
- •1. Topographic Surface Anatomy
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •3. Superficial Face
- •Guide
- •Facts & Hints
- •4. Neck
- •Guide
- •Facts & Hints
- •5. Nasal Region
- •Guide
- •Facts & Hints
- •6. Oral Region
- •Guide
- •Facts & Hints
- •7. Pharynx
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •13. Cerebral Vasculature
- •Guide
- •Facts & Hints
- •14. Topographic Anatomy
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •16. Spinal Cord
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Thorax
- •18. Topographic Anatomy
- •Guides
- •Facts & Hints
- •19. Mammary Gland
- •Guides
- •Facts & Hints
- •20. Body Wall
- •Guides
- •Facts & Hints
- •21. Lungs
- •Guides
- •Facts & Hints
- •22. Heart
- •Guides
- •Facts & Hints
- •23. Mediastinum
- •Guides
- •Facts & Hints
- •Abdomen
- •24. Topographic Anatomy
- •Guide
- •Facts & Hints
- •25. Body Wall
- •Guide
- •Facts & Hints
- •26. Peritoneal Cavity
- •Guide
- •Facts & Hints
- •27. Viscera (Gut)
- •Guide
- •Facts & Hints
- •28. Viscera (Accessory Organs)
- •Guide
- •Facts & Hints
- •29. Visceral Vasculature
- •Guide
- •Facts & Hints
- •30. Innervation
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •32. Topographic Anatomy
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •35. Urinary Bladder
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •39. Testis, Epididymis & Ductus Deferens
- •Guide
- •Facts & Hints
- •40. Rectum
- •Guide
- •Facts & Hints
- •41. Vasculature
- •Guide
- •Facts & Hints
- •42. Innervation
- •Guide
- •Facts & Hints
- •Upper Limb
- •43. Topographic Anatomy
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •48. Neurovasculature
- •Guide
- •Facts & Hints
- •Lower Limb
- •49. Topographic Anatomy
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •51. Knee
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •Guide
- •Facts & Hints
- •54. Neurovasculature
- •Guide
- •Facts & Hints

27 Viscera (Gut)
STUDYAIMS
At the end of your study, you should be able to:
Describe the structure of the stomach and its neurovascular supply
Describe the structure of the duodenum, its immediate anatomic relationships, and its neurovascular supply Understand the orientation of the small bowel within the abdomen and describe its divisions and neurovascular supply Understand the course of the large bowel within the abdomen and describe its divisions and neurovascular supply List distinguishing features of the jejunum, ileum, and large intestine
211 / 425
GUIDE
Abdomen: Viscera (Gut)
Stomach
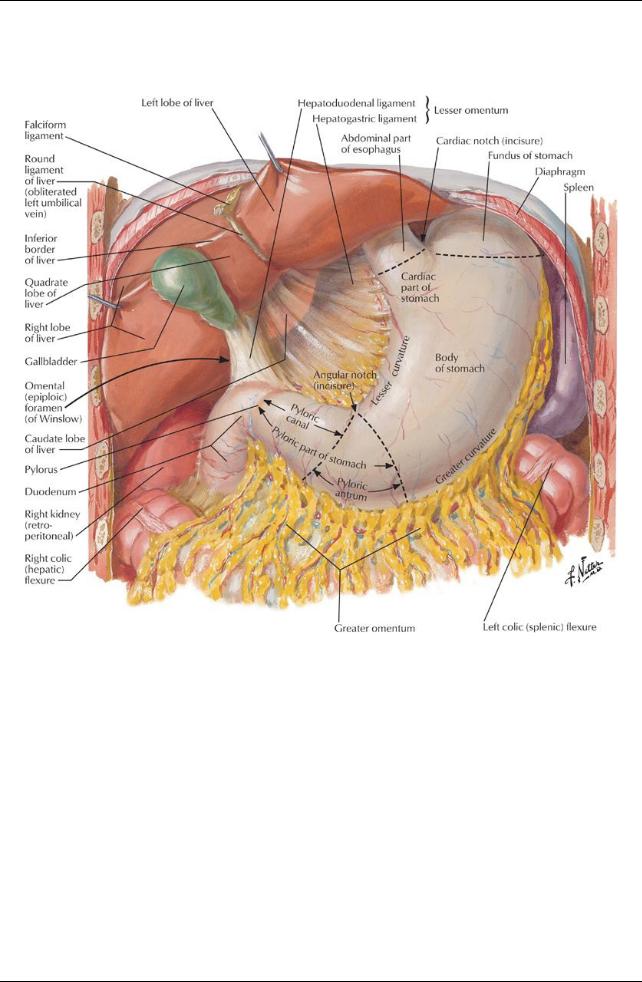
[Plate 267, Stomach in Situ]
212 / 425
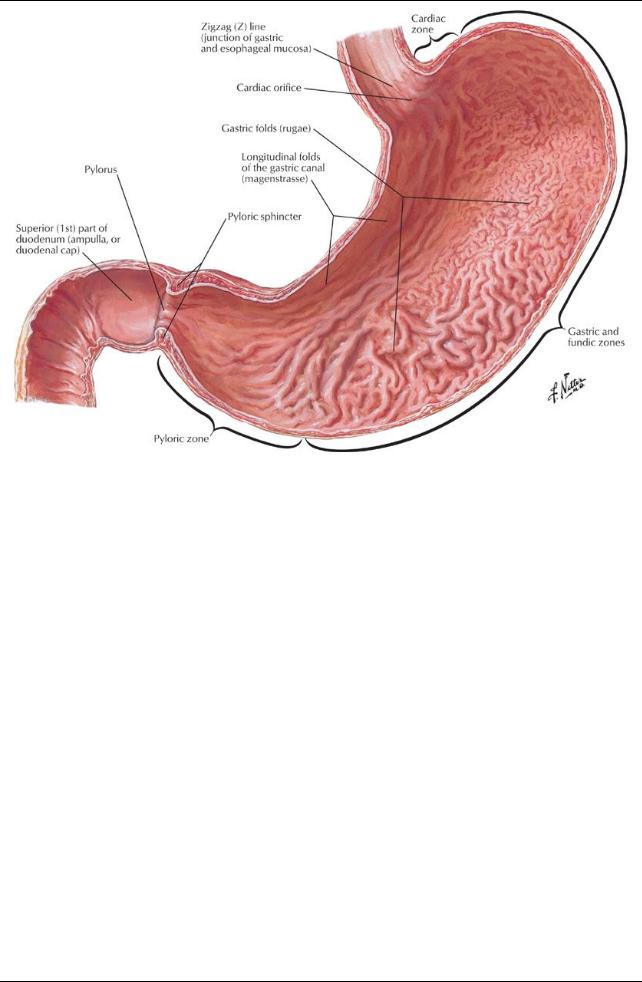
[Plate 268, Mucosa of Stomach]
213 / 425
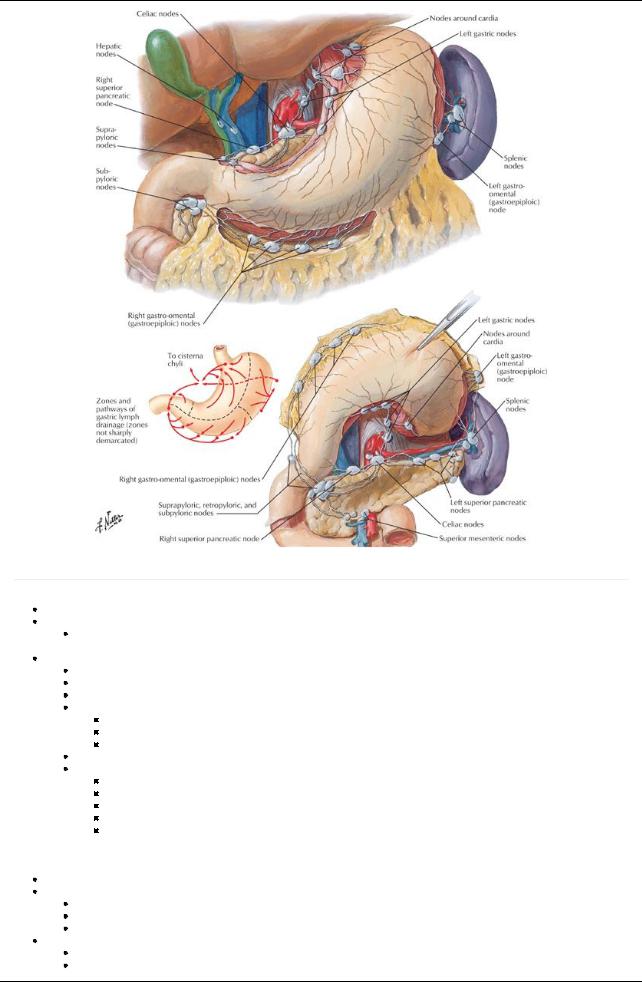
[Plate 293, Lymph Vessels and Nodes of Stomach]
page 142 page 143
J-shaped enlargement of the gastrointestinal tract Chief function: enzymatic digestion
Acidic gastric secretions convert food into liquid chime
 Passes fairlyquicklyinto the duodenum Parts of the stomach
Passes fairlyquicklyinto the duodenum Parts of the stomach
Greater curvature: long, convexborder
Lesser curvature: short, concave border
Cardia: surrounds cardial (esophageal) orifice
Fundus: dilated upper part
Above the level of the esophageal orifice
Dilated byfluid, food, but mainlygas
Separated from esophagus bycardiac notch
Body: between fundus and pyloric antrum
Pyloric part
Begins at level of angular incisure: indentation two thirds of the wayalong the lesser curvature
Widest region: pyloric antrum
Antrum leads to pyloric canal
Pylorus: surrounds pyloric orifice Pyloric sphincter
a.Thick, circular middle layer of muscularis externa
b.Controls passage of chime into duodenum
c.Normallyclosed in tonic contraction, except during peristalsis
Three muscle layers: outer longitudinal, inner circular, and innermost oblique Internal surface thrown into numerous longitudinal folds-rugae
Gastric canal = longitudinal fold along lesser curvature
Forms during swallowing
Accommodates the passage of liquid
Covered byperitoneum except where blood vessels run over it, and over a small area posterior to the cardiac orifice
Double layer of peritoneum extends between stomach and liver and duodenum and liver: lesser omentum Two layers of lesser omentum wrap around stomach and leave greater curvature as great omentum
214 / 425
Vascular supply(Section 4-6: Abdomen-Visceral Vasculature)
Arteries
Left gastric from celiac trunk
Right gastric from common hepatic artery
Right gastroepiploic (gastro-omental) from proper hepatic or gastroduodenal arteries
Left gastroepiploic from splenic artery
Short gastric arteries (four to five) from distal splenic artery
Veins
Follow the arteries
Right and left gastrics drain to portal vein
Short gastrics and left gastroepiploic drain into splenic vein → superior mesenteric vein (SMV) → portal vein
Right gastroepiploic drains to SMV
Lymphatics
Follow the arteries
 Drain into gastric, gastroepiploic, pancreaticosplenic, and pyloric nodes Innervation (Section 4-7: Abdomen-Innervation)
Drain into gastric, gastroepiploic, pancreaticosplenic, and pyloric nodes Innervation (Section 4-7: Abdomen-Innervation)
Parasympathetic supply
From anterior and posterior vagal trunks
Increase peristalsis and relaxpyloric sphincter
Sympathetic supply
From T6-T9 spinal cord segments via great splanchnic nerve to celiac plexus Inhibit peristalsis and contract pyloric sphincter
Duodenum
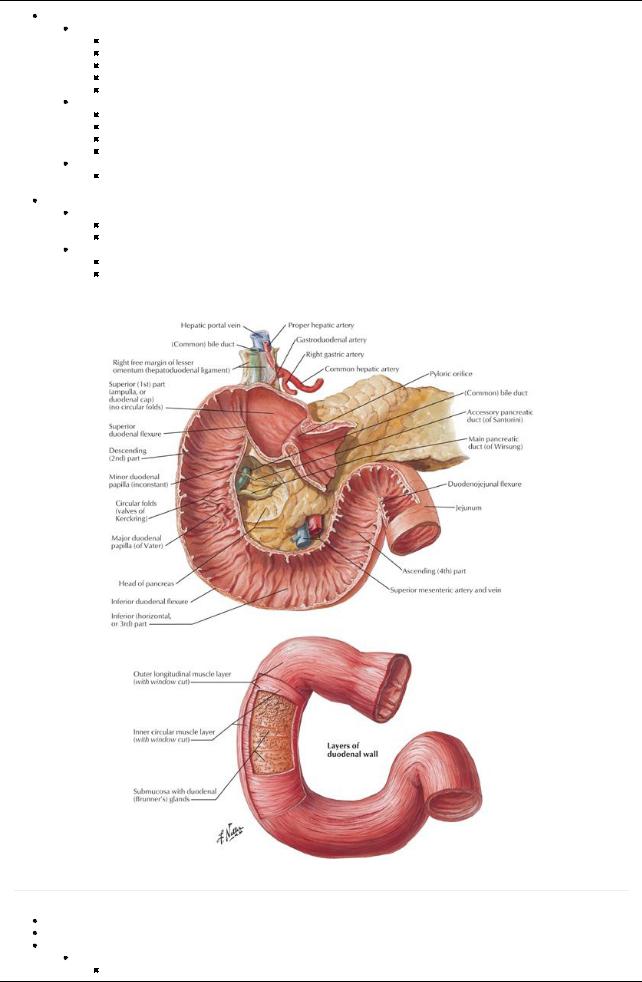
[Plate 271, Mucosa and Musculature of Duodenum]
page 143
page 144
First and shortest part of small intestine
Follows a C-shaped course around the head of the pancreas
Consists of four parts (parts 2 through 4 are retroperitoneal)
Superior (first) part: anterolateral to bodyof L1
Ascends from pylorus
215 / 425
Is connected to liver byhepatoduodenal ligament (part of lesser omentum)
Portal vein, bile duct, and IVC located posteriorly
Descending (second) part
Descends along the right of L1-L3
Contains major duodenal papilla on posteromedial wall = opening of hepatopancreatic ampulla
Horizontal (third) part
Crosses inferior vena cava (IVC), aorta, and L3 vertebra
Is crossed bysuperior mesenteric artery(SMA) and SMVand root of mesentery
Ascending (fourth) part
Ascends to L2 on the left side
Curves anteriorlyat the duodenojejunal flexure
 Flexure is supported bythe ligament of Treitz Vascular supply(Section 4-6: Abdomen-Visceral Vasculature)
Flexure is supported bythe ligament of Treitz Vascular supply(Section 4-6: Abdomen-Visceral Vasculature)
Arteries
Gastroduodenal artery, branch of common hepatic → superior anterior and posterior pancreaticoduodenal arteries
SMA→ anterior and posterior inferior pancreaticoduodenal arteries
Important anastomoses between celiac trunk and SMAvia duodenal arteries
Veins
Follow the arteries
Drain directlyor indirectlyinto the portal vein
Lymphatics
Follow the arteries
 Drain into pancreaticoduodenal, pyloric, superior mesenteric, and celiac lymph nodes Innervation (Section 4-7: Abdomen-Innervation)
Drain into pancreaticoduodenal, pyloric, superior mesenteric, and celiac lymph nodes Innervation (Section 4-7: Abdomen-Innervation)
Parasympathetic supplyfrom the vagus via celiac and superior mesenteric plexuses
Sympathetic supplyvia celiac and superior mesenteric plexuses, traveling on pancreaticoduodenal arteries
Jejunum and ileum
[Plate 273, Ileocecal Region]
page 144
page 145
Begins at duodenojejunal juncture and ends at ileocecal junction
216 / 425

Together are approximately6 m long The mesentery
Double layered fold of peritoneum
Attaches jejunum and ileum to posterior abdominal wall
Root of mesentery
Follows an oblique line
Runs inferiorlyand to the right, from ligament of Treitzto ileocolic junction
 Between two layers are SMA, SMV, lymph nodes, fat, and autonomic nerves Jejunum
Between two layers are SMA, SMV, lymph nodes, fat, and autonomic nerves Jejunum
Approximatelytwo fifths of the length
Mainlyin the left upper quadrant (LUQ)
 Thick-walled and veryvascular Ileum
Thick-walled and veryvascular Ileum
Approximatelythree fifths of the length
Mainlyin the right lower quadrant (RLQ)
Thin-walled and less vascular
Terminates at the ileocecal junction
Vascular supply(Section 4-6: Abdomen-Visceral Vasculature)
Arteries
Superior mesenteric artery
Fifteen to 18 branches from SMAto jejunum and ileum
Branches unite to form loops or arches (arterial arcades)
Arcades give rise to straight arteries = vasa recta
Double row of arcades to ileum
Veins
SMVdrains ileum and jejunum
Posterior to neck of pancreas joins splenic vein to form portal vein
Lymphatics
Specialised lymphatic vessels that absorb fat = lacteals
Absorbed fat = chyle
Lacteals found in villi (finger-like projections of intestinal mucosa)
Lacteals drain to lymphatic plexuses in walls of jejunum and ileum
Lymphatics pass between the layers of the mesenteryto mesenteric lymph nodes and then to superior mesenteric or ileocolic nodes
 Lymph drains to cisterna chyli Innervation (Section 4-7: Abdomen-Innervation)
Lymph drains to cisterna chyli Innervation (Section 4-7: Abdomen-Innervation)
Parasympathetic supply
Preganglionic fibers from the posterior vagal trunks
Synapse on postganglionic cells in myenteric and submucosal plexuses in intestinal wall
Sympathetic supply
Preganglionic fibers from T5-T9 spinal cord segments → sympathetic trunks → greater and lesser splanchnic nerves Synapse on postganglionic cells in celiac and superior mesenteric ganglia
Large intestine (colon)
217 / 425

[Plate 276, Mucosa and Musculature of Large Intestine]
218 / 425
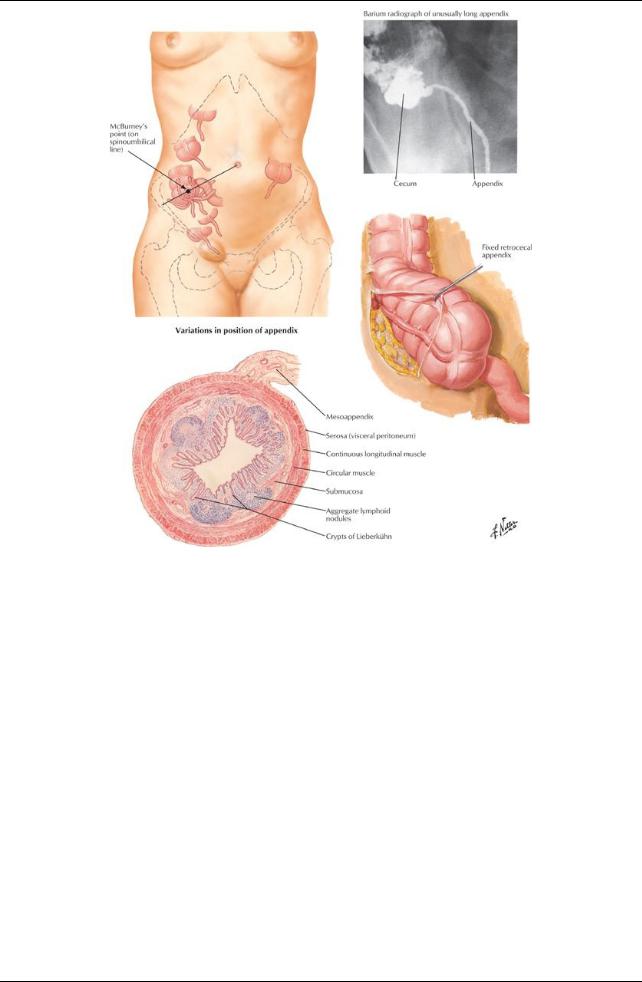
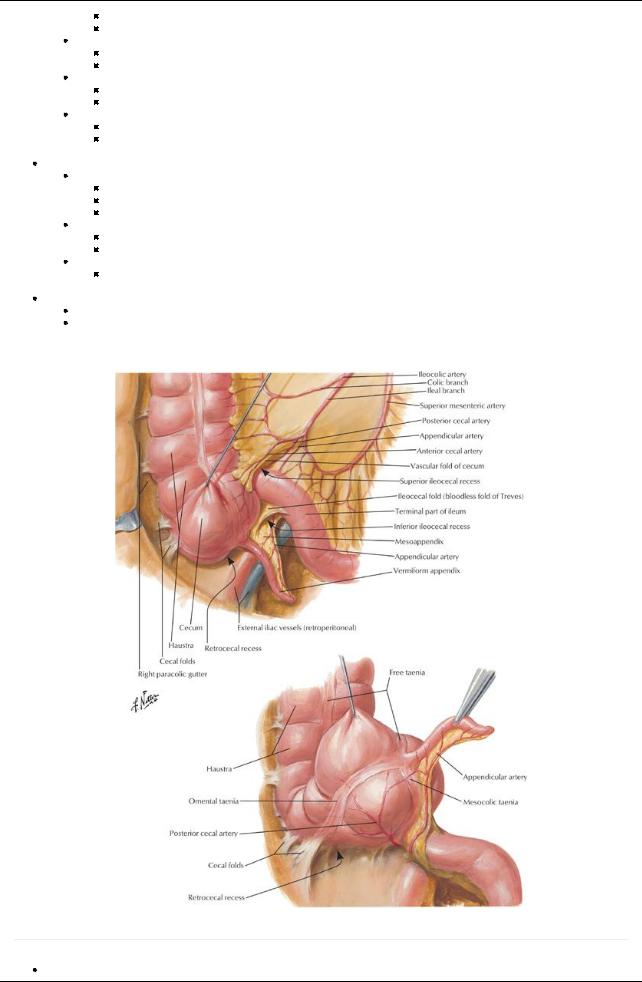
[Plate 275, (Vermiform) Appendix]
219 / 425
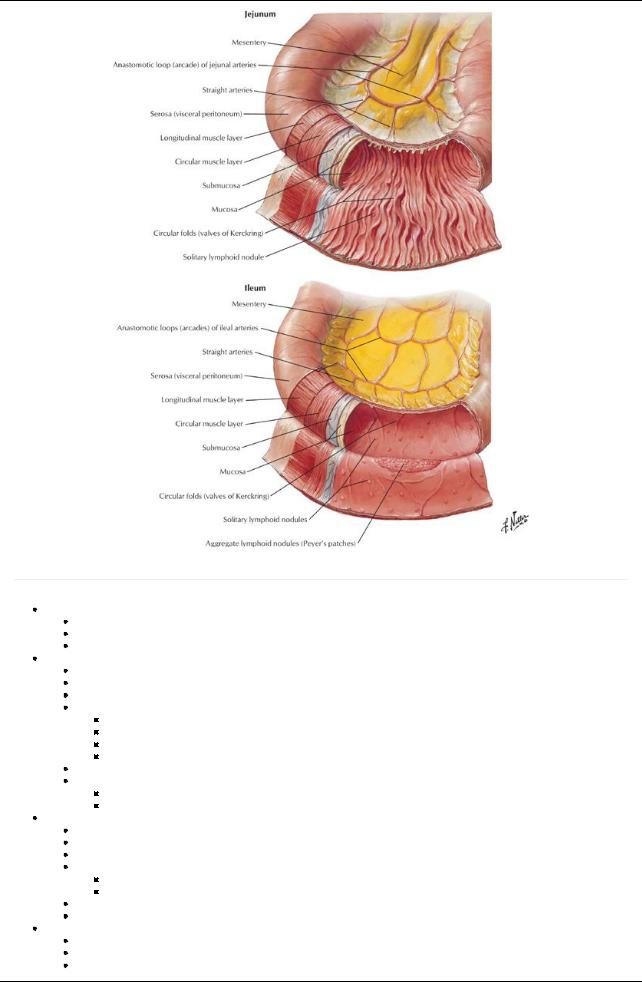
[Plate 272, Mucosa and Musculature of Small Intestine]
page 145 page 146
Characterized by:
Teniae coli: 3 thickened longitudinal bands of muscle (absent from appendix and rectum)
Haustra: sacculations of the colon caused byteniae coli
Appendices epiploicae: fattylobules of omentum
Cecum
Blind pouch, approximately7.5 cm in diameter
No mesentery, but maybe bound to the abdominal wall bycecal folds of peritoneum
Invaginated byileum to form the ileocecal valve-does not prevent reflux
Vermiform appendix
Arises from the posteromedial side of cecum
Usuallyretrocecal
Has a short mesenteryfrom cecum: mesoappendix
Supplied byappendicular arteryfrom ileocolic artery
Vascular supply: ileocolic arteryand vein, with lymph to ileocolic nodes
Nerves: sympathetic and parasympathetic nerves from the superior mesenteric plexus
Parasympathetic fibers from vagus nerves
Sympathetic fibers from lower thoracic spinal cord segments
Ascending colon
On right side of posterior abdominal wall
Extends from cecum to liver, where it turns at right colic flexure (hepatic flexure)
Is secondarilyretroperitoneal
Vascular supplyfrom branches/tributaries of SMA/SMV
Ileocolic arteryand vein
Right colic arteryand vein
Lymphatics to epicolic and paracolic nodes
Nerve supplyfrom the superior mesenteric plexus
Transverse colon
Extends from hepatic flexure on the right to splenic flexure on the left
Largest and most mobile section of colon
Attached to posterior abdominal wall byits mesentery: the transverse mesocolon
220 / 425

Vascular supplyfrom branches/tributaries of SMA/SMV
Left colic arteryand vein
Right colic arteryand vein
Middle colic arteryand vein
Lymphatic drainage to middle colic nodes
Nerve supply
Superior mesenteric plexus along right and middle colic arteries
 Inferior mesenteric plexus along left colic arteries Descending colon
Inferior mesenteric plexus along left colic arteries Descending colon
On left side of posterior abdominal wall
Extends from splenic flexure to sigmoid colon
Is secondarilyretroperitoneal
Mayhave a short mesenteryin one third of people
Vascular supplyfrom branches/tributaries of IMA/IMV
Left colic arteryand vein
Superior sigmoid arteryand vein
Lymphatic drainage to the epicolic and paracolic nodes
Innervation
Sympathetic fibers from the lumbar sympathetic trunk and superior hypogastric plexus

 Parasympathetic fibers from the pelvic splanchnic nerves Sigmoid colon
Parasympathetic fibers from the pelvic splanchnic nerves Sigmoid colon
S-shaped loop of variable length
Links descending colon with rectum
Long mesenterywith a V-shaped root: sigmoid mesocolon
Vascular supplyfrom branches/tributaries of inferior mesenteric artery(IMA)/inferior mesenteric vein (IMV)
Left colic arteryand vein
Superior sigmoid arteryand vein
Lymphatic drainage to the epicolic and paracolic nodes
Innervation
Sympathetic fibers from the lumbar sympathetic trunk and superior hypogastric plexus
Parasympathetic fibers from the pelvic splanchnic nerves
Rectum and anal canal (Section 5-9: Pelvis and Perineum-Rectum and Anal Canal)
Rectum
Begins anterior to the bodyof the S3 vertebra
Is approximately15 cm long
Connects sigmoid colon and anal canal
Fixed, and continuous with the anal canal
Anal canal
Begins at distal end of rectal ampulla Extends from pelvic diaphragm to anus
221 / 425
