
- •CONTENTS
- •Preface
- •Contributors
- •1 Introduction to Toxicology
- •1.1 Definition and Scope, Relationship to Other Sciences, and History
- •1.1.2 Relationship to Other Sciences
- •1.1.3 A Brief History of Toxicology
- •1.3 Sources of Toxic Compounds
- •1.3.1 Exposure Classes
- •1.3.2 Use Classes
- •1.4 Movement of Toxicants in the Environment
- •Suggested Reading
- •2.1 Introduction
- •2.2 Cell Culture Techniques
- •2.2.1 Suspension Cell Culture
- •2.2.2 Monolayer Cell Culture
- •2.2.3 Indicators of Toxicity in Cultured Cells
- •2.3 Molecular Techniques
- •2.3.1 Molecular Cloning
- •2.3.2 cDNA and Genomic Libraries
- •2.3.3 Northern and Southern Blot Analyses
- •2.3.4 Polymerase Chain Reaction (PCR)
- •2.3.5 Evaluation of Gene Expression, Regulation, and Function
- •2.4 Immunochemical Techniques
- •Suggested Reading
- •3.1 Introduction
- •3.2 General Policies Related to Analytical Laboratories
- •3.2.1 Standard Operating Procedures (SOPs)
- •3.2.2 QA/QC Manuals
- •3.2.3 Procedural Manuals
- •3.2.4 Analytical Methods Files
- •3.2.5 Laboratory Information Management System (LIMS)
- •3.3 Analytical Measurement System
- •3.3.1 Analytical Instrument Calibration
- •3.3.2 Quantitation Approaches and Techniques
- •3.4 Quality Assurance (QA) Procedures
- •3.5 Quality Control (QC) Procedures
- •3.6 Summary
- •Suggested Reading
- •4 Exposure Classes, Toxicants in Air, Water, Soil, Domestic and Occupational Settings
- •4.1 Air Pollutants
- •4.1.1 History
- •4.1.2 Types of Air Pollutants
- •4.1.3 Sources of Air Pollutants
- •4.1.4 Examples of Air Pollutants
- •4.1.5 Environmental Effects
- •4.2 Water and Soil Pollutants
- •4.2.1 Sources of Water and Soil Pollutants
- •4.2.2 Examples of Pollutants
- •4.3 Occupational Toxicants
- •4.3.1 Regulation of Exposure Levels
- •4.3.2 Routes of Exposure
- •4.3.3 Examples of Industrial Toxicants
- •Suggested Reading
- •5 Classes of Toxicants: Use Classes
- •5.1 Introduction
- •5.2 Metals
- •5.2.1 History
- •5.2.2 Common Toxic Mechanisms and Sites of Action
- •5.2.3 Lead
- •5.2.4 Mercury
- •5.2.5 Cadmium
- •5.2.6 Chromium
- •5.2.7 Arsenic
- •5.2.8 Treatment of Metal Poisoning
- •5.3 Agricultural Chemicals (Pesticides)
- •5.3.1 Introduction
- •5.3.3 Organochlorine Insecticides
- •5.3.4 Organophosphorus Insecticides
- •5.3.5 Carbamate Insecticides
- •5.3.6 Botanical Insecticides
- •5.3.7 Pyrethroid Insecticides
- •5.3.8 New Insecticide Classes
- •5.3.9 Herbicides
- •5.3.10 Fungicides
- •5.3.11 Rodenticides
- •5.3.12 Fumigants
- •5.3.13 Conclusions
- •5.4 Food Additives and Contaminants
- •5.5 Toxins
- •5.5.1 History
- •5.5.2 Microbial Toxins
- •5.5.3 Mycotoxins
- •5.5.4 Algal Toxins
- •5.5.5 Plant Toxins
- •5.5.6 Animal Toxins
- •5.6 Solvents
- •5.7 Therapeutic Drugs
- •5.8 Drugs of Abuse
- •5.9 Combustion Products
- •5.10 Cosmetics
- •Suggested Reading
- •6 Absorption and Distribution of Toxicants
- •6.1 Introduction
- •6.2 Cell Membranes
- •6.3 Mechanisms of Transport
- •6.3.1 Passive Diffusion
- •6.4 Physicochemical Properties Relevant to Diffusion
- •6.4.1 Ionization
- •6.5 Routes of Absorption
- •6.5.1 Extent of Absorption
- •6.5.2 Gastrointestinal Absorption
- •6.5.3 Dermal Absorption
- •6.5.4 Respiratory Penetration
- •6.6 Toxicant Distribution
- •6.6.1 Physicochemical Properties and Protein Binding
- •6.7 Toxicokinetics
- •Suggested Reading
- •7 Metabolism of Toxicants
- •7.1 Introduction
- •7.2 Phase I Reactions
- •7.2.4 Nonmicrosomal Oxidations
- •7.2.5 Cooxidation by Cyclooxygenases
- •7.2.6 Reduction Reactions
- •7.2.7 Hydrolysis
- •7.2.8 Epoxide Hydration
- •7.2.9 DDT Dehydrochlorinase
- •7.3 Phase II Reactions
- •7.3.1 Glucuronide Conjugation
- •7.3.2 Glucoside Conjugation
- •7.3.3 Sulfate Conjugation
- •7.3.4 Methyltransferases
- •7.3.7 Acylation
- •7.3.8 Phosphate Conjugation
- •Suggested Reading
- •8 Reactive Metabolites
- •8.1 Introduction
- •8.2 Activation Enzymes
- •8.3 Nature and Stability of Reactive Metabolites
- •8.4 Fate of Reactive Metabolites
- •8.4.1 Binding to Cellular Macromolecules
- •8.4.2 Lipid Peroxidation
- •8.4.3 Trapping and Removal: Role of Glutathione
- •8.5 Factors Affecting Toxicity of Reactive Metabolites
- •8.5.1 Levels of Activating Enzymes
- •8.5.2 Levels of Conjugating Enzymes
- •8.5.3 Levels of Cofactors or Conjugating Chemicals
- •8.6 Examples of Activating Reactions
- •8.6.1 Parathion
- •8.6.2 Vinyl Chloride
- •8.6.3 Methanol
- •8.6.5 Carbon Tetrachloride
- •8.6.8 Acetaminophen
- •8.6.9 Cycasin
- •8.7 Future Developments
- •Suggested Reading
- •9.1 Introduction
- •9.2 Nutritional Effects
- •9.2.1 Protein
- •9.2.2 Carbohydrates
- •9.2.3 Lipids
- •9.2.4 Micronutrients
- •9.2.5 Starvation and Dehydration
- •9.2.6 Nutritional Requirements in Xenobiotic Metabolism
- •9.3 Physiological Effects
- •9.3.1 Development
- •9.3.2 Gender Differences
- •9.3.3 Hormones
- •9.3.4 Pregnancy
- •9.3.5 Disease
- •9.3.6 Diurnal Rhythms
- •9.4 Comparative and Genetic Effects
- •9.4.1 Variations Among Taxonomic Groups
- •9.4.2 Selectivity
- •9.4.3 Genetic Differences
- •9.5 Chemical Effects
- •9.5.1 Inhibition
- •9.5.2 Induction
- •9.5.3 Biphasic Effects: Inhibition and Induction
- •9.6 Environmental Effects
- •9.7 General Summary and Conclusions
- •Suggested Reading
- •10 Elimination of Toxicants
- •10.1 Introduction
- •10.2 Transport
- •10.3 Renal Elimination
- •10.4 Hepatic Elimination
- •10.4.2 Active Transporters of the Bile Canaliculus
- •10.5 Respiratory Elimination
- •10.6 Conclusion
- •Suggested Reading
- •11 Acute Toxicity
- •11.1 Introduction
- •11.2 Acute Exposure and Effect
- •11.3 Dose-response Relationships
- •11.4 Nonconventional Dose-response Relationships
- •11.5 Mechanisms of Acute Toxicity
- •11.5.1 Narcosis
- •11.5.2 Acetylcholinesterase Inhibition
- •11.5.3 Ion Channel Modulators
- •11.5.4 Inhibitors of Cellular Respiration
- •Suggested Reading
- •12 Chemical Carcinogenesis
- •12.1 General Aspects of Cancer
- •12.2 Human Cancer
- •12.2.1 Causes, Incidence, and Mortality Rates of Human Cancer
- •12.2.2 Known Human Carcinogens
- •12.3 Classes of Agents Associated with Carcinogenesis
- •12.3.2 Epigenetic Agents
- •12.4 General Aspects of Chemical Carcinogenesis
- •12.5 Initiation-Promotion Model for Chemical Carcinogenesis
- •12.6 Metabolic Activation of Chemical Carcinogens and DNA Adduct Formation
- •12.7 Oncogenes
- •12.8 Tumor Suppressor Genes
- •12.8.1 Inactivation of Tumor Suppressor Genes
- •12.8.2 p53 Tumor Suppressor Gene
- •12.9 General Aspects of Mutagenicity
- •12.10 Usefulness and Limitations of Mutagenicity Assays for the Identification of Carcinogens
- •Suggested Reading
- •13 Teratogenesis
- •13.1 Introduction
- •13.2 Principles of Teratology
- •13.3 Mammalian Embryology Overview
- •13.4 Critical Periods
- •13.5 Historical Teratogens
- •13.5.1 Thalidomide
- •13.5.2 Accutane (Isotetrinoin)
- •13.5.3 Diethylstilbestrol (DES)
- •13.5.4 Alcohol
- •13.6 Testing Protocols
- •13.6.1 FDA Guidelines for Reproduction Studies for Safety Evaluation of Drugs for Human Use
- •13.6.3 Alternative Test Methods
- •13.7 Conclusions
- •Suggested Reading
- •14 Hepatotoxicity
- •14.1 Introduction
- •14.1.1 Liver Structure
- •14.1.2 Liver Function
- •14.2 Susceptibility of the Liver
- •14.3 Types of Liver Injury
- •14.3.1 Fatty Liver
- •14.3.2 Necrosis
- •14.3.3 Apoptosis
- •14.3.4 Cholestasis
- •14.3.5 Cirrhosis
- •14.3.6 Hepatitis
- •14.3.7 Oxidative Stress
- •14.3.8 Carcinogenesis
- •14.4 Mechanisms of Hepatotoxicity
- •14.5 Examples of Hepatotoxicants
- •14.5.1 Carbon Tetrachloride
- •14.5.2 Ethanol
- •14.5.3 Bromobenzene
- •14.5.4 Acetaminophen
- •14.6 Metabolic Activation of Hepatotoxicants
- •Suggested Reading
- •15 Nephrotoxicity
- •15.1 Introduction
- •15.1.1 Structure of the Renal System
- •15.1.2 Function of the Renal System
- •15.2 Susceptibility of the Renal System
- •15.3 Examples of Nephrotoxicants
- •15.3.1 Metals
- •15.3.2 Aminoglycosides
- •15.3.3 Amphotericin B
- •15.3.4 Chloroform
- •15.3.5 Hexachlorobutadiene
- •Suggested Reading
- •16 Toxicology of the Nervous System
- •16.1 Introduction
- •16.2 The Nervous system
- •16.2.1 The Neuron
- •16.2.2 Neurotransmitters and their Receptors
- •16.2.3 Glial Cells
- •16.3 Toxicant Effects on the Nervous System
- •16.3.1 Structural Effects of Toxicants on Neurons
- •16.3.2 Effects of Toxicants on Other Cells
- •16.4 Neurotoxicity Testing
- •16.4.1 In vivo Tests of Human Exposure
- •16.4.2 In vivo Tests of Animal Exposure
- •16.4.3 In vitro Neurochemical and Histopathological End Points
- •16.5 Summary
- •Suggested Reading
- •17 Endocrine System
- •17.1 Introduction
- •17.2 Endocrine System
- •17.2.1 Nuclear Receptors
- •17.3 Endocrine Disruption
- •17.3.1 Hormone Receptor Agonists
- •17.3.2 Hormone Receptor Antagonists
- •17.3.3 Organizational versus Activational Effects of Endocrine Toxicants
- •17.3.4 Inhibitors of Hormone Synthesis
- •17.3.5 Inducers of Hormone Clearance
- •17.3.6 Hormone Displacement from Binding Proteins
- •17.4 Incidents of Endocrine Toxicity
- •17.4.1 Organizational Toxicity
- •17.4.2 Activational Toxicity
- •17.4.3 Hypothyroidism
- •17.5 Conclusion
- •Suggested Reading
- •18 Respiratory Toxicity
- •18.1 Introduction
- •18.1.1 Anatomy
- •18.1.2 Cell Types
- •18.1.3 Function
- •18.2 Susceptibility of the Respiratory System
- •18.2.1 Nasal
- •18.2.2 Lung
- •18.3 Types of Toxic Response
- •18.3.1 Irritation
- •18.3.2 Cell Necrosis
- •18.3.3 Fibrosis
- •18.3.4 Emphysema
- •18.3.5 Allergic Responses
- •18.3.6 Cancer
- •18.3.7 Mediators of Toxic Responses
- •18.4 Examples of Lung Toxicants Requiring Activation
- •18.4.1 Introduction
- •18.4.2 Monocrotaline
- •18.4.3 Ipomeanol
- •18.4.4 Paraquat
- •18.5 Defense Mechanisms
- •Suggested Reading
- •19 Immunotoxicity
- •19.1 Introduction
- •19.2 The Immune System
- •19.3 Immune Suppression
- •19.4 Classification of Immune-Mediated Injury (Hypersensitivity)
- •19.5 Effects of Chemicals on Allergic Disease
- •19.5.1 Allergic Contact Dermatitis
- •19.5.2 Respiratory Allergens
- •19.5.3 Adjuvants
- •19.6 Emerging Issues: Food Allergies, Autoimmunity, and the Developing Immune System
- •Suggested Reading
- •20 Reproductive System
- •20.1 Introduction
- •20.2 Male Reproductive Physiology
- •20.3 Mechanisms and Targets of Male Reproductive Toxicants
- •20.3.1 General Mechanisms
- •20.3.2 Effects on Germ Cells
- •20.3.3 Effects on Spermatogenesis and Sperm Quality
- •20.3.4 Effects on Sexual Behavior
- •20.3.5 Effects on Endocrine Function
- •20.4 Female Reproductive Physiology
- •20.5 Mechanisms and Targets of Female Reproductive Toxicants
- •20.5.1 Tranquilizers, Narcotics, and Social Drugs
- •20.5.2 Endocrine Disruptors (EDs)
- •20.5.3 Effects on Germ Cells
- •20.5.4 Effects on the Ovaries and Uterus
- •20.5.5 Effects on Sexual Behavior
- •Suggested Reading
- •21 Toxicity Testing
- •21.1 Introduction
- •21.2 Experimental Administration of Toxicants
- •21.2.1 Introduction
- •21.2.2 Routes of Administration
- •21.3 Chemical and Physical Properties
- •21.4 Exposure and Environmental Fate
- •21.5 In vivo Tests
- •21.5.1 Acute and Subchronic Toxicity Tests
- •21.5.2 Chronic Tests
- •21.5.3 Reproductive Toxicity and Teratogenicity
- •21.5.4 Special Tests
- •21.6 In vitro and Other Short-Term Tests
- •21.6.1 Introduction
- •21.6.2 Prokaryote Mutagenicity
- •21.6.3 Eukaryote Mutagenicity
- •21.6.4 DNA Damage and Repair
- •21.6.5 Chromosome Aberrations
- •21.6.6 Mammalian Cell Transformation
- •21.6.7 General Considerations and Testing Sequences
- •21.7 Ecological Effects
- •21.7.1 Laboratory Tests
- •21.7.2 Simulated Field Tests
- •21.7.3 Field Tests
- •21.8 Risk Analysis
- •21.9 The Future of Toxicity Testing
- •Suggested Reading
- •22 Forensic and Clinical Toxicology
- •22.1 Introduction
- •22.2 Foundations of Forensic Toxicology
- •22.3 Courtroom Testimony
- •22.4.1 Documentation Practices
- •22.4.2 Considerations for Forensic Toxicological Analysis
- •22.4.3 Drug Concentrations and Distribution
- •22.5 Laboratory Analyses
- •22.5.1 Colorimetric Screening Tests
- •22.5.2 Thermal Desorption
- •22.5.6 Enzymatic Immunoassay
- •22.6 Analytical Schemes for Toxicant Detection
- •22.7 Clinical Toxicology
- •22.7.1 History Taking
- •22.7.2 Basic Operating Rules in the Treatment of Toxicosis
- •22.7.3 Approaches to Selected Toxicoses
- •Suggested Reading
- •23 Prevention of Toxicity
- •23.1 Introduction
- •23.2 Legislation and Regulation
- •23.2.1 Federal Government
- •23.2.2 State Governments
- •23.2.3 Legislation and Regulation in Other Countries
- •23.3 Prevention in Different Environments
- •23.3.1 Home
- •23.3.2 Workplace
- •23.3.3 Pollution of Air, Water, and Land
- •23.4 Education
- •Suggested Reading
- •24 Human Health Risk Assessment
- •24.1 Introduction
- •24.2 Risk Assessment Methods
- •24.2.2 Exposure Assessment
- •24.2.3 Dose Response and Risk Characterization
- •24.3 Noncancer Risk Assessment
- •24.3.1 Default Uncertainty and Modifying Factors
- •24.3.2 Derivation of Developmental Toxicant RfD
- •24.3.3 Determination of RfD and RfC of Naphthalene with the NOAEL Approach
- •24.3.4 Benchmark Dose Approach
- •24.3.5 Determination of BMD and BMDL for ETU
- •24.3.6 Quantifying Risk for Noncarcinogenic Effects: Hazard Quotient
- •24.3.7 Chemical Mixtures
- •24.4 Cancer Risk Assessment
- •24.5 PBPK Modeling
- •Suggested Reading
- •25 Analytical Methods in Toxicology
- •25.1 Introduction
- •25.2 Chemical and Physical Methods
- •25.2.1 Sampling
- •25.2.2 Experimental Studies
- •25.2.3 Forensic Studies
- •25.2.4 Sample Preparation
- •25.2.6 Spectroscopy
- •25.2.7 Other Analytical Methods
- •Suggested Reading
- •26 Basics of Environmental Toxicology
- •26.1 Introduction
- •26.2 Environmental Persistence
- •26.2.1 Abiotic Degradation
- •26.2.2 Biotic Degradation
- •26.2.3 Nondegradative Elimination Processes
- •26.3 Bioaccumulation
- •26.4 Toxicity
- •26.4.1 Acute Toxicity
- •26.4.2 Mechanisms of Acute Toxicity
- •26.4.3 Chronic Toxicity
- •26.4.5 Abiotic and Biotic Interactions
- •26.5 Conclusion
- •Suggested Reading
- •27.1 Introduction
- •27.2 Sources of Toxicants to the Environment
- •27.3 Transport Processes
- •27.3.1 Advection
- •27.3.2 Diffusion
- •27.4 Equilibrium Partitioning
- •27.5 Transformation Processes
- •27.5.1 Reversible Reactions
- •27.5.2 Irreversible Reactions
- •27.6 Environmental Fate Models
- •Suggested Reading
- •28 Environmental Risk Assessment
- •28.1 Introduction
- •28.2 Formulating the Problem
- •28.2.1 Selecting Assessment End Points
- •28.2.2 Developing Conceptual Models
- •28.2.3 Selecting Measures
- •28.3 Analyzing Exposure and Effects Information
- •28.3.1 Characterizing Exposure
- •28.3.2 Characterizing Ecological Effects
- •28.4 Characterizing Risk
- •28.4.1 Estimating Risk
- •28.4.2 Describing Risk
- •28.5 Managing Risk
- •Suggested Reading
- •29 Future Considerations for Environmental and Human Health
- •29.1 Introduction
- •29.2 Risk Management
- •29.3 Risk Assessment
- •29.4 Hazard and Exposure Assessment
- •29.5 In vivo Toxicity
- •29.6 In vitro Toxicity
- •29.7 Biochemical and Molecular Toxicology
- •29.8 Development of Selective Toxicants
- •Glossary
- •Index

228 CHEMICAL CARCINOGENESIS
Table 12.1 Some General Characteristics of Malignant and Benign Neoplasms
Benign |
Malignant |
|
|
Generally slow growing |
May be slow to rapid growing |
Few mitotic figures |
Numerous mitotic figures |
Well-differentiated architecture, resembles that |
Some lack differentiation, disorganized; loss |
of parent tissue |
of parent tissue architecture |
Sharply demarcated mass that does not invade |
Locally invasive, infiltrating into |
surrounding tissue |
surrounding normal tissue |
No metastases |
Metastases |
|
|
are derived from blood-forming cells and lymphoid tissue. Melanoma is derived from melanocytes and retinoblastoma, glioblastoma, and neuroblastoma are derived from the stem cells of the retina, glia, and neurons, respectively. According to the American Cancer Society, (1) the lifetime risk for developing cancer in the United States is about 1 in 3 for women and 1 in 2 for men, (2) in 2003 about 1.3 million new cancer cases are expected to be diagnosed not including carcinoma in situ or basal or squamous cell skin cancer, and (3) cancer is a leading cause of death in the United States and approximately 25% of all deaths are due to cancer.
12.2HUMAN CANCER
Although cancer is known to occur in many groups of animals, the primary interest and the focus of most research is in human cancer. Nevertheless, much of the mechanistic research and the hazard assessment is carried out in experimental animals. A consideration of the general aspects of human carcinogenesis follows.
12.2.1Causes, Incidence, and Mortality Rates of Human Cancer
Cancer cases and cancer deaths by sites and sex for the United States are shown in Figure 12.4. Breast, lung, and colon and rectum cancers are the major cancers in females while prostate, lung, and colon and rectum are the major cancer sites in males. A comparison of cancer deaths versus incidence for a given site reveals that prognosis for lung cancer cases is poor while that for breast or prostate cancer cases is much better. Age-adjusted cancer mortality rates (1930–1998) for selected sites in males are shown in Figure 12.5 and for females is shown in Figure 12.6. The increase in the mortality rate associated with lung cancer in both females and males is striking and is due to cigarette smoking. It is estimated that 87% of lung cancers are due to smoking. Lung cancer death rates in males and females began to increase in the mid-1930s and mid-1960s, respectively. These time differences are due to the fact that cigarette smoking among females did not become popular until the 1940s while smoking among males was popular in the early 1900s. Taking into account these differences along with a 20 to 25 year lag period for the cancer to develop explains the differences in the temporal increase in lung cancer death rates in males and female. Another disturbing statistic is that lung cancer, a theoretically preventable cancer, has recently surpassed breast cancer as the cancer responsible for the greatest number of cancer deaths in

|
|
|
HUMAN CANCER |
229 |
|
Cancer Cases by Site and Sex |
|
Cancer Deaths by Site and Sex |
|
||
Male |
Female |
|
Male |
Female |
|
Prostate |
Breast |
|
Lung & bronchus |
Lung & bronchus |
|
189,000 (30%) |
203,500 (31%) |
|
89,200 (31%) |
65,700 (25%) |
|
Lung & bronchus |
Lung & bronchus |
|
Prostate |
Breast |
|
90,200 (14%) |
79,200 (12%) |
|
30,200 (11%) |
39,600 (15%) |
|
Colon & rectum |
Colon & rectum |
|
Colon & rectum |
Colon & rectum |
|
72,600 (11%) |
75,700 (12%) |
|
27,800 (10%) |
28,800 (11%) |
|
Urinary bladder |
Uterine corpus |
|
Pancreas |
Pancreas |
|
41,500 (7%) |
39,300 (6%) |
|
14,500 (5%) |
15,200 (6%) |
|
Melanoma of the skin |
Non-Hodgkin's lymphoma |
Non-Hodgkin's lymphoma |
Ovary |
|
|
30,100 (5%) |
25,700 (4%) |
|
12,700 (5%) |
13,900 (5%) |
|
Non-Hodgkin's lymphoma |
Melanoma of the skin |
|
Leukemia |
Non-Hodgkin's lymphoma |
|
28,200 (4%) |
23,500 (4%) |
|
12,100 (4%) |
11,700 (4%) |
|
Kidney |
Ovary |
|
Esophagus |
Leukemia |
|
19,100 (3%) |
23,300 (4%) |
|
9,600 (3%) |
9,600 (4%) |
|
Oral cavity |
Thyroid |
|
Liver |
Uterine corpus |
|
18,900 (3%) |
15,800 (2%) |
|
8,900 (3%) |
6,600 (2%) |
|
Leukemia |
Pancreas |
|
Urinary bladder |
Brain |
|
17,600 (3%) |
15,600 (2%) |
|
8,600 (3%) |
5,900 (2%) |
|
Pancreas |
Urinary bladder |
|
Kidney |
Multiple myeloma |
|
14,700 (2%) |
15,000 (2%) |
|
7,200 (3%) |
5,300 (2%) |
|
All Sites |
All Sites |
|
All Sites |
All Sites |
|
637,500 (100%) |
647,400 (100%) |
|
288,200 (100%) |
267,300 (100%) |
|
*Excludes basal and squamous cell skin cancers and in situ carcinoma |
|
©2002, American Cancer Society, Inc., |
|
||
except urinary bladder. Percentages may not total 100% due to rounding. |
Surveillance Research |
|
|||
Figure 12.4 Cancer cases and cancer deaths by sites and sex: 2002 estimates. (From American Cancer Society’s Facts and Figures—2002, reprinted with permission of the American Cancer Society, Inc.)
women. In addition to lung cancer, smoking also plays a significant role in cancer of the mouth, esophagus, pancreas, pharynx, larynx, bladder, kidney, and uterine cervix. Overall, the age-adjusted national total cancer death rate is increasing. In 1930 the number of cancer deaths per 100,000 people was 143. In 1940, 1950, 1970, 1984, and 1992 the rate had increased to 152, 158, 163, 170, and 172, respectively. According to the American Cancer Society, when lung cancer deaths due to smoking are excluded, the total age-adjusted cancer mortality rate had actually decreased by 16% between 1950 and 1993. However, it is important to realize that death and incidence rates for some types of cancers are increasing while the rates for others are decreasing or remaining constant.
Major insights into the etiologies of cancer have been attained through epidemiological studies that relate the roles of hereditary, environmental, and cultural influences on cancer incidence as well as through laboratory studies using rodent/cellular systems. Cancer susceptibility is determined by complex interactions between age, environment, and an individual’s genetic makeup. It is estimated from epidemiological studies that 35–80% of all cancers are associated with the environment in which we live and work. The geographic migration of immigrant populations and differences in cancer incidence among communities has provided a great deal of information regarding the role of the environment and specific cancer incidences. For example, Japanese immigrants and the sons of Japanese immigrants living in California begin to assume a cancer death rate similar to the California white population (Figure 12.7). These results implicate

230 |
CHEMICAL CARCINOGENESIS |
|
|
|
|
||
|
80 |
|
|
|
Lung & |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Bronchus |
|
|
male population |
60 |
|
|
|
|
|
|
40 |
|
|
|
|
|
|
|
100,000 |
|
|
|
|
|
|
|
|
|
Stomach |
|
Colon & |
Prostate |
|
|
|
|
|
|
|
|||
|
|
|
|
Rectum |
|
|
|
Rate per |
|
|
|
|
|
|
|
20 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Pancreas |
|
|
|
|
|
Leukemia |
|
|
|
|
|
Liver |
|
|
|
|
|
0 |
|
|
|
|
|
|
|
1930 |
1940 |
1950 |
1960 |
1970 |
1980 |
1990 |
*Per 100,000, age-adjusted to the 1970 US standard population. Note: Due to changes in ICD coding, numerator information has changed over time. Rates for cancers of the liver, lung & bronchus, and colon & rectum are affected by these coding changes.
Source: US Mortality Public Use Data Tapes 1960-1998, US Mortality Volumes 1930-1959, National Center for Health Statistics, Centers for Disease Control and Prevention, 2001.
American Cancer Society, Surveillance Research, 2002
Figure 12.5 Age-adjusted mortality rates (1030–1998) for selected sites in males. (From American Cancer Society’s Facts and Figures—2002, reprinted with permission of the American Cancer Society, Inc.)
a role of the environment in the etiology of cancer. It should be noted that the term environment is not restricted to exposure to human-made chemicals in the environment but applies to all aspects of our lifestyle including smoking, diet, cultural and sexual behavior, occupation, natural and medical radiation, and exposure to substances in air, water, and soil. The major factors associated with cancer and their estimated contribution to human cancer incidence are listed in Table 12.2. Only a small percentage of total cancer occurs in individuals with a hereditary mutation/hereditary cancer syndrome (ca. 5%). However, an individual’s genetic background is the “stage” in which the cancer develops and susceptibility genes have been identified in humans. For example, genetic polymorphisms in enzymes responsible for the activation of chemical carcinogens may represent a risk factor as is the case for polymorphisms in the N-acetyl-transferase gene and the risk of bladder cancer. These types of genetic risk factors are of low penetrance (low to moderate increased risk); however, increased risk is usually associated with environmental exposure. While the values presented in Table 12.2 are a best estimate, it is clear that smoking and diet constitute the major factors associated with human cancer incidence. If one considers all of the categories that pertain to human-made chemicals, it is estimated that their contribution to human

|
|
|
|
|
|
HUMAN CANCER |
231 |
|
|
80 |
|
|
|
|
|
|
|
female population |
60 |
|
|
|
|
|
|
|
40 |
|
|
|
|
|
|
|
|
Rate per 100,000 |
|
|
|
|
|
|
|
|
|
Uterust |
|
|
|
Lung & |
|
|
|
|
|
|
Breast |
|
Bronchus |
|
|
|
|
|
|
|
|
|
|
||
20 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Stomach |
|
|
|
|
Colon & |
|
|
|
|
|
|
|
|
|
|
|
|
Ovary |
|
|
|
|
Rectum |
|
|
|
|
|
|
|
|
|
|
|
|
0 |
|
|
Pancreas |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
1930 |
1940 |
1950 |
1960 |
1970 |
1980 |
1990 |
|
*Per 100,000, age-adjusted to the 1970 US standard population. †Uterus cancer death rates are for uterine cervix and uterine corpus combined.
Note: Due to changes in ICD coding, numerator information has
changed over time. Rates for cancers of the liver, lung & bronchus, and colon & rectum are affected by these coding changes.
Source: US Mortality Public Use Data Tapes 1960–1998, US Mortality Volumes 1930–1959, National Center for Health Statistics, Centers for Disease Control and Prevention, 2001.
American Cancer Society, Surveillance Research, 2002
Figure 12.6 Age-adjusted mortality rates (1030–1998) for selected sites in females. (From
American Cancer Society’s Facts and Figures—2002, reprinted with permission of the American Cancer Society, Inc.)
cancer incidence is approximately 10%. However, the factors listed in Table 12.2 are not mutually exclusive since there is likely to be interaction between these factors in the multi-step process of carcinogenesis.
12.2.2Known Human Carcinogens
Two of the earliest observations that exposure of humans to certain chemicals or substances is related to an increased incidence of cancer were made independently by two English physicians, John Hill in 1771 and Sir Percival Pott in 1776. Hill observed an increased incidence of nasal cancer among snuff users, while Pott observed that chimney sweeps had an increased incidence of scrotal cancer. Pott attributed this to topical exposure to soot and coal tar. It was not until nearly a century and a half later in 1915 when two Japanese scientists, K. Yamagiwa and K. J. Itchikawa, substantiated Pott’s observation by demonstrating that multiple topical applications of coal tar to rabbit skin produced skin carcinomas. This experiment is important for two major
232 CHEMICAL CARCINOGENESIS
Japan |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Japanese |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||
Immigrants |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
to California |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
stomach |
|
|
||||
Sons of |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
liver |
|
|
|||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||||||
Japanese |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||||
Immigrants |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
colon |
|
|
||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
prostate |
|
|
||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||
California |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||
Whites |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
0 |
1 |
2 |
3 |
4 |
5 |
6 |
|
7 |
|||||||||||||
|
|
|
|
|
|
|
|
Death Rate From Cancers |
|
|
|||||||||||
|
|
|
|
(Compared With Rate for California Whites) |
|
|
|||||||||||||||
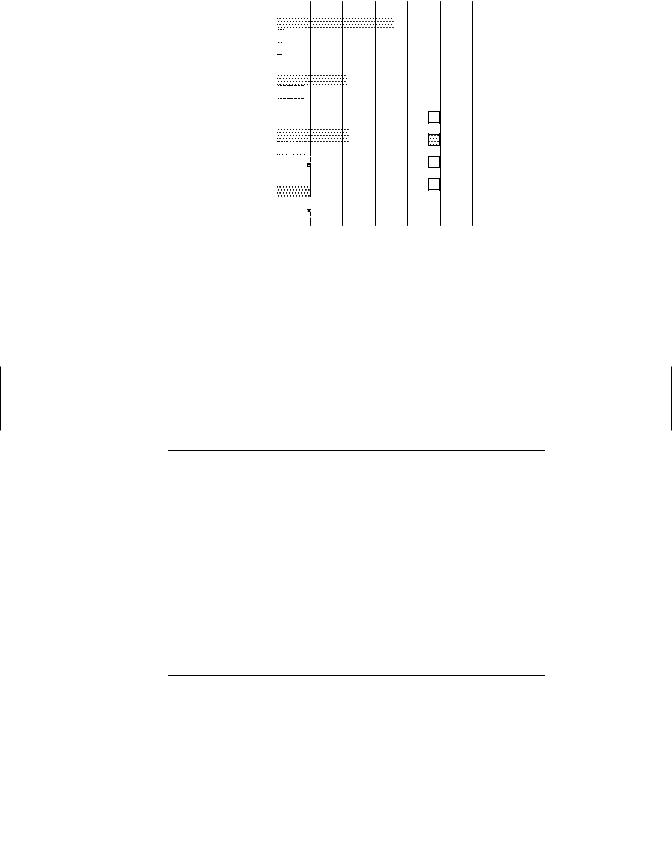
Figure 12.7 Change in incidence of various cancers with migration from Japan to the United States provides evidence that the cancers are caused by components of the environment that differ in the two countries. The incidence of each kind of cancer is expressed as the ratio of the death rate in the populations being considered to that in a hypothetical population of California whites with the same age distribution; the death rates for whites are thus defined as 1. (Adapted from J. Cairns, in Readings from Scientific American-Cancer Biology, W. H. Freeman, 1986, p. 13.)
Table 12.2 Proportions of Cancer Deaths Attributed to Various Different Factors
|
Best Estimate |
Range of Acceptable |
|
Major Factors |
(%) |
Estimates (%) |
|
|
|
|
|
Diet |
35 |
10 |
–70 |
Tobacco |
30 |
25 |
–40 |
Infection |
10 |
1 |
–? |
Reproductive and sexual behavior |
7 |
1 |
–13 |
Occupation |
4 |
2 |
–8 |
Geophysical factors |
3 |
2 |
–4 |
Alcohol |
3 |
2 |
–4 |
Pollution |
2 |
<1 |
–5 |
Food additives |
1 |
−5 |
–2 |
Medicines |
1 |
0.5 |
–3 |
Industrial products |
1 |
<1 |
–2 |
Unknown |
? |
|
? |
Source: Adapted from R. Doll and R. Peto, The Causes of Cancer, Oxford Medical Publications, 1981.

HUMAN CANCER |
233 |
reasons: (1) it was the first demonstration that a chemical or substance could produce cancer in animals, and (2) it confirmed Pott’s initial observation and established a relationship between human epidemiology studies and animal carcinogenicity. Because of these important findings, Yamagiwa and Itchikawa are considered the fathers of experimental chemical carcinogenesis. In the 1930s Kennaway and coworkers isolated a single active carcinogenic chemical from coal tar and identified it as benzo[a]pyrene, a polycyclic aromatic hydrocarbon that results from the incomplete combustion of organic molecules. Benzo[a]pyrene has also been identified as one of the carcinogens in cigarette smoke. The p53 tumor suppressor gene can be mutationally inactivated by numerous carcinogens, including the carcinogenic metabolite of benzo[a]pyrene.
Epidemiological studies have provided sufficient evidence that exposure to a variety of chemicals, agents, or processes are associated with human cancer. For example, the following causal associations have emerged between exposure and the development of specific cancers: vinyl chloride and hepatic cancer, amine dyes and bladder cancer, benzene and leukemia, diethylstilbestrol and clear cell carcinoma of the vagina, and cigarette smoking and lung cancer. Naturally occurring chemicals or agents such as asbestos, aflatoxin B1, betel nut, nickel, and certain arsenic compounds are also associated with an increased incidence of certain human cancers. Both epidemiological studies and rodent carcinogenicity studies are important in the identification and classification of potential human carcinogens. The strongest evidence for establishing whether exposure to a given chemical is carcinogenic in humans comes from epidemiological studies. However, these studies are complicated by the fact that it often takes 20 to 30 years after carcinogen exposure for a clinically detectable cancer to develop. This delay is problematic and can result in inaccurate historical exposure information and additional complexity due to the interference of a large number of confounding variables. This lag period can also prevent the timely identification of a putative carcinogen and result in unnecessary exposure. Therefore methods to identify potential human carcinogens have been developed. The long-term rodent bioassay also known as the two-year rodent carcinogenesis bioassay (see Chapter 21) is currently used in an attempt to identify potential human carcinogens. It is clear that almost all human carcinogens identified to date are rodent carcinogens; however, it is not known if all rodent carcinogens are human carcinogens. Indeed, identification of possible human carcinogens based on rodent carcinogenicity can be extremely complicated (see below). Table 12.3 contains the list of the known human carcinogens as listed by the International Agency for Research on Cancer (IARC). In addition Table 12.3 includes information on carcinogenic complex mixtures and occupations associated with increased cancer incidence. In vitro mutagenicity assays are also used to identify mutagenic agents that may have carcinogenic activity (see Chapter 21).
12.2.3Classification of Human Carcinogens
Identification and classification of potential human carcinogens through the two-year rodent carcinogenesis bioassay is complicated by species differences, use of high doses (MTD, maximum tolerated dose), the short life span of the rodents, high background tumor incidence in some organs, sample size, and the need to extrapolate from high to low doses for human risk assessment. Although these problems are by no means trivial, the rodent two-year bioassay remains the “gold standard” for the classification

234 CHEMICAL CARCINOGENESIS
Table 12.3 List of Agents, Substances, Mixtures, and Exposure Circumstances Known to be Human Carcinogens
Aflatoxins 4-Aminobiphenyl
Arsenic and certain arsenic compounds Asbestos
Azathioprine Benzene Benzidine
Beryllium and certain beryllium compounds N,N-bis-(2-Chloroethyl)-2-naphthylamine (chlornaphazine) Bis(chloromethyl) ether and chloromethyl methyl ether 1,4-Butanediol dimethylsulfonate (Myleran )
Cadmium and certain cadmium compounds Chlorambucil
1-(2-Chloroethyl)-3-(4-methylcyclohexyl)-1-nitrosourea (MeCCNU) Chromium and certain chromium compounds
Cyclophosphamide Cyclosporin A (cyclosporin) Diethylstilbestrol Epstein-Barr virus
Erionite Estrogen therapy
Estrogens, nonsteroidal Estrogens, steroidal Ethylene oxide
Etoposide in combination with cisplatin and bleomycin
Helicobacter pylori
Hepatitis B virus (chronic infection) Hepatitis C virus (chronic infection)
Herbal remedies containing plant species of the genus Aristolochia Human immunodeficiency virus, type 1
Human papillomavirus, type 16 Human papillomavirus, type 18
Human T-cell lymphotropic virus, type 1 Melphalan
Methoxsalen with ultraviolet A therapy (PUVA)
MOPP and other combined chemotherapy including alkylating agents Mustard gas
2-Naphthylamine Neutrons
Nickel compounds
Opisthorchis viverrini
Oral contraceptives Radionuclides α-particle emitting Radionuclides β-particle emitting Radon
Schistosoma haematobium
Silica
Solar radiation
Talc containing asbestiform fibers

HUMAN CANCER |
235 |
Table 12.3 (continued )
Tamoxifen 2,3,7,8-Tetrachlorodibenzo-para-dioxin Thiotepa [tris(1-aziridinyl)phosphine sulfide] Thorium dioxide
Treosulfan Vinyl chloride
X and gamma(γ ) Radiation
Mixtures
Alcoholic beverages
Analgesic mixtures containing phenacetin
Betel quid with tobacco
Coal tar and coal pitches
Mineral oils
Salted fish
Shale oils
Soots
Tobacco smoke and tobacco smokeless products
Wood dust
Exposure circumstances
Aluminium production
Auramine manufacture
Boot and show manufacture and repair
Coal gasification
Coke gasification
Furniture and cabinet making
Haematite mining with exposure to radon
Iron and steel founding
Isopropanol manufacture
Manufacture of magenta
Painter
Rubber industry
Strong inorganic acid mists containing sulfuric acid
of potential human carcinogens. Criteria for the classification of carcinogens used by the National Toxicology Program’s Tenth Report on Carcinogens, 2002, are shown in Table 12.4; the criteria used by Environmental Protection Agency (EPA) and the International Agency for Research on Cancer (IARC) are shown in Table 12.5. Carcinogens are classified by the weight of evidence for carcinogenicity referred to as sufficient, limited, or inadequate based on both epidemiological studies and animal data. EPA is planning to change their guidelines for carcinogen risk assessment and their carcinogen classification scheme. New guidelines will emphasize the incorporation of biological mechanistic data in the analysis, and will not rely solely on rodent tumor data. In addition the six alphanumeric categories listed in Table 12.5 will be replaced by three descriptors for classifying human carcinogenic potential. Carcinogens will be classified by the EPA as (1) known/likely to be a human carcinogen, (2) cannot be determined to be a human carcinogen, and (3) not likely to be a human carcinogen.
- #15.08.20134.04 Mб17Hastie T., Tibshirani R., Friedman J. - The Elements of Statistical Learning Data Mining, Inference and Prediction (2002)(en).djvu
- #
- #
- #
- #
- #
- #
- #
- #15.08.201315.44 Mб27Hudlicky M, Pavlath A.E. (eds.) - Chemistry of Organic Fluorine Compounds 2[c] A critical Review (1995)(en).djvu
- #
- #
