
Gale Encyclopedia of Genetic Disorder / Gale Encyclopedia of Genetic Disorders, Two Volume Set - Volume 2 - M-Z - I
.pdfpockets of pus that form around infections in the skin or in the body organs.
Diagnosis
About half of children who see a doctor for frequent infections are normal; another 30% may have allergies, 10% have some other type of serious disorder, and 10% have a primary or secondary immunodeficiency. A diagnosis of SCID is usually made based on a complete medical history and physical examination, in addition to multiple blood tests and chest x rays. The gene in X- linked recessive SCID is called the interleukin receptor gamma chain gene or IL2RG. The autosomal recessive forms of SCID are caused by a variety of different genes; one of the more common is called the adenosine deaminase gene or ADA. Since newborns do not routinely have a test to count white blood cells, SCID is not usually suspected and then diagnosed until the child develops their first infection. A pattern of recurrent infections suggests an immunodeficiency.
Once a couple has had a child with SCID, and they have had the genetic cause identified by DNA studies (performed from a small blood sample), prenatal testing for future pregnancies may be considered on a research basis for some types of SCID. (Note that prenatal testing may not be possible if a mutation cannot be identified). Prenatal diagnosis is available via either CVS (chorionic villus sampling) or amniocentesis. CVS is a biopsy of the placenta performed in the first trimester or the first 12 weeks of pregnancy under ultrasound guidance. Ultrasound is the use of sound waves to visualize the locations of the developing baby and the placenta. The genetic makeup of the placenta is identical to the fetus (developing baby) and therefore the prescence or absence of one of the SCID genes can be determined from this tissue. Amniocentesis is a procedure performed under ultrasound guidance where a long thin needle is inserted into the mother’s abdomen, into the uterus, to withdraw a couple of tablespoons of amniotic fluid (fluid surrounding the developing baby) to study. The SCID gene can be studied using cells from the amniotic fluid. Other genetic tests, such as a chromosome analysis, may also be performed on either a CVS or amniocentesis. A small risk of miscarriage is associated with CVS and amniocentesis.
Treatment and management
The best treatment for SCID is a bone marrow transplant (BMT). A bone marrow transplant involves taking cells that are normally present in bone marrow (the center of bones that produce and store blood cells), and giving them back to the child with SCID or to another
person. The goal of BMT is to infuse healthy bone marrow cells into a person after their own unhealthy bone marrow has been eliminated. BMT helps to strengthen a child with SCID’s immune system.
Other treatment for SCID includes treating each infection promptly and accurately. Injections are also available to help boost a child’s immune system.
In the year 2000, gene therapy was first reported to be successful in two French patients with SCID. The idea behind gene therapy is to replace an abnormal gene with a normal copy. In SCID, bone marrow is removed to isolate the patients’ stem cells. Stem cells are special cells in the bone marrow that produce lymphocytes. In a laboratory, the normal gene is added to the abnormal stem cells. The genetically altered stem cells now have the normal gene and are transplanted back into the patient. Once the functioning stem cells with the normal gene enter the bone marrow, they reproduce quickly and replace stem cells that have the abnormal gene. So, ultimately, the patient with SCID produces B and T cells normally and can fight off infections without antibiotics or other treatment. The long-term effects of gene therapy are unknown, since the children treated are still very young.
Prognosis
When SCID is diagnosed early, successful bone marrow transplantation usually corrects the problem and the child lives a normal life. This means children can go to school, mix with playmates, and take part in sports. However, the quality of life for individuals with severe cases of SCID can be greatly impaired if they do not receive a bone marrow transplant. Children with SCID may not live long if they do not receive the proper treatment or if their disease goes undiagnosed.
Resources
PERIODICALS
Buckley, Rebecca H. “Gene Therapy for Human SCID: Dreams Become Reality.” Nature Medicine 6 (June 2000): 623.
Stephenson, Joan. “Gene Therapy Trials Show Efficacy.”
Journal of the American Medical Association 283 (February 2, 2000): 589.
ORGANIZATIONS
Immune Deficiency Foundation. 40 W. Chesapeake Ave., Suite 308, Towson, MD 21204. (800) 296-4433. Fax: (410) 3219165. http://www.primaryimmune.org .
National Organization for Rare Disorders (NORD). PO Box 8923, New Fairfield, CT 06812-8923. (203) 746-6518 or (800) 999-6673. Fax: (203) 746-6481. http://www
.rarediseases.org .
WEBSITES
International Patient Organization for Patients with Primary
Immunodeficiencies. www.ipopi.org .
immunodeficiency combined Severe
G A L E E N C Y C L O P E D I A O F G E N E T I C D I S O R D E R S |
1043 |
Short-rib polydactyly
Pediatric Primary ImmuneDeficiency. www.pedpid.com .
Severed Combined ImmuneDeficiency Homepage.
www.scid.net .
Catherine L. Tesla, MS, CGC
I Short-rib polydactyly
Definition
Short-rib polydactyly (SRP) syndromes are a group of skeletal dysplasias consisting of short ribs, short limbs, extra fingers or toes, and various internal organ abnormalities present at birth. There are four types of SRP and all are fatal shortly after birth due to underdevelopment of the lungs.
Description
In 1972, R. M. Saldino and C. D. Noonan first described two siblings with a dwarfism syndrome and symptoms of extremely shortened limbs, short ribs, small chest, abnormal bone formation, extra fingers, and internal organ damage. Since then, three additional SRP subtypes have been identified, all named after those who first described them. The subtypes are: SRP type I (SaldinoNoonan), SRP type II (Majewski), SRP type III (VermaNamauf), and SRP type IV (Beemer-Langer). While each subtype has distinguishing features, there is a great amount of overlap between them. There is still debate about whether the different types are caused by different genetic changes or if they result from the same genetic change and are variable between patients. Some people believe that the subtypes are different expressions of a single syndrome.
The SRP syndromes also overlap with two other dwarfism syndromes, asphyxiating thoracic dysplasia (Jeune syndrome) and Ellis van Creveld syndrome. These syndromes, like the SRP types, have shortened limbs and ribs, small chest, and extra fingers or toes. These syndromes may all be genetically related.
The exact cause of these syndromes is unknown but they all result in abnormal bone development and growth prenatally. This causes shortened bones in the arms, legs, and ribcage. The ribcage is also constricting, leaving very little room for the lung growth. Development can also be abnormal in the internal organs, including the heart, kidneys, liver, and pancreas. The cause of death for these newborns is usually inability to breathe due to severely underdeveloped lungs.
Short-rib Polydactyly Syndrome |
|
Short ribs |
Extra fingers and toes |
Extra fingers and toes |
Kidney cysts |
Congenital heart defect |
Cleft lip and cleft palate |
Constricted chest, lung problems |
|
(Gale Group)
Genetic profile
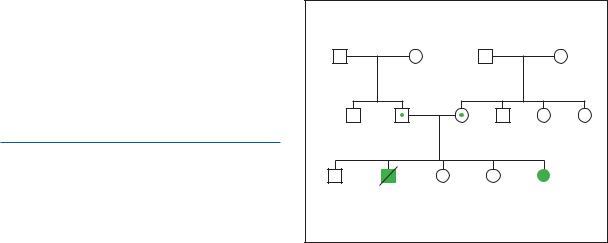
Even though the exact genetic cause of the SRP syndromes is unknown, it is well-documented that they are inherited as autosomal recessive conditions. This is because babies with SRP are born to unaffected parents and many parents have had more than one affected child. Parents of an affected child are assumed to be carriers. Those parents have a 25% chance of having another affected child with each pregnancy.
The gene (or genes) involved in the SRP syndromes has not yet been identified but is suspected to be on chromosome 4. Some researchers feel that the SRP gene is near the region of the gene for Ellis van Creveld syndrome on chromosome 4. The gene for another dwarfism syndrome, thanatophoric dysplasia, is also located in this area. Research is still being done to find the SRP gene (or genes) and learn more about its role during early development.
Demographics
Approximately 2-3 births per 10,000 are affected with some type of skeletal dysplasia. The SRP syndromes account for a small percentage of these. Due to the rarity of the SRP syndromes, an exact incidence is unknown.
Signs and symptoms
There is much overlap of symptoms between the SRP subtypes and it is often difficult to distinguish between them. They all have extremely shortened bones of the arms, legs, and ribs. They all also have a small, constricted chest.
Saldino-Noonan (type I) is considered the most severe type. Features reported with this type include spur
1044 |
G A L E E N C Y C L O P E D I A O F G E N E T I C D I S O R D E R S |

polydactyly rib-Short
These two x rays illustrate the developmental differences between a normal infant (left) and that of an infant with short ribpolydactyly syndrome. (Greenwood Genetic Center)
formation on the bones, abnormal vertebrae (bones of the spinal column), and decreased ossification (hardening of the bones). Heart defects are common. Cysts are often seen on the kidneys and pancreas. Extra fingers and/or toes (polydactyly) are a classic feature and are usually on the same side of the hand/foot as the “pinkie” finger/little toe (postaxial). Sex reversal has also been reported. This means that the baby is genetically male but has visible female genitalia.
Majewski (type II) also has cystic kidneys and postaxial polydactyly. This type can also have preaxial polydactyly where the extra fingers/toes are on the same side of the hand/foot as the thumb/big toe. Other distinguishing features include cleft lip and palate and liver damage. The tibia (one of the bones of the lower leg) is often oval shaped and shorter than the fibula (the other bone of the lower leg). The ends of the bones may also appear smooth on an x ray.
Verma-Namauf (type III) has much overlap with Saldino-Noonan (type I) and may be a milder variant. Internal organ involvement is less common. The ends of the bones may appear jagged and widened on an x ray. The vertebrae are often small and flat. Polydactyly is also common in this type. Visible genitalia may be ambiguous (not clearly male or female).
Beemer-Langer (type IV), like Majewski, can have cleft lip and palate and liver damage. Cysts on the kidneys and pancreas are common. Polydactyly is usually absent but has been reported. A distinguishing feature of this type is bowed or curved bones.
Diagnosis
Diagnosis of the SRP syndromes can be difficult. A careful examination of internal organs and x ray evaluation is needed to distinguish SRP syndromes from
G A L E E N C Y C L O P E D I A O F G E N E T I C D I S O R D E R S |
1045 |

Shprintzen-Goldberg craniosynostosis syndrome
K E Y T E R M S
Dwarfism—Any condition that results in extremely shortened limbs.
Skeletal dysplasia—A group of syndromes consisting of abnormal prenatal bone development and growth.
Jeune syndrome and Ellis van Creveld syndrome. When SRP syndrome is suspected, x rays and internal organ involvement can also help to determine the particular type.
The main features of SRP syndromes (short bones, short ribs, small chest) can be seen on prenatal ultrasound. This is the only method of prenatal diagnosis for at-risk families. Genetic testing for the SRP syndromes is not available.
Treatment and management
There is no treatment or cure for the SRP syndromes. The abnormal prenatal bone development is irreversible. The chest is usually too small to allow for lung growth after birth. Internal organs with cysts may not be functional.
Infants born with SRP syndromes are given minimum care for warmth and comfort. Due to the poor prognosis, extreme measures to prolong life are rarely taken.
Prognosis
The prognosis for infants born with SRP syndromes is quite poor. These babies usually die within hours or days of birth due to underdeveloped lungs.
Resources
PERIODICALS
Sarafoglou, K., et al. “Short-rib Polydactyly: More Evidence of a Continuous Spectrum.”Clinical Genetics 56 (1999):145148.
ORGANIZATIONS
SRPS Family Network. http://www.srps.net .
WEBSITES
“Short Rib-Polydactyly Syndrome, Type 1.” Online Mendelian Inheritance in Man. http://ncbi.nlm.nih.gov/entrez/ dispomim.cgi?id=263530 .
Amie Stanley, MS
I Shprintzen-Goldberg
craniosynostosis syndrome
Definition
Shprintzen-Goldberg craniosynostosis syndrome (SGS) is a disorder of the connective tissue, featuring craniosynostosis and marfanoid body type.
Description
SGS, also known as marfanoid craniosynostosis syndrome, is one of a group of disorders characterized by craniosynostosis and marfanoid body type. It is a condition that involves craniofacial, skeletal, and other abnormalities. SGS is caused by genetic mutations (changes affecting the structure and function of the gene) in a gene that contributes to the formation of connective tissue.
Genetic profile
SGS is associated with abnormalities of the elastic fibers of connective tissue. Elastic fibers are complex in structure and are composed of at least 19 different proteins. Mutations in three of the genes that encode the majority of these 19 proteins cause abnormalities in several body systems, including the skeletal system, blood vessels, and eye.
SGS shares characteristics with the Marfan syndrome, which is an inherited genetic disorder of the connective tissue which involves the eye, heart, aorta, and skeletal system. Marfan syndrome is caused by mutations in the fibrillin-1 (FBN1) gene, which is located on chromosome 15. Since SGS is similar in many ways to Marfan syndrome, studies of the FBN1 gene were conducted on SGS patients to see if they also had mutations in this gene. There were indeed abnormalities found in the FBN1 genes of persons with SGS. Researchers think that these mutations predispose a person to develop SGS, but that other factors are required in addition to the mutation in the gene to develop the disease. The other factors may be genetic mutations, environmental influences, or a combination of these, but they are not well-understood at this time.
The mutations appear to be sporadic in nature (not inherited), and are autosomal dominant (only one mutation is necessary to be predisposed to the disease). Sporadic genetic mutations in the sperm occur (in any gene, not just FBN1) at a higher rate in older men (over 45 years) and there is in fact one case report of a child with SGS in which the father was 49 years old. The father of another child with SGS reportedly had chemotherapy and radiation treatment prior to conception of the child.
1046 |
G A L E E N C Y C L O P E D I A O F G E N E T I C D I S O R D E R S |

The recurrence risk for siblings is probably low, although such data is not available.
Demographics
There are 15 reported cases as of 2000, with the first case being described in 1981. The ratio of females to males is 10:5, making females affected twice as often as males. Ethnicities would be expected to be affected equally with sporadic mutations, although data regarding SGS specifically is limited.
Signs and symptoms
Findings in SGS include skeletal abnormalities, hydrocephalus, and mental retardation. Most babies have been born well-nourished and had a relatively long birth length. The most frequently described craniofacial features of SGS include abnormal head shape (dolichocephaly), a high, prominent forehead, bulging eyes (ocular proptosis), wide spaced eyes (hypertelorism), downslanting eyes, strabismus (wandering eye), small jaw (maxillary hypoplasia), high narrow palate (roof of the mouth), and low-set ears.
The main skeletal findings in persons with SGS include long, thin fingers (arachnodactyly—or spiderlike fingers), flat feet (pes planus), “bird” chest deformity (pectus deformity), scoliosis (curvature of the spine), and joint hypermobility (loose joints).
Other features can include clubfoot, enlarged aortic root, mitral valve prolapse (floppy heart valve which allows flow of blood back into the chamber of the heart that it came from), low muscle tone (hypotonia), developmental delay, mental retardation, very little body fat, and small penis in males. Myopia (near-sightedness) and abdominal wall defects (developmental problem that occurs during formation of the fetus where parts of the intestine or other organs can protrude outside of the body; usually surgically correctable) can also occur.
Radiologic findings include hydrocephalus (water on the brain), certain brain malformations (Chiari-I malformation or dilatation of the lateral ventricles), abnormalities in the first and second cervical vertebrae (vertebrae in the neck), square shaped vertebrae, thin ribs, thinning of the bones, and craniofacial abnormalities.
Diagnosis
There are more than 75 syndromes associated with craniosynostosis. There are also a number of different syndromes associated with both craniosynostosis and marfanoid body type. X-ray evaluation can be helpful in determining whether a person has SGS, as they tend to have abnormal first and second cervical vertebrae, hydro-
K E Y T E R M S
Aortic root—The location where the aorta (main heart blood vessel) inserts in the heart. Enlargement of the aortic root can cause it to rupture.
Craniosynostosis—Premature, delayed, or otherwise abnormal closure of the sutures of the skull.
Marfanoid—Term for body type which is similar to people with Marfan syndrome. Characterized by tall, lean body with long arms and long fingers.
cephalus (water on the brain), and certain brain malformations.
SGS must be differentiated from other syndromes with craniosynostosis and marfaniod body type. Two such syndromes include Idaho syndrome II and AntleyBixler syndrome. Idaho syndrome II has less severe craniofacial problems than SGS and has abnormal leg bones and absent patellae (knee caps). Antley-Bixler syndrome is an inherited syndrome with craniofacial abnormalities, abnormal arm and leg bones, and fractures in the femurs (thigh bones). These characteristics are different from SGS. A clinical geneticist is a physician who has special training in recognizing and diagnosing rare genetic conditions and is a good resource for differentiating among these complicated and similar conditions.
Treatment and management
Cardiology evaluation is important since several children have been reported to have severe cardiac disease with SGS. Aortic root must be evaluated and measured routinely to minimize the risk for rupture. Enlarged aortic roots may need to be surgically repaired.
Patients should have an opthalmalogic evaluation, since mutations in the FBR1 gene are associated with abnormalities in the eyes.
Surgical correction of craniofacial problems or pectus are sometimes necessary or desirable. Shunting (surgical placement of a shunt to drain the accumulated fluid in the brain to the abdominal cavity to relieve pressure) may be required for patients with hydrocephalus. Orthopedic devices may be required for scoliosis or other bone abnormalities.
Special education for mentally retarded individuals or individuals with developmental delay is recommended.
Genetic counseling is recommended for persons with relatives diagnosed with SGS.
syndrome craniosynostosis Goldberg-Shprintzen
G A L E E N C Y C L O P E D I A O F G E N E T I C D I S O R D E R S |
1047 |

Sickle cell disease
Prognosis
SGS does not alter lifespan, although complications from associated abnormalities such as mental retardation or respiratory problems can cause problems.
Resources
BOOKS
Gorlin, R.J., M.M. Cohen, and L.S. Levin. “Marfaniod Features and Craniosynostosis (including Shprintzen-Goldberg Syndrome).” In Syndromes of the Head and Neck. New York: Oxford University Press, 1990.
PERIODICALS
Furlong, J., T.W. Kurczynski, and J.R. Hennessy. “New Marfanoid Syndrome with Craniosynostosis.” American Journal of Medical Genetics 26 (1987): 599-604.
Greally, M.T., et al. “Shprintzen-Goldberg Syndrome: A Clinical Analysis.” American Journal of Medical Genetics
76 (1998): 202-212.
Lee, Y.C., et al. “Marfanoid Habitus, Dysmorphic Features, and Web Neck.” Southerna Medical Journal 93 (2000): 11971200
ORGANIZATIONS
Coalition for Heritable Disorders of Connective Tissue (CHDCT). 382 Main Street, Port Washington, NY 11050. (516) 883-8712. http://www.chdct.org .
Hydrocephalus Association. 870 Market St. Suite 705, San Francisco, CA 94102. (415) 732-7040 or (888) 598-3789. Fax: (415) 732-7044. hydroassoc@aol.com. http://www
.hydroassoc.org .
WEBSITES
National Organization for Rare Diseases (NORD).www.rarediseases.org .
“Shprintzen-Goldberg Craniosynostosis Syndrome.” Online
Mendelian inheritance in Man (OMIM). http://www
.ncbi.nlm.nig.gov/entrez/dispomim.cgi?id=182212 .
Amy Vance, MS, CGC
Sialidoses types I and II see Neuraminidase deficiency
I Sickle cell disease
Definition
Sickle cell disease describes a group of inherited blood disorders characterized by chronic anemia, painful events, and various complications due to associated tissue and organ damage.
Description
The most common and well-known type of sickle cell disease is sickle cell anemia, also called SS disease. All types of sickle cell disease are caused by a genetic change in hemoglobin, the oxygen-carrying protein inside the red blood cells. The red blood cells of affected individuals contain a predominance of a structural variant of the usual adult hemoglobin. This variant hemoglobin, called sickle hemoglobin, has a tendency to develop into rod-like structures that alter the shape of the usually flexible red blood cells. The cells take on a shape that resembles the curved blade of the sickle, an agricultural tool. Sickle cells have a shorter life span than normally-shaped red blood cells. This results in chronic anemia characterized by low levels of hemoglobin and decreased numbers of red blood cells. Sickle cells are also less flexible and more sticky than normal red blood cells, and can become trapped in small blood vessels preventing blood flow. This compromises the delivery of oxygen, which can result in pain and damage to associated tissues and organs. Sickle cell disease presents with marked variability, even within families.
Demographics
Carriers of the sickle cell gene are said to have sickle cell trait. Unlike sickle cell disease, sickle cell trait does not cause health problems. In fact, sickle cell trait is protective against malaria, a disease caused by bloodborne parasites transmitted through mosquito bites. According to a widely accepted theory, the genetic mutation associated with the sickle cell trait occurred thousands of years ago. Coincidentally, this mutation increased the likelihood that carriers would survive malaria infection. Survivors then passed the mutation on to their offspring, and the trait became established throughout areas where malaria was common. As populations migrated, so did the sickle cell trait. Today, approximately one in 12 African Americans has sickle cell trait.
Worldwide, it has been estimated that one in every 250,000 babies is born annually with sickle cell disease. Sickle cell disease primarily affects people of African, Mediterranean, Middle Eastern, and Asian Indian ancestry. In the United States, sickle cell disease is most often seen in African Americans, in whom the disease occurs in one out of every 400 births. The disease has been described in individuals from several different ethnic backgrounds and is also seen with increased frequency in Latino Americans—particularly those of Caribbean, Central American, and South American ancestry. Approximately one in every 1,000-1,400 Latino births are affected.
1048 |
G A L E E N C Y C L O P E D I A O F G E N E T I C D I S O R D E R S |
Sickle Cell Anemia |
diseaseSicklecell |
(Gale Group)
Genetic profile
Humans normally make several types of the oxygencarrying protein hemoglobin. An individual’s stage in development determines whether he or she makes primarily embryonic, fetal, or adult hemoglobins. All types of hemoglobin are made of three components: heme, alpha (or alpha-like) globin, and beta (or beta-like) globin. Sickle hemoglobin is the result of a genetic change in the beta globin component of normal adult hemoglobin. The beta globin gene is located on chromosome 11. The sickle cell form of the beta globin gene results from the substitution of a single DNA nucleotide, or genetic building-block. The change from adenine to thymine at codon (position) 6 of the beta globin gene leads to insertion of the amino acid valine—instead of glutamic acid—at this same position in the beta globin protein. As a result of this change, sickle hemoglobin has unique properties in comparison to the usual type of adult hemoglobin.
Most individuals have two normal copies of the beta globin gene, which make normal beta globin that is incorporated into adult hemoglobin. Individuals who have sickle cell trait (called sickle cell carriers) have one normal beta globin gene and one sickle cell gene. These individuals make both the usual adult hemoglobin and sickle hemoglobin in roughly equal proportions, so they do not experience any health problems as a result of having the trait. Although traces of blood in the urine and difficulty in concentrating the urine can occur, neither represents a significant health problem as a result of sickle cell trait. Of the millions of people with sickle cell trait worldwide, a small handful of individuals have experienced acute symptoms. In these very rare cases, individuals were subject to very severe physical strain.
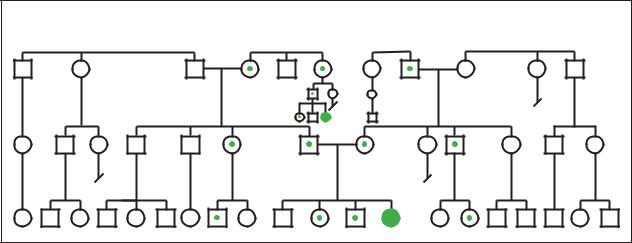
When both members of a couple are carriers of sickle cell trait, there is a 25% chance in each pregnancy for the baby to inherit two sickle cell genes and have sickle cell anemia, or SS disease. Correspondingly, there is a 50% chance the baby will have sickle cell trait and a 25% chance that the baby will have the usual type of hemoglobin.
Other types of sickle cell disease include SC disease, SD disease, and S/beta thalassemia. These conditions are caused by the co-inheritance of the sickle cell gene and another altered beta globin gene. For example, one parent may have sickle cell trait and the other parent may have hemoglobin C trait (another hemoglobin trait that does not cause health problems). For this couple, there would be a 25% chance of SC disease in each pregnancy.
Signs and symptoms
Normal adult hemoglobin transports oxygen from the lungs to tissues throughout the body. Sickle hemoglobin can also transport oxygen. However, once the oxygen is released, sickle hemoglobin tends to polymerize (line-up) into rigid rods that alter the shape of the red blood cell. Sickling of the red blood cell can be triggered by low oxygen, such as occurs in organs with slow blood flow. It can also be triggered by cold temperatures and dehydration.
Sickle cells have a decreased life span in comparison to normal red blood cells. Normal red blood cells survive for approximately 120 days in the bloodstream; sickle cells last only 10-12 days. As a result, the bloodstream is chronically short of red blood cells and hemoglobin, and the affected individual develops anemia.
Sickle cells can create other complications. Due to their shape, they do not fit well through small blood
G A L E E N C Y C L O P E D I A O F G E N E T I C D I S O R D E R S |
1049 |

Sickle cell disease
Scanning electron micrograph (SEM) of red blood cells taken from a person with sickle cell anemia. The red blood cells at the bottom are normal; the diseased, sickle-shaped cell appears at the top. (Photo Researchers, Inc.)
vessels. As an aggravating factor, the outside surfaces of sickle cells may have altered chemical properties that increase the cells’ ‘stickiness’. These sticky sickle cells are more likely to adhere to the inside surfaces of small blood vessels, as well as to other blood cells. As a result of the sickle cells’ shape and stickiness, blockages form in small blood vessels. Such blockages prevent oxygenated blood from reaching areas where it is needed, causing pain as well as organ and tissue damage.
The severity of symptoms cannot be predicted based solely on the genetic inheritance. Some individuals with sickle cell disease develop healthor life-threatening problems in infancy, but others may have only mild symptoms throughout their lives. Individuals may experience varying degrees of health at different stages in the lifecycle. For the most part, this clinical variability is unpredictable, and the reasons for the observed variability can not usually be determined. However, certain types of sickle cell disease (i.e. SC disease) tend to result in fewer and less severe symptoms on average than other types of sickle cell disease (i.e. SS disease). Some additional modifying factors are known. For example, elevated levels of fetal hemoglobin in a child or adult can decrease the quantity and severity of some symptoms and complications. Fetal hemoglobin is a normally occurring hemoglobin that usually decreases from over 90% of the total hemoglobin to under one percent during the first year of life. This change is genetically determined,
although some individuals may experience elevated levels of fetal hemoglobin due to variation in the genes that control fetal hemoglobin production. Such individuals often experience a reduction in their symptoms and complications due to the ability of fetal hemoglobin to prevent the polymerization of sickle hemoglobin, which leads to sickling of the red blood cell.
There are several symptoms that warrant immediate medical attention, including the following:
•Signs of infection (fever greater than 101°F or 38.3°C, coughs frequently or breathing trouble, unusual crankiness, feeding difficulties)
•Signs of severe anemia (pale skin or lips, yellowing of the skin or eyes, very tired, very weak)
•Signs indicating possible dehydration (vomiting, diarrhea, fewer wet diapers)
•Other signs (pain or swelling in the abdomen, swollen hands or feet, screams when touched).
These can be signs of various complications that occur in sickle cell disease.
Infections and effects on the spleen
Children with sickle cell disease who are under age three are particularly prone to life-threatening bacterial infections. Streptococcus pneumoniae is the most common offending bacteria, and invasive infection from this organism leads to death in 15% of patients. The spleen, an organ that helps to fight bacterial infections, is particularly vulnerable to the effects of sickling. Sickle cells can impede blood flow through the spleen, causing organ damage, which usually results in loss of spleen function by late childhood. The spleen can also become enlarged due to blockages and/or increased activity of the spleen. Rapid enlargement of the spleen may be a sign of another complication called splenic sequestration, which occurs mostly in young children and can be life-threatening. Widespread sickling in the spleen prevents adequate blood flow from the organ, removing increasing volumes of blood from the circulation and leading to accompanying signs of severe anemia.
Painful events
Painful events, also known as vaso-occlusive events, are a hallmark symptom of sickle cell disease. The frequency and duration of the pain can vary tremendously from person to person and over an individual’s lifecycle. Painful events are the most common cause of hospitalizations in sickle cell disease. However, only a small portion of individuals with sickle cell disease experience frequent and severe painful events. Most painful events can be managed at home. Pain results when small blood
1050 |
G A L E E N C Y C L O P E D I A O F G E N E T I C D I S O R D E R S |
vessel blockages prevent oxygen from reaching tissues. Pain can affect any area of the body, although the extremities, chest, abdomen, and bones are frequently affected sites. There is some evidence that cold temperatures or infection can trigger a painful event, but most events occur for unknown reasons. The hand-foot syndrome, or dactylitis, is a particular type of painful event. Most common in toddlers, dactylitis results in pain and swelling in the hands and feet, sometimes accompanied by a fever.
Anemia
Sickle cells have a high turnover rate leading to a deficit of red blood cells in the bloodstream. Common symptoms of anemia include fatigue, paleness, and a shortness of breath. A particularly severe form of ane- mia—aplastic anemia—occurs following infection with parvovirus. Parvovirus causes extensive destruction of the bone marrow, bringing production of new red blood cells to a halt. Bone marrow production resumes after seven to 10 days; however, given the short lives of sickle cells, even a brief shut-down in red blood cell production can cause a rapid decline in hemoglobin concentrations.
Delayed growth
The energy demands of the bone marrow for red blood cell production compete with the demands of a growing body. Children with sickle cell anemia may have delayed growth and reach puberty at a later age than normal. By early adulthood, they catch up on growth and attain normal height; however, weight typically remains below average.
Stroke
Children with sickle cell disease have a significantly elevated risk of having a stroke, which can be one of the most concerning complications of sickle cell disease. Approximately 11% of individuals with sickle cell disease will have a recognizable stroke by the age of 20. Magnetic resonance imaging studies have found that 17% of children with sickle cell anemia have evidence of a previous stroke or clinically ‘silent’ stroke-like events called transient ischemic events. Stroke in sickle cell disease is usually caused by a blockage of a blood vessel, but about one fourth of the time may be caused by a hemorrhage (or rupture) of a blood vessel.
Strokes result in compromised delivery of oxygen to an area of the brain. The consequences of stroke can range from life-threatening, to severe physical or cognitive impairments, to apparent or subtle learning disabilities, to undetectable effects. Common stroke symptoms include weakness or numbness that affects one side of the body,
sudden behavioral changes, loss of vision, confusion, loss of speech or the ability to understand spoken words, dizziness, headache, seizures, vomiting, or even coma.
Approximately two-thirds of the children who have a stroke will have at least one more. Transfusions have been shown to decrease the incidence of a second stroke. A recent study showed that children at highest risk to experience a first stroke were 10 times more likely to stroke if untreated when compared to high-risk children treated with chronic blood transfusion therapy. High-risk children were identified using transcranial doppler ultrasound technology to detect individuals with increased blood flow speeds due to constricted intracranial blood vessels.
Acute chest syndrome
Acute chest syndrome (ACS) is a leading cause of death for individuals with sickle cell disease, and recurrent attacks can lead to permanent lung damage. Therefore, rapid diagnosis and treatment is of great importance. ACS can occur at any age and is similar but distinct from pneumonia. Affected persons may experience fever, cough, chest pain, and shortness of breath. ACS seems to have multiple causes including infection, sickling in the small blood vessels of the lungs, fat embolisms in the lungs, or a combination of factors.
Priapism
Males with sickle cell anemia may experience priapism, a condition characterized by a persistent and painful erection of the penis. Due to blood vessel blockage by sickle cells, blood is trapped in the tissue of the penis. Priapism may be short in duration or it may be prolonged. Priapism can be triggered by low oxygen (hypoxemia), alcohol consumption, or sexual intercourse. Since priapism can be extremely painful and result in damage to this tissue causing impotence, rapid treatment is essential.
Kidney disease
The environment in the kidney is particularly prone to damage from sickle cells. Signs of kidney damage can include blood in the urine, incontinence, and enlarged kidneys. Adults with sickle cell disease often experience insufficient functioning of the kidneys, which can progress to kidney failure in a small percentage of adults with sickle cell disease.
Jaundice and gallstones
Jaundice is indicated by a yellow tone in the skin and eyes, and alone it is not a health concern. Jaundice may occur if bilirubin levels increase, which can occur with high levels of red blood cell destruction. Bilirubin is the
disease cell Sickle
G A L E E N C Y C L O P E D I A O F G E N E T I C D I S O R D E R S |
1051 |
Sickle cell disease
final product of hemoglobin degradation, and is typically removed from the bloodstream by the liver. Therefore, jaundice can also be a sign of a poorly functioning liver, which may also be evidenced by an enlarged liver. Increased bilirubin also leads to increased chance for gallstones in children with sickle cell disease. Treatment, which may include removal of the gall bladder, may be selected if the gallstones start causing symptoms.
Retinopathy
The blood vessels that supply oxygen to the retina— the tissue at the back of the eye—may be blocked by sickle cells, leading to a condition called retinopathy. This is one of the only complications that is actually more common in SC disease as compared to SS disease. Retinopathy can be identified through regular ophthalmology evaluations and effectively treated in order to avoid damage to vision.
Joint problems
Avascular necrosis of the hip and shoulder joints, in which bone damage occurs due to compromised blood flow due to sickling, can occur later in childhood. This complication can affect an individual’s physical abilities and result in substantial pain.
Diagnosis
Inheritance of sickle cell disease or trait cannot be prevented, but it may be predicted. Screening is recommended for individuals in high-risk populations. In the United States, African Americans and Latino Americans have the highest risk of having the disease or trait. Sickle cell is also common among individuals of Mediterranean, Middle Eastern, and Eastern Indian descent.
A complete blood count (CBC) will describe several aspects of an individual’s blood cells. A person with sickle cell disease will have a lower than normal hemoglobin level, together with other characteristic red blood cell abnormalities. A hemoglobin electrophoresis is a test that can help identify the types and quantities of hemoglobin made by an individual. This test uses an electric field applied across a slab of gel-like material. Hemoglobins migrate through this gel at various rates and to specific locations, depending on their size, shape, and electrical charge. Although sickle hemoglobin (Hb S) and regular adult hemoglobin (called Hb A) differ by only one amino acid, they can be clearly separated using hemoglobin electrophoresis. Isoelectric focusing and high-performance liquid chromatography (HPLC) use similar principles to separate hemoglobins and can be used instead of or in various combinations with hemo-
globin electrophoresis to determine the types of hemoglobin present.
Another test, called the ‘sickledex’ can help confirm the presence of sickle hemoglobin, although this test cannot provide accurate or reliable diagnosis when used alone. When Hb S is present, but there is an absence or only a trace of Hb A, sickle cell anemia is a likely diagnosis. Additional beta globin DNA testing, which looks directly at the beta globin gene, can be performed to help confirm the diagnosis and establish the exact genetic type of sickle cell disease. CBC and hemoglobin electrophoresis are also typically used to diagnosis sickle cell trait and various other types of beta globin traits.
Diagnosis of sickle cell disease can occur under various circumstances. If an individual has symptoms that are suggestive of this diagnosis, the abovedescribed screening tests can be performed followed by DNA testing, if indicated. Screening at birth using HPLC or a related technique offers the opportunity for early intervention. More than 40 states include sickle cell screening as part of the usual battery of blood tests done for newborns. This allows for early identification and treatment. Hemoglobin trait screening is recommended for any individual of a high-risk ethnic background who may be considering having children. When both members of a couple are found to have sickle cell trait, or other related hemoglobin traits, they can receive genetic counseling regarding the risk of sickle cell disease in their future children and various testing options.
Sickle cell disease can be identified before birth through the use of prenatal diagnosis. Chorionic villus sampling (CVS) can be offered as early as 10 weeks of pregnancy and involves removing a sample of the placenta made by the baby and testing the cells. CVS carries a risk of causing a miscarriage that is between one-half to one percent.
Amniocentesis is generally offered between 16 and 18 weeks of pregnancy, but can sometimes be offered earlier. Two to three tablespoons of the fluid surrounding the baby is removed. This fluid contains fetal cells that can be tested. This test carries a risk of causing a miscarriage, which is less than one percent. Pregnant woman and couples may choose prenatal testing in order to prepare for the birth of a baby that may have sickle cell disease.
Preimplantation genetic diagnosis (PGD) is a relatively new technique that involves in-vitro fertilization followed by genetic testing of one cell from each developing embryo. Only the embryos unaffected by sickle cell disease are transferred back into the uterus. PGD is currently available on a research basis only, and is relatively expensive.
1052 |
G A L E E N C Y C L O P E D I A O F G E N E T I C D I S O R D E R S |
