
- •Preface
- •Content
- •Tissues
- •Nerve Tissue
- •Skin - Epidermis
- •Skin - Dermis
- •Skin - Glands
- •Subcutaneous Layer
- •Skeleton
- •Axial Skeleton
- •Cranium
- •Cranial Bones – Inferior Nasal Concha
- •Vertebral Column
- •Sacrum and Coccyx
- •Ribs
- •Sternum
- •Clavicle
- •Scapula
- •Humerus
- •Ulna
- •Radius
- •Metacarpals and Phalanges
- •Pelvis - Male
- •Femur
- •Tibia
- •Fibula
- •Tarsal Bones - Cuboid and Navicular
- •Phalanges
- •Patella
- •Skeletal Muscles
- •Transversospinales Muscles
- •Cervical Hypaxial Muscles
- •Thoracic and Abdominal Hypaxial Muscles
- •Shoulder Muscles - Rotator Cuff
- •Shoulder Muscles - Prime Movers
- •Anterior Brachial Muscles
- •Posterior Brachial Muscles
- •Posterior Thigh Muscles
- •Thigh Muscles
- •Lateral Leg Muscles
- •Posterior Leg Muscles
- •Spinal Nerves
- •Dorsal Rami
- •Intercostal Nerves
- •Cutaneous Nerves
- •Autonomic Nerves
- •Spinal Cord
- •Brain
- •Cerebrum
- •Cerebellum
- •Meninges
- •Hypothalamus
- •Pituitary Gland
- •Pineal Gland
- •Thymus
- •Pancreas
- •Ovaries
- •Testes
- •Blood
- •Heart
- •Lymphatics
- •Larynx
- •Lungs
- •Cast of Trachea and Bronchial Tree
- •Esophagus
- •Stomach
- •Pancreas
- •Large Intestine
- •Mesenteries
- •Omenta
- •Female Reproductive Organs
- •Ovary
- •Vagina
- •Ductus Deferens and Spermatic Cord
- •Penis
- •Index
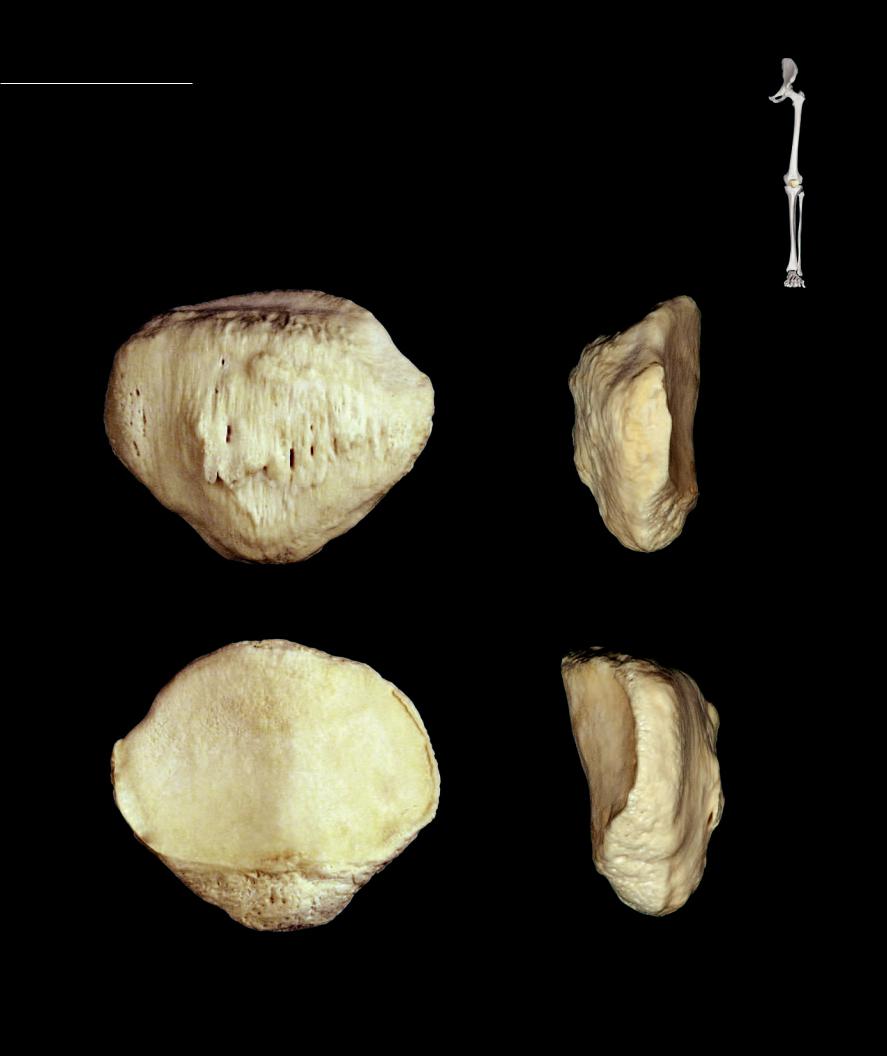
Patella The patella is the largest sesamoid bone of the body. A sesamoid bone is a bone that forms within a tendon. The patella occupies the posterior half of the quadriceps tendon just anterior
to the knee joint. It is a disc-like bone with a curved superior margin and a triangular inferior border. The posterior surface of the bone is smooth and articulates with the femur, while the anterior surface of the bone is rough by its attachment to the quadriceps tendon.
1 Base
2 Apex
3 Articular surface
4 Anterior surface
1
1
3
4 |
4 |
2
2
1
3
4
3 |
3 |
2
2
122
7 Articular System
Joints, simply defined, are the meeting places between bones. This simple definition describes a joint as any place
in the skeleton where one skeletal element contacts another skeletal element. It is important to understand that, as a part of this definition, the bones never contact each other directly. Instead, there is al-
ways some other connective tissue between the bony contact surfaces. Joints come in a wide variety of structural junctions, with an accompanying variety of functions.
Because joints have various functions and those functions do not always deal with movement, it is illogical to define joints by their movements. The best method for classifying joints is based on their structure. Because the structure of joints includes the connective tissues between the neighboring bones, a classification based on the structure of those tissues
is logical. At the simplest level, there are two basic ways bones connect with one another to form joints. Either they are connected by solid masses of connective tissue, or they are bound together by a connective tissue capsule, which surrounds a lubricated cavity between the adjoining bones.
Joints formed by a solid core of connective tissue between the neighboring bones are called synarthroses. There are two subcategories of synarthroses — fibrous joints, which have connective tissue cores of connective tissue proper, typically dense irregular connective tissue, and cartilage joints, which use some form of cartilage as the connecting tissue between the bones. The capsular joints, with their lubricated cavity, are called diarthroses or synovial joints. There are numerous subcategories of diarthroses, each
based on the structure and function of their articular surfaces.
In addition to joints, this chapter will also illustrate other closely related synovial structures — bursae and synovial (tendon) sheaths.
Find more information about arthrology in
R E A L A N AT O M Y
123
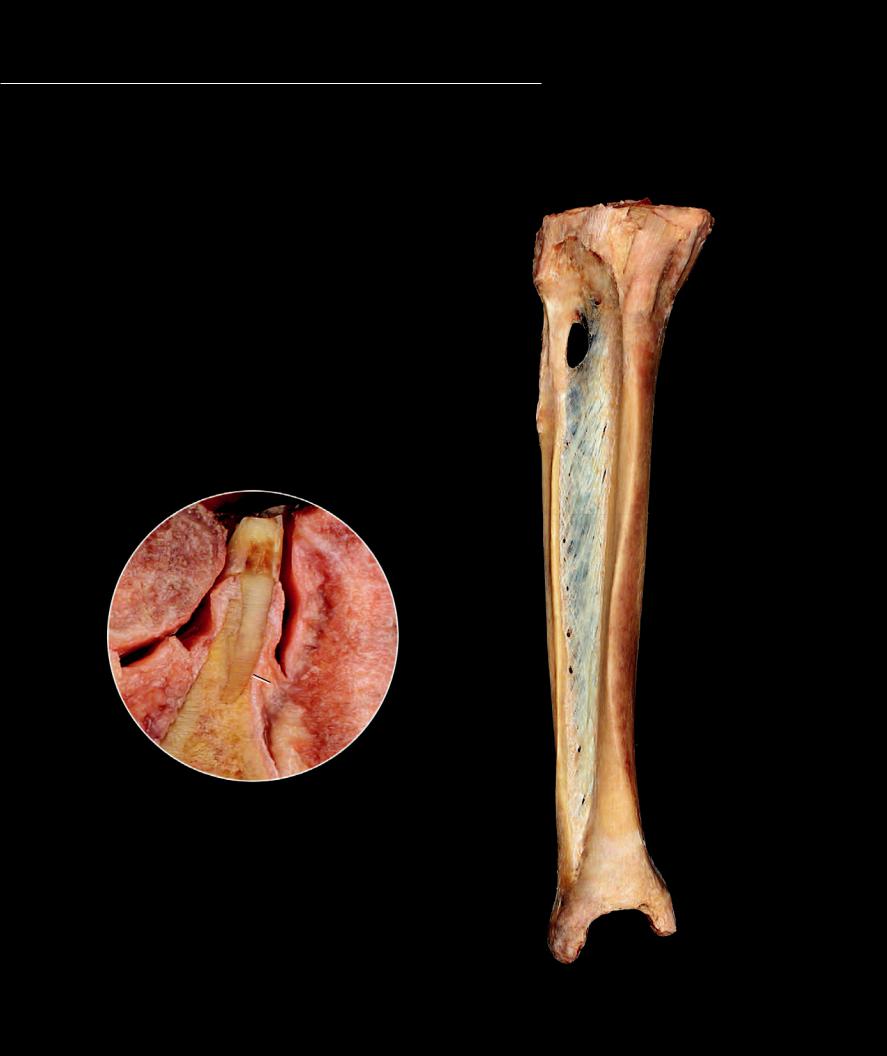
Fibrous joints are synarthrotic joints that bind bone to bone with collagenous connective tissue. The amount of connective
tissue binding the neighboring bones can vary considerably. Examples of fi brous joints are depicted on this and the facing page. Gomphoses and sutures (the four different suture types are shown on the opposite page) have a very thin membrane of collagenous connective tissue anchoring neighboring bony structures to one another. On the other hand, the syndesmoses between the tibia and fi bula — both the interosseous membrane and the tibiofi bular ligaments at the distal end — have considerably more binding connective tissue. There is also an example of another syndesmosis, the interspinous ligament, in the next section.
1 |
Periodontal membrane |
10 |
2 |
Crown of tooth |
|
3 |
Root of tooth |
|
4 |
Gingiva |
|
5 |
Mandible |
|
6 |
Tibia |
|
7 |
Fibula |
|
8 |
Interosseous membrane |
|
9 |
Anterior tibiofibular ligament of tibiofibular syndesmosis |
|
10 |
Patellar ligament (cut) |
|
7
6
8
2
4
3
1
5
Dento-alveolar syndesmosis or gomphosis
Sagittal section of tooth in mandible
9
Crural skeleton – tibia and fibula
Anterior view
124
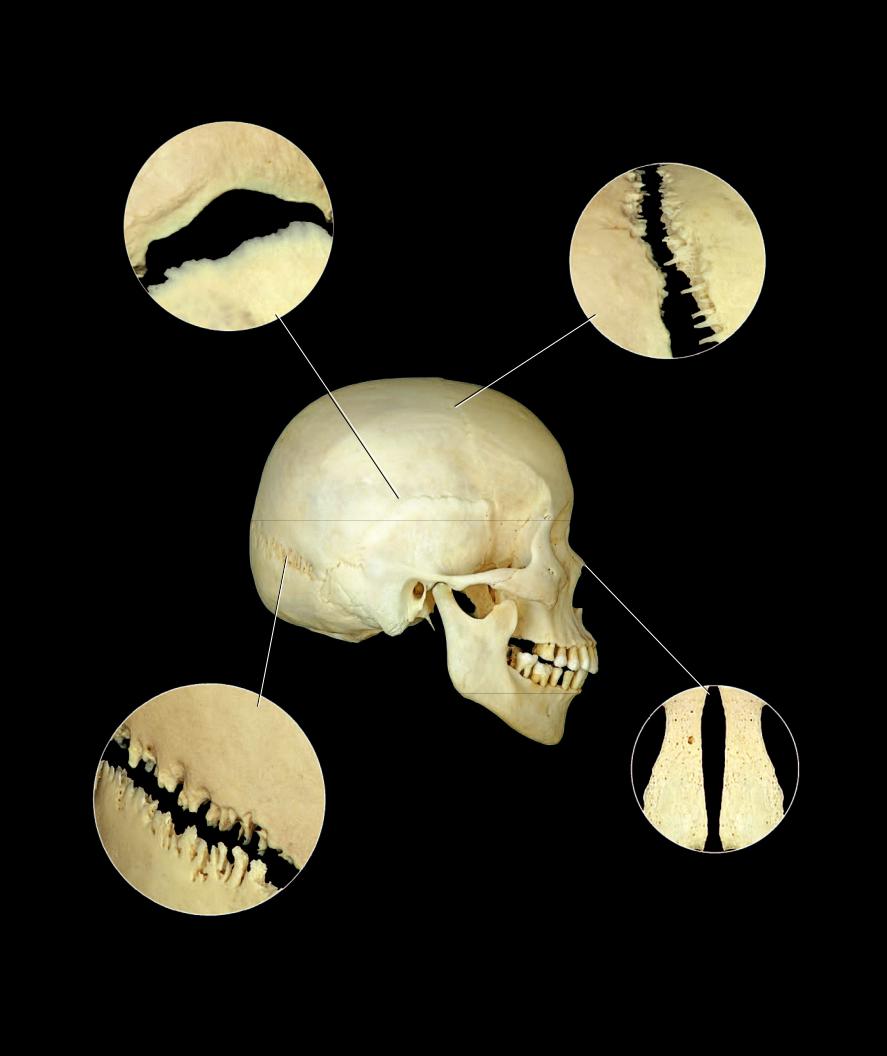
Squamous-type suture
Squamous or temporoparietal suture
Serrate-type suture
Coronal or frontoparietal suture
Plane-type suture
Internasal suture
Denticulate-type suture
Lamboidal or parieto-occipital suture
125
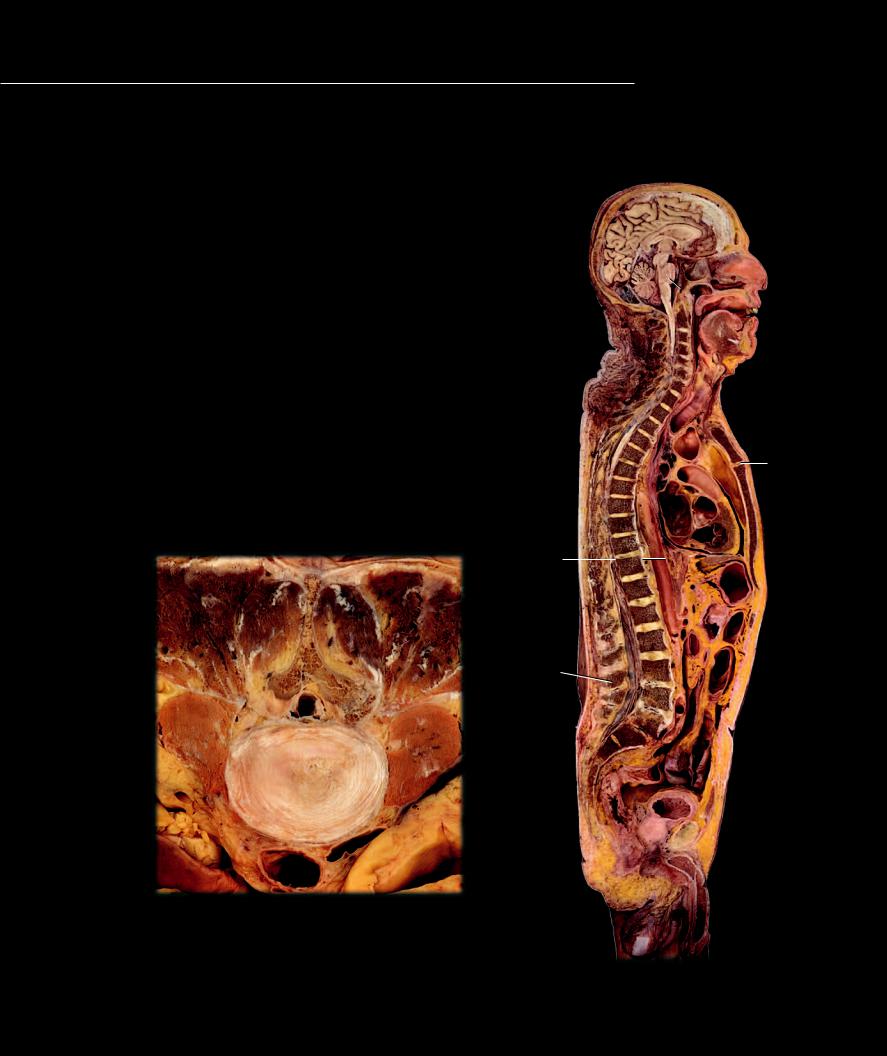
Like the fi brous joints, the cartilaginous joints join neighboring skeletal ele-
ments with a solid mass of connective tissue, but the uniting tissue is some type of cartilage instead of collagenous connective tissue proper. The three types of cartilaginous joints are: 1) synchondroses, 2) symphyses, and 3) epiphysial cartilages or primary cartilaginous joints. The photos on these facing pages depict the different categories of cartilaginous joints. A few syndesmoses from the fibrous joint category are also evident.
1 Intervertebral disc (symphysis)
2 Nucleus pulposus of intervertebral disc
3 Anulus fibrosus of intervertebral disc
4 Pubic symphysis
5 Manubriosternal synchondrosis
6 Spheno-occipital synchondrosis
7 Epiphysial cartilage or primary cartilaginous joint
8 Sternocostal (synchondrosis)
9 Sternocostal (typically synovial but can be symphysial)
10Interchondral (synovial)
11Interchondral (synchondrosis)
12Costochondral (synchondrosis)
13Interspinous ligament (vertebral syndesmosis)
14Nuchal ligament (vertebral syndesmosis)
15Anterior longitudinal ligament (vertebral syndesmosis)
16Posterior longitudinal ligament (vertebral syndesmosis)
17Body of vertebra
18Spinous process of vertebra
19Lamina of vertebra
20Psoas major muscle
21Aorta
22Inferior vena cava
18
19
20
2
3
22
21
Transverse section of lumbar intervertebral disc
Inferior view
126
6
14
5
16 |
|
15 |
|
17
1
18  13
13
4
Sagittal section of head and trunk
Medial view

7
7
Fetal skeleton
Posterior view
Epiphysial cartilage
200x
8
9
9
12
9
9
9
10
10
11
1
1
Radiograph of juvenile wrist region
Anterior view
Joints of the thoracic cage
Anterior view
127
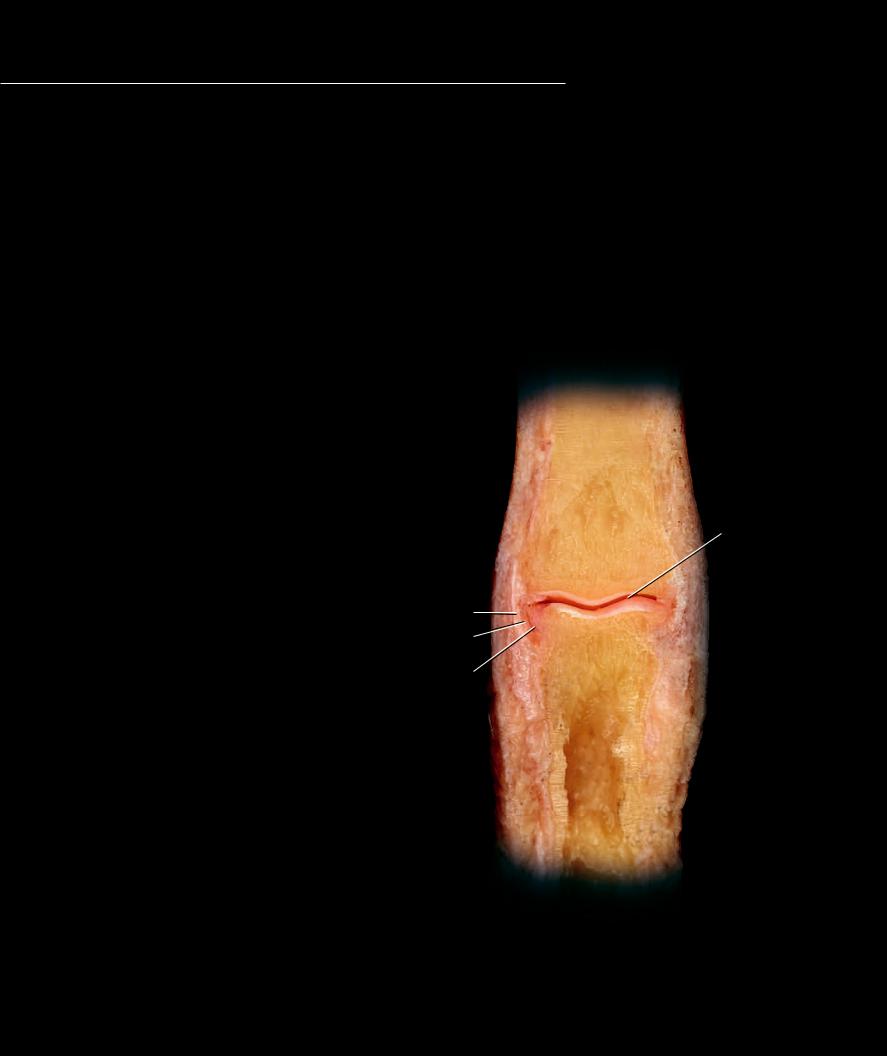
Diarthroses differ from synarthroses in one major way: instead of connecting neighboring bones by a solid mass
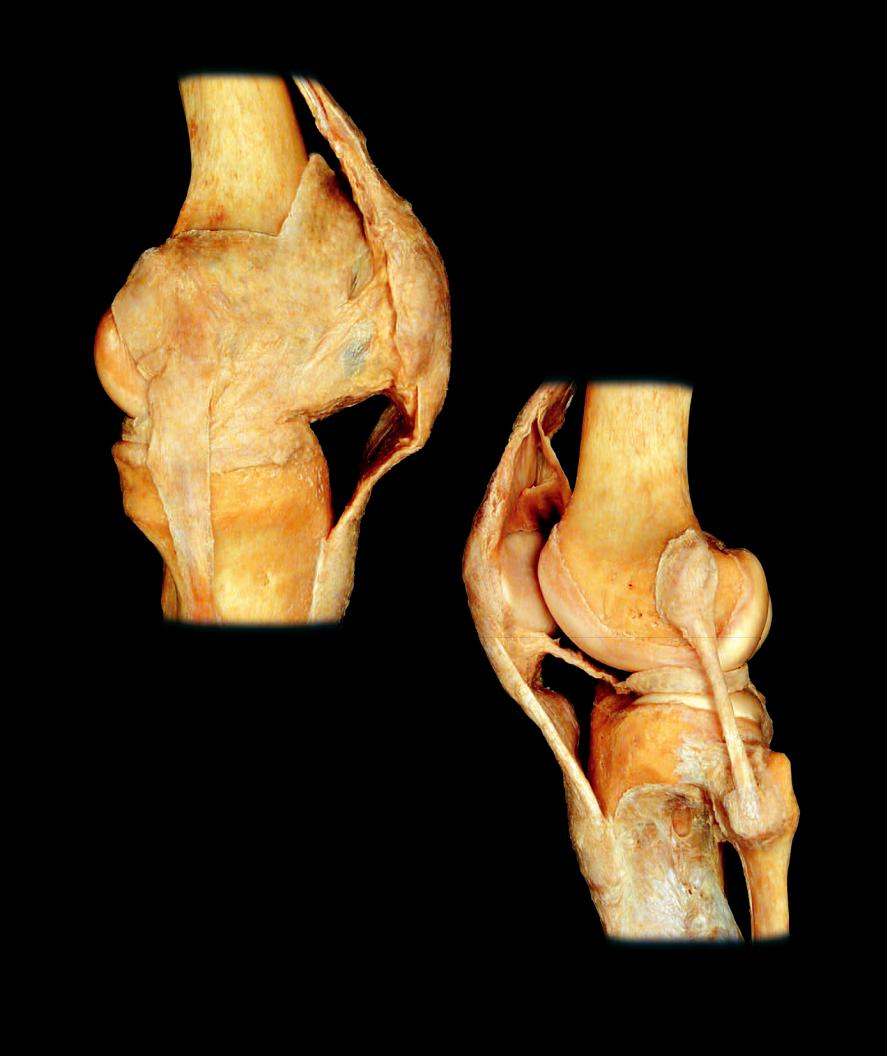
of connectve tissue, the bony connection consists of a double-layered connective tissue capsule that surrounds a lubricated cavity between the bones. Within the capsule the ends of neighboring bony surfaces are covered by a smooth layer of hyaline cartilage. As a result of this design there is typically a much greater range of motion present in synovial joints, and they form the joints of the skeleton that are responsible for the major movements of the body. The outer layer of the capsule, the fi brous membrane, is continuous with the periosteum on the adjoining bones, while the inner layer of the capsule, the synovial membrane, attaches from the border of the articular cartilage on one bone to the border of the articular cartilage on the other bone. Additionally, the synovial membrane secretes synovial fl uid, a lubricant that reduces friction between the mobile cartilage-covered articular surfaces of the bones. The section through a fi nger joint below and the dissections of the knee joint on the opposite page illustrate the basic features of a synovial joint. The pages that follow depict the major synovial joints of the skeleton. One other key feature among synovial joints that is responsible for their varied range of motion is the shape of the adjoining bone surfaces. It is this feature that anatomists use to describe the different types of synovial joints.
1 |
Middle phalanx of index finger |
|
|
2 |
Proximal phalanx of index finger |
|
|
3 |
Fibrous membrane of joint capsule |
|
|
4 |
Synovial membrane of joint capsule |
|
|
5 |
Articular cartilage |
|
|
6 |
Joint cavity |
|
|
7 |
Collateral ligament |
|
|
8 |
Quadriceps tendon |
|
|
9 |
Patellar ligament |
|
|
10 |
Suprapatellar bursa |
1 |
|
11 |
Synovial fold |
||
12 |
Meniscus |
|
|
13 |
Periosteum |
6 |
|
14 |
Junction of periosteum (removed) with fibrous membrane |
||
|
|||
15 |
Junction of synovial membrane (removed) with articular cartilage |
|
|
16 |
Femur with periosteum removed |
|
|
17 |
Tibia with periosteum removed |
|
|
18 |
Fibula with periosteum removed |
5 |
|
19 |
Patella within quadriceps tendon |
||
|
|
7 |
|
|
|
3 |
4
2
Proximal interphalangeal joint showing design of synovial joint
Frontal section, anterior view
128
16
8
14
19
3
|
9 |
|
7 |
14 |
10 |
|
|
4 |
|
17 |
|
|
|
5 |
|
|
5 |
|
|
15 |
Dissection of knee showing design of synovial joint |
11 |
|
|
Medial view |
|
12
7 5
15
18
13
Dissection of knee showing design of synovial joint
Lateral view
129
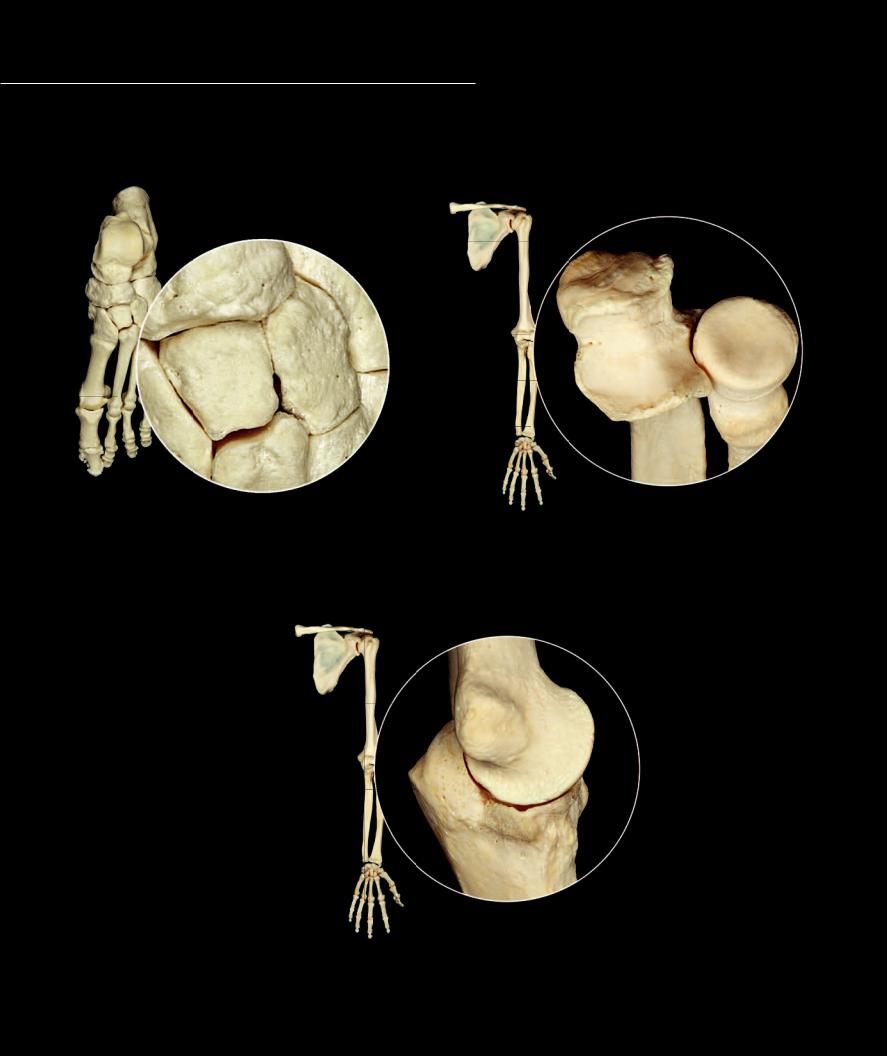
There are seven types of synovial joints in the body. Each of the different synovial joints has the basic structural features common to all synovial joints but is
further classified based on the shape of and motion that occurs at the articular surfaces of the joint. The different types of synovial joint are depicted below and on the opposite page. Note the shapes of the reciprocal surfaces as you study these photos.
Plane joint examples |
|
|
Intertarsal joints |
|
Pivot joint examples |
|
|
Proximal radio-ulnar joint of elbow |
|
|
|
Hinge joint example
Humero-ulnar joint of elbow
130
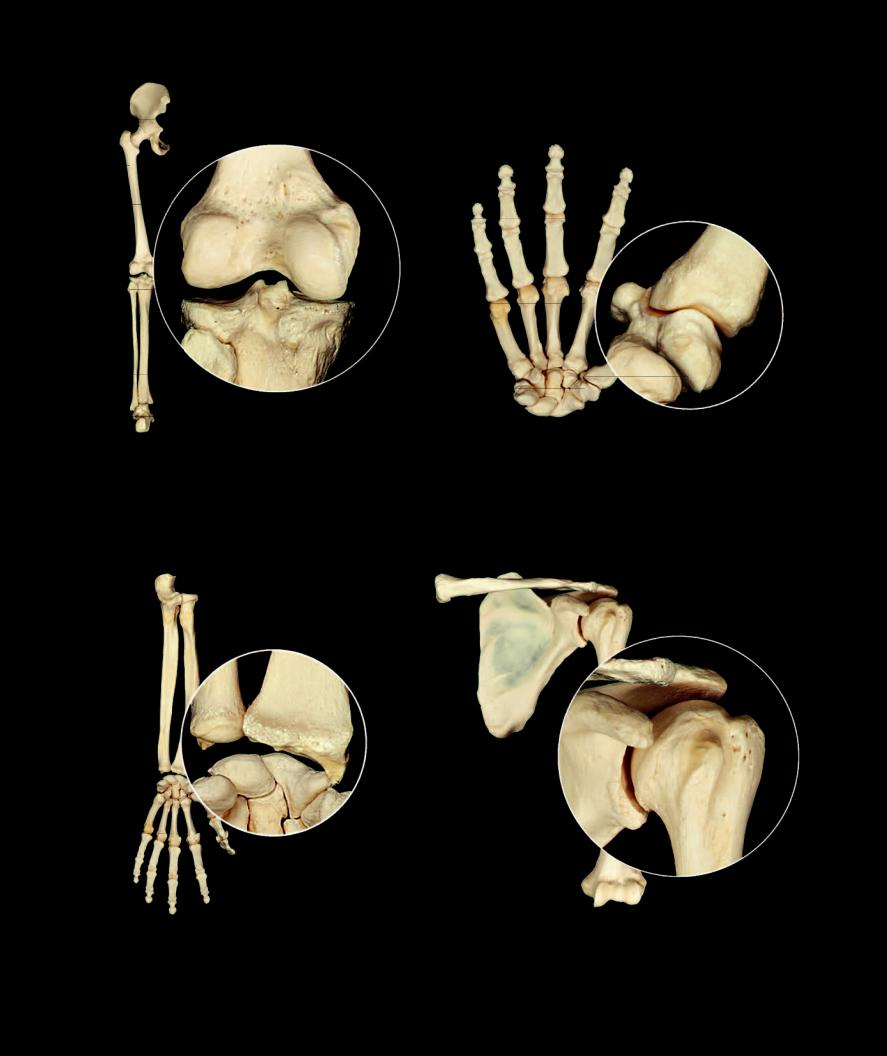
Bicondylar joint example |
Saddle joint example |
Metacarpal-carpal joint of thumb |
|
Knee joint |
|
Condylar joint example |
Ball and socket joint example |
|
Shoulder joint |
||
Wrist joint |
||
|
131
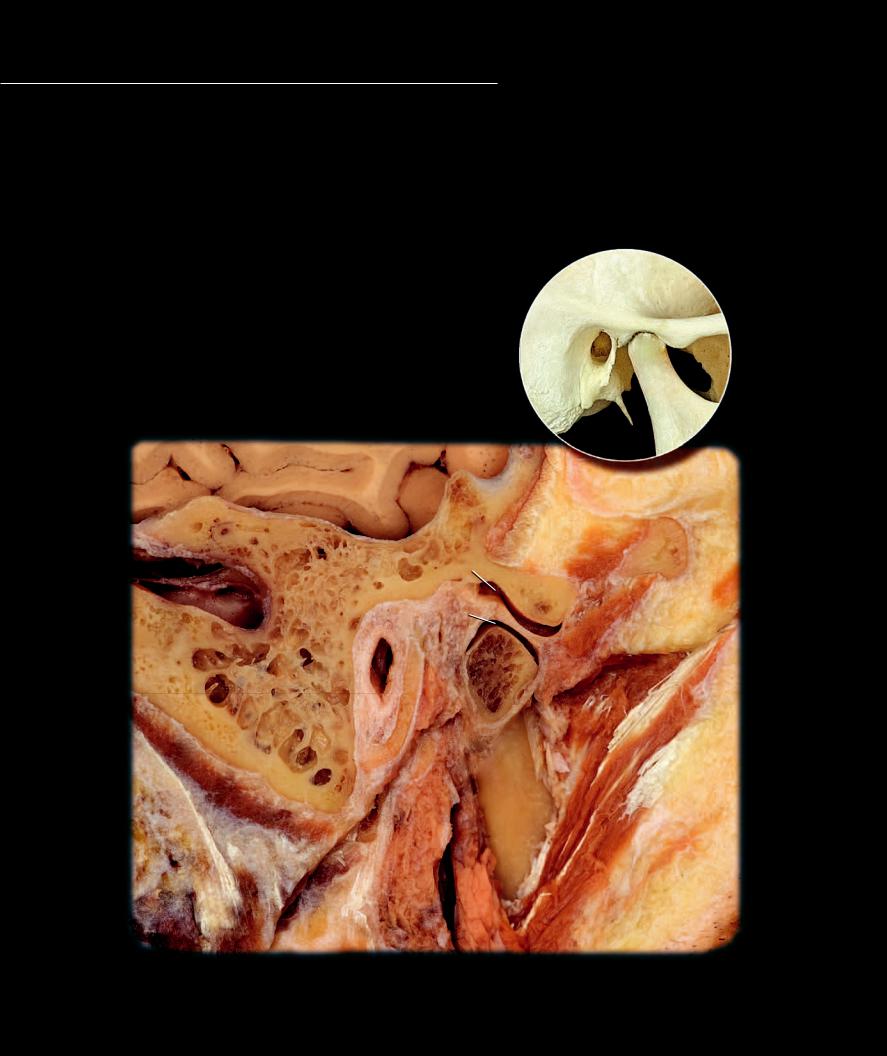
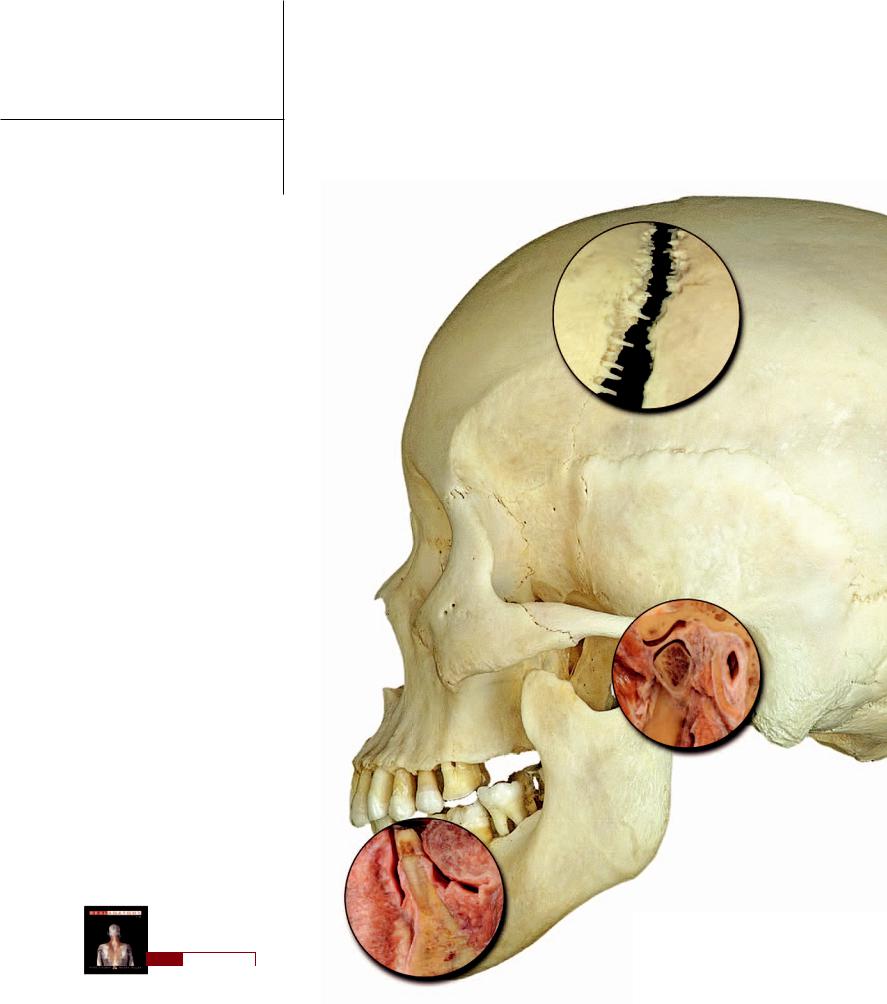
The complex temporomandibular joint differs from other synovial joints by having an articular disc that usually separates the joint into two separate
synovial capsules, one above and one below the disc. The articular surfaces have a covering of dense fi brocartilage rather than the typical hyaline cartilage of most synovial joints. With its associated ligaments this joint structure accounts for the complex series of movements that are essential during the activities of eating and speech. Each temporomandibular joint is a condylar joint and both joints together form a bicondylar joint. The fi brous membrane of the articular capsule spans from temporal bone to mandible only on the lateral side. Anteriorly, medially, and posteriorly the fi bers attach from mandible and temporal bone to the articular disc. Extrinsic ligaments that help stabilize the joint are the lateral temporomandibular ligament, sphenomandibular ligament, and stylomandibular ligament.
1 |
Mandibular condyle |
8 |
Articular disc |
2 |
Mandibular ramus |
9 |
Joint (articular) capsule |
3 |
Articular tubercle of temporal bone |
10 |
Masseter muscle |
4 |
Mastoid process of temporal bone |
11 |
Parotid gland |
5 |
Mastoid air cells |
12 |
Brain |
6 |
Superior compartment of articular cavity |
13 |
External acoustic meatus |
7 |
Inferior compartment of articular cavity |
14 |
Sigmoid venous sinus |
12 |
Bones of temporomandibular joint |
|
|
|
Lateral view |
6 |
|
14 |
|
7 |
3 |
|
8 |
13 |
9 |
|
1 |
5
4
2
10
11
Section of right temporomandibular joint
Lateral view of sagittal section
132
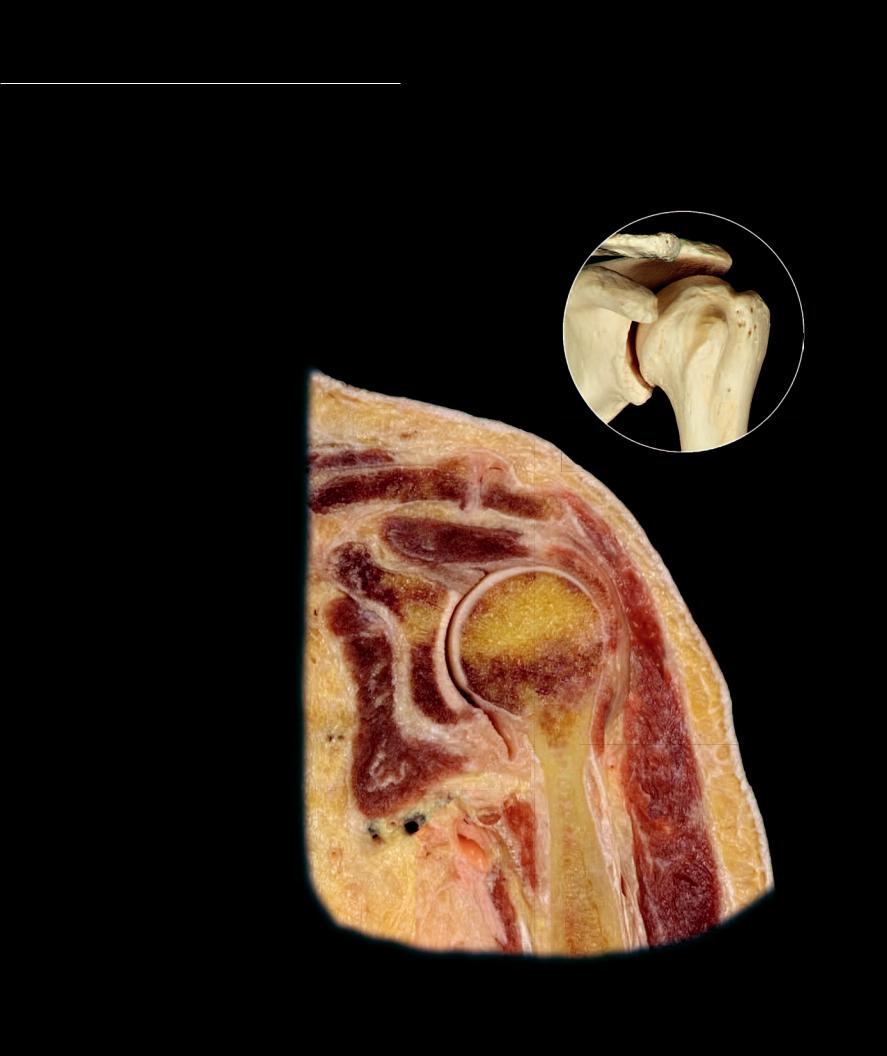
The glenohumeral or shoulder joint is a ball and socket joint and is the most mobile joint in the body. The tremendous range of motion at this joint is the result of few external ligaments that present little
limitation to movement, and shallow, ovoid articular surfaces that make movements in all planes of space possible. In fact, surrounding muscles and tendons play a more signifi cant role in joint support than do the joint structures. The capsular ligament is extremely lax, providing limited support to the joint. Blending with the capsule are the tendons of four muscles. Together the capsule and tendons form the rotator cuff, which is the major support structure of the joint.
1 Articular cartilage
2 Synovial membrane
3 Fibrous membrane
4 Glenoid labrum
5 Acromioclavicular ligament
6 Clavicle
7 Humerus
8 Glenoid of scapula
9 Acromion of scapula
10Supraspinatus muscle
11Subscapularis muscle
12Deltoid muscle
13Tendon of long head of biceps brachii
14Skin
15Subcutaneous layer
|
5 |
Bones of glenohumeral joint |
|
|
|
||
6 |
|
Anterior view |
|
|
|
9 |
|
|
10 |
|
|
|
|
13 |
|
|
4 |
|
|
8 |
1 |
|
|
|
7 |
|
|
|
|
|
|
|
1 |
|
|
|
|
12 |
14 |
11
2
4 3
15
Section of left glenohumeral joint
Anterior view of frontal section
133
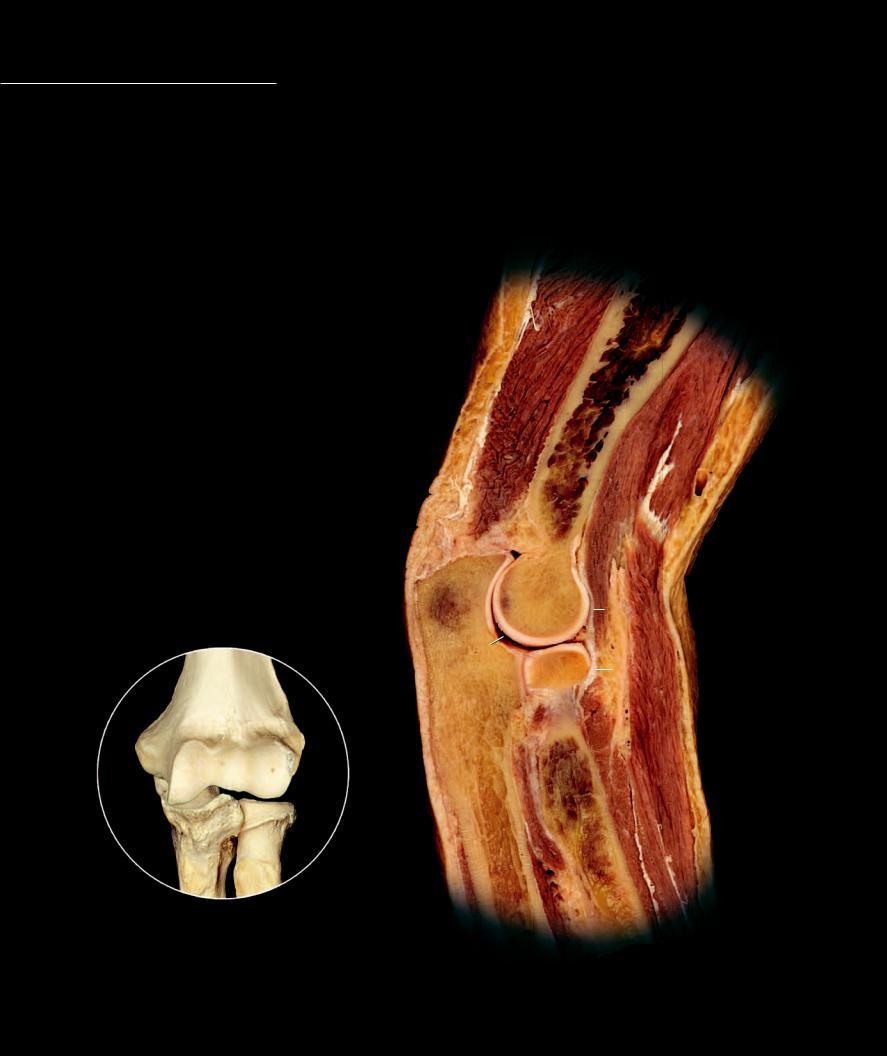
The elbow joint is a complex joint comprised of multiple articular surfaces within one articular capsule. The elbow joint can be subdivided into three distinct articular interfaces — the humero-ulnar joint (hinge), the humeroradial joint (combined hinge and pivot), and
the proximal radioulnar joint (pivot). Two distinct pairs of movements occur as a result of the articulations within the elbow joint — the hinged movements of fl exion and extension, and the rotational movements of pronation and supination. Unlike the shoulder joint, the joints fo the elbow have strong extrinsic ligaments that limit movemnts and stabilize the articulating bones. The fi brous capsule is thin anteriorly and posteriorly, allowing for free range of motion during fl exion and extension. On either side the capsule is reinforced by strong extrinsic ligaments, the ulnar collateral and radial collateral ligaments. Wrapping from the back of the ulna at the base of the olecranon to the front of the ulna at the lateral surface of the coronoid process is the semicircular anular ligament. With the radial notch of the ulna this ligament forms a fi bro-osseous ring for the pivoting action of the radial head.
1 |
Articular cartilage |
|
|
|
2 |
Joint (articular) capsule |
|
|
|
3 |
Articular (synovial) cavity |
|
|
|
4 |
Capitulum of humerus |
|
|
|
5 |
Olecranon of ulna |
|
|
|
6 |
Head of radius |
|
|
|
7 |
Anular ligament |
10 |
8 |
|
8 |
Biceps brachii muscle |
|||
|
||||
|
|
|||
9 |
Brachialis muscle |
|
|
10Triceps brachii muscle
11Brachioradialis muscle
9
4 |
|
|
|
|
|
|
5 |
|
|
|
2 |
|
|
|
|
|
||||
1 |
1 |
|
|
|
|
|
3 |
|
|
|
|
|
|
6 |
|
|
7 |
11 |
||
|
||||||
|
|
|
|
|
|
|
Bones of elbow joint
Anterior view
Section of pronated left elbow joint
Medial view of sagittal section
134
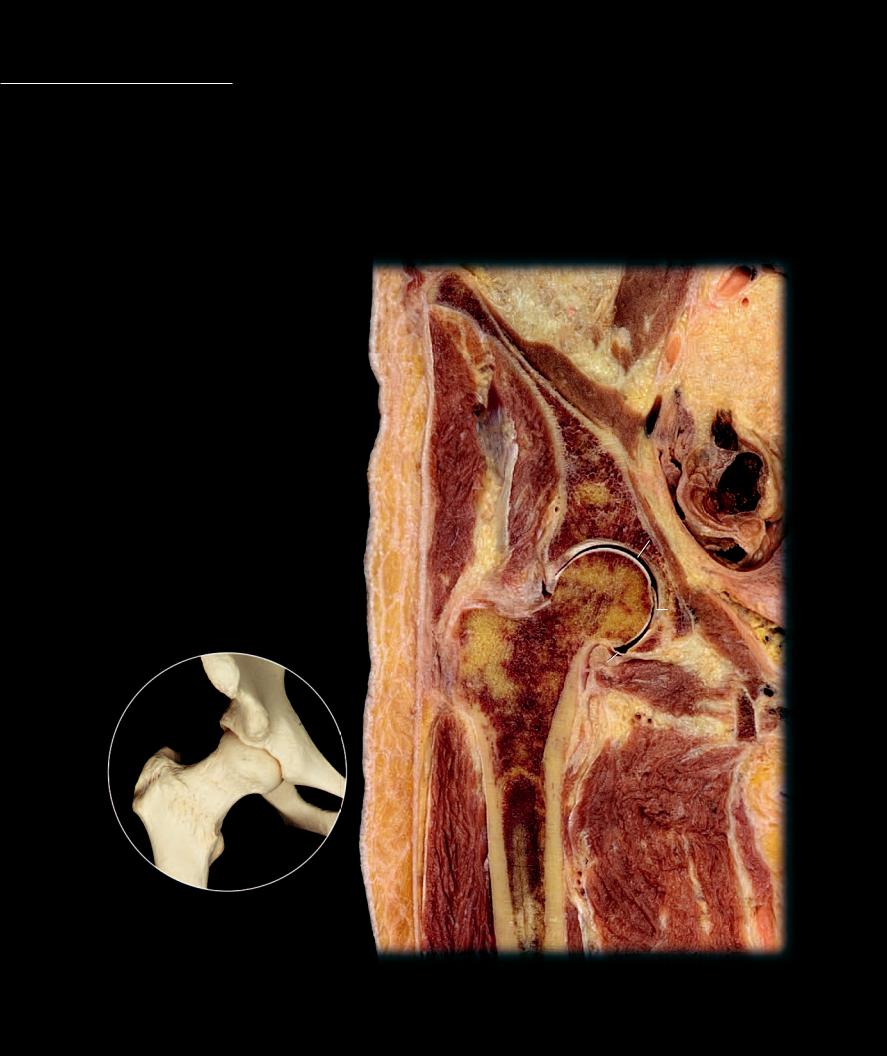
Like the shoulder joint the hip joint, also a ball and socket joint, allows for great freedom of motion, although the range of motion is not quite as great as that of the shoulder. This comparative decrease in mobility results from the deep hip socket with its extended labrum, which almost
completely engulfs the head of the femur. In addition, thick extrinsic ligaments tightly surround the joint to form a strong, reinforced capsule. The three major ligaments of the hip joint, the iliofemoral, pubofemoral, and ischiofemoral, form a sheath around the fi brous capsule. The iliofemoral ligament is argued to be the strongest ligament in the human body. Often called the Y-shaped ligament it passes superior and anterior to the joint, running from the anterior inferior iliac spine to the intertrochanteric line. With the thinner pubofemoral and ischiofemoral ligaments it spirals around the joint to stabilize this powerful joint. In additon to these large ligaments, a triangular fl at band, the ligament of the head of the femur, extends from the fovea of the femoral head to the margins of the acetabular fossa. This ligament is also important because it functions as a pathway for blood vessels that supply the bone tissue in the head of the femur.
1 Ligament of head of femur
2 Joint (articular) capsule
3 Articular cartilage of acetabulum
4 Articular cartilage of femur
5 Articular (synovial) cavity
6 Acetabular labrum
7 Fovea capitis of femur
8 Head of femur
9 Greater trochanter of femur
10Os coxae
11Psoas major muscle
12Iliacus muscle
13Adductor muscles
14Vastus lateralis muscle
15Gluteus medius muscle
16Gluteus minimis muscle
17Obturator internus muscle
18Obturator externus muscle
19Skin
20Subcutaneous layer
21External iliac artery
22Intestine
Bones of hip joint
Anterior view
21
11
|
|
12 |
|
15 |
|
|
|
16 |
|
10 |
22 |
|
|
||
|
|
|
5 |
|
3 |
4 |
|
|
|
|
|
19 |
6 |
|
|
|
|
|
|
|
|
8 |
7 |
|
|
|
|
1 |
|
|
|
||
|
9 |
17 |
||
|
|
|
|
|
20 |
|
2 |
|
|
|
18 |
|||
|
|
|||
14
13
Section of right hip joint
Anterior view of frontal section
135
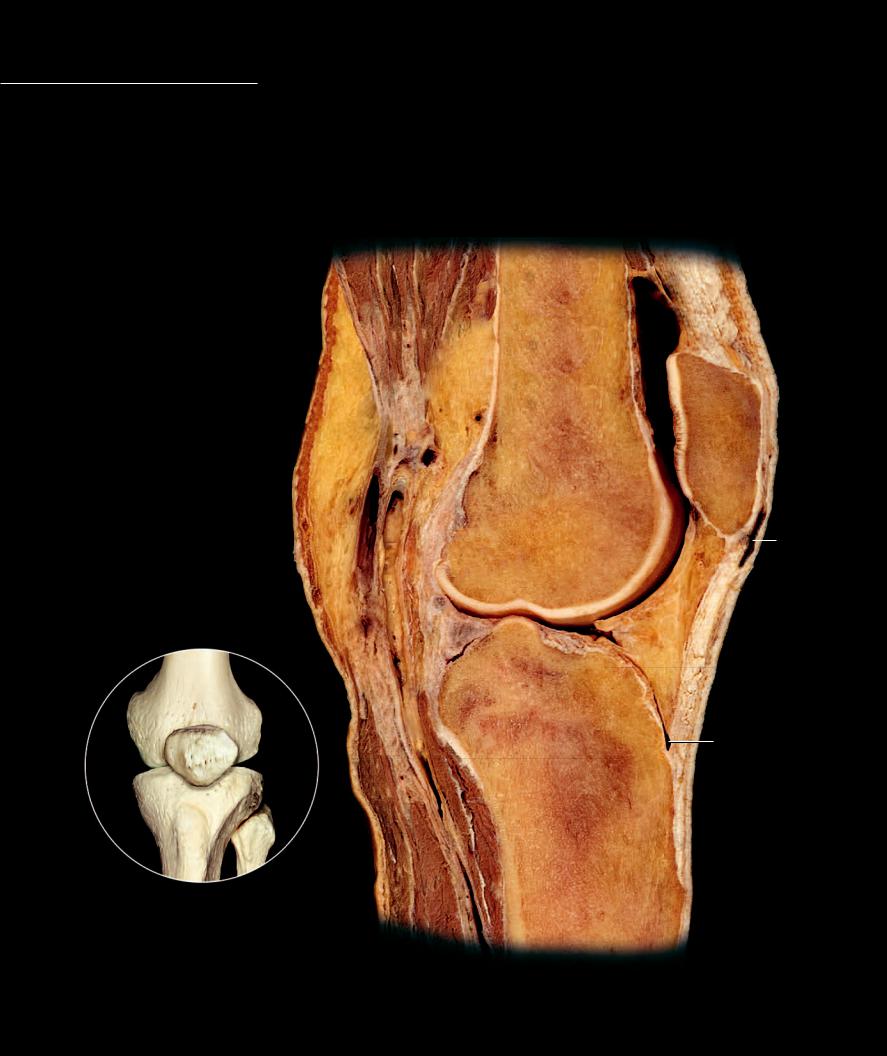
The knee joint is a combined bicondylar and saddle joint. The relationships between the femur and the tibia provide no interlocking joint mechanisms or stability between the neighboring bones, and from this perspective the knee joint is completely unstable. The strength
of the knee joint is dependent on strong ligaments and surrounding muscles. Although its primary motions are of a hinge nature, it is a complex joint with subtle rotational and sliding movements also. The major stabilizers of the joint are four strong ligaments. Two collateral ligaments support the joint on either side, while two cruciate ligaments criss-cross through the middle of the joint. The tibial or medial collateral ligament is a strong, fl at band that stretches from the femoral epicondyle to the tibial condyle. Posteriorly it fi rmly attaches to the joint capsule and the medial meniscus, while anteriorly bursae separate it from these structures. The fi bular or lateral collateral ligament is a strong cord that runs from the lateral femoral
1 |
Articular (synovial) cavity |
|
|
|
|
|
2 |
Articular cartilage |
|
|
|
|
|
3 |
Medial meniscus |
|
|
|
|
|
4 |
Suprapatellar bursa |
|
|
|
|
|
5 |
Prepatellar bursa |
|
|
17 |
|
|
6 |
Infrapatellar bursa |
|
4 |
|
|
|
7 |
Infrapatellar fat pad |
|
|
|
|
|
8 |
Fibrous membrane of joint capsule |
|
22 |
|
|
|
|
|
|
|
|
||
9 |
Synovial membrane of joint capsule |
|
|
|
|
|
10 |
Lateral meniscus |
23 |
|
|
|
|
11 |
Fibular collateral ligament |
|
9 |
|
|
|
12 |
Tibial collateral ligament |
|
2 |
|
|
|
13 |
Anterior cruciate ligament |
|
|
|
|
|
14 |
Posterior cruciate ligament |
26 |
18 |
|
|
|
15 |
Oblique popliteal ligament |
|
|
|
|
|
16 |
Patellar ligament |
|
|
21 |
|
|
17 |
Quadriceps tendon |
|
|
|
|
|
|
|
|
|
|
||
18 |
Femur |
|
|
|
|
|
19 |
Tibia |
|
|
|
|
|
20 |
Fibula |
|
|
|
|
|
21 |
Patella |
|
|
|
|
|
22 |
Periosteum |
|
|
|
|
|
23 |
Semimembranosus muscle |
|
|
|
|
5 |
24 |
Gastrocnemius muscle |
|
|
8 |
|
|
|
|
|
|
|||
25 |
Soleus muscle |
|
|
|
|
|
26 |
Popliteal fat |
|
|
|
|
|
|
|
|
2 |
|
|
|
3 |
1 |
16 |
|
7 |
|||
|
|||
|
|
6
19
24
Bones of knee joint |
25 |
Anterior view |
|
Section of right knee joint
Lateral view of sagittal section
136
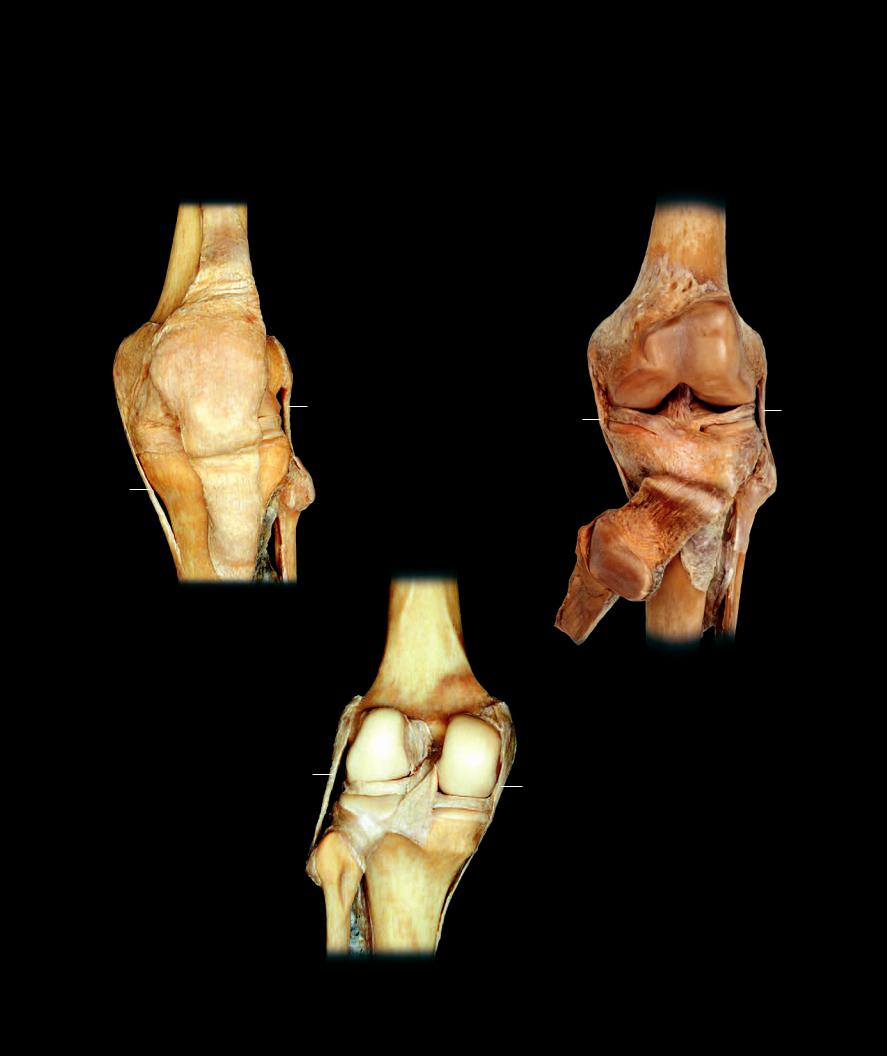
epicondyle to the head of the fi bula. Unlike the tibial collateral ligament it does not attach to the lateral meniscus or joint capsule. The cruciate ligaments stabilize the knee from excessive anterior-posterior and rotational movements. The anterior cruciate ligament ascends posterolaterally from the medial aspect of the intercondylar area to the medial aspect of the lateral condyle of the femur. The shorter posterior cruciate ligament ascends from the posterior intercondylar area to the medial femoral condyle. Both cruciates have fi bers that blend with the lateral meniscus. In additon to these ligamentous structures, two semilunar menisci project into the capsule between the femoral condyles and the articular plateaus of the tibia. The large, extensive articular capsule connects the femur, patella, and tibia.
18
17
18
8 |
|
|
|
|
|
|
|
|
|
|
2 |
|
|
|
|
||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||
|
|
|
|
|
11 |
|
|
|
|
|
13 |
1 |
10 |
|
11 |
||
|
|
|
|
|
|
|
|
|
|
||||||||
|
|
|
10 |
|
|
|
|
|
12 |
|
3 |
|
|||||
|
|
|
|
|
|
|
|
|
|
|
|
||||||
|
|
|
|
|
|
|
|
|
|
|
|
||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
3 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||
12 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
19 |
16 |
|
|
|
|
|
|
|
|
16 |
|
20 |
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||||
|
|
|
20 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
22 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
21 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
19 |
|
|
|
|
|
|
Dissection of left knee joint |
|
17 |
|
|
|
|
|
|||||||||
|
|
Anterior view |
|
|
|
|
|
|
|
|
|
|
|||||
|
|
|
|
|
|
|
|
18 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Dissection of left knee joint |
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
Anterior view |
|
|
|
|
|
|
|
|
|
|
|
|
13 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
2 |
|
|
|
|
|
|
|
|
|
|
|
11 |
|
|
14 |
|
|
12 |
|
|
|
|
|
|
||
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||
|
|
|
10 |
15 |
3 |
|
|
|
|
|
|
|
|||||
|
|
|
|
|
|
|
|
|
|
||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||
20
19
Dissection of left knee joint
Posterior view
137

A synovial bursa is a small sac-like structure interposed between structures that generate significant amounts of friction.
Bursae have a similar design to the articular capsule of a synovial joint. These small bags have an outer fi brous membrane of dense irregular collagenous connective tissue and an inner lining of synovial membrane. The synovial membrane produces a small amount of synovia as a lubricant inside the sac. The fi brous membrane binds to surrounding tissues, allowing the juxtaposed walls of synovial membrane to rub together in a frictionless manner. Many bursae arise as outgrowths of synovial joint cavities. In some cases these pinch off from the joint forming sacs that are independent from the joint, while other bursal sacs retain their connections with the joint cavity. A synovial sheath is a modifi ed bursa that wraps around a tendon to protect it from friction on all sides. In the tight confines of the wrist, ankle, and digits, tendons often pass beneath fi brous bands called retinacula. The retinaculum is a connective tissue band that crosses over the tendons and keeps them from being displaced upward when the muscle shortens and bends the joints. Because the retinaculum and bone create a fi broosseous tunnel around the tendon, considerable friction can occur on all surfaces of the tendon at these locations. As the tendon moves through the tunnel, the juxtaposed synovial membranes smoothly glide over each other with minimal friction.
1 |
Suprapatellar bursa |
|
2 |
Prepatellar bursa |
|
3 |
Infrapatellar bursa |
|
4 |
Synovial (tendon) sheath |
|
5 |
Retinaculum |
|
6 |
Flexor digitorum superficialis tendon |
1 |
7 |
Flexor digitorum profundus tendon |
|
8 |
Lumbrical muscles |
|
9 |
Flexor digiti minimi brevis muscle |
|
10 |
Abductor digiti minimi muscle |
|
2
7
3
6
5
Synovial bursae around the knee joint
Medial view of sagittal section
88
4
9
10
Tendon sheath of fingers
Anterior view, pin inserted into tendon sheath
138
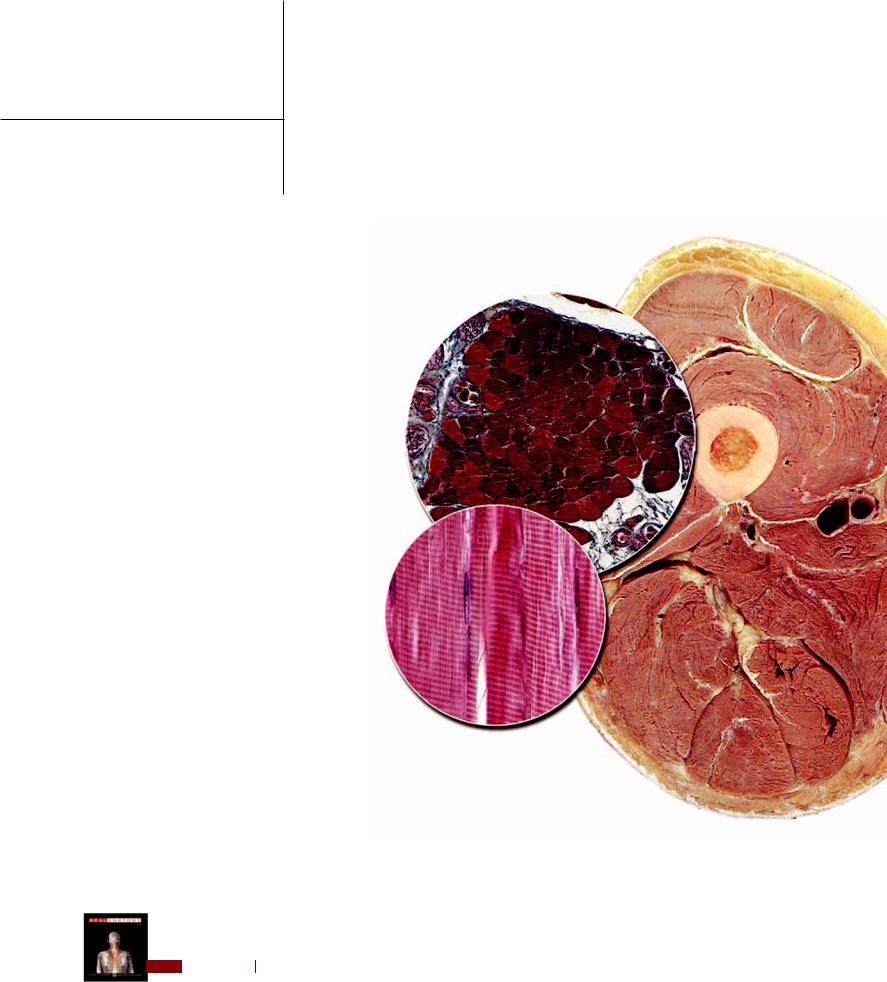
8 Muscular System
Bodies are designed to move! We move when we walk, jog, or run, activities that transport our bodies from one location to another. In addition to moving from location to location we also move in other ways. For example, think about grasping something with your hands and placing it in your mouth, or protecting yourself by kicking at something with your lower limb. How about throwing something? All of
these activities are forms of movement that occur without moving from one location to another, yet they are movements nonetheless. Like moving about, these other types of movements are
not only essential for survival, but define the broad spectrum for the majority of human movement. Reflect for a moment on the wide variety of movements that you make without moving from place to place. For example, think about the variety of intricate movements required to eat a meal, movements such as grasping, manipulating, cutting, chewing, and swallowing. Another example is getting dressed for the day. From the simple movements of pulling on clothing to the intricate movements of buttoning shirts and tying shoelaces, getting dressed involves a wide variety of movements. And here is something else to ponder — how about all the movements involved in communication? Think of the wide array of movements
that you produce as you communicate with others — whether the communication involves writing a note on a piece of paper, typing a letter on the keyboard of a computer, signaling pleasure and happiness with a smile, or using your voice to talk to a friend on the telephone.
We could go on and on discussing the wide variety of movement and its importance, but the bottom line is all movement results from the combined activity
of individual muscles. The most detailed movements you
make can be broken down into the simple actions of individual muscles moving the bones of the skeleton at the joints. This chapter introduces the muscular system. On the pages that follow you will see the structural design of a typical muscle and whole body views of
the muscles of the body. Our approach to the skeletal muscles of the body is based on their embryonic origins. The four chapters that follow this chapter cover each of the developmental groups of muscles — muscles of the head, muscles of the trunk, muscles of the upper limb, and muscles of the lower limb. The logic of this approach will be further discussed as we introduce each chapter.
Find more information about the muscular system in
R E A L A N AT O M Y
139
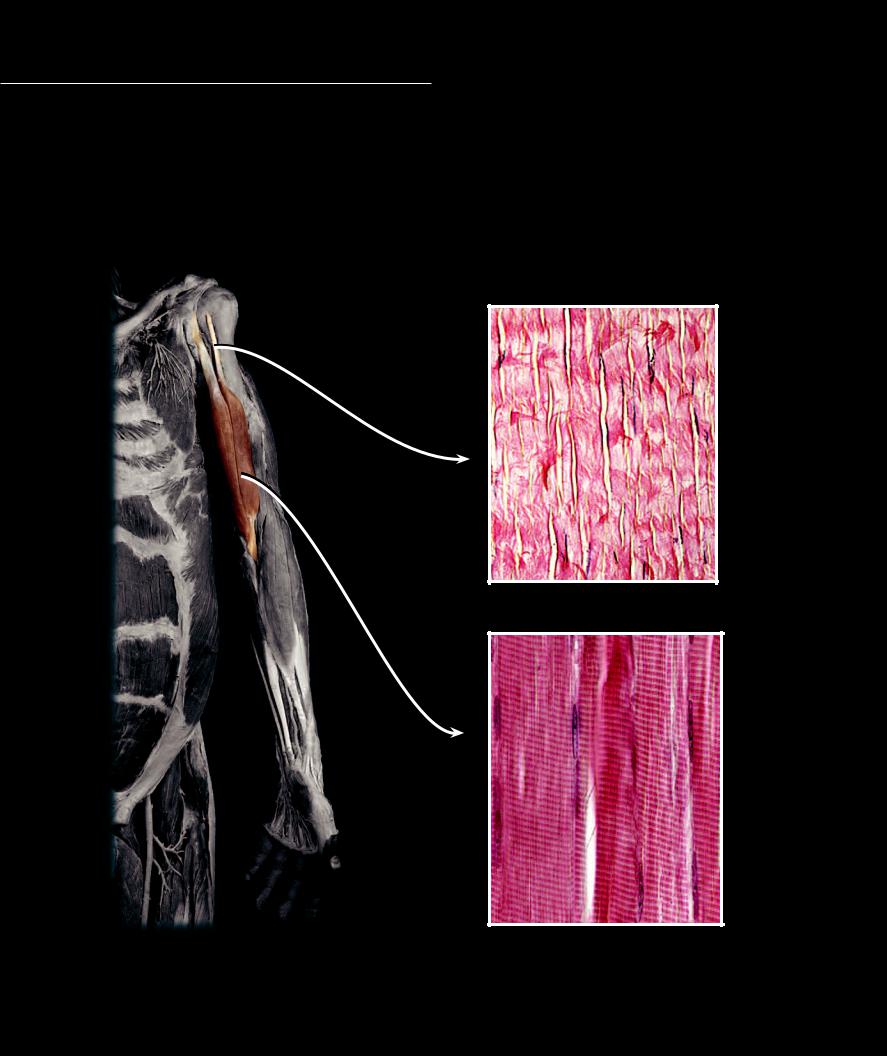
While there is a wide variety to the shape, size, and architecture of the skeletal muscles of the body, most muscles share a common basic design — a tendon of origin, a muscle body
or belly, and a tendon of insertion. The tendons, projecting from the muscle belly, are a continuation of the connective tissue surrounding the muscle cells within the belly of the muscle. As the connective tissue projects beyond the muscle cells, it condenses to become the tendons, which merge and blend with the periosteum to attach the muscle to bone.
1 |
Muscle belly or body |
7 |
Biceps brachii muscle |
13 |
Blood vessels in perimysium |
2 |
Tendon of origin |
8 |
Brachialis muscle |
14 |
Nerve in perimysium |
3 |
Tendon of insertion |
9 |
Triceps brachii muscle |
15 |
Fascia |
4 |
Collagen fiber |
10 |
Epimysium |
16 |
Sucutaneous layer |
5 |
Muscle cell or fiber |
11 |
Perimysium |
17 |
Skin |
6 |
Nucleus |
12 |
Endomysium |
18 |
Periosteum |
2
2
1 |
4 |
3
Dense regular connective tissue of tendon
200x
6
5
Dissection of brachium highlighting biceps brachii as example of muscle anatomy
Anterior view
140
Skeletal muscle tissue of muscle belly
400x
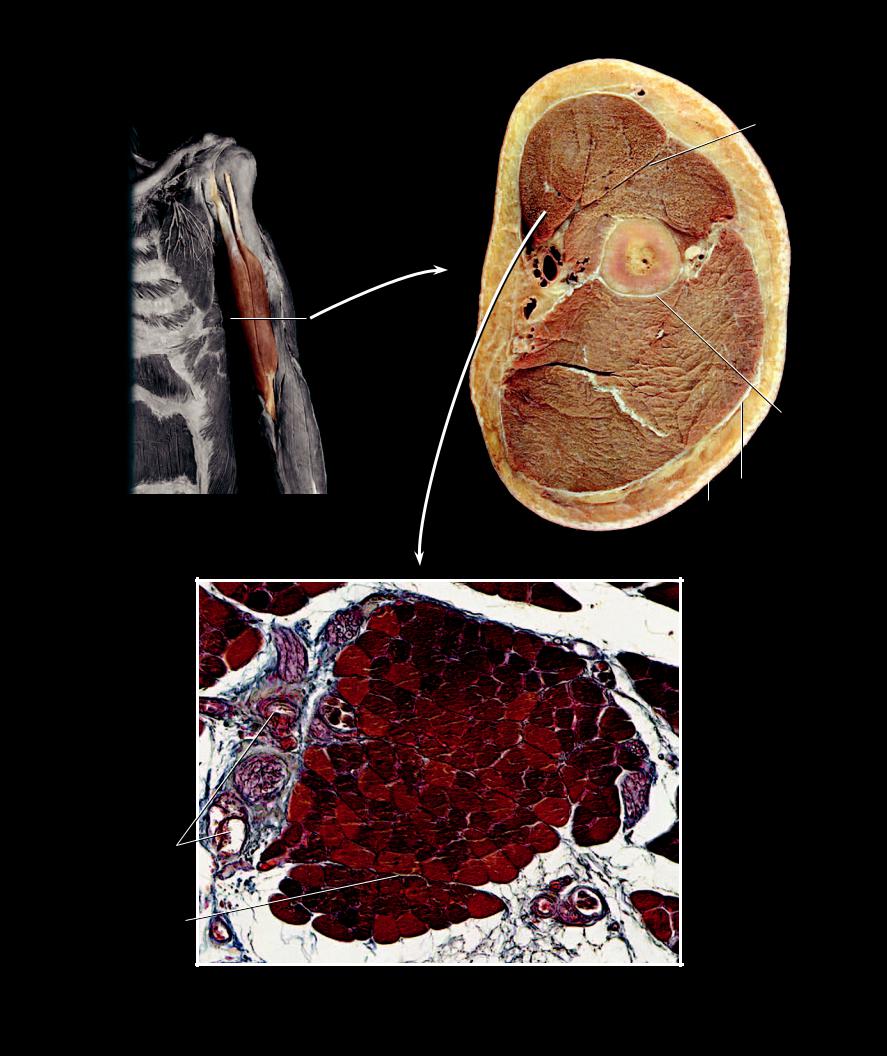
10
7
8
7
9
18
|
|
15 |
|
16 |
|
|
|
|
Dashed line shows level of transverse section |
17 |
|
|
|
|
Anterior view |
|
|
|
Transverse section of left brachium at level of dashed line |
|
|
Inferior (distal) view, anterior at top |
|
|
11 |
|
5
5
14
5
13
12
5
Photomicrograph of muscle fasciculus
Transverse section, 100x
141
