
- •Preface to the 3rd edition
- •General Pharmacology
- •Systems Pharmacology
- •Therapy of Selected Diseases
- •Subject Index
- •Abbreviations
- •General Pharmacology
- •History of Pharmacology
- •Drug and Active Principle
- •The Aims of Isolating Active Principles
- •European Plants as Sources of Effective Medicines
- •Drug Development
- •Congeneric Drugs and Name Diversity
- •Oral Dosage Forms
- •Drug Administration by Inhalation
- •Dermatological Agents
- •From Application to Distribution in the Body
- •Potential Targets of Drug Action
- •External Barriers of the Body
- •Blood–Tissue Barriers
- •Membrane Permeation
- •Binding to Plasma Proteins
- •The Liver as an Excretory Organ
- •Biotransformation of Drugs
- •Drug Metabolism by Cytochrome P450
- •The Kidney as an Excretory Organ
- •Presystemic Elimination
- •Drug Concentration in the Body as a Function of Time—First Order (Exponential) Rate Processes
- •Time Course of Drug Concentration in Plasma
- •Time Course of Drug Plasma Levels during Repeated Dosing (A)
- •Time Course of Drug Plasma Levels during Irregular Intake (B)
- •Accumulation: Dose, Dose Interval, and Plasma Level Fluctuation (A)
- •Dose–Response Relationship
- •Concentration–Effect Curves (B)
- •Concentration–Binding Curves
- •Types of Binding Forces
- •Agonists—Antagonists
- •Other Forms of Antagonism
- •Enantioselectivity of Drug Action
- •Receptor Types
- •Undesirable Drug Effects, Side Effects
- •Drug Allergy
- •Cutaneous Reactions
- •Drug Toxicity in Pregnancy and Lactation
- •Pharmacogenetics
- •Placebo (A)
- •Systems Pharmacology
- •Sympathetic Nervous System
- •Structure of the Sympathetic Nervous System
- •Adrenergic Synapse
- •Adrenoceptor Subtypes and Catecholamine Actions
- •Smooth Muscle Effects
- •Cardiostimulation
- •Metabolic Effects
- •Structure–Activity Relationships of Sympathomimetics
- •Indirect Sympathomimetics
- •Types of
- •Antiadrenergics
- •Parasympathetic Nervous System
- •Cholinergic Synapse
- •Parasympathomimetics
- •Parasympatholytics
- •Actions of Nicotine
- •Localization of Nicotinic ACh Receptors
- •Effects of Nicotine on Body Function
- •Aids for Smoking Cessation
- •Consequences of Tobacco Smoking
- •Dopamine
- •Histamine Effects and Their Pharmacological Properties
- •Serotonin
- •Vasodilators—Overview
- •Organic Nitrates
- •Calcium Antagonists
- •ACE Inhibitors
- •Drugs Used to Influence Smooth Muscle Organs
- •Cardiac Drugs
- •Cardiac Glycosides
- •Antiarrhythmic Drugs
- •Iron Compounds
- •Prophylaxis and Therapy of Thromboses
- •Possibilities for Interference (B)
- •Heparin (A)
- •Hirudin and Derivatives (B)
- •Fibrinolytics
- •Intra-arterial Thrombus Formation (A)
- •Formation, Activation, and Aggregation of Platelets (B)
- •Inhibitors of Platelet Aggregation (A)
- •Presystemic Effect of ASA
- •Plasma Volume Expanders
- •Lipid-lowering Agents
- •Diuretics—An Overview
- •NaCl Reabsorption in the Kidney (A)
- •Aquaporins (AQP)
- •Osmotic Diuretics (B)
- •Diuretics of the Sulfonamide Type
- •Potassium-sparing Diuretics (A)
- •Vasopressin and Derivatives (B)
- •Drugs for Gastric and Duodenal Ulcers
- •Laxatives
- •Antidiarrheal Agents
- •Drugs Affecting Motor Function
- •Muscle Relaxants
- •Nondepolarizing Muscle Relaxants
- •Depolarizing Muscle Relaxants
- •Antiparkinsonian Drugs
- •Antiepileptics
- •Pain Mechanisms and Pathways
- •Eicosanoids
- •Antipyretic Analgesics
- •Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
- •Cyclooxygenase (COX) Inhibitors
- •Local Anesthetics
- •Opioid Analgesics—Morphine Type
- •General Anesthesia and General Anesthetic Drugs
- •Inhalational Anesthetics
- •Injectable Anesthetics
- •Sedatives, Hypnotics
- •Benzodiazepines
- •Pharmacokinetics of Benzodiazepines
- •Therapy of Depressive Illness
- •Mania
- •Therapy of Schizophrenia
- •Psychotomimetics (Psychedelics, Hallucinogens)
- •Hypothalamic and Hypophyseal Hormones
- •Thyroid Hormone Therapy
- •Glucocorticoid Therapy
- •Follicular Growth and Ovulation, Estrogen and Progestin Production
- •Oral Contraceptives
- •Antiestrogen and Antiprogestin Active Principles
- •Aromatase Inhibitors
- •Insulin Formulations
- •Treatment of Insulin-dependent Diabetes Mellitus
- •Treatment of Maturity-Onset (Type II) Diabetes Mellitus
- •Oral Antidiabetics
- •Drugs for Maintaining Calcium Homeostasis
- •Drugs for Treating Bacterial Infections
- •Inhibitors of Cell Wall Synthesis
- •Inhibitors of Tetrahydrofolate Synthesis
- •Inhibitors of DNA Function
- •Inhibitors of Protein Synthesis
- •Drugs for Treating Mycobacterial Infections
- •Drugs Used in the Treatment of Fungal Infections
- •Chemotherapy of Viral Infections
- •Drugs for the Treatment of AIDS
- •Drugs for Treating Endoparasitic and Ectoparasitic Infestations
- •Antimalarials
- •Other Tropical Diseases
- •Chemotherapy of Malignant Tumors
- •Targeting of Antineoplastic Drug Action (A)
- •Mechanisms of Resistance to Cytostatics (B)
- •Inhibition of Immune Responses
- •Antidotes and Treatment of Poisonings
- •Therapy of Selected Diseases
- •Hypertension
- •Angina Pectoris
- •Antianginal Drugs
- •Acute Coronary Syndrome— Myocardial Infarction
- •Congestive Heart Failure
- •Hypotension
- •Gout
- •Obesity—Sequelae and Therapeutic Approaches
- •Osteoporosis
- •Rheumatoid Arthritis
- •Migraine
- •Common Cold
- •Bronchial Asthma
- •Emesis
- •Alcohol Abuse
- •Local Treatment of Glaucoma
- •Further Reading
- •Further Reading
- •Picture Credits
- •Drug Indexes

14 Drug Administration
Drug Administration by Inhalation
Inhalation in the form of an aerosol, a gas, or a mist permits drugs to be applied to the bronchial mucosa and, to a lesser extent, to the alveolar membranes. This route is chosen for drugs intended to affect bronchial smooth muscle or the consistency of bronchial mucus. Furthermore, gaseous or volatile agents can be administered by inhalation with the goal of alveolar absorption and systemic effects (e.g., inhalational anesthetics, p.216). Aerosols are formed when a drug solution or micronized powder is converted into a mist or dust, respectively.
In conventional sprays (e.g., nebulizer), the air blast required for the aerosol formation is generated by the stroke of a pump. Alternatively, the drug is delivered from a solution or powder packaged in a pressurized canister equipped with a valve through which a metered dose is discharged. During use, the inhaler (spray dispenser) is held directly in front of the mouth and actuated at the start of inspiration. The effectiveness of delivery depends on the position of the device in front of the mouth, the size of the aerosol particles, and the coordination between opening the spray valve and inspiration. The size of the aerosol particles determines the speed at which they are swept along by inhaled air, and hence the depth of penetration into the respiratory tract. Particles > 100 µm in diameter are trapped in the oropharyngeal cavity; those having diameters between 10 and 60 µm will be deposited on the epithelium of the bronchial tract. Particles < 2 µm in diameter can reach the alveoli, but they will be exhaled again unless they settle out.
Drug deposited on the mucous lining of the bronchial epithelium is partly absorbed and partly transported with bronchial mucustoward the larynx. Bronchial mucus travels upward owing to the orally directed undulatory beat of the epithelial cilia. Physiologically, this mucociliary transport functions to remove inspired dust particles.
Thus, only a portion of the drug aerosol (~ 10%) gains access to the respiratory tract and just a fraction of this amount penetrates the mucosa, whereas the remainder of the aerosol undergoes mucociliary transport to the laryngopharynx and is swallowed. The advantage of inhalation (i.e., localized application without systemic load) is fully exploited by using drugs that are poorly absorbed from the intestine (tiotropium, cromolyn) or are subject to first-pass elimination (p.42); for example, glucocorticoids such as beclomethasone dipropionate, budesonide, flunisolide, and fluticasone dipropionate or β-agonists such as salbutamol and fenoterol.
Even when the swallowed portion of an inhaled drug is absorbed in unchanged form, administration by this route has the advantage that drug concentrations at the bronchi will be higher than in other organs.
The ef ciencyofmucociliary transportdepends on the force of kinociliary motion and the viscosity of bronchial mucus. Both factors can be altered pathologically (e.g., by smoker’s cough or chronic bronchitis).
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.
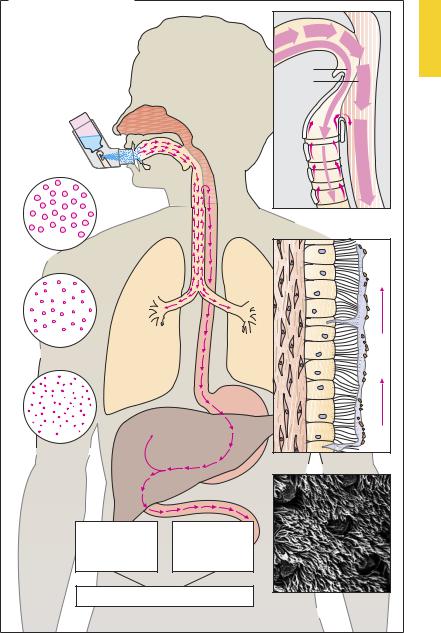
Drug Administration by Inhalation |
15 |
A. Application by inhalation |
|
|
Depth of |
|
|
penetration |
|
|
of inhaled |
|
|
aerosolized |
|
10% |
drug solution |
|
|
|
90% |
|
|
|
|
|
|
Drug swept up |
|
|
is swallowed |
100 m |
|
|
Nasopharynx |
|
Larynx |
|
|
|
10 m |
|
|
Trachea, bronchi |
|
|
|
|
1 cm/min |
>2 m |
|
|
Bronchioli, alveoli |
|
Mucociliary transport |
|
|
|
As complete |
As little |
|
presystemic |
enteral |
|
elimination |
absorption |
|
as possible |
as possible |
|
Low systemic burden |
Surface view of ciliated |
|
|
|
|
|
|
epithelium |
|
|
(scanning EM photograph) |
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.

16 Drug Administration
Dermatological Agents
Pharmaceutical preparations applied to the outer skin are intended either to provide skin care and protection from noxious influences (A) or to serve as a vehicle for drugs that are to be absorbed into the skin or, if appropriate, into the general circulation (B).
Skin Protection (A)
Protective agents are of several kinds to meet different requirements according to skin condition (dry, low in oil, chapped vs. moist, oily, elastic), and the type of noxious stimuli (prolonged exposure to water, regular use of alcohol-containing disinfectants, intense solar irradiation). Distinctions among protective agents are based upon consistency, physicochemical properties (lipophilic, hydrophilic), and the presence of additives.
Dusting powders are sprinkled onto the intact skin and consist of talc, magnesium stearate, silicon dioxide (silica), or starch. They adhere to the skin, forming a low-fric- tion film that attenuates mechanical irritation. Powders exert a drying (evaporative) effect.
Lipophilic ointment (oil ointment) consists of a lipophilic base (paraf n oil, petroleum jelly, wool fat) and may contain up to 10% powder materials, such as zinc oxide, titanium oxide, starch, or a mixture of these. Emulsifying ointments are made of paraf ns and an emulsifying wax, and are miscible with water.
Paste (oil paste) is an ointmentcontaining more than 10% pulverized constituents.
Lipophilic (oily) cream is an emulsion of water in oil, easier to spread than oil paste or oil ointment.
Hydrogel and water-soluble ointment achieve their consistency by means of different gel-forming agents (gelatin, methylcellulose, polyethylene glycol). Lotions are aqueous suspensions of water-insoluble and solid constituents.
Hydrophilic (aqueous) cream isanoil-in- water emulsion formed with the aid of an emulsifier; it may also be considered an oil- in-water emulsion of an emulsifying ointment.
All dermatological agents having a lipophilic base adhere to the skin as a waterrepellent coating. They do not wash off and they also prevent (occlude) outward passage of water from the skin. The skin is protected from drying, and its hydration and elasticity increase. Diminished evaporation of water results in warming of the occluded skin. Hydrophilic agents wash off easily and do not impede transcutaneous output of water. Evaporation of water is felt as a cooling effect.
Dermatological Agents as Vehicles (B)
In order to reach its site of action, a drug must leave its pharmaceutical preparation and enter the skin if a local effect is desired (e.g., glucocorticoid ointment), or be able to penetrate it if a systemic action is intended (transdermal delivery system, e.g., nitroglycerin patch, p.124). The tendency for the drug to leave the drug vehicle is higher the more the drug and vehicle differ in lipophilicity (high tendency: hydrophilic drug and lipophilic vehicle; and vice versa). Because the skin represents a closed lipophilic barrier (p.22), only lipophilic drugs are absorbed. Hydrophilic drugs fail even to penetrate the outer skin when applied in a lipophilic vehicle. This formulation can be useful when high drug concentrations are required at the skin surface (e.g., neomycin ointment for bacterial skin infections).
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.

|
|
|
|
|
|
|
|
Dermatological Agents |
17 |
|
|
||||||
A. Dermatologicals as skin protectants |
|
|
|
|
|
|
|
|
|
|
|||||||
|
|
|
|
|
|
|
|
|
|
||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Powder |
Solid |
Liquid |
|
|
|
|
|
|
|
|
|
|||||
|
|
|
Solution |
|
|
|
|||||||||||
|
|
|
|
|
|
|
|
|
|
||||||||
|
|
|
|
|
|
|
|
|
|
Aqueous |
|
Alcoholic |
|
|
|
||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||||
|
|
|
|
|
|
Dermatologicals |
|
|
|
|
|
||||||
|
Paste |
|
|
solution |
|
tincture |
|
|
|
||||||||
|
|
|
|
|
Semi-solid |
|
|
|
|
|
|
|
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||
|
Oily paste |
|
|
|
|
|
|
|
|
|
|
||||||
|
|
Hydrogel |
|
|
|
||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||
|
Ointment |
|
|
|
|
|
|
|
Lotion |
|
|
|
|||||
|
Lipophilic |
Hydrophilic |
|
Cream |
|
|
Suspen- |
|
Emulsion |
|
|
|
|||||
|
|
|
|
|
|
|
|
|
|
|
|||||||
|
ointment |
ointment |
|
Lipophilic |
Hydrophilic |
|
|
sion |
|
|
|
|
|
||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||
|
|
|
|
|
|
cream |
cream |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Fat, oil |
|
Water in oil |
|
Oil in water |
|
Gel, water |
|
Occlusive |
|
|
|
|
Permeable, |
|
|
|
|
|
|
|
coolant |
|
|
|
|
Perspiration |
|
|
||
|
|
|
impossible |
possible |
|
|
|
|
Dry, non-oily skin |
|
Oily, moist skin |
||||
B. Dermatologicals as drug vehicles |
|
|
|
|
|||
|
Lipophilic drug |
Lipophilic drug |
Hydrophilic drug |
Hydrophilic drug |
|||
|
in lipophilic |
in hydrophilic |
in lipophilic |
in hydrophilic |
|||
|
base |
base |
base |
base |
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Stratum corneum
Epithelium
Subcutaneous fat tissue
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.
