
- •Preface to the 3rd edition
- •General Pharmacology
- •Systems Pharmacology
- •Therapy of Selected Diseases
- •Subject Index
- •Abbreviations
- •General Pharmacology
- •History of Pharmacology
- •Drug and Active Principle
- •The Aims of Isolating Active Principles
- •European Plants as Sources of Effective Medicines
- •Drug Development
- •Congeneric Drugs and Name Diversity
- •Oral Dosage Forms
- •Drug Administration by Inhalation
- •Dermatological Agents
- •From Application to Distribution in the Body
- •Potential Targets of Drug Action
- •External Barriers of the Body
- •Blood–Tissue Barriers
- •Membrane Permeation
- •Binding to Plasma Proteins
- •The Liver as an Excretory Organ
- •Biotransformation of Drugs
- •Drug Metabolism by Cytochrome P450
- •The Kidney as an Excretory Organ
- •Presystemic Elimination
- •Drug Concentration in the Body as a Function of Time—First Order (Exponential) Rate Processes
- •Time Course of Drug Concentration in Plasma
- •Time Course of Drug Plasma Levels during Repeated Dosing (A)
- •Time Course of Drug Plasma Levels during Irregular Intake (B)
- •Accumulation: Dose, Dose Interval, and Plasma Level Fluctuation (A)
- •Dose–Response Relationship
- •Concentration–Effect Curves (B)
- •Concentration–Binding Curves
- •Types of Binding Forces
- •Agonists—Antagonists
- •Other Forms of Antagonism
- •Enantioselectivity of Drug Action
- •Receptor Types
- •Undesirable Drug Effects, Side Effects
- •Drug Allergy
- •Cutaneous Reactions
- •Drug Toxicity in Pregnancy and Lactation
- •Pharmacogenetics
- •Placebo (A)
- •Systems Pharmacology
- •Sympathetic Nervous System
- •Structure of the Sympathetic Nervous System
- •Adrenergic Synapse
- •Adrenoceptor Subtypes and Catecholamine Actions
- •Smooth Muscle Effects
- •Cardiostimulation
- •Metabolic Effects
- •Structure–Activity Relationships of Sympathomimetics
- •Indirect Sympathomimetics
- •Types of
- •Antiadrenergics
- •Parasympathetic Nervous System
- •Cholinergic Synapse
- •Parasympathomimetics
- •Parasympatholytics
- •Actions of Nicotine
- •Localization of Nicotinic ACh Receptors
- •Effects of Nicotine on Body Function
- •Aids for Smoking Cessation
- •Consequences of Tobacco Smoking
- •Dopamine
- •Histamine Effects and Their Pharmacological Properties
- •Serotonin
- •Vasodilators—Overview
- •Organic Nitrates
- •Calcium Antagonists
- •ACE Inhibitors
- •Drugs Used to Influence Smooth Muscle Organs
- •Cardiac Drugs
- •Cardiac Glycosides
- •Antiarrhythmic Drugs
- •Drugs for the Treatment of Anemias
- •Iron Compounds
- •Prophylaxis and Therapy of Thromboses
- •Possibilities for Interference (B)
- •Heparin (A)
- •Hirudin and Derivatives (B)
- •Fibrinolytics
- •Intra-arterial Thrombus Formation (A)
- •Formation, Activation, and Aggregation of Platelets (B)
- •Inhibitors of Platelet Aggregation (A)
- •Presystemic Effect of ASA
- •Plasma Volume Expanders
- •Lipid-lowering Agents
- •Diuretics—An Overview
- •NaCl Reabsorption in the Kidney (A)
- •Aquaporins (AQP)
- •Osmotic Diuretics (B)
- •Diuretics of the Sulfonamide Type
- •Potassium-sparing Diuretics (A)
- •Vasopressin and Derivatives (B)
- •Drugs for Gastric and Duodenal Ulcers
- •Laxatives
- •Antidiarrheal Agents
- •Drugs Affecting Motor Function
- •Muscle Relaxants
- •Nondepolarizing Muscle Relaxants
- •Depolarizing Muscle Relaxants
- •Antiparkinsonian Drugs
- •Antiepileptics
- •Pain Mechanisms and Pathways
- •Eicosanoids
- •Antipyretic Analgesics
- •Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
- •Cyclooxygenase (COX) Inhibitors
- •Local Anesthetics
- •Opioid Analgesics—Morphine Type
- •General Anesthesia and General Anesthetic Drugs
- •Inhalational Anesthetics
- •Injectable Anesthetics
- •Sedatives, Hypnotics
- •Benzodiazepines
- •Pharmacokinetics of Benzodiazepines
- •Therapy of Depressive Illness
- •Mania
- •Therapy of Schizophrenia
- •Psychotomimetics (Psychedelics, Hallucinogens)
- •Hypothalamic and Hypophyseal Hormones
- •Thyroid Hormone Therapy
- •Glucocorticoid Therapy
- •Follicular Growth and Ovulation, Estrogen and Progestin Production
- •Oral Contraceptives
- •Antiestrogen and Antiprogestin Active Principles
- •Aromatase Inhibitors
- •Insulin Formulations
- •Treatment of Insulin-dependent Diabetes Mellitus
- •Treatment of Maturity-Onset (Type II) Diabetes Mellitus
- •Oral Antidiabetics
- •Drugs for Maintaining Calcium Homeostasis
- •Drugs for Treating Bacterial Infections
- •Inhibitors of Cell Wall Synthesis
- •Inhibitors of Tetrahydrofolate Synthesis
- •Inhibitors of DNA Function
- •Inhibitors of Protein Synthesis
- •Drugs for Treating Mycobacterial Infections
- •Drugs Used in the Treatment of Fungal Infections
- •Chemotherapy of Viral Infections
- •Drugs for the Treatment of AIDS
- •Drugs for Treating Endoparasitic and Ectoparasitic Infestations
- •Antimalarials
- •Other Tropical Diseases
- •Chemotherapy of Malignant Tumors
- •Targeting of Antineoplastic Drug Action (A)
- •Mechanisms of Resistance to Cytostatics (B)
- •Inhibition of Immune Responses
- •Antidotes and Treatment of Poisonings
- •Therapy of Selected Diseases
- •Hypertension
- •Angina Pectoris
- •Antianginal Drugs
- •Acute Coronary Syndrome— Myocardial Infarction
- •Congestive Heart Failure
- •Hypotension
- •Gout
- •Obesity—Sequelae and Therapeutic Approaches
- •Osteoporosis
- •Rheumatoid Arthritis
- •Migraine
- •Common Cold
- •Atopy and Antiallergic Therapy
- •Bronchial Asthma
- •Emesis
- •Alcohol Abuse
- •Local Treatment of Glaucoma
- •Further Reading
- •Further Reading
- •Picture Credits
- •Drug Indexes

Systems Pharmacology
Drugs Acting on the Sympathetic Nervous System 84 Drugs Acting on the Parasympathetic Nervous System 102
Nicotine |
112 |
|
|
|
|
|
|
Biogenic Amines |
116 |
|
|
|
|||
Vasodilators |
122 |
|
|
|
|
|
|
Inhibitors of the Renin–Angiotensin–Aldosterone System 128 |
|||||||
Drugs Acting on Smooth Muscle |
130 |
|
|||||
Cardiac Drugs |
132 |
|
|
|
|
||
Antianemics |
140 |
|
|
|
|
|
|
Antithrombotics |
144 |
|
|
|
|||
Plasma Volume Expanders |
156 |
|
|
||||
Drugs Used in Hyperlipoproteinemias |
158 |
||||||
Diuretics |
162 |
|
|
|
|
|
|
Drugs for the Treatment of Peptic Ulcers 170 |
|||||||
Laxatives |
174 |
|
|
|
|
|
|
Antidiarrheals |
180 |
|
|
|
|
||
Drugs Acting on the Motor System 182 |
|||||||
Drugs for the Suppression of Pain |
194 |
|
|||||
Antipyretic Analgesics 196 |
|
|
|||||
Nonsteroidal Anti-inflammatory Drugs |
200 |
||||||
Local Anesthetics |
202 |
|
|
|
|||
Opioids |
208 |
|
|
|
|
|
|
General Anesthetics |
214 |
|
|
|
|||
Psychopharmacologicals |
220 |
|
|
||||
Hormones 238 |
|
|
|
|
|
||
Antibacterial Drugs |
268 |
|
|
|
|||
Antifungal Drugs |
284 |
|
|
|
|||
Antiviral Drugs 286 |
|
|
|
|
|||
Antiparasitic Drugs |
292 |
|
|
|
|||
Anticancer Drugs |
298 |
|
|
|
|||
Immune Modulators |
304 |
|
|
|
|||
Antidotes |
308 |
|
|
|
|
|
|

84 Drugs Acting on the Sympathetic Nervous System
Sympathetic Nervous System
In the course of phylogeny an ef cient control system evolved that enabled the functions of individual organs to be orchestrated in increasingly complex life forms and permitted rapid adaptation to changing environmental conditions. This regulatory system consists of the central nervous system (CNS) (brain plus spinal cord) and two separate pathways for two-way communication with peripheral organs, namely, the somatic and the autonomic nervous systems. The somatic nervous system, comprising exteroceptive andinteroceptive afferents,special sense organs, and motor efferents, serves to perceive external states and to target appropriate body movement (sensory perception: threat † response: flight or attack). The autonomic (vegetative) nervous system
(ANS) together with the endocrine system controls the milieu interieur. It adjusts internal organ functions to the changing needs of the organism. Neural control permits very quick adaptation, whereas the endocrine system provides for a long-term regulation of functionalstates. The ANS operateslargely beyond voluntary control: it functions autonomously. Itscentralcomponentsreside in the hypothalamus, brainstem, and spinal cord. The ANS also participates in the regulation of endocrine functions.
The ANS has sympathetic and parasympathetic (p.102) branches. Both are made up of centrifugal (efferent) and centripetal (afferent)nerves. In manyorgansinnervated by both branches, respective activation of the sympathetic and parasympathetic input evokes opposing responses.
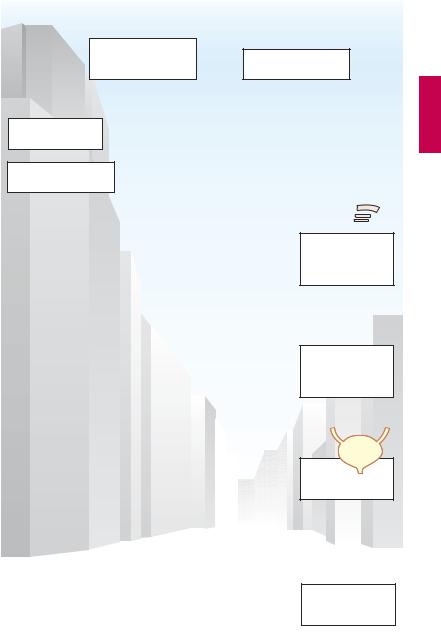
In various disease states (organ malfunctions), drugs are employed with the intention of normalizing susceptible organ functions. To understand the biological effects of substances capable of inhibiting or exciting sympathetic or parasympathetic nerves, one must first envisage the functions subserved by the sympathetic and parasympathetic divisions (A, Response to sympathetic activa-
tion). In simplistic terms, activation of the sympathetic division can be considered a means by which the body achieves a state of maximal work capacity as required in fight-or-flight situations.
In both cases, there is a need for vigorous activity of skeletal musculature. To ensure adequate supply of oxygen and nutrients, blood flow in skeletal muscle is increased; cardiac rate and contractility are enhanced, resulting in a larger blood volume being pumped into the circulation. Narrowing of splanchnic blood vessels diverts blood into vascular beds in muscle.
Because digestion of food in the intestinal tract is dispensable and essentially counterproductive, the propulsion of intestinal contents is slowed to the extent that peristalsis diminishes and sphincters are narrowed. However, in order to increase nutrient supply to heart and musculature, glucose from the liver and free fatty acids from adipose tissue must be released into the blood. The bronchi are dilated, enabling tidal volume and alveolar oxygen uptake to be increased.
Sweat glands are also innervated by sympathetic fibers (wet palms due to excitement); however, these are exceptional as regards their neurotransmitter (ACh, p.110).
The lifestyles of modern humans are different from those of our hominid ancestors, but biological functions have remained the same: a “stress”-induced state of maximal work capacity, albeit without energy-con- suming muscle activity.
Sympathetic Nervous System |
85 |
A. Response to sympathetic activation |
|
|
CNS: |
|
|
drive |
Eyes: |
|
alertness |
pupillary dilation |
|
Saliva: |
|
|
little, viscous |
|
|
Bronchi: |
|
|
dilation |
|
|
|
Heart: |
|
Skin: |
rate |
|
force |
||
perspiration |
||
blood pressure |
||
(cholinergic) |
||
|
||
|
Fat tissue: |
|
|
lipolysis |
|
|
fatty acid |
|
|
liberation |
|
Liver: |
|
|
glycogenolysis |
Bladder: |
|
glucose release |
sphincter tone |
|
|
detrusor muscle |
|
GI tract: |
|
|
peristalsis |
|
|
sphincter tone |
|
|
blood flow |
|
|
|
Skeletal muscle: |
|
|
blood flow |
|
|
glycogenolysis |

86 Drugs Acting on the Sympathetic Nervous System
Structure of the Sympathetic Nervous System
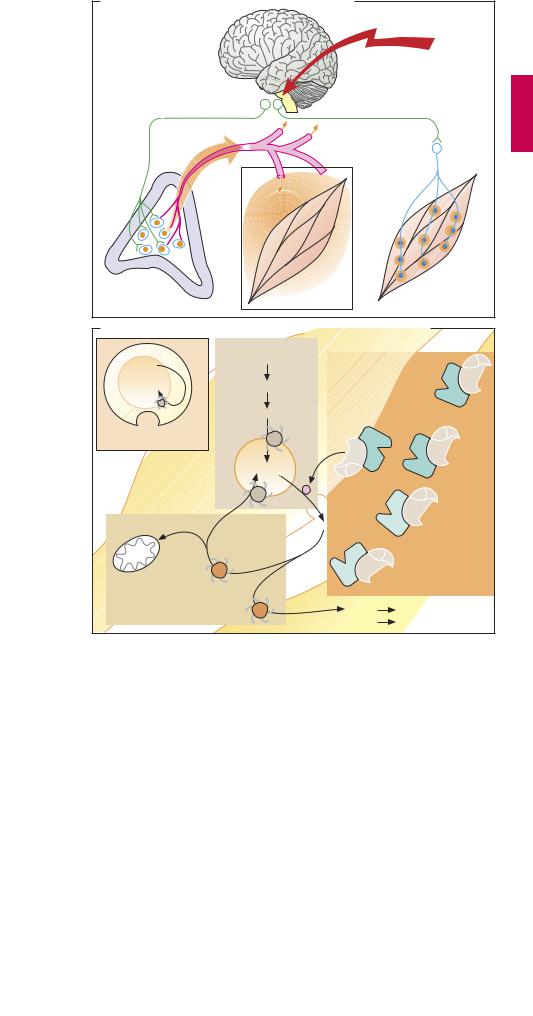
The sympathetic preganglionic neurons (first neurons) project from the intermediolateral column of the spinal gray matter to the paired paravertebral ganglionic chain lying alongside the vertebral column and to unpaired prevertebral ganglia. These ganglia represent sites of synaptic contact between preganglionic axons (1st neurons) and nerve cells (2nd neurons or sympathocytes) that emit axons terminating at postganglionic synapses (or contacts) on cells in various end organs. In addition, there are preganglionic neurons that project either to peripheral ganglia in end organs or to the adrenal medulla.
Sympathetic transmitter substances.
Whereas acetylcholine (see p.104) serves as the chemical transmitter at ganglionic synapses between first and second neurons, norepinephrine (noradrenaline) is the mediator at synapses of the second neuron (B). This second neuron does not synapse with only a single cell in the effector organ; rather it branches out, each branch making en passant contacts with several cells. At these junctions the nerve axons form enlargements (varicosities) resembling beads on a string. Thus, excitation of the neuron leads to activation of a larger aggregate of effector cells, although the action of released norepinephrine may be confined to the region of each junction. Excitation of preganglionic neurons innervating the adrenal medulla causes liberation of acetylcholine. This, in turn, elicits secretion of epinephrine (adrenaline) into the blood, by which it is distributed to body tissues as a hormone (A).
Adrenergic Synapse
Within the varicosities, norepinephrine is stored in small membrane-enclosed vesicles (granules, 0.05–0.2 µm in diameter). In the
axoplasm, norepinephrine is formed by stepwise enzymatic synthesis from L-tyrosine, which is converted by tyrosine hydroxylase to L-Dopa (see p.188). L-Dopa in turn is decarboxylated to dopamine, which is taken up into storage vesicles by the vesicular monoamine transporter (VMAT). In the vesicle, dopamine is converted to norepinephrine by dopamine β-hydroxylase. In the adrenal medulla, the major portion of norepinephrine undergoes enzymatic methylation to epinephrine.
When stimulated electrically, the sympathetic nerve discharges the contents of part of its vesicles, including norepinephrine, into the extracellular space. Liberated norepinephrine reacts with adrenoceptors located postjunctionally on the membrane of effector cells or prejunctionally on the membrane of varicosities. Activation of pre-syn- aptic α2-receptors inhibits norepinephrine release. Through this negative feedback, release can be regulated.
The effect of released norepinephrine wanes quickly, because ~ 90% is transported back into the axoplasm by a specific transport mechanism (norepinephrine transporter, NAT) and then into storage vesicles by the vesicular transporter (neuronal reuptake). The NAT can be inhibited by tricyclic antidepressants and cocaine. Moreover, norepinephrine is taken up by transporters into the effector cells (extraneuronal monoamine transporter, EMT). Part of the norepinephrine undergoing reuptake is enzymatically inactivated to normetanephrine via catecholamine O-methyltransferase (COMT, present in the cytoplasm of postjunctional cells) and to dihydroxymandelic acid via monoamine oxidase (MAO, present in mitochondria of nerve cells and postjunctional cells).
The liver is richly endowed with COMT and MAO; it therefore contributes significantly to the degradation of circulating norepinephrine and epinephrine. The end product of the combined actions of MAO and COMT is vanillylmandelic acid.
Structure of the Sympathetic Nervous System |
87 |
A. Epinephrine as hormone, norepinephrine as transmitter |
|
|
|
|
|
|
|||
Psychic |
|
|
|
|
|
|
or physical |
|
|
stress |
|
|
|
|
|
|
|
stress |
|
First neuron |
|
|
|
|
|
|
First neuron |
|
|
Adrenal |
|
|
|
|
Second neuron |
|
|||
medulla |
|
|
|
|
|
|
|
|
|
Epinephrine |
|
|
|
|
|
|
|
Norepinephrine |
|
B. Second neuron of sympathetic system, varicosity, norepinephrine release |
|
||||||||
|
Synthesis |
|
Sympathetic nerve |
|
|
||||
|
|
|
|
|
|
|
|
|
|
Nor- |
Tyrosine |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
epinephrine |
|
|
|
|
|
|
|
|
G |
Epinephrine |
L-Dopa |
|
|
|
|
|
|
|
q/11 |
|
|
|
|
|
|
|
α |
||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
1 |
|
Dopamine |
|
|
|
|
|
|
|
|
|
VMAT |
|
|
|
|
|
|
|
|
Adrenal chromaffin cell |
|
|
|
|
|
|
|
|
G |
|
|
|
|
|
|
|
|
|
|
|
|
|
G |
α |
|
|
|
i |
|
|
Norepinephrine |
|
i |
2 |
|
α 2 |
|
||
|
|
|
|
|
|||||
|
|
|
|
|
|
|
|
||
|
|
– |
|
|
|
|
|
|
Receptors |
|
VMAT |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
G |
|
|
|
|
|
|
|
|
β |
s |
|
|
|
|
|
|
|
|
|
|
|
Transport, degradation |
|
|
|
|
|
|
1 |
|
|
|
|
|
|
|
|
|
|
|
|
MAO |
|
|
|
G |
|
|
|
|
|
NAT |
|
|
β |
s |
|
|
|
|
|
|
|
|
|
|
|
|
|||
|
|
|
2 |
|
|
|
|
|
|
|
EMT |
|
COMT |
|
|
Effector cell |
|||
|
|
|
MAO |
|
|
|
|||
|
|
|
|
|
|
|
|||
