
- •Contents
- •Foreword
- •1.1.1 Haemostasis
- •1.1.2 Inflammatory Phase
- •1.1.3 Proliferative Phase
- •1.1.4 Remodelling and Resolution
- •1.7 The Surgeon’s Preoperative Checklist
- •1.8 Operative Note
- •2.4.1 Local Risks
- •2.4.2 Systemic Risks
- •2.5 Basic Oral Anaesthesia Techniques
- •2.5.1 Buccal Infiltration Anaesthetic
- •2.5.2 Mandibular Teeth
- •2.5.2.1 Conventional ‘Open-Mouth’ Technique
- •2.5.2.2 Akinosi ‘Closed-Mouth’ Technique
- •2.5.2.3 Gow–Gates Technique
- •2.5.2.4 Mandibular Long Buccal Block
- •2.5.2.5 Mental Nerve Block
- •2.5.3 Maxillary Teeth
- •2.5.3.1 Greater Palatine Block
- •2.5.3.2 Palatal Infiltration
- •2.5.3.3 Nasopalatine Nerve Block
- •2.5.3.4 Posterior Superior Alveolar Nerve Block
- •2.6 Adjunct Methods of Local Anaesthesia
- •2.6.1 Intraligamentary Injection
- •2.6.2 Intrapulpal Injection
- •2.7 Troubleshooting
- •3.1 Retractors
- •3.2 Elevators, Luxators, and Periotomes
- •3.3 Dental Extraction Forceps
- •3.4 Ancillary Soft Tissue Instruments
- •3.5 Suturing Instruments
- •3.6 Surgical Suction
- •3.7 Surgical Handpiece and Bur
- •3.8 Surgical Irrigation Systems
- •3.9 Mouth Props
- •4.1 Maxillary Incisors
- •4.2 Maxillary Canines
- •4.3 Maxillary Premolars
- •4.4 Maxillary First and Second Molars
- •4.5 Mandibular Incisors
- •4.6 Mandibular Canines and Premolars
- •4.7 Mandibular Molars
- •5.3 Common Soft Tissue Flaps for Dental Extraction
- •5.4 Bone Removal
- •5.5 Tooth Sectioning
- •5.6 Cleanup and Closure
- •6.2 Damage to Adjacent Teeth or Restorations
- •7.4.1.1 Erupted
- •7.4.1.2 Unerupted/Partially Erupted
- •7.4.2 Mandibular Third Molars
- •7.4.2.1 Mesioangular
- •7.4.2.2 Distoangular/Vertical
- •7.4.2.3 Horizontal
- •7.4.2.4 Full Bony Impaction (Early Root Development)
- •8.1 Ischaemic Cardiovascular Disease
- •8.5 Diabetes Mellitus
- •8.6.1 Bleeding Diatheses
- •8.6.2 Medications
- •8.6.2.1 Management of Antiplatelet Agents Prior to Dentoalveolar Surgery
- •8.6.2.2 Management of Patients Taking Warfarin Prior to Dentoalveolar Surgery
- •8.6.2.3 Management of Patients Taking Direct Anticoagulant Agents Prior to Dentoalveolar Surgery
- •8.8 The Irradiated Patient
- •8.8.1 Management of the Patient with a History of Head and Neck Radiotherapy
- •9.5.1 Alveolar Osteitis
- •9.5.2 Acute Facial Abscess
- •9.5.3 Postoperative Haemorrhage
- •9.5.4 Temporomandibular Joint Disorder
- •9.5.5 Epulis Granulomatosa
- •9.5.6 Nerve Injury
- •B.1.3 Consent
- •B.1.4 Local Anaesthetic
- •B.1.5 Use of Sedation
- •B.1.6 Extraction Technique
- •B.1.7 Outcomes Following Extraction
- •B.2.1 Deciduous Incisors and Canines
- •B.2.2 Deciduous Molars
- •Bibliography
- •Index
3.9 tLath otor 53
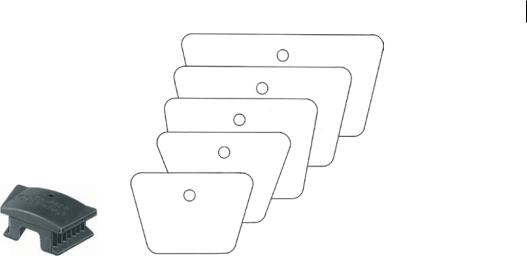
Large Edentulous
Large Adult
Adult Size
Child Size
Small Child Size
1/1
Figure 3.18 Mouth prop. A number of sizes are available. Source: KLS Martin.
critical when using surgical burs, as a coolant to prevent thermal osteonecrosis of the bone. In surgical situations, conventional dental unit water lines for irrigation are not suitable, as nonsterile, pressurised irrigation solutions may predispose to infection of the wound.
Some surgical handpieces come equipped to accommodate a saline bag, which will deliver the saline at the surgical handpiece tip as a coolant. Alternatively, a simple method is the use of a Monoject syringe with sterile saline solution (Figure 3.17).
3.9 Mouth Props
Application of a mouth prop is a useful safety and behaviour-modification technique (Figure 3.18). It allows the patient to keep their mouth open without active effort, and reduces the likelihood of inadvertent mouth closure whilst sharp instruments are inside. Whilst a mouth prop is only absolutely indicated for cases under general anaesthetic, its use in awake patients improves surgical access, stabilises the jaws, and reduces inadvertent swallowing by the patient.
https://t.me/DentalBooksWorld
https://t.me/DentalBooksWorld

55
4
Simple Extraction Techniques
This chapter discusses the specific techniques for extraction of individual teeth in the maxillary and mandibular arch in a detailed, step-wise format. Surgical extractions and third molars are discussed in the subsequent chapters.
4.1Maxillary Incisors
1)Difficulty Assessment. Single-rooted maxillary incisor teeth have largely straight roots, with a slight distal curvature (Figure 4.1). Rarely, this curvature can be significant enough at the tooth apex to warrant a surgical extraction approach. This can be readily assessed on plain-film imaging.
2)Obtain Consent. The general risks of dental extraction apply for maxillary incisors. Any prosthetic rehabilitation plan for anterior teeth should be included in the consent process.
3)Basic Equipment Required. An upper straight forceps can be used for maxillary central and lateral incisors. A straight elevator should be available to expand the periodontal ligament prior to forceps placement.
4)Final Check. Confirm the tooth number and location with radiograph.
5)Local Anaesthetic. Infiltration of the buccal vestibule will provide sufficient anaesthesia for the maxillary buccal soft tissue and periodontal ligament. Localised palatal infiltration is required to anaesthetise the palatal gingiva.
6)Positioning. Lie the patient flat, with the maxillary teeth at the same vertical height as the surgeon’s elbow. Stand on the side of the patient that corresponds with the hand dominance of the surgeon. For example, a right-handed practitioner standing on the right side of the patient increases biomechanical advantage when removing the tooth.
7)Elevation. Apply the straight elevator to the mesial and distal areas of the periodontal ligament. Using a wheel-and-axle motion, gently expand the periodontal ligament until a small amount of mobility is noted in the tooth. Take care to elevate between tooth and bone only, and not against adjacent teeth. The thumb and finger of the nondominant hand should be used to support the alveolus of the tooth being extracted, to guide the application of force to the tooth socket only, and to prevent instrument slippage.
Principles of Dentoalveolar Extractions, First Edition. Seth Delpachitra, Anton Sklavos and Ricky Kumar. © 2021 John Wiley & Sons Ltd. Published 2021 by John Wiley & Sons Ltd.
Companion website: www.wiley.com/go/delpachitradentoalveolarextractions
https://t.me/DentalBooksWorld

56 4 Simple Extraction Techniques
Periodontal
ligament
Cementoenamel
junction
Initial apical pressur
Upper straight forceps
Sagittal view
Rapid, small clockwise-counterclockwise rotational movements
90°rotation
buccal toward midline
Figure 4.1 Extraction of a maxillary incisor tooth.
8)Delivery. Apply the beaks of the straight forceps on to the cementoenamel junction of the tooth. Initially, use apical pressure to slide the beaks as deep on to the root as possible. Employ rapid, small clockwise–counterclockwise rotational movements to continue tearing the periodontal ligament. Finally, rotate the buccal part of the crown towards the midline. This final movement reduces the risk of fracture of the curved root tip, as anterior maxillary alveolar bone is more pliable than thick palatal bone.
9)Assessment. Assess the tooth root to ensure it has been removed complete. Flush the socket with saline to remove any surgical debris. Examine the socket for bleeding, alveolar bone fracture, or soft tissue trauma, and manage as appropriate.
https://t.me/DentalBooksWorld
