion
- •Anechoic
- •Hypoechoic
- •Echogenic
- •12.2 Seminal Vesicles
- •Diffuse Change
- •Hypoechoic
- •Circumscribed Change
- •Anechoic
- •Echogenic
- •Irregular
- •12.3 Testis, Epididymis
- •Diffuse Change
- •Enlargement
- •Decreased Size
- •Circumscribed Lesion
- •Anechoic or Hypoechoic
- •Irregular/Echogenic
- •Epididymal Lesion
- •Anechoic
- •Hypoechoic
- •Intrascrotal Mass
- •Anechoic or Hypoechoic
- •Echogenic
- •13 Female Genital Tract
- •Masses
- •Abnormalities of Size or Shape
- •Uterus
- •Abnormalities of Size or Shape
- •Myometrial Changes
- •Intracavitary Changes
- •Endometrial Changes
- •Fallopian Tubes
- •Hypoechoic Mass
- •Anechoic Cystic Mass
- •Solid Echogenic or Nonhomogeneous Mass
- •14 Thyroid Gland
- •Diffuse Changes
- •Enlarged Thyroid Gland
- •Small Thyroid Gland
- •Hypoechoic Structure
- •Hyperechoic Structure
- •Circumscribed Changes
- •Anechoic
- •Hypoechoic
- •Isoechoic
- •Hyperechoic
- •Irregular
- •Differential Diagnosis of Hyperthyroidism
- •Types of Autonomy
- •15 Pleura and Chest Wall
- •Chest Wall
- •Masses
- •Parietal Pleura
- •Nodular Masses
- •Diffuse Pleural Thickening
- •Pleural Effusion
- •Anechoic Effusion
- •Echogenic Effusion
- •Complex Effusion
- •16 Lung
- •Masses
- •Anechoic Masses
- •Hypoechoic Masses
- •Complex Masses
- •Index
Kidneys |
Anomalies, Malformations |
|
Horseshoe Kidney |
|||
|
|
|
|
|||
|
|
|
|
Aplasia, Hypoplasia |
|
Fetal Lobulation |
|
|
|
|
Cystic Malformation |
|
|
|
|
|
|
Anomalies of Number, |
|
|
|
|
|
|
Position, or Rotation |
|
|
|
|
|
|
Fusion Anomaly |
|
|
|
|
|
|
|
|
|
|
|
|
|
Anomalies of the Renal Calices |
|
|
|
|
|
|
Vascular Anomaly |
|
|
|
|
|
Diffuse Changes |
|
|
|
|
|
|
|
|
||
|
|
|
Circumscribed Changes |
|
|
|
|
|
|
|
|
||
Horseshoe Kidney
Kidney

















In the most common fusion anomaly, the symmetrical horseshoe kidney, the lower poles of the kidneys are fused together across the midline. Horseshoe kidney has an incidence of 1:425 in the general population. The descriptive term is best understood in the excretory urogram, where an AP view displays the typical horseshoe pattern (Fig. 9.16).
It is not unusual for horseshoe kidney to be missed in ultrasound, as the scan planes may not completely define the inferior outline of the lower pole. A “never-ending” lower pole should always raise suspicion of this anomaly. Ultrasound may occasionally suggest a misdiagnosis of preaortic lymphoma unless horseshoe kidney is considered in the differential diagnosis. The apparent “tumor mass” in these
cases is the isthmus joining the two lower poles, which may consist of renal parenchyma or a fibrous band (Fig. 9.17). Color Doppler ultrasound usually establishes the diagnosis by demonstrating the typical vascular configuration.
Incomplete horseshoe kidney is diagnosed when ultrasound shows the typical medial extension of the lower pole, often crossing the aorta, but the contralateral kidney is absent. Morphologically, this results in an elongated L-shaped or sigmoid kidney. Fusion of the upper and lower poles results in a ring-shaped kidney. A cake-shaped kidney results when the fusion occurs over broader areas, producing an irregularly shaped organ. Combinations with polycystic kidney disease are also possible.
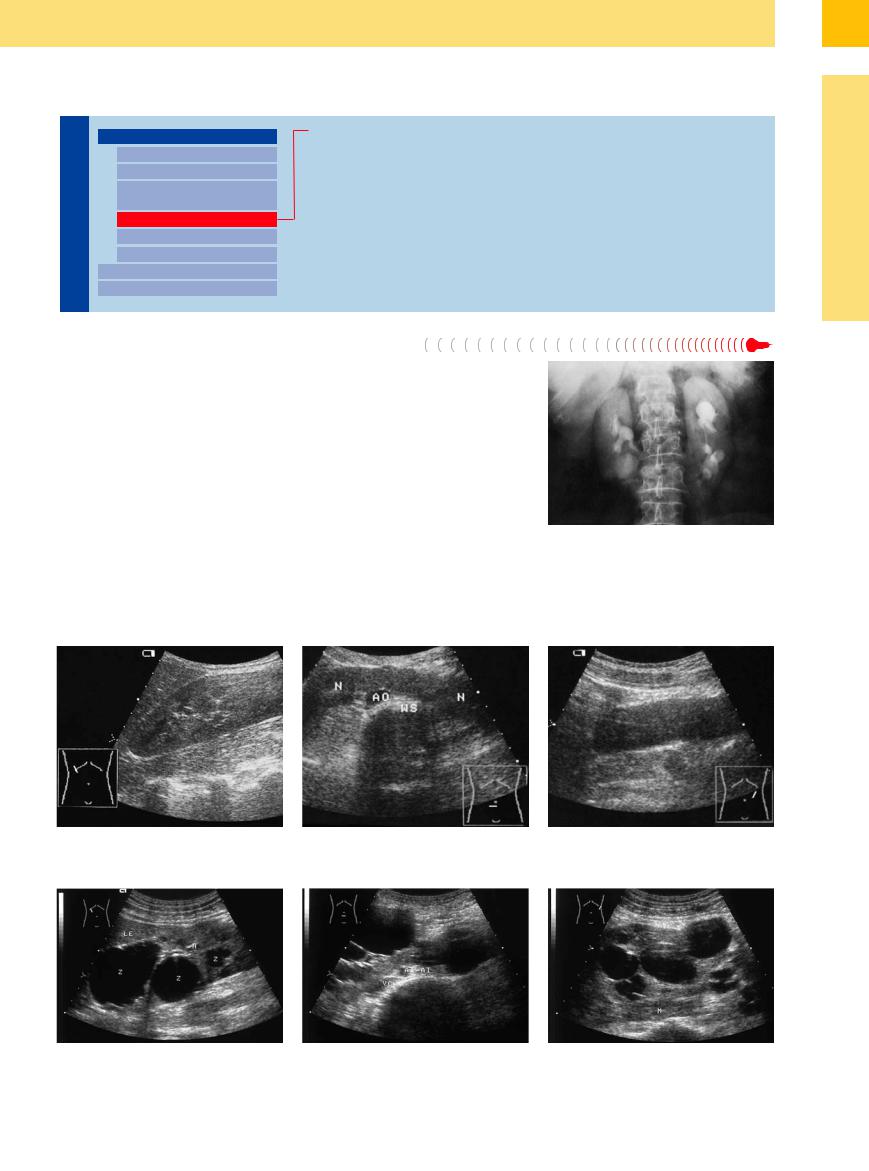
Fig. 9.16 Radiograph of a horseshoe kidney. The horseshoe shape of the kidney is appreciated in this AP view following intravenous contrast administration.
9
Anomalies, Malformations
Fig. 9.17 Horseshoe kidney. |
b and c The renal parenchyma (N) continues to the left across the aorta (AO) and spinal column (WS). |
a Right kidney with an unbounded lower pole. |
|
d–f Horseshoe kidney combined with polycystic kidney disease in a 50-year-old man.
327

9
Kidneys
Fetal Lobulation



















































As a developmental disturbance, fetal lobulation presents as an incomplete fusion of fetal nephrons (see Fig. 9.66).
Anomalies of the Renal Calices
Kidneys

Anomalies, Malformations
Aplasia, Hypoplasia
Cystic Malformation
Anomalies of Number, Position, or Rotation
Fusion Anomaly
Anomalies of the Renal Calices Vascular Anomaly
Diffuse Changes Circumscribed Changes
Caliceal Diverticulum
Megacalicosis
Caliceal Diverticulum
















































Caliceal diverticula are epithelialized protru- |
ferentiation from caliectasis due to obstructing |
sions of caliceal tissue that often contain crys- |
caliceal stones, which are more common in |
talline precipitate and stones as a result of flow |
older patients. |
stasis (see Fig.11.10, p. 384). They require dif- |
|
Megacalicosis 




















































This is a congenital dilatation of the calices, which is usually asymptomatic.
Vascular Anomaly
Kidneys

Anomalies, Malformations
Aplasia, Hypoplasia
Cystic Malformation
Anomalies of Number, Position, or Rotation
Fusion Anomaly
Anomalies of the Renal Calices Vascular Anomaly
Diffuse Changes Circumscribed Changes
Aberrant Vessels
Renovascular Malformations
Aberrant Vessels
Vessels
A crossing interlobar artery will occasionally narrow the neck of the calix, causing prestenotic dilatation of the upper calix. Ultrasound then shows an abnormal expansion of the affected calix with no visible outflow obstruction (stone).
A more common aberrant configuration is a lower pole artery arising separately from the aorta and narrowing the upper ureter, causing pyelectasis. Ultrasound shows an anechoic mass in the pyelocaliceal system obstructing the proximal ureter but does not demonstrate
a causative lesion (tumor, stone). This anomaly should always be suspected in cases of this kind (see Fig.11.11, p. 385). The differential diagnosis should also include pyelectasis due to an ampullary renal pelvis and a hypermobile kidney with proximal kinking of the ureter.
328
