
- •Preface to the 3rd edition
- •General Pharmacology
- •Systems Pharmacology
- •Therapy of Selected Diseases
- •Subject Index
- •Abbreviations
- •General Pharmacology
- •History of Pharmacology
- •Drug and Active Principle
- •The Aims of Isolating Active Principles
- •European Plants as Sources of Effective Medicines
- •Drug Development
- •Congeneric Drugs and Name Diversity
- •Oral Dosage Forms
- •Drug Administration by Inhalation
- •Dermatological Agents
- •From Application to Distribution in the Body
- •Potential Targets of Drug Action
- •External Barriers of the Body
- •Blood–Tissue Barriers
- •Membrane Permeation
- •Binding to Plasma Proteins
- •The Liver as an Excretory Organ
- •Biotransformation of Drugs
- •Drug Metabolism by Cytochrome P450
- •The Kidney as an Excretory Organ
- •Presystemic Elimination
- •Drug Concentration in the Body as a Function of Time—First Order (Exponential) Rate Processes
- •Time Course of Drug Concentration in Plasma
- •Time Course of Drug Plasma Levels during Repeated Dosing (A)
- •Time Course of Drug Plasma Levels during Irregular Intake (B)
- •Accumulation: Dose, Dose Interval, and Plasma Level Fluctuation (A)
- •Dose–Response Relationship
- •Concentration–Effect Curves (B)
- •Concentration–Binding Curves
- •Types of Binding Forces
- •Agonists—Antagonists
- •Other Forms of Antagonism
- •Enantioselectivity of Drug Action
- •Receptor Types
- •Undesirable Drug Effects, Side Effects
- •Drug Allergy
- •Cutaneous Reactions
- •Drug Toxicity in Pregnancy and Lactation
- •Pharmacogenetics
- •Placebo (A)
- •Systems Pharmacology
- •Sympathetic Nervous System
- •Structure of the Sympathetic Nervous System
- •Adrenergic Synapse
- •Adrenoceptor Subtypes and Catecholamine Actions
- •Smooth Muscle Effects
- •Cardiostimulation
- •Metabolic Effects
- •Structure–Activity Relationships of Sympathomimetics
- •Indirect Sympathomimetics
- •Types of
- •Antiadrenergics
- •Parasympathetic Nervous System
- •Cholinergic Synapse
- •Parasympathomimetics
- •Parasympatholytics
- •Actions of Nicotine
- •Localization of Nicotinic ACh Receptors
- •Effects of Nicotine on Body Function
- •Aids for Smoking Cessation
- •Consequences of Tobacco Smoking
- •Dopamine
- •Histamine Effects and Their Pharmacological Properties
- •Serotonin
- •Vasodilators—Overview
- •Organic Nitrates
- •Calcium Antagonists
- •ACE Inhibitors
- •Drugs Used to Influence Smooth Muscle Organs
- •Cardiac Drugs
- •Cardiac Glycosides
- •Antiarrhythmic Drugs
- •Iron Compounds
- •Prophylaxis and Therapy of Thromboses
- •Possibilities for Interference (B)
- •Heparin (A)
- •Hirudin and Derivatives (B)
- •Fibrinolytics
- •Intra-arterial Thrombus Formation (A)
- •Formation, Activation, and Aggregation of Platelets (B)
- •Inhibitors of Platelet Aggregation (A)
- •Presystemic Effect of ASA
- •Plasma Volume Expanders
- •Lipid-lowering Agents
- •Diuretics—An Overview
- •NaCl Reabsorption in the Kidney (A)
- •Aquaporins (AQP)
- •Osmotic Diuretics (B)
- •Diuretics of the Sulfonamide Type
- •Potassium-sparing Diuretics (A)
- •Vasopressin and Derivatives (B)
- •Drugs for Gastric and Duodenal Ulcers
- •Laxatives
- •Antidiarrheal Agents
- •Drugs Affecting Motor Function
- •Muscle Relaxants
- •Nondepolarizing Muscle Relaxants
- •Depolarizing Muscle Relaxants
- •Antiparkinsonian Drugs
- •Antiepileptics
- •Pain Mechanisms and Pathways
- •Eicosanoids
- •Antipyretic Analgesics
- •Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
- •Cyclooxygenase (COX) Inhibitors
- •Local Anesthetics
- •Opioid Analgesics—Morphine Type
- •General Anesthesia and General Anesthetic Drugs
- •Inhalational Anesthetics
- •Injectable Anesthetics
- •Sedatives, Hypnotics
- •Benzodiazepines
- •Pharmacokinetics of Benzodiazepines
- •Therapy of Depressive Illness
- •Mania
- •Therapy of Schizophrenia
- •Psychotomimetics (Psychedelics, Hallucinogens)
- •Hypothalamic and Hypophyseal Hormones
- •Thyroid Hormone Therapy
- •Glucocorticoid Therapy
- •Follicular Growth and Ovulation, Estrogen and Progestin Production
- •Oral Contraceptives
- •Antiestrogen and Antiprogestin Active Principles
- •Aromatase Inhibitors
- •Insulin Formulations
- •Treatment of Insulin-dependent Diabetes Mellitus
- •Treatment of Maturity-Onset (Type II) Diabetes Mellitus
- •Oral Antidiabetics
- •Drugs for Maintaining Calcium Homeostasis
- •Drugs for Treating Bacterial Infections
- •Inhibitors of Cell Wall Synthesis
- •Inhibitors of Tetrahydrofolate Synthesis
- •Inhibitors of DNA Function
- •Inhibitors of Protein Synthesis
- •Drugs for Treating Mycobacterial Infections
- •Drugs Used in the Treatment of Fungal Infections
- •Chemotherapy of Viral Infections
- •Drugs for the Treatment of AIDS
- •Drugs for Treating Endoparasitic and Ectoparasitic Infestations
- •Antimalarials
- •Other Tropical Diseases
- •Chemotherapy of Malignant Tumors
- •Targeting of Antineoplastic Drug Action (A)
- •Mechanisms of Resistance to Cytostatics (B)
- •Inhibition of Immune Responses
- •Antidotes and Treatment of Poisonings
- •Therapy of Selected Diseases
- •Hypertension
- •Angina Pectoris
- •Antianginal Drugs
- •Acute Coronary Syndrome— Myocardial Infarction
- •Congestive Heart Failure
- •Hypotension
- •Gout
- •Obesity—Sequelae and Therapeutic Approaches
- •Osteoporosis
- •Rheumatoid Arthritis
- •Migraine
- •Common Cold
- •Bronchial Asthma
- •Emesis
- •Alcohol Abuse
- •Local Treatment of Glaucoma
- •Further Reading
- •Further Reading
- •Picture Credits
- •Drug Indexes

142 Antianemics
Iron Compounds
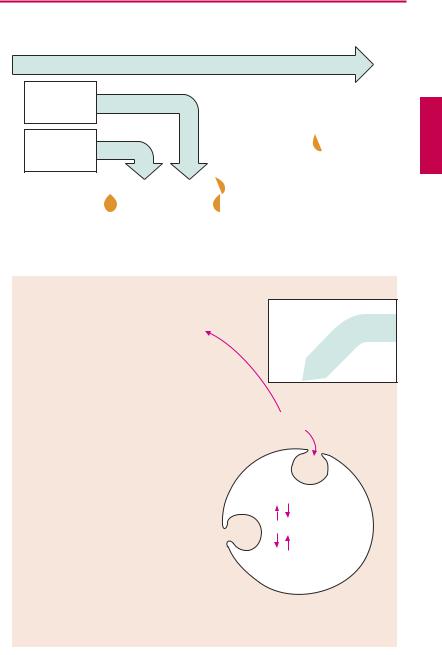
Not all iron ingested in food is equally absorbable. Trivalent Fe3+ is virtually not taken up from the neutral milieu of the small bowel, where the divalent Fe2+ is markedly better absorbed. Uptake is particularly ef cient in the form of heme (present in hemoglobin and myoglobin). Within the mucosal cells of the gut, iron is oxidized and either deposited as ferritin (see below) or passed on to the transport protein, transferrin. The amount absorbed does not exceed that needed to balance losses due to epithelial shedding from skin and mucosae or hemorrhage (socalled“mucosal block”). Inmenthisamount is ~ 1 mg/day, in women it is ~ 2 mg/day (because of menstrual blood loss); it corresponds to about 10% of the dietary intake. The transferrin–iron complex undergoes endocytotic uptake into erythrocyte precursors to be utilized for hemoglobin synthesis. About 70% of the total body store of iron (~ 5 g) is contained within erythrocytes. When these are degraded by macrophages of the mononuclear phagocyte system, iron is liberated from hemoglobin. Fe3+can be stored as ferritin (= protein apoferritin + Fe3+) or be returned to erythropoiesis sites via transferrin.
A frequent cause of iron deficiency is chronic blood loss due to gastric/intestinal ulcers or tumors. One liter of blood contains 500 mg of iron in healthy condition. Despite a significant increase in absorption rate, absorption isunable to keep up with lossesand the body store of iron falls. Iron deficiency results in impaired synthesis of hemoglobin and anemia.
The treatment of choice (after the cause of bleeding has been found and eliminated) consists in the oral administration of Fe2+- compounds, e.g., ferrous sulfate (daily dose 100 mg of iron, equivalent to 300 mg of FeSO4, divided into multiple doses). Replenishing of iron stores may take several months. Oral administration, however, is ad-
vantageous in that it is impossible to overload the body with iron through an intact mucosa because of its demand-regulated absorption (mucosal block).
Adverse effects. The frequent gastrointestinal complaints (epigastric pain, diarrhea, constipation) necessitate intake ofiron preparations with or after meals, although absorption is higher from the empty stomach.
Interactions. Antacids inhibit iron absorption. Combination with ascorbic acid (vitamin C) to protect Fe2+ from oxidation to Fe3+ is theoretically sound but practically is not needed.
Parenteral administration of Fe3+ salts is indicated only when adequate oral replacement is not possible. There is a risk of overdosage, with iron deposition in tissues (hemosiderosis). The binding capacity of transferrin is limited and free Fe3+ is toxic. Therefore, Fe3+complexes are employed that can donate Fe3+ directly to transferrin or can be phagocytosed by macrophages, enabling iron to be incorporated into the ferritin store. Possible adverse effects are: with i.m. injection, persistent pain at the injection site and skin discoloration; with i.v. injection, flushing, hypotension, anaphylactic shock.
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.
|
|
Iron Compounds |
143 |
|
A. Iron: possible routes of administration and fate in the organism |
|
|
||
|
Fe(III) salts nonabsorbable |
|
|
|
Oral |
|
|
|
|
intake |
Fe(II) salts |
|
|
|
|
Heme-Fe |
|
|
|
|
|
Fe(III) |
|
|
Absorption |
|
Fe(III) |
|
|
Duodenum |
|
|
|
|
|
|
|
|
|
upper jejunum |
|
|
|
|
|
|
Ferritin |
|
|
|
|
Parenteral |
|
|
Transport |
|
administration |
|
|
Fe(III) |
Fe(III) |
|
|
|
Plasma |
|
|
||
|
|
|
|
|
|
Transferrin |
|
|
|
|
|
i.v. |
i.m. |
|
Uptake into |
Hemoglobin |
|
|
|
erythroblast |
|
Fe(III) complexes |
|
|
|
|
|
|
|
bone marrow |
|
|
|
|
|
|
Fe(III) |
|
|
Erythrocyte |
|
Ferritin |
|
|
|
|
|
|
|
blood |
|
|
|
|
|
|
Hemosiderin |
|
|
|
|
= aggregated |
|
|
|
|
ferritin |
|
|
Loss through |
|
Uptake into macrophages |
|
|
bleeding |
|
|
||
|
spleen, liver, bone marrow |
|
||
|
|
|
||
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.

144 Antithrombotics
Prophylaxis and Therapy of Thromboses
Upon vascular injury, the coagulation system is activated: thrombocytes and fibrin molecules coalesce into a “plug” that seals the defect and halts bleeding (hemostasis). Unnecessary formation of an intravascular clot—a thrombosis—can be life-threatening. If the clot forms on an atheromatous plaque in a coronary artery, myocardial infarction is imminent; a thrombus in a deep leg vein can be dislodged and carried into a lung artery and can cause pulmonary embolism.
Drugs that decrease the coagulability of blood, such as coumarins and heparin (A) are employed for the prophylaxis of thromboses. In addition, attempts are directed, by means of acetylsalicylic acid, at inhibiting the aggregation of blood platelets, which are prominently involved in intra-ar- terial thrombogenesis (p.152). For the therapy of thrombosis, drugs are used that dissolve the fibrin meshwork—fibrinolytics (p.150).
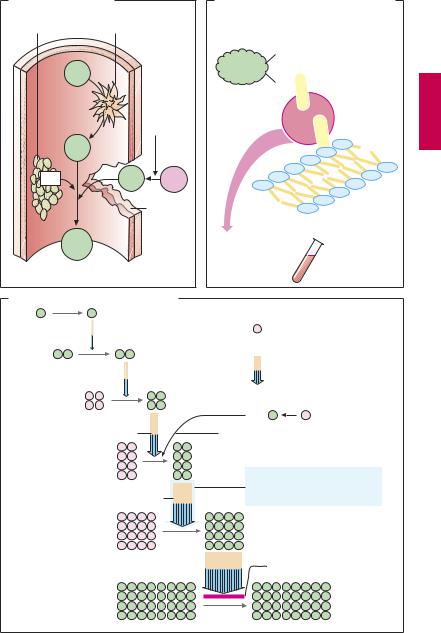
An overview of the coagulation cascade and sites of action for coumarins and heparin is shown in (A). There are two ways to initiate the cascade (B): (1) conversion of factor XII into its active form (XIIa, intrinsic system) at intravascular sites denuded of endothelium; (2) conversion of factor VII into VIIa (extrinsic system) under the influence of a tissue-derived lipoprotein (tissue thromboplastin). Both mechanisms converge via factor X into a common final pathway.
The clotting factors are protein molecules. “Activation” mostly means proteolysis (cleavage of protein fragments) and, with the exception of fibrin, conversion into proteinhydrolyzing enzymes (proteases). Some activated factors require the presence of phospholipids (PL) and Ca2+ for their proteolytic activity. Conceivably, Ca2+ ions cause the adhesion of factor to a phospholipid surface, as depicted in (B). Phospholipids are contained in platelet factor 3 (PF3), which is released from aggregated platelets, and in tissue
thromboplastin (A). The sequential activation of several enzymes allows the aforementioned reactions to “snowball” (symbolized in C by increasing number of particles), culminating in massive production of fibrin.
Ca2+-chelators (B) prevent the enzymatic activity of Ca2+-dependent factors; they contain COO– groups that bind Ca2+ ions (C): citrate and EDTA (ethylenediaminetetraacetic acid) form soluble complexes with Ca2+; oxalate precipitates Ca2+ as insoluble calcium oxalate. Chelation of Ca2+ cannot be used in vivo for therapeutic purposes because Ca2+ concentrations would have to be lowered to a level incompatible with life (hypocalcemic tetany). These compounds (sodium salts) are, therefore, used only for rendering blood incoagulable outside the body. This effect can be reversed at any time by addition of Ca2+ ions.
In vivo, the progression of the coagulation cascade can be inhibited as follows (C):
1.Coumarin derivatives decrease the blood concentrations of inactive factors II, VII, IX and X, by inhibiting their synthesis in the liver.
2.The complex consisting of heparin and antithrombin III neutralizes the protease activity of activated factors; unlike unfractionated heparin, low-molecular-weight heparin fragments or the “minimal molecular subunit of heparin,” fondaparinux, inhibit only activated factor Xa when complexed with antithrombin III.
3.Hirudin and its derivatives (bivalirudin, lepirudin) block the active center of thrombin.
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.
Prophylaxis and Therapy of Thromboses |
145 |
A. Activation of clotting |
|
|
B. Inhibition of clotting by removal of Ca2+ |
|
Platelets |
Endothelial defect |
Clotting factor |
|
|
|
|
|
|
|
|
|
|
COO– |
|
XII |
|
|
COO– |
|
|
|
|
|
|
|
|
Tissue |
+ |
+ |
|
|
kinase |
Ca |
|
|
|
thrombo- |
|
|
XIIa |
|
|
|
– |
|
|
– |
– |
|
|
|
|
|
|
|
|
|
– |
|
PF3 |
VIIa |
VII |
– |
|
|
|
|
– |
|
|
|
Vessel |
|
Phospholipids, |
|
|
rupture |
|
|
|
|
|
e.g., PF3 |
|
|
|
|
|
|
Fibrin |
|
|
Ca2+ chelation |
|
|
|
|
Citrate |
only in vitro |
|
|
|
EDTA |
|
|
|
|
|
|
|
|
|
Oxalate |
|
C. Inhibition of clotting cascade in vivo |
|
|
||
XII |
XIIa |
|
|
|
|
|
Synthesis susceptible to |
|
|
|
inhibition by coumarins |
XI |
XIa |
|
Reaction susceptible to |
|
|
|
|
|
|
|
inhibition by heparin– |
|
|
|
antithrombin complex |
|
IX |
IXa |
|
|
|
VIIa |
VII |
|
VIII + Ca2+ + Pl |
Ca2+ + Pl (phospholipids) |
|
|
X |
Xa |
|
|
|
Susceptible to inhibition also |
|
|
|
by low-molecular-weight |
|
|
V + Ca2+ + Pl |
heparin and fondaparinux |
|
|
Prothrombin II |
IIa Thrombin |
|
|
|
|
Hirudin |
|
Fibrinogen I |
|
Ia Fibrin |
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.
