
- •Preface to the 3rd edition
- •General Pharmacology
- •Systems Pharmacology
- •Therapy of Selected Diseases
- •Subject Index
- •Abbreviations
- •General Pharmacology
- •History of Pharmacology
- •Drug and Active Principle
- •The Aims of Isolating Active Principles
- •European Plants as Sources of Effective Medicines
- •Drug Development
- •Congeneric Drugs and Name Diversity
- •Oral Dosage Forms
- •Drug Administration by Inhalation
- •Dermatological Agents
- •From Application to Distribution in the Body
- •Potential Targets of Drug Action
- •External Barriers of the Body
- •Blood–Tissue Barriers
- •Membrane Permeation
- •Binding to Plasma Proteins
- •The Liver as an Excretory Organ
- •Biotransformation of Drugs
- •Drug Metabolism by Cytochrome P450
- •The Kidney as an Excretory Organ
- •Presystemic Elimination
- •Drug Concentration in the Body as a Function of Time—First Order (Exponential) Rate Processes
- •Time Course of Drug Concentration in Plasma
- •Time Course of Drug Plasma Levels during Repeated Dosing (A)
- •Time Course of Drug Plasma Levels during Irregular Intake (B)
- •Accumulation: Dose, Dose Interval, and Plasma Level Fluctuation (A)
- •Dose–Response Relationship
- •Concentration–Effect Curves (B)
- •Concentration–Binding Curves
- •Types of Binding Forces
- •Agonists—Antagonists
- •Other Forms of Antagonism
- •Enantioselectivity of Drug Action
- •Receptor Types
- •Undesirable Drug Effects, Side Effects
- •Drug Allergy
- •Cutaneous Reactions
- •Drug Toxicity in Pregnancy and Lactation
- •Pharmacogenetics
- •Placebo (A)
- •Systems Pharmacology
- •Sympathetic Nervous System
- •Structure of the Sympathetic Nervous System
- •Adrenergic Synapse
- •Adrenoceptor Subtypes and Catecholamine Actions
- •Smooth Muscle Effects
- •Cardiostimulation
- •Metabolic Effects
- •Structure–Activity Relationships of Sympathomimetics
- •Indirect Sympathomimetics
- •Types of
- •Antiadrenergics
- •Parasympathetic Nervous System
- •Cholinergic Synapse
- •Parasympathomimetics
- •Parasympatholytics
- •Actions of Nicotine
- •Localization of Nicotinic ACh Receptors
- •Effects of Nicotine on Body Function
- •Aids for Smoking Cessation
- •Consequences of Tobacco Smoking
- •Dopamine
- •Histamine Effects and Their Pharmacological Properties
- •Serotonin
- •Vasodilators—Overview
- •Organic Nitrates
- •Calcium Antagonists
- •ACE Inhibitors
- •Drugs Used to Influence Smooth Muscle Organs
- •Cardiac Drugs
- •Cardiac Glycosides
- •Antiarrhythmic Drugs
- •Iron Compounds
- •Prophylaxis and Therapy of Thromboses
- •Possibilities for Interference (B)
- •Heparin (A)
- •Hirudin and Derivatives (B)
- •Fibrinolytics
- •Intra-arterial Thrombus Formation (A)
- •Formation, Activation, and Aggregation of Platelets (B)
- •Inhibitors of Platelet Aggregation (A)
- •Presystemic Effect of ASA
- •Plasma Volume Expanders
- •Lipid-lowering Agents
- •Diuretics—An Overview
- •NaCl Reabsorption in the Kidney (A)
- •Aquaporins (AQP)
- •Osmotic Diuretics (B)
- •Diuretics of the Sulfonamide Type
- •Potassium-sparing Diuretics (A)
- •Vasopressin and Derivatives (B)
- •Drugs for Gastric and Duodenal Ulcers
- •Laxatives
- •Antidiarrheal Agents
- •Drugs Affecting Motor Function
- •Muscle Relaxants
- •Nondepolarizing Muscle Relaxants
- •Depolarizing Muscle Relaxants
- •Antiparkinsonian Drugs
- •Antiepileptics
- •Pain Mechanisms and Pathways
- •Eicosanoids
- •Antipyretic Analgesics
- •Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
- •Cyclooxygenase (COX) Inhibitors
- •Local Anesthetics
- •Opioid Analgesics—Morphine Type
- •General Anesthesia and General Anesthetic Drugs
- •Inhalational Anesthetics
- •Injectable Anesthetics
- •Sedatives, Hypnotics
- •Benzodiazepines
- •Pharmacokinetics of Benzodiazepines
- •Therapy of Depressive Illness
- •Mania
- •Therapy of Schizophrenia
- •Psychotomimetics (Psychedelics, Hallucinogens)
- •Hypothalamic and Hypophyseal Hormones
- •Thyroid Hormone Therapy
- •Glucocorticoid Therapy
- •Follicular Growth and Ovulation, Estrogen and Progestin Production
- •Oral Contraceptives
- •Antiestrogen and Antiprogestin Active Principles
- •Aromatase Inhibitors
- •Insulin Formulations
- •Treatment of Insulin-dependent Diabetes Mellitus
- •Treatment of Maturity-Onset (Type II) Diabetes Mellitus
- •Oral Antidiabetics
- •Drugs for Maintaining Calcium Homeostasis
- •Drugs for Treating Bacterial Infections
- •Inhibitors of Cell Wall Synthesis
- •Inhibitors of Tetrahydrofolate Synthesis
- •Inhibitors of DNA Function
- •Inhibitors of Protein Synthesis
- •Drugs for Treating Mycobacterial Infections
- •Drugs Used in the Treatment of Fungal Infections
- •Chemotherapy of Viral Infections
- •Drugs for the Treatment of AIDS
- •Drugs for Treating Endoparasitic and Ectoparasitic Infestations
- •Antimalarials
- •Other Tropical Diseases
- •Chemotherapy of Malignant Tumors
- •Targeting of Antineoplastic Drug Action (A)
- •Mechanisms of Resistance to Cytostatics (B)
- •Inhibition of Immune Responses
- •Antidotes and Treatment of Poisonings
- •Therapy of Selected Diseases
- •Hypertension
- •Angina Pectoris
- •Antianginal Drugs
- •Acute Coronary Syndrome— Myocardial Infarction
- •Congestive Heart Failure
- •Hypotension
- •Gout
- •Obesity—Sequelae and Therapeutic Approaches
- •Osteoporosis
- •Rheumatoid Arthritis
- •Migraine
- •Common Cold
- •Bronchial Asthma
- •Emesis
- •Alcohol Abuse
- •Local Treatment of Glaucoma
- •Further Reading
- •Further Reading
- •Picture Credits
- •Drug Indexes
|
128 |
Inhibitors of the RAA System |
|
|
|
ACE Inhibitors |
elimination. Enalaprilat has a stronger and |
||
|
longer-lasting effect than captopril. |
|||
|
|
|
|
|
|
|
Angiotensin-converting enzyme (ACE) is a |
Indications are hypertension and cardiac |
|
|
|
component of the antihypotensive renin– |
failure. |
|
|
|
angiotensin–aldosterone (RAA) system. Re- |
Lowering of elevated blood pressure is |
|
|
|
nin is produced by specialized smooth |
predominantly brought about bydiminished |
|
|
|
muscle cells in the wall of the afferent arte- |
production of angiotensin II. Impaired deg- |
|
|
|
riole of the renal glomerulus. These cells |
radation of kinins that exert vasodilating ac- |
|
|
|
belong to the juxtaglomerular apparatus, |
tions may contribute to the effect. |
|
|
|
the site of contact between afferent arteriole |
In heart failure, cardiac output rises again |
|
|
|
and distal tubule, which plays an important |
after administration of an ACE inhibitor be- |
|
|
|
part in controlling nephron function. Stimuli |
cause ventricular afterload diminishes ow- |
|
|
||||
|
|
eliciting release of renin are: drop in renal |
ing to a fall in peripheral resistance. Venous |
|
|
|
perfusion pressure, decreased rate of deliv- |
congestion abates as a result of (1) increased |
|
|
|
ery of Na+ or Cl– to the distal tubules, as well |
cardiac output and (2) reduction in venous |
|
|
|
as β-adrenoceptor-mediated sympathoacti- |
return (decreased aldosterone secretion, de- |
|
|
|
vation. The glycoprotein renin enzymatically |
creased tonus of venous capacitance ves- |
|
|
|
cleaves the decapeptide angiotensin I from |
sels). |
|
|
|
its circulating precursor substrate angioten- |
|
|
|
|
sinogen. The enzyme ACE, in turn, produces |
Undesired effects. The magnitude of the |
|
|
|
biologically active angiotensin II from angio- |
antihypertensive effect of ACE inhibitors de- |
|
|
|
tensin I. |
|
pends on the functional state of the RAA |
|
|
ACE is a rather nonspecific peptidase that |
system. When the latter has been activated |
|
|
|
can cleave C-terminal dipeptides from vari- |
by loss of electrolytes and water (resulting |
|
|
|
ous peptides (dipeptidyl carboxypeptidase). |
from treatment with diuretic drugs), by car- |
|
|
|
As “kininase II,” it contributes to the inacti- |
diac failure, or by renal arterial stenosis, ad- |
|
|
|
vation of kinins, such as bradykinin. ACE is |
ministration of ACE inhibitors may initially |
|
|
|
also present in blood plasma; however, en- |
cause an excessive fall in blood pressure. Dry |
|
|
|
zyme localized in the luminal side of vascu- |
cough is a fairly frequent side effect, possibly |
|
|
|
lar endothelium is primarily responsible for |
caused by reduced inactivation of kinins in |
|
|
|
the formation of angiotensin II. |
the bronchial mucosa. In most cases, ACE |
|
|
|
Angiotensin II can raise blood pressure in |
inhibitors are well tolerated and effective. |
|
|
|
different ways, including (1) vasoconstric- |
Newer analogues include lisinopril, perindo- |
|
|
|
tion in both the arterial and venous limb of |
pril, ramipril, quinapril, fosinopril, benaze- |
|
|
|
the circulation; (2) stimulation of aldoste- |
pril, cilazapril, and trandolapril. |
|
|
|
rone secretion, leading to increased renal |
|
|
|
|
reabsorption of NaCl and water, hence an |
Antagonists at angiotensin II receptors. |
|
|
|
increased blood volume; (3) a central in- |
Two receptor subtypes can be distinguished: |
|
|
|
crease in sympathotonus and, peripherally, |
AT1, which mediates the above actions of |
|
|
|
enhanced release and effects of norepi- |
angiotensin II; and AT2, whose physiological |
|
|
|
nephrine. Chronically elevated levels of an- |
role is still unclear. Losartan is an AT1 recep- |
|
|
|
giotensin II can increase muscle mass in |
tor antagonist whose main (antihyperten- |
|
|
|
heart and arteries (trophic effect). |
sive) and side effects resemble those of ACE |
|
|
|
|
|
inhibitors. However, because it does not in- |
|
|
ACE inhibitors, such as captopril and enalap- |
hibit degradation of kinins, it does not cause |
|
|
|
rilat, the active metabolite of enalapril, occu- |
dry cough. Losartan is used in the therapy of |
|
|
|
py the enzyme as false substrates. Af nity |
hypertension. Other analogues are valsartan, |
|
|
|
significantly influences ef cacy and rate of |
irbesartan, eprosartan, and candesartan. |
|
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.
|
|
|
|
ACE Inhibitors |
129 |
||||
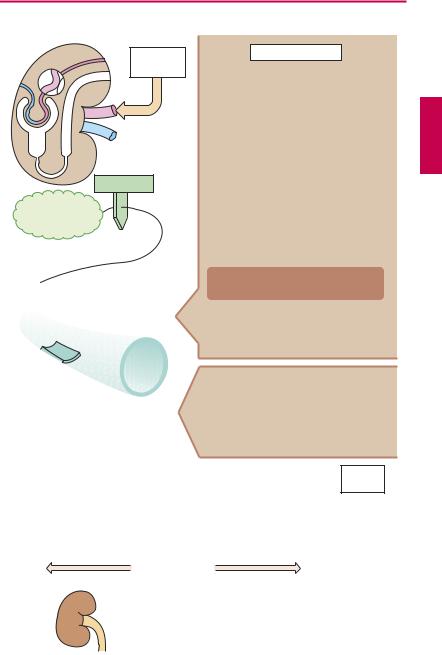
A. Renin-angiotensin-aldosterone system and inhibitors |
|
|
|
|
|
|
|||
Kidney |
|
|
|
ACE inhibitors |
|
|
|||
|
RR |
|
|
|
|
|
|
|
|
|
|
O |
O |
|
|
|
|
|
|
|
HO |
C |
C |
CH |
CH2 |
SH |
|
|
|
|
|
|
N |
CH3 |
|
|
Captopril |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
O |
O |
|
|
|
|
|
|
|
HO |
C |
C |
CH |
NH |
CH |
CH2 |
CH2 |
|
|
|
|
N |
CH3 |
|
C |
O |
|
|
|
|
|
|
|
|
|
|||
|
Renin |
|
|
|
|
O |
CH2 |
CH3 |
|
|
Enalaprilat |
|
|
Enalapril |
|
||||
|
|
|
|
|
|||||
Angiotensinogen |
|
ACE |
|
|
|
|
|
||
(α 2-globulin) |
|
|
|
|
|
Kinins |
|||
|
Ang I |
Angiotensin |
|
|
|
||||
|
|
|
I-converting |
|
|
|
|
||
|
|
|
enzyme |
carboxypeptidase |
|
|
|||
|
Angiotensin I (Ang I) |
|
Dipeptidyl |
|
|
||||
|
|
|
Kininase |
|
|||||
COOH |
(biologically inactive) |
|
|
|
|||||
|
|
|
|
II |
|
|
|||
|
|
|
|
|
|
|
|||
|
|
|
|
|
|
|
|
||
|
Ang II |
|
|
|
|
|
Degradation |
||
|
ACE |
|
|
|
|
|
|
products |
|
Vascular |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
endothelium |
|
|
|
|
|
|
|
|
|
|
Losartan |
|
|
CH2OH |
|
|
|||
|
Angiotensin II |
|
|
Cl |
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
N |
N |
|
|
|
H |
|
H2N |
|
|
|
|
|
|
N |
N |
|
|
H3C |
|
|
|
|
|
N |
N |
|
Receptors |
|
|
|
|
|
|
|
|
|
|
|
AT1-receptor antagonists |
||||||
|
|
|
|
||||||
|
Venous |
HMV |
|
|
|
|
RR |
||
|
supply |
|
|
|
|
||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Peripheral |
|
|||
|
|
|
|
|
resistance |
|
|||
|
Venous |
Resistance vessels |
|
|
|
||||
|
capacitance vessels |
|
|
|
|||||
|
Vasoconstriction |
|
|
|
|
|
|
|
|
NaCl |
Aldosterone |
|
|
|
|
Sympatho- |
|
||
H2O |
secretion |
|
|
|
|
activation |
|
||
|
|
|
|
|
|
|
|
|
|
|
K+ |
|
|
|
|
|
|
|
|
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.

130 Drugs Acting on Smooth Muscle
Drugs Used to Influence Smooth Muscle Organs
Bronchodilators. Narrowing of bronchioles raises airway resistance, e.g., in bronchial or bronchitic asthma. Several substances that are employed as bronchodilators are described elsewhere in more detail: β2-sympa- thomimetics (p.88; given by pulmonary, parenteral, or oral route), the methylxanthine theophylline (p.338; given parenterally or orally), and the parasympatholytics ipratropium and tiotropium (p.108).
Spasmolytics. N-butylscopolamine (p.108) is used for the relief of painful spasms of the biliary or ureteral ducts. Its poor absorption (N.B. quaternary N; absorption rate < 10%) necessitates parenteral administration. Because the therapeutic effect is usually weak, a potent analgesic is given concurrently, e.g., the opioid meperidine. Note that some spasms of intestinal musculature can be effectively relieved by organic nitrates (in biliary colic) or by nifedipine (esophageal hypertension and achalasia).
Myometrial relaxants (tocolytics). β2-Sym- pathomimetics such as fenoterol, given orally or parenterally, can prevent premature labor or interrupt labor in progress when dangerous complications necessitate caesarean section. Tachycardia is a side effect produced reflexly because of β2-mediated vasodilation or a direct stimulation of cardiac β1-recep- tors. Recently, atosiban, a structurally altered oxytocin derivative, has become available. It acts as an antagonist at oxytocin receptors, is given parenterally, and lacks the cardiovascular side effects of β2-sympathomimetics, but often causes nausea and vomiting.
Myometrial stimulants. The neurohypophyseal hormone oxytocin (p.238) is given parenterally (or by the nasal or buccal route) before, during, or after labor in order to prompt uterine contractions or to enhance them. Certain prostaglandins or analogues of
them (p.196; F2α, dinoprost; E2, dinoprostone, sulprostone) are capable of inducing rhythmic uterine contractions and cervical relaxation at any time. They are mostly employed as abortifacients (local or parenteral application).
Ergot alkaloids are obtained from Secale cornutum (ergot), the sclerotium of a fungus (Claviceps purpurea) parasitizing rye. Consumption of flour from contaminated grain was once the cause of epidemic poisonings (ergotism) characterized by gangrene of the extremities (St. Anthony’s fire) and CNS disturbances (hallucinations).
Ergot alkaloids contain lysergic acid (see ergotamine formula in A). They act on uterine and vascular muscle. Ergometrine particularly stimulates the uterus. It readily induces a tonic contraction of the myometrium (tetanus uteri). This jeopardizes placental blood flow and fetal oxygen supply. Ergometrine is not used therapeutically. The semisynthetic derivative methylergometrine is used only after delivery for uterine contractions that are too weak.
Ergotamine, as well as the ergotoxine alkaloids (ergocristine, ergocryptine, ergocornine), have a predominantly vascular action. Depending on the initial caliber, constriction or dilation may be elicited. The mechanism of action is unclear; a partial agonism at α-adrenoceptors may be important. Ergotamine is used in the treatment of migraine (p.334). Its derivative, dihydroergotamine, is furthermore employed in orthostatic complaints (p.324).
Other lysergic acid derivatives are the 5-HT antagonist methysergide, the dopamine agonist bromocriptine (p.116), and the hallucinogen lysergic acid diethylamide (LSD, p.236).
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.

Drugs Acting on Smooth Muscle |
131 |
A. Drugs used to alter smooth-muscle function |
|
|||||
Bronchial asthma |
|
Biliary/renal colic |
O2 |
|||
|
|
|
Spasm |
|
|
|
|
|
|
smooth muscle |
|
||
Bronchodilation |
|
Spasmolysis |
Inhibition of labor |
|||
β 2-Sympathomimetics |
N-Butylscopolamine |
β 2-Sympathomimetics |
||||
e.g., fenoterol |
||||||
e.g., salbutamol |
|
|
||||
|
CH3 |
Oxytocin antagonist |
||||
|
|
|
|
|||
|
|
|
|
H3C CH2 CH2 CH2 N+ |
||
|
O |
|
|
Atosiban |
||
H3C |
H |
|
|
|||
|
|
|
|
|||
N |
N |
|
Scopolamine |
|
||
|
|
Induction of labor |
||||
|
|
|
||||
|
|
|
|
|||
O |
N |
N |
|
|
||
|
|
|
||||
|
CH3 |
|
|
Nitrates |
Oxytocin |
|
Theophylline |
|
|
e.g., nitroglycerin |
Prostaglandins |
||
|
|
|
|
|
||
Ipratropium |
|
|
|
F2α , E2 |
||
Secale cornutum |
|
Tonic contraction of uterus |
||||
(ergot) |
|
|
|
|||
|
|
|
|
e.g., ergometrine |
||
|
|
|
|
|
Oxygen supply |
|
|
|
|
|
|
diminished |
|
|
|
|
|
|
Contraindication |
|
Fungus: |
|
|
before delivery |
|||
Claviceps purpurea |
|
Indication: |
||||
|
|
|
|
|
||
|
|
|
|
|
postpartum |
|
|
Secale alkaloids |
|
uterine atonia |
|||
|
|
|
||||
|
Effect on |
|
|
|
||
|
vasomotor tone |
|
|
|||
e.g., ergotamine |
|
|
||||
|
O |
|
|
|
|
|
H |
C |
NH |
R |
|
|
|
|
N |
CH3 |
|
|
|
|
|
|
|
|
|
||
HN |
|
|
|
|
|
|
|
|
|
|
Fixation of lumen at intermediate caliber |
||
Luellmann, Color Atlas of Pharmacology © 2005 Thieme
All rights reserved. Usage subject to terms and conditions of license.
