
- •Contents
- •Foreword
- •1.1.1 Haemostasis
- •1.1.2 Inflammatory Phase
- •1.1.3 Proliferative Phase
- •1.1.4 Remodelling and Resolution
- •1.7 The Surgeon’s Preoperative Checklist
- •1.8 Operative Note
- •2.4.1 Local Risks
- •2.4.2 Systemic Risks
- •2.5 Basic Oral Anaesthesia Techniques
- •2.5.1 Buccal Infiltration Anaesthetic
- •2.5.2 Mandibular Teeth
- •2.5.2.1 Conventional ‘Open-Mouth’ Technique
- •2.5.2.2 Akinosi ‘Closed-Mouth’ Technique
- •2.5.2.3 Gow–Gates Technique
- •2.5.2.4 Mandibular Long Buccal Block
- •2.5.2.5 Mental Nerve Block
- •2.5.3 Maxillary Teeth
- •2.5.3.1 Greater Palatine Block
- •2.5.3.2 Palatal Infiltration
- •2.5.3.3 Nasopalatine Nerve Block
- •2.5.3.4 Posterior Superior Alveolar Nerve Block
- •2.6 Adjunct Methods of Local Anaesthesia
- •2.6.1 Intraligamentary Injection
- •2.6.2 Intrapulpal Injection
- •2.7 Troubleshooting
- •3.1 Retractors
- •3.2 Elevators, Luxators, and Periotomes
- •3.3 Dental Extraction Forceps
- •3.4 Ancillary Soft Tissue Instruments
- •3.5 Suturing Instruments
- •3.6 Surgical Suction
- •3.7 Surgical Handpiece and Bur
- •3.8 Surgical Irrigation Systems
- •3.9 Mouth Props
- •4.1 Maxillary Incisors
- •4.2 Maxillary Canines
- •4.3 Maxillary Premolars
- •4.4 Maxillary First and Second Molars
- •4.5 Mandibular Incisors
- •4.6 Mandibular Canines and Premolars
- •4.7 Mandibular Molars
- •5.3 Common Soft Tissue Flaps for Dental Extraction
- •5.4 Bone Removal
- •5.5 Tooth Sectioning
- •5.6 Cleanup and Closure
- •6.2 Damage to Adjacent Teeth or Restorations
- •7.4.1.1 Erupted
- •7.4.1.2 Unerupted/Partially Erupted
- •7.4.2 Mandibular Third Molars
- •7.4.2.1 Mesioangular
- •7.4.2.2 Distoangular/Vertical
- •7.4.2.3 Horizontal
- •7.4.2.4 Full Bony Impaction (Early Root Development)
- •8.1 Ischaemic Cardiovascular Disease
- •8.5 Diabetes Mellitus
- •8.6.1 Bleeding Diatheses
- •8.6.2 Medications
- •8.6.2.1 Management of Antiplatelet Agents Prior to Dentoalveolar Surgery
- •8.6.2.2 Management of Patients Taking Warfarin Prior to Dentoalveolar Surgery
- •8.6.2.3 Management of Patients Taking Direct Anticoagulant Agents Prior to Dentoalveolar Surgery
- •8.8 The Irradiated Patient
- •8.8.1 Management of the Patient with a History of Head and Neck Radiotherapy
- •9.5.1 Alveolar Osteitis
- •9.5.2 Acute Facial Abscess
- •9.5.3 Postoperative Haemorrhage
- •9.5.4 Temporomandibular Joint Disorder
- •9.5.5 Epulis Granulomatosa
- •9.5.6 Nerve Injury
- •B.1.3 Consent
- •B.1.4 Local Anaesthetic
- •B.1.5 Use of Sedation
- •B.1.6 Extraction Technique
- •B.1.7 Outcomes Following Extraction
- •B.2.1 Deciduous Incisors and Canines
- •B.2.2 Deciduous Molars
- •Bibliography
- •Index
26 2 Local Anaesthesia
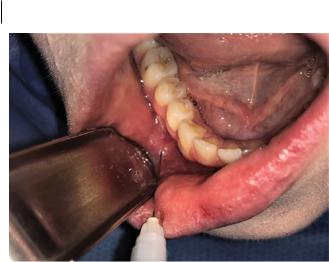
Figure 2.9 Mental nerve block.
1)Position the patient in the dental chair, lying flat with head slightly extended and mouth open.
2)Retract the labial mucosa to keep the soft tissues under tension.
3)Insert the needle into the mucosa in the deepest part of the vestibule, between the lower first and second premolar teeth, to a depth of approximately 2 mm (Figure 2.9). It is not necessary for the needle tip to contact bone for this technique to be successful.
4)Aspirate the syringe to ensure the needle point has not traversed the intravascular space of a blood vessel.
5)Deposit the anaesthetic solution slowly; a slow rate of injection significantly reduces discomfort for the patient.
6)Allow the local anaesthetic sufficient time to anaesthetise the tissues, based upon the pharmacokinetic properties of the solution, and monitor the patient for any adverse reaction.
2.5.3 Maxillary Teeth
The maxillary teeth, periodontium, and mucosa are innervated by the maxillary division of the trigeminal nerve (Figure 2.10). This nerve trunk exits the cranium via the foramen rotundum, entering the pterygopalatine fossa. One of the branches given off in the pterygopalatine fossa is the posterior superior alveolar nerve, which passes through the pterygomaxillary fissure into the infratemporal fossa and descends on to the posterior surface of the maxilla, before traversing forward and innervating the posterior maxillary gingiva and teeth. Branches of this nerve supply the maxillary molars, and the mucosa on the buccal aspect of those teeth.
The nerve continues to branch as it courses anteriorly, giving rise to the middle superior alveolar nerve, which innervates the maxillary premolars and associated buccal gingiva, and finally the anterior superior alveolar nerve, which innervates the maxillary incisors, canines, and associated buccal gingiva.
The greater and lesser palatine nerves arise from the pterygopalatine ganglion located within the pterygopalatine fossa. These nerves descend through the palatine canal. The greater palatine nerve exits on to the posterior surface of the maxilla via the greater palatine foramen and gives rise to branches which supply the palatal mucosa from the midline to the canine tooth. The lesser palatine nerve exits the lesser palatine foramen and supplies innervation to the soft palate.
https://t.me/DentalBooksWorld

2.5 asic Oal Anaesthesia echniiqes 27
|
Nasal cavity |
Posterior superior |
|
|
|
|
|
alveolar nerve |
|
|
Foramen rotundum |
|
|
Maxillary branch of |
|
|
trigeminal nerve |
Infraorbital nerve |
|
Trigeminal |
|
ganglion |
|
|
|
|
|
|
|
|
|
|
|
|
Pterygomaxillary fissure |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Pterygopalatine ganglion |
|
|
|
|
|
|
|
|
|
|
Middle superior |
|
|
|
|
|
|
|
|
Pterygopalatine fossa |
|
|
|
|
|
|
|
|||
|
|
|
|
|
|
|
Lesser palatine nerve |
||
alveolar nerve |
|
|
|
Greater palatine nerve |
|||||
|
|
|
|||||||
Anterior superior |
|
|
|
Palatine canal |
|||
alveolar nerve |
|
|
|
|
|
|
|
|
|
|
|
|
|
||
Nasopalatine |
|
|
|
Greater and lesser |
|||
nerve |
|
|
|
|
|
palatine foramens |
|
|
|
|
|
||||
Incisive foramen |
|
|
|
|
|||
|
|
|
|
|
|
|
Pterygoid process |
|
|
|
|
|
|
|
|
Figure 2.10 Anatomy of nerve supply to the maxilla.
The nasopalatine nerve travels anteriorly from the pterygopalatine ganglion through the sphenopalatine foramen, entering the nasal cavity. It travels anteriorly then inferiorly, entering the incisive canal and on to the anterior aspect of the hard palate via the incisive foramen. The nasopalatine nerve supplies the sensation to the palatal mucosa of the canines and incisors.
2.5.3.1 Greater Palatine Block
This nerve block can be used to provide anaesthesia for the palatal mucosa of the maxilla to the midline and up to the canine area. In the majority of cases, this foramen is adjacent or just distal to the second maxillary molar area.
1)Position the patient in the dental chair, lying flat with head slightly extended and mouth open.
2)Using the back end of a dental mirror or similar instrument, place pressure on the palatal mucosa adjacent to the third molar area 1–2cm medial to the gingival margin of the tooth.
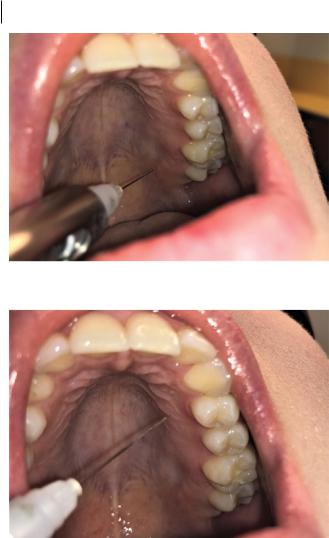
3)Advance the needle into the mucosa in this region (Figure 2.11).
4)Aspirate the syringe to ensure the needle point has not traversed the intravascular spaceof a blood vessel.
5)Deposit the anaesthetic solution slowly; a slow rate of injection significantly reduces discomfort for the patient. Due to the keratinised nature of the palatal mucosa, only a small volume of solution can be injected into this space to produce anaesthesia.
6)Allow the local anaesthetic sufficient time to anaesthetise the tissues, based upon the pharmacokinetic properties of the solution, and monitor the patient for any adverse reaction.
https://t.me/DentalBooksWorld
28 2 Local Anaesthesia
Figure 2.11 Greater palatine block.
Figure 2.12 Palatal infiltration.
2.5.3.2Palatal Infiltration
1)Position the patient in the dental chair, lying flat with head slightly extended and mouth open.
2)Using the back end of a dental mirror or similar instrument, place pressure on the palatal mucosa adjacent to the site of injection.
3)Advance the needle through the depth of the palatal mucosa, adjacent to the teeth where anaesthesia is required (Figure 2.12).
4)Aspirate the syringe to ensure the needle point has not traversed the intravascular space of a blood vessel.
5)Deposit the anaesthetic solution slowly; a slow rate of injection significantly reduces discomfort for the patient. Due to the keratinised nature of the palatal mucosa, only minute volumes of solution can be injected into the palatal mucosal to produce anaesthesia. Examine for blanching of the tissues as evidence of successful infiltration of anaesthetic solution.
6)Allow the local anaesthetic sufficient time to anaesthetise the tissues, based upon the pharmacokinetic properties of the solution, and monitor the patient for any adverse reaction.
https://t.me/DentalBooksWorld
2.5 asic Oal Anaesthesia echniiqes 29
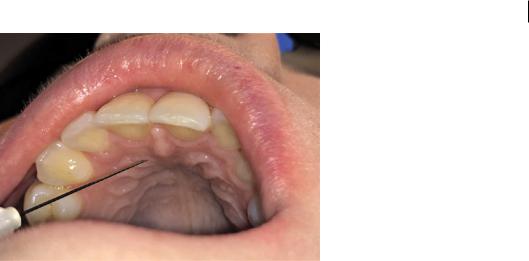
Figure 2.13 Nasopalatine nerve block. SoqOce: Seth Delpachitra.
2.5.3.3Nasopalatine Nerve Block
The nasopalatine nerve supplies sensation to the palatal gingiva posterior to the maxillary incisors and canines. This nerve can be anaesthetised by depositing local anaesthesia around the incisive papilla.
1)Position the patient in the dental chair, lying flat with head slightly extended and mouth open.
2)Locate the incisive papilla, which is often readily discernible as a raised midline structure posterior to the central incisors.
3)Insert the needle adjacent to the incisive papilla (Figure 2.13).
4)Aspirate the syringe to ensure the needle point has not traversed the intravascular space of a blood vessel.
5)Deposit the anaesthetic solution slowly; a slow rate of injection significantly reduces discomfort for the patient. Due to the keratinised nature of the palatal mucosa, only minute volumes of solution can be injected into the palatal mucosal to produce anaesthesia. Examine for blanching of the tissues as evidence of successful infiltration of anaesthetic solution.
6)Allow the local anaesthetic sufficient time to anaesthetise the tissues, based upon the pharmacokinetic properties of the solution, and monitor the patient for any adverse reaction.
2.5.3.4Posterior Superior Alveolar Nerve Block
If anaesthesia of the hemimaxilla is required (e.g. in a full maxillary dental clearance), a posterior superior alveolar nerve block may be used in lieu of multiple buccal infiltration anaesthetics. This technique is not dissimilar to conventional buccal infiltration; the major difference is that the location of anaesthetic solution deposition is in the infratemporal fossa just behind the posterior maxilla, where the posterior superior alveolar nerve trunk travels.
1)Position the patient in the dental chair, lying flat with head slightly extended and mouth slightly open.
2)Palpate the zygomatic buttress and take note of its relative position, usually just superior to the first or second maxillary molar.
3)Retract the buccal tissues, such that the buccal gingiva, maxillary tuberosity, and cervical margin of the maxillary teeth can be visualised and the buccal soft tissues are taut.
https://t.me/DentalBooksWorld
