
Ghai Essential Pediatrics8th
.pdf
Eighth
Edition

Contents
|
Preface to the Eighth Edition |
vii |
7. |
Micronutrients in |
|
|
|
Preface to the First Edition |
ix |
|
Health and Disease |
110 |
|
|
List of Contributors |
xi |
|
Ashima Gulati, Arvind Bagga |
|
|
|
|
|
|
|
Fat soluble vitamins 110 |
|
1. |
Introduction to Pediatrics |
|
|
Water soluble vitamins 117 |
|
|
|
Vinod KPaul |
|
|
|
Minerals and trace elements 121 |
|
|
|
|
|
|
|
|
|
Pediatrics as a specialty |
|
|
|
|
|
|
Health system in India 2 |
|
8. |
Newborn Infants |
124 |
|
|
National programs on child health 3 |
|
|
Ramesh Agarwal, Vinod KPaul, Ashok K Deorari |
||
|
|
|
|
|
||
|
|
|
|
|
Resuscitation of a newborn 125 |
|
2. |
Normal Growth and its Disorders |
7 |
|
Routine care 133 |
|
|
|
Thermal protection 143 |
|
||||
|
|
|
|
|
|
|
|
Ramesh Agarwal, Naveen Sankhyan, Vandana Jain |
|
Fluid and electrolyte management 146 |
|||
|
Somatic growth 11 |
|
|
|
Kangaroo mother care 148 |
|
|
Assessment of physical growth 11 |
|
|
Breastfeeding 150 |
|
|
|
Disorders of growth 35 |
|
|
Care of low birth weight babies |
155 |
|
|
Abnormalities of head size and shape 39 |
|
|
Infections in the neonates 162 |
|
|
3. Development |
|
|
|
Perinatal asphyxia 166 |
|
|
|
42 |
|
Respiratory distress 168 |
|
||
|
Ramesh Agarwal, Vandana Jain, Naveen Sankhyan |
|
Jaundice 172 |
|
||
|
Normal development |
42 |
|
|
Congenital malformations 176 |
|
|
|
|
Followup of high risk neonates |
178 |
||
|
Behavioral disorders |
57 |
|
|
||
|
|
|
Metabolic disorders 179 |
|
||
|
Habit disorders and tics 59 |
|
|
|
||
|
|
|
|
|
Effect of maternal conditions on fetus and neonates 181 |
|
4. Adolescent Health and |
|
|
|
|
||
|
Development |
|
63 |
9. Immunization and Immunodeficiency |
||
Tushar R Godbole.Vijayalakshmi Bhatia
Physical aspects 63
Cognitive and social development 63
Problems faced by adolescents 65
Role of health care provider 67
5. Fluid and Electrolyte Disturbances 70
Kamran Afzal
Composition of body fluids 70 Deficit therapy 72
Sodium 73
Potassium 76
Calcium 79 Magnesium 82 Acid-base disorders 83
6. Nutrition |
88 |
Vinod KPaul, Rakesh Lodha, Anuja Agarwala |
|
Macronutrients 88 |
|
Normal diet 90 |
|
Undernutrition 95 |
|
Management of malnutrition |
l00 |
184
Aditi Sinha, Surjit Singh
Immunity 184
Primary immunodeficiency disorders 185 Immunization 188
Commonly used vaccines 190 Vaccine administration 203 Immunization programs 205
Immunization in special circumstances 206
10. Infections and Infestations |
209 |
Tanu Singha!, Rakesh Lodha, SK Kabra |
|
Fever 209 |
|
Common viral infections 213 |
|
Viral hepatitis 220 |
|
Human immunodeficiency virus (HIV) |
229 |
Common bacterial infections 240
Tuberculosis 250
Fungal infections 259
Protozoa! infections 260
Congenital and perinatal infections 272
Helminthic infestations 273

-....E s s e n t ail P e d ait rics _________________________________
_ _ _ _ _ _ _ _ _ _ _ _ _ _ _
11.Diseases of Gastrointestinal System and Liver
Anshu Srivastava, Barath Jagadisan, SK Yachha
Gastrointestinal disorders 278 Acute diarrhea 291 Persistent diarrhea 297 Chronic diarrhea 299 Gastrointestinal bleeding 306
Disorders of the hepatobiliary system 309 Acute viral hepatitis 312
Liver failure 313
Chronic liver disease 316
12. Hematological Disorders
Tulika Seth
Anemia 330
Approach to hemolytic anemia 337 Hematopoietic stem cell transplantation 347 Approach to a bleeding child 349 Thrombotic disorders 355
Leukocytosis, leukopenia 357
13. Otolaryngology
Sandeep Samant, Grant T Rohman, Jerome W Thompson
Diseases of the ear 359
Diseases of the nose and sinuses 363 Diseases of the oral cavity and pharynx 366 Diseases of the larynx and trachea 368 Diseases of the salivary glands 370
14. Disorders of Respiratory System
SK Kabra
Common respiratory symptoms 371 Investigations for respiratory illness 373 Respiratory tract infections 374
Acute lower respiratory tract infections 376 Bronchial asthma 382
Foreign body aspiration 391 Lung abscess 391 Bronchiectasis 392
Cystic fibrosis 393
Acute respiratory distress syndrome (ARDS) 393
15.Disorders of Cardiovascular System
R Krishna Kumar, R Tandon, Manu Raj
Congestive cardiac failure 396
Congenital heart disease 400
Acyanotic congenital heart defects 413
Cyanotic heart disease 420
Obstructive lesions 429
Rheumatic fever and rheumatic heart disease 433
278Infective endocarditis 443 Myocardial diseases 447 Pericardia! diseases 450 Systemic hypertension 451
Pulmonary arterial hypertension 456 Rhythm disorders 457
Preventing adult cardiovascular disease 462
16. Disorders of Kidney and |
|
Urinary Tract |
464 |
Arvind Bagga, Aditi Sinha, RN Srivastava
Renal anatomy and physiology 464
330Diagnostic evaluation 467 Acute glomerulonephritis 474 Nephrotic syndrome 477 Chronic glomerulonephritis 483 Urinary tract infections 483 Acute kidney injury 487 Chronic kidney disease 493 Renal replacement therapy 497
Disorders of renal tubular transport 497 Enuresis 504
Congenital abnormalities of kidney and
359 |
urinary tract 505 |
|
|
|
|
|
Cystic kidney diseases |
507 |
|
17. Endocrine and Metabolic |
|
|
Disorders |
510 |
PSN Menon, Anurag Bajpai, Kanika Ghai
Disorders of pituitary gland 511
Disorders of thyroid gland 516
Disorders of calcium metabolism 521
371Disorders of adrenal glands 523 Obesity 528
Disorders of the gonadal hormones 53l Diabetes mellitus 54l
|
18. Central Nervous System |
549 |
|
|
Veena Kalra |
|
|
|
Approach to neurological diagnosis |
549 |
|
|
Seizures 552 |
|
|
|
Febrile convulsions 556 |
|
|
|
Epilepsy 557 |
|
|
|
Coma 561 |
|
|
|
Acute bacterial meningitis 563 |
|
|
|
Tuberculous meningitis 566 |
|
|
|
Encephalitis and encephalopathies |
568 |
|
396 |
lntracranial space occupying lesions |
570 |
|
|
Subdural effusion 573 |
|
|
|
Hydrocephalus 574 |
|
|
|
Neural tube defects 575 |
|
|
|
Acute hemiplegia of childhood |
577 |
|
|
Paraplegia and quadriplegia |
578 |
|
|
Ataxia 579 |
|
|
|
Cerebral palsy 581 |
|
|

___________________________________:c:on.:;t::ent:s. . ....J-
Degenerative brain disorders 583
Mental retardation 584
Neurocutaneous syndromes 586
19. Neuromuscular Disorders
Sheffali Gulati
Approach to evaluation 587
Disorders affecting anterior horn cells 588 Peripheral neuropathies 589
Acute flaccid paralysis 592 Neuromuscular junction disorders 593 Muscle disorders 594
20. Childhood Malignancies
Sadhna Shankar, Rachna Seth
Leukemia 599
Lymphoma 608 Brain tumors 612 Retlnoblastoma 614 Neuroblastoma 616 Wilms tumor 617
Soft tissue sarcoma 618 Bone tumors 619
Malignant tumors of the liver 620 Histiocytoses 620
Oncologic emergencies 622
Hematopoietic stem cell transplantation 623
21. Rheumatological Disorders
Surjit Singh
Arthritis 624
Systemic lupus erythematosus 628 Juvenile dermatomyositis 629 Scleroderma 630
Mixed connective tissue disease 630 Vasculitides 631
24. |
Eye Disorders |
665 |
|
Radhika Tandon |
|
|
Pediatric eye screening |
665 |
|
Congenital and developmental abnormalities 666 |
|
587 |
Acquired eye diseases |
667 |
|
|
|
25. |
Skin Disorders |
672 |
|
Neena Khanna. Seemab Rasool |
|
|
Basic principles 672 |
|
|
Genodermatoses 675 |
|
|
Nevi 679 |
|
|
Eczematous dermatitis |
680 |
Disorders of skin appendages 682
Papulosquamous disorders 684
599Disorders of pigmentation 686 Drug eruptions 686
Infections 687
Diseases caused by arthropods 694
26. |
Poisonings, Injuries and |
|
|||
|
Accidents |
|
|
696 |
|
|
P Ramesh Menon |
|
|
|
|
|
Poisoning 696 |
|
|
|
|
|
Common poisonings 700 |
|
|
||
|
Envenomation 703 |
|
|
|
|
|
Injuries and accidents |
704 |
|
|
|
27. |
Pediatric Critical Care |
708 |
|||
624 |
Rakesh Lodha, Manjunatha Sarthi |
|
|||
Assessment and monitoring of a seriously ill child |
708 |
||||
|
|||||
|
Pediatric basic and advanced life support 71O |
|
|||
|
Shock 715 |
|
|
|
|
|
Mechanical ventilation |
719 |
|
|
|
|
Nutrition in critically ill children |
720 |
|
||
|
Sedation, analgesia and paralysis 721 |
|
|||
|
Nosocomial infections in PICU |
721 |
|
||
|
Transfusions 723 |
|
|
|
|
22. Genetic Disorders
Neerja Gupta, Madhulika Kabra
Chromosomal disorders 636 Single gene disorders 64l Polygenic inheritance 644 Therapy for genetic disorders 644
Prevention of genetic disorders 645
23. Inborn Errors of Metabolism
Neerja Gupta, Madhulika Kabra
Suspecting an inborn error of metabolism 647
Aminoacidopathies 652 Urea cycle defects 653 Organic acidurias 655
Defects of carbohydrate metabolism 655 Mitochondial fatty acid oxidation defects 657 Lysosomal storage disorders 659
635 |
28. Common Medical Procedures |
727 |
|
|
Sidharth Kumar Sethi. Arvind Bagga
|
Obtaining blood specimens |
727 |
|
|||
|
Removal of aspirated foreign body |
727 |
||||
|
Nasogastric tube insertion 728 |
|
||||
|
Venous catheterization |
728 |
|
|
||
|
Capillary blood (hell prick) |
730 |
|
|||
|
Umbilical vessel catheterization 730 |
|
||||
|
Arterial catheterization |
731 |
|
|
||
647 |
lntraosseous Infusion 731 |
|
|
|||
|
|
|
||||
|
Lumbar puncture |
732 |
|
|
|
|
|
Thoracocentesis |
733 |
|
|
|
|
|
Abdominal paracentesis or ascitic tip 734 |
|||||
|
Catheterization of bladder |
734 |
|
|||
|
Peritoneal dialysis |
734 |
|
|
|
|
|
Bone marrow aspiration and biopsy |
736 |
||||
|
Liver biopsy |
737 |
|
|
|
|
|
Renal biopsy |
738 |
|
|
|
|

___E s s en tia iPed i a tr ics________________________________
_ _ _ _ _ _ _ _ _ _ _ _ _ _
29. Rational Drug Therapy |
739 |
Outpatient management of sick child age 2 months
Anu Thukral, Ashok K Deorari |
upto 5 years 758 |
|
Revision in IMNCI guidelines 767 |
||
|
30. Integrated Management of Neonatal
and Childhood Illness |
751 |
AK Patwari, S Aneja
IMNCI strategy 751
Outpatient management of young infants age up to 2 months 752
31. Rights of Children |
768 |
Rajeev Seth |
|
Child abuse and neglect |
769 |
Adoption 770 |
|
Index |
773 |

Introduction to Pediatrics
The branch of medicine that deals with the care of children and adolescents is pediatrics. This term has roots in the Greek word pedo pais (a child) and iatros (healer). Pediatrics covers the age group less than 18 yr of age. A physician who specializes in health care of children and adolescents is a pediatrician. The goal of the specialty is to enable a child to survive, remain healthy, and attain the highest possible potential of growth, development and intellectual achievement. Child health encompasses approaches, interventions and strategies that preserve, protect, promote and restore health of children at individual and population level.
Children under 15 yr of age comprise about 30% of India's population. Childhood is the state when the human being is growing and developing. It is time to acquire habits, values and lifestyles that would make children responsible adults and citizens. The family, society and nation are duty bound to make children feel secure, cared for, and protected from exploitation,violence and societal ills. Female children face gender bias in access to healthcare and nutrition. A civilized society nurtures all its children, girls and boys alike, with love, generosity and benevolence.
Child is not a miniature adult. The principles of adult medicine cannot be directly adapted to children. Pediatric biology is unique and risk factors of pediatric disease are distinct. Clinical manifestations of childhood diseases may be different from adults.Indeed, many disorders are unique to children. Drug dosages in children are specific and not a mathematical derivation of the adult doses. Nutrition is a critical necessity for children not only to sustain life, but to ensure their growth and development.
Pediatrics as a Specialty
Pediatrics is a fascinating specialty. It encompasses care of premature neonates on the one hand, and adolescents, on theother. The discipline of pediatrics has branched into well developed superspecialties (such as neonatology, nephrology, pulmonology, infectious disease, critical care,
Vinod K Paul
neurology, hematooncology, endocrinology and cardiology). Pediatrics covers intensive care of neonates and children using the most sophisticated technology, on the one hand, and providing home care to newborns and children, on the other. Child health is thus a state-of-art clinical science as well as a rich public health discipline.
Medical students should possess competencies for the care of healthy and sick children. The agenda of high child mortality due to pneumonia, neonatal infections, preterm birth complications, diarrhea, birth asphyxia and vaccine preventable diseases is still unfinished. The benefits of advancing pediatric specialties must reach all children. Besides, an increasing body of knowledge on pediatric origins of noncommunicable diseases of the adult is set to change the paradigm of child health. Primary prevention, identification of earlymarkers andtimely treatment of adult disorders are the emerging imperatives in pediatrics.
Historical Perspective
Medical care of children finds place in the ancient Indian, Greek and Chinese systems of health. But as a formal discipline, pediatrics took root in Europe and the US in the 19th century when some of the famous children hospitals were established. BJ Hospital for Children, Mumbai was the first child hospital to be established in India in 1928. Postgraduate diploma in pediatrics was started there in 1944; postgraduate degree programs began in the fifties. Pediatrics became an independent subject in MBBS course in mid-nineties. The first DM program in neonatology started in 1989 at PGIMER, Chandigarh and in pediatric neurology at AIIMS in 2004.
Challenge of High Child Mortality
India has the highest number of child births as well as child deaths for any single nation in the world. Each year, as many as 27 million babies are born in the country. This comprises 20% of the global birth cohort. Of the 7.8 million
1

|
s -------- |
- |
e_s_es__nia tl dP tnciae · -------------- |
||
___ |
----------- |
|
|
|
|
under 5 child deaths in the world in 2010, 1.7 million (23%) occur in our country. The mortality risk is highest in the neonatal period. National programs focus generally on child deaths under the age of 5 yr (under-5 mortality). Table 1.1providesthe most recentfigureson the key child mortality indices.
Table 1.1: Child mortality indices in India
Indices |
Level in 2012 |
Under 5 mortality rate (USMR) |
52 per 1000 live births |
Infant mortality rate (IMR) |
42 per 1000 live births |
Neonatal mortality rate (NMR) |
29 per 1000 live births |
Early neonatal mortality rate (ENMR) |
23 per 1000 live births |
USMR Number of deaths under the age of 5 years per 1000 live births !MR Number of deaths under the age of 1 year per 1000 live births NMR Number of deaths under the age of 28 days per 1000 live births ENMR Number of deaths under the age of 7 days per 1000 live births
In terms of under 5 mortality (U5MR), India ranks 46th among 193 countries. The U5MR in India (52 per 1000 live births) is unacceptably high given our stature as an economic, scientific and strategic power. U5MR in Japan (3), UK (5), USA (8), Sri Lanka (17), China (18) and Brazil (19) is worth comparing with that of India. Great nations not only have negligible child mortality, but also ensure good health, nutrition, education and opportunities to their children. Majority (56%) of under 5 deaths occur in the neonatal period (<28 days of life), and the neonatal mortality accounts for 70% infant deaths.
There has been a steady decline in child deaths. U5MR has declined by almost 50% between 1990 and 2010 from 117 to 59 per 1000 live births.However, decline in neonatal mortality rate (NMR) has been slower. In the decade of 2001-10, infant mortality rate (IMR) declined by 34%, while NMR decreased by 17.5% (Fig. 1.1). More worrying is the fact that the level of early neonatal mortality (deaths under 7 days of life) has remained unchanged.
Reduction in infant mortality is the foremost development goal of the country. India is a signatory of the millennium declaration and thereby committed to the Millennium Development Goals (MDC). The MDC 4 encompasses reduction of U5MR by two-thirds by 2015 from the 1990 baseline. Since the U5MR in 1990 was 117 per 1000 live births, the MDC4 goal is to attain U5MR of 39 per 1000 live births by 2015. This corresponds to an IMR of 29 per 1000 live births. Given the prevailing levels (Fig. 1.1), India would have to further accelerate her child survival action to attain MDC 4. This is difficult, but achievable. The XII Plan aims to bring IMR to 25 per 1000 live births by 2017.
Why do children die?
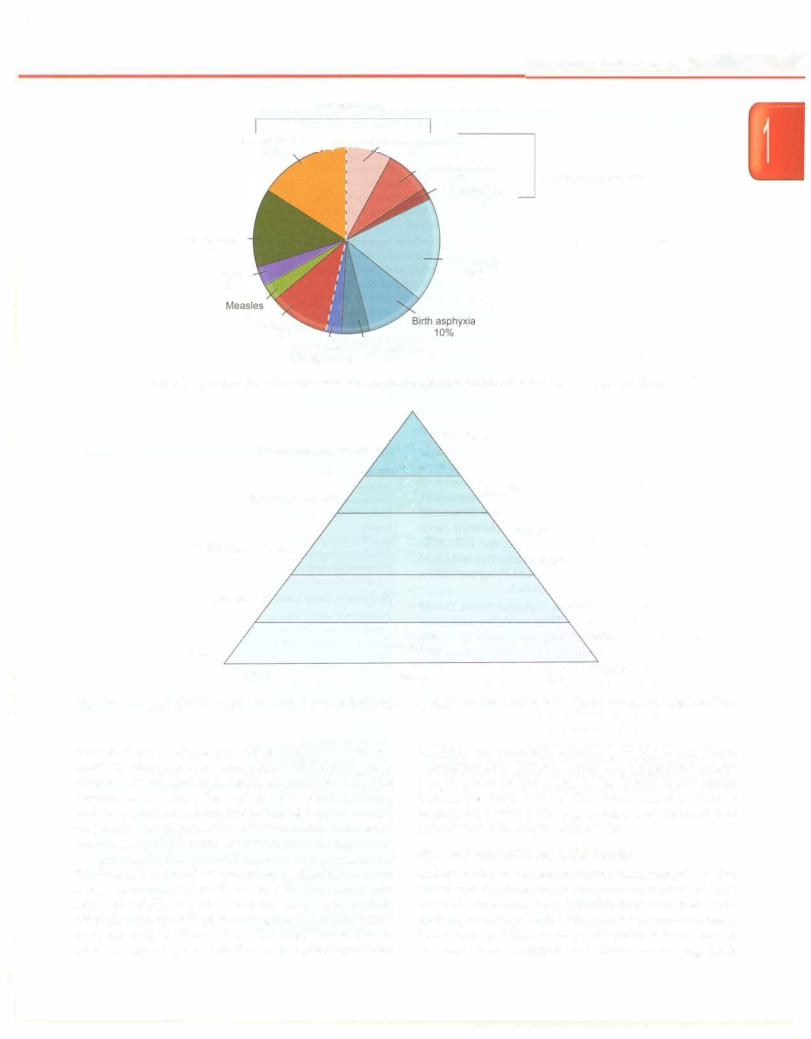
Theeightimportantcauses of under 5mortality inchildren in India are: (i) pneumonia (24%), (ii) complications of prematurity (18%), (iii) diarrhea (11%), (iv) birth asphyxia (10%), (v) neonatal sepsis (8%), (vi) congenital anomalies (4%), (vii) measles (3%), and (viii) injuries (3%) (Fig. 1.2). The above causes are the proximate conditions that lead to death. Poverty, illiteracy, low caste, rural habitat, harmful cultural practices, and poor access to safe water andsanitation are importantdeterminants ofchild health. Undernutrition is a critical underlying intermediate risk factor of child mortality, associated with 35% of under 5 child deaths. Undernutrition causes stunting and wasting, predisposes to infections and is associated with adult disorders (hypertension, diabetes, heart disease) and low economic productivity.
Health System in India
The rural health system in India is depicted in Fig. 1.3. At the bottom of the pyramid is the village with an average population of 1,000. There are two workers at this level, an Accredited Social Health Activist (ASHA) who is a woman volunteer from the same village placed as the frontline worker of the health sector, and an Anganwadi
80 |
|
|
|
|
|
|
|
|
|
|
|
|
|
70 |
|
|
|
|
|
|
|
|
|
|
|
|
|
60 |
|
|
|
|
|
|
|
|
|
|
|
|
|
50 |
|
|
|
|
|
|
|
|
|
|
|
|
|
40 |
|
|
|
|
|
|
|
|
|
|
|
|
|
30 |
|
|
|
|
|
|
|
|
|
|
|
|
|
20 |
|
|
15 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
10 |
|
|
|
|
|
|
|
|
|
|
|
|
|
0 |
+---r----,---,----,---,---,---,-----r---,----,---,-------,------, |
||||||||||||
|
2000 |
2001 |
2002 |
2003 |
2004 |
2005 |
2006 |
2007 |
2008 |
2009 |
2010 |
2011 |
2012 |
-+- IMR
..... NMR
...,_ EarlyNMR
"*" Late NMR
Fig. 1.1: Trends in neonatal and infant mortality rates (Data from Sample Registration System)
Introduction to Pediatrics -
|
|
Pneumonia 24% |
|
||
|
|
|
|
|
|
Pneumonia |
_-._-__Neonatal pneumonia |
|
|||
|
|||||
16% |
|
8% |
|
|
|
|
|
|
Neonatal sepsis |
|
|
|
|
|
8% |
Neonatal infections 18% |
|
|
|
|
|
Neonatal diarrhea |
|
Other disorders |
|
2% |
|
||
|
|
|
|
||
14% |
|
|
|
|
|
|
|
|
|
Prematurity |
|
Injury |
|
18% |
|
||
3% |
|
|
|
|
|
3% Diarrhea |
|
|
|
|
|
|
11%Other neonatal Malformations |
|
|||
|
conditions 3% |
4% |
|
|
|
Fig. 1.2: Causes of under 5 child deaths. The area to the right of the dotted line indicates neonatal conditions
Pediatrician, MO, nurses |
Medical |
Population |
|
||||
colleges |
|
|
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
Tertiary hospitals |
|
|
||
|
|
|
|
|
|
|
|
|
|
|
District |
|
|
1800,000 |
|
Pediatrician, MO, nurses |
|
|
hospitals |
|
|
|
|
|
|
(n=615) |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Community health centers |
500,000 |
|
||||
|
|
|
|||||
Pediatrician, MO, nurses |
|
|
(n=4,809) |
|
|
|
|
|
|
|
|
|
|
100,000 |
|
MO, nurses |
Primary health centers |
30,000 |
|||||
|
|
(n=23,887) |
|
|
|||
|
|
|
|
|
|||
|
|
|
Subcenters |
|
|
|
5,000 |
ANM |
|
|
(n=148,124) |
|
|
|
|
|
|
|
|
|
|
|
|
ASHA |
|
|
Village |
|
|
AWW |
1,000 |
|
|
|
|
|
|||
Fig. 1.3: Rural health system in India. ANM auxiliary nurse midwife; ASHA accredited social health activist; AWW anganwadi worker, MO medical officer
worker of the health sector, and an Anganwadi Worker (AWW), belonging to the Integrated Child Development Services (ICDS), and responsible for nutrition and child development services. For every5,000population, there is asubcenter where 1-2 AuxiliaryNurse Midwives (A.NM) areposted.Therolesof ASHA,AWWand A.NM inmaternal, newborn and child health are shown in Table 1.2.
A primaryhealthcenter (PHC) caters to a population of 30,000 and is manned by one or two medical officers and nurses. A communityhealth center (CHC) covers a popu lation of 100,000 and has provision for general medical officersas alsospecialists,includinga pediatrician.District hospitals and medical college hospitals provide more advancedspecialty services. The private practitioners and
facilities are primarily located in urban areas. Rural population also accesses services of unqualified practi tioners which are not a part of the formal health sector. Unlike the rural system, the urban health system is unstructured with multiple providers and dominance of private sectorfor healthcareservices.
National Programs on Child Health
Child health has been at the core of our health policy. The Universal Immunization Program launched in 1985 focusedonimmunizationagainstsixdiseases (tuberculosis, poliomyelitis, diphtheria, pertussis, tetanus andmeasles). The Diarrheal Disease Control Program was initiated in 1981 and AcuteRespiratoryInfections Control Programin

__Essen tialPed ia trics__________________________________
_______________
Table 1.2: Roles of grassroots functionaries in child health |
|
Provider |
Role in maternal, newborn and child health |
Accredited Social Health |
Mobilizing pregnant mother for antenatal check and care |
Activist (ASHA) |
Accompanying pregnant mother to facility for delivery |
|
Home care of the newborn |
|
Facilitating immunization |
|
Promoting complementary feeding |
|
Primary care in diarrhea and pneumonia |
|
Health education |
Anganwadi Worker (AWW) |
Providing nutrition supplement to pregnant mother |
|
Facilitating antenatal checks and immunization |
|
Promoting infant and young child feeding |
|
Growth monitoring of children |
|
Supplementary nutrition to children |
|
Managing malnourished children |
|
Providing IMNCI services for neonates and children |
|
Nonformal preschool education |
Auxiliary Nurse Midwife (ANM) |
Antenatal checks and care of pregnant mothers |
|
Immunization |
Supervising ASHA and AWW in newborn and child care
Providing IMNCI services for neonates and children
Health education
IMNCI Integrated Management of Neonatal and Childhood Illness
1990. In 1992, India launched the Child Survival and Safe Motherhood Program (CSSM) by combining interventions for child survival (immunization, control of diarrheal disease, respiratory infections, vitamin A supplementation, essential newborn care) and maternal health (antenatal care, deliveries in institutions, emergency obstetric care). In 1997, the Program for Family Planning and the CSSM Programwere merged to createthe Reproductive and Child Health Program. In phase 2 of the RCH Program (2005), adolescent health component was added.
The government launched the National Rural Health Mission (NRHM) in 2005. This mission included investment in public health, improvements in health systems, focus on communities, decentralization and demand-side interventions to improve effectiveness of the programs. The RCH Program was integrated into the NRHM, with prime focus on child and maternal health. Strategies include deployment of more than 900,000ASHAs; an increase in ANMs, nurses and doctors; setting up of village health and sanitation; strengthened primary health care infrastructure; strengthened program management capacity, establishment of patient welfare committees at facilities and creation of emergency transport networks.
The RMNCH+A Strategy (2073): Ongoing Programs for Neonates, Children and Adolescents
Table 1.3: Intervention packages under the RMNCH+A Strategy Adolescent health
Adolescent nutrition and folic acid supplementation Adolescent FriendlyHealthServices (AdolescentHealthClinics) Counselingonadolescent reproductive healthand other health issues
Scheme for promotion of menstrual hygiene among rural adolescent girls
Preventive health checkups and screening for diseases, deficiencyanddisability
Pregnancy, child birth and immediate newborn care
Preventive use of folic acid in periconceptional period Antenatal package and tracking of high-risk pregnancies Skilled obstetric care and essential newborn care including resuscitation
Emergency obstetric and newborn care (EmONC) Postpartum care for mother and baby Postpartum IUCD insertion and sterilization
Implementation of preconception and prenatal diagnostic techniques Act
Newborn and child care
Home based newborn care Facility based newborn care
Integrated Management of Common Childhood Illnesses Immunization
Child health screening and early intervention (Rashtriya Bal Swasthya Karyakram)
Reproductive health
In 2013, the government reviewed maternal and child health program under NRHM and launched a Strategic Approach to Reproductive, Maternal, Newborn, Child and Adolescent Health (RMNCH+A) under the XII Plan. The intervention packages under the RMNCH+A strategy are summarized in Table 1.3; details are shown in Table 1.4.
Community based doorstep distribution of contraceptives Promotion of spacing methods
Sterilization services Comprehensive abortion care
Prevention and management of sexually transmitted diseases or reproductive infections
IUCD intrauterine contraceptive device

Future of Child Health
The nation is addressing child health challenges with greaterdynamismthan ever before. Investments arebeing madeforhealthprogramsandhealthsystemstrengthening. Conditional cash transfers and entitlements are enshrined to stimulate demand for maternal, newborn and child
Introduction to Pediatrics -
healthcare. ICDSisbeing strengthened,particularly inhigh burdendistricts toaddresschildhoodundernutrition. The country is surging ahead with stronger economy and accelerated development. Indiaispoisedtoattainlow child mortality rate, and improve remarkably the health and nutrition status of her children in near future.
Table 1.4: Summary of maternal, newborn and child health services in the RMNCH+A Strategy under NRHM
Pregnancy, childbirth and |
Interventions |
immediate newborn care |
|
Skilled obstetric care and essential newborn care including resuscitation
Emergency obstetric and newborn care (EmONC)
Postpartum care for mother and baby
Newborn and child care
Home-based newborn care
Facility-based newborn care
Package
Facility deliveries by skilled birth attendants Neonatal resuscitation
Essentialnewborn care (warmth, hygienic care, breastfeeding, extra care of small babies, problem detection)
Linkages to facility-based newborn care for sick neonates
Program drivers: The schemes that drive uptake of the intervention packages Janani Suraksha Yojana (]SY) that provides cash incentive to the woman (and to the
ASHA) for delivery in the facility
Janani Shishu Suraksha Karyakram (JSSK) that entitles the mother and less than one month neonate to free delivery, medicines/blood, diet, pickup and drop in government
facilities
Navjat Shishu Suraksha Kan;akram that aims to train nurses and doctors in neonatal resuscitation
Interventions
Home visits by ASHAs (six for facility born babies, on days 3, 7, 14, 21, 28 and 42; an extra visit on day 1 for home births)
Interventions for infants
Examination; counsel for warmth; breastfeeding; hygiene; extra care of low birthweight babies; detection of sickness, referral
Interventions for mother
Postpartum care and counseling for family planning
ASHA given cash incentive for home care, birthweight record, birth registration and immunization (BCG, first dose OPV and DPT)
Special newborn care units (SNCU)
These specialized newborn units at district hospitals with specialized equipments including radiant warmers. These units have a minimum of 12-16 beds with a staff of 3 physicians, 10 nurses and 4 support staff to provide round the clock services for new born requiring special care, such as those with very low birthweight, neonatal sepsis/ pneumonia and common complications
Newborn stabilization units (NBSU)
These are step down units providing facilities for neonates from the periphery where babies can be stabilized through effective care. These are set up in CHCs and provide services, including resuscitation, provision of warmth, initiation of breastfeeding, prevention of infection and cord care, supportive care: oxygen, IV fluids, provision for monitoring of vital signs and referral
Newborn care comers (NBCC)
These are special corners within the labor room at all facilities (PHC, CHC, DH) where deliveries occur. Services include resuscitation, provision of warmth, prevention of infections and early initiation of breastfeeding
Program drivers: The schemes that drive uptake of the intervention packages Janani Shishu Suraksha Kan;akram (JSSK) that entitles the mother and neonate to free
delivery, medicines/blood, diet, pickup and drop in government facilities
Contd...
