
- •Leukemia
- •Normal haemopoiesis
- •Hemoblastosis
- •Haemopoiesis
- •Leukemia
- •Types of leukemia
- •Classification of leukemia
- •Classification of AML
- •Pictures of blood
- •Myeloid Maturation
- •Lymphoblast/Myeloblast
- •Epidemiology of acute leukemia
- •Etiology
- •Two-hit model of leukemogenesis
- •Clinical presentation
- •Stages of acute leukemia
- •Extramedullar clinical presentation of acute leukemia
- •Leukemia cutis and chloroma
- •Gum hyperplasia
- •Diagnostics of leukemia
- •Morphological method
- •Normal bone marrow
- •Acute leukemia
- •Acute lymphoblastic leukemia
- •Hodjkin`s lymphoma
- •Immunophenotyping
- •Cytochemical study
- •Cytogenetics and molecular genetics (FISH)
- •Prognosis in acute leukemia
- •Treatment of leukemia
- •Male patient., 85 years old
- •Physical examination at admission
- •Chronic myelogenous leukemia
- •Mechanism of formation of Philadelphia chromosome
- •Epidemiology оf CML
- •Phases of CML
- •Diagnostics of CML
- •Blood smear in CML
- •Bone marrow in CML
- •Blastic crisis
- •Cytogenetics
- •Treatment targets
- •Principles of treatment
- •Chronic lymphocytic leukemia
- •Epidemiology and etiology of CLL
- •Clinical presentation
- •Classification of CLL (Binet) (1989)
- •Diagnostic criteria
- •Chronic lymphocytic leukemia
- •Mature lymphocytes with normal structure. Gumprecht shadows
- •Bone marrow in CLL
- •Principles of treatment
- •Lymphomas
- •Hodgkin’s lymphoma
- •Clinical presentation
- •Stages of Hodgkin Lymphoma
- •Morphological classification
- •Diagnosis
- •Reed-Sternberg cells
- •Treatment
- •Non-Hodgkin’s lymphoma
- •Hodgkin’s vs
Principles of treatment
• Chemotherapy
oTyrosine kinase inhibitors
oOther myelosupressive drugs (alfa-interferon, hydroxyurea, etc)
•Stem cell transplantation
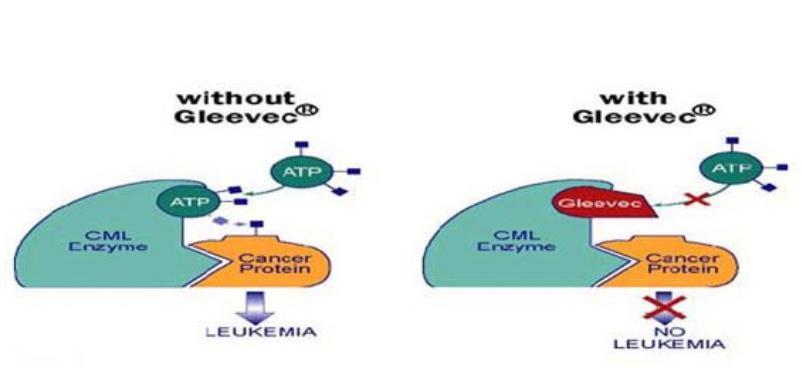
Mechanism of action of Imatinib
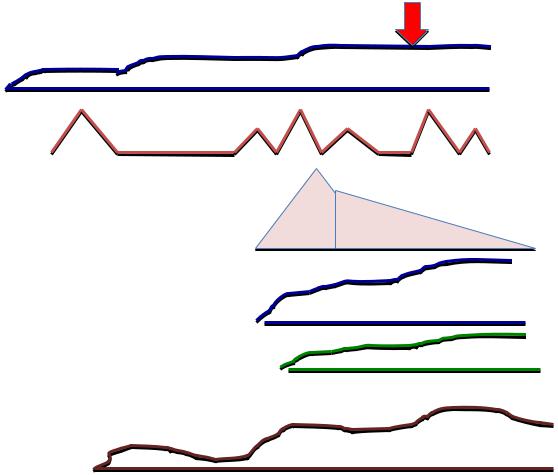
2012 |
2013 |
2014 |
Male, 65 years, engineer |
|
hospitalization |
General weakness
Fever
Weight loss
Heaviness in right hypochondrium
Hepatomegaly
Peripheral lymphadenopathy
CBC
WBC Promyelocytes Myelocytes Metamyelocytes Hb
38 |
37,2 |
38,1 |
37,3 |
38,2 |
37,1 |
|
|
|
-10 |
-6 kg |
|
kg |
||
|
30х109/l |
Ph-chromosome+ |
50х109/l |
|
|
2% |
|
23% |
|
20% |
110 g/l |
100 g/l |
Chronic lymphocytic leukemia
•В-cell prolipherative disease
•Proliferation of mature but functionally incompetent lymphocytes expressing CD19, CD23, CD20,CD5-markers
•Association with immune deficiency and viruses.
Epidemiology and etiology of CLL
•The most common leukemia in adults in Western countries: 30% of all leukemias
•Median age 69 years
•M/F 1,5 : 1,0
•Family history is important
•Often asymptomatic
•Association with immunodeficiency and viral infections
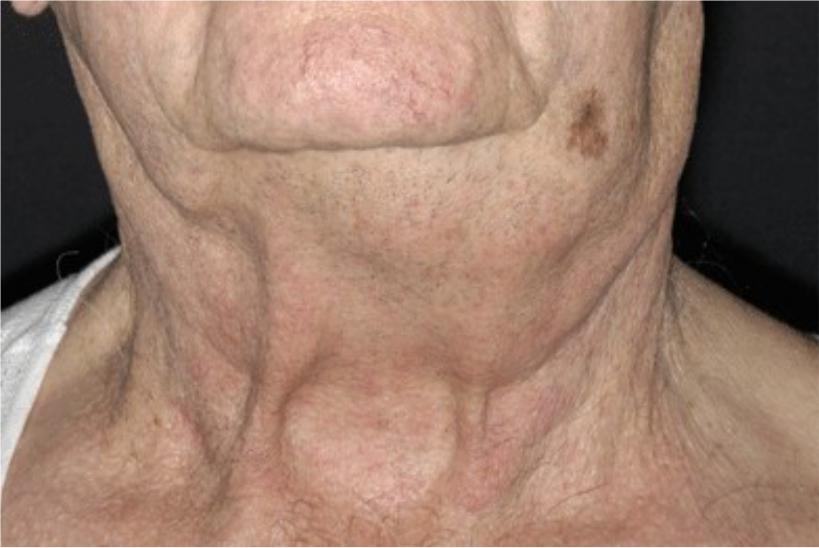
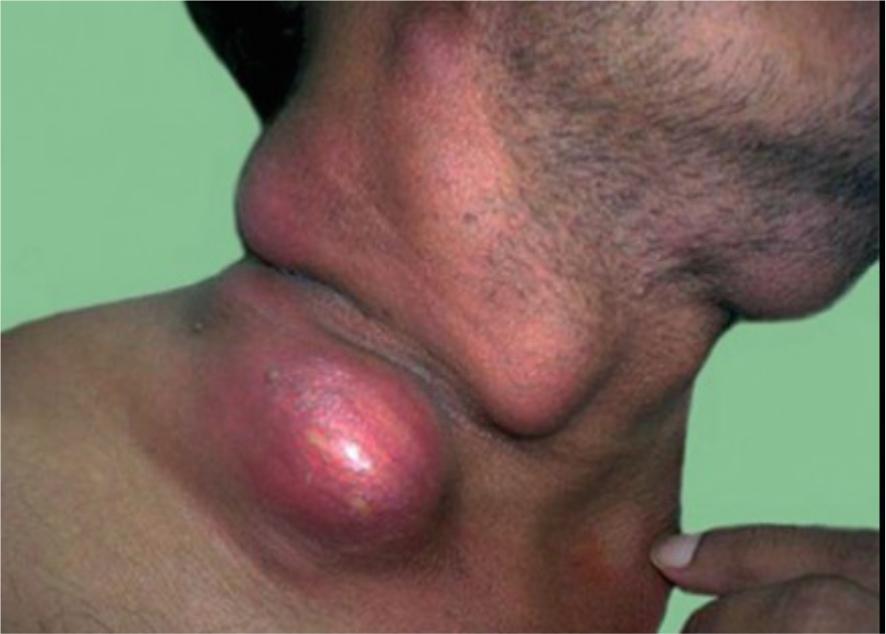
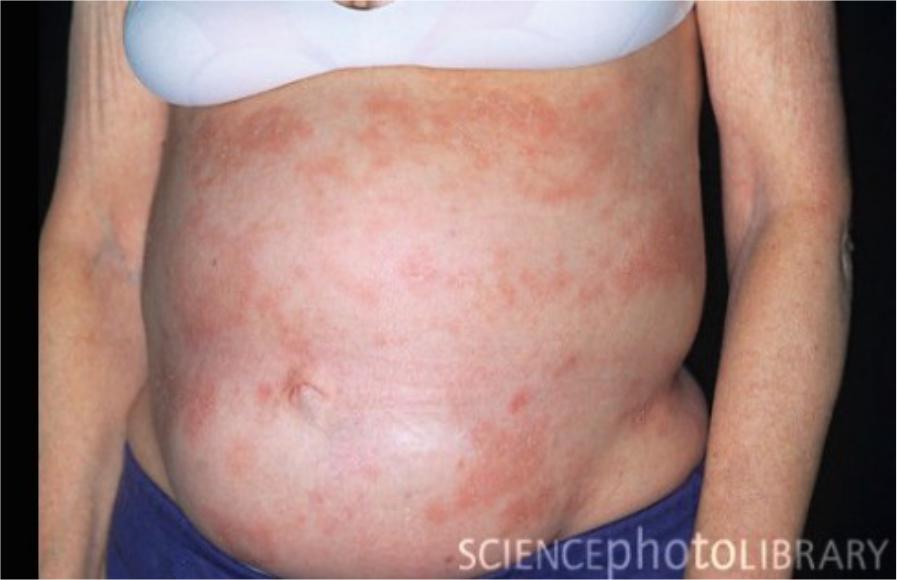
Clinical presentation
25-50 % asymptomatic at early stages
1.Lymphoproliferative syndrome
•Progressive lymphadenopathy
•Splenomegaly, hepatomegaly
2.Constitutional symptoms
•Fever, malaise, swellings, weight loss
3.Signs of tumor proliferation
4.Specific features (repeated infections, autoimmune hemolytic anemia, thrombocytopenia)
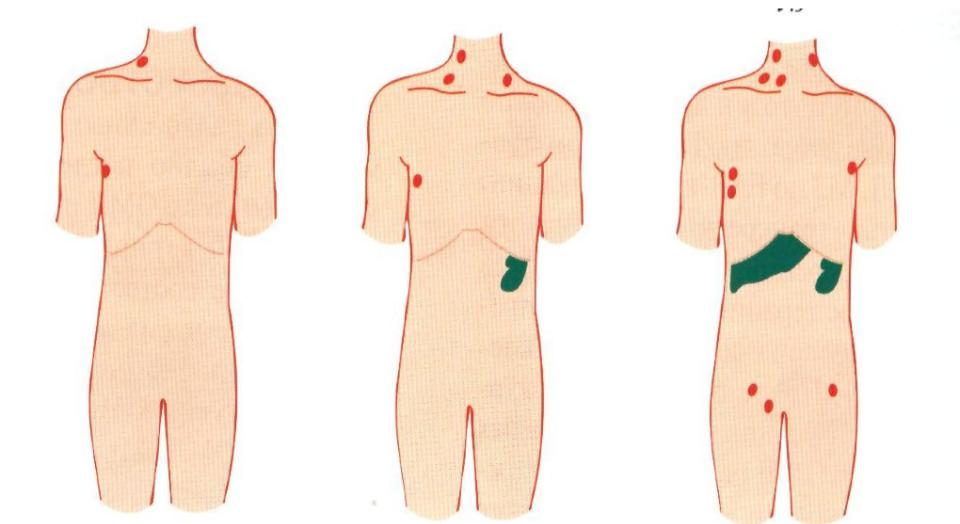
Classification of CLL (Binet) (1989)
Based on the number of involved regions

Diagnostic criteria
1.Absolute lymphocytosis > 5х109/л with < 55% of prolymphocytes
2.Presence of CD19, CD20, CD23,and CD5 on B-cells (peripheral blood flow cytometry)
3.Lymphocytes should dominate in bone marrow (>30% of nuclear cells)
