
- •LIVER DISEASES
- •LIVER DISEASES
- •Do you know that …
- •Liver structure v. portae system
- •Liver
- •Liver functions
- •Major risk factors for liver disease
- •Symptoms of liver disorders
- •Fatigue
- •Jaundice
- •Jaundice or icterus
- •Jaundice: major types
- •Causes of jaundice
- •Darkening of the Urine
- •Pale (light) Stools
- •Liver Pain
- •Ascites
- •Ascites, umbilical hernia
- •Ascites
- •Симптомы и синдромы заболеваний печени
- •ПОРТАЛЬНАЯ ГИПЕРТЕНЗИЯ
- •Possible levels of block in portal hypertension
- •Hepatocellular cytolisis
- •Stigmata of chronic liver disease
- •Cholestasis syndrom
- •CHOLESTASIS
- •Etiology of Dupuitren contracture
- •Etiologic factors of gynecomastia
- •polyneuropathia
- •ПРИЧИНЫ ПОРТАЛЬНОЙ ГИПЕРТЕНЗИИ
- •Расширенные вены передней стенки живота, асцит
- •ЭГДС.
- •Расширение v. рortae и vv. hepaticae
- •ПЕЧЕНОЧНОКЛЕТОЧНАЯ
- •ПРИЧИНЫ ПЕЧЕНОЧНОЙ НЕДОСТАТОЧНОСТИ
- •Синдром печеночно-клеточной недостаточности
- •Печеночная энцефалопатия
- •ГЕПАТОРЕНАЛЬНЫЙ СИНДРОМ I и II тип
- •Патогенеза гепаторенального синдрома
- •Типы гепаторенального синдрома
- •ФАКТОРЫ, ПРОВОЦИРУЮЩИЕ РАЗВИТИЕ ГЕПАТОРЕНАЛЬНОГО СИНДРОМА (на фоне поражения печени)
- •Желтуха, ксантелазмы
- •ГИПЕРСПЛЕНИЗМ
- •Маркеры хронической алкогольной интоксикации
- •Классификация тяжести поражения печени по Чайлд-Пью
- •ЭГДС – расширенные вены пищевода
- •Пункционная биопсия печени под контролем УЗИ (цирроз)
- •Мелкоочаговое поражение печени при остром гепатите
- •Асцит, расширенная v.portae, неровность контуров при циррозе печени
- •Сцинтиграфия печени с метастазами
- •Сцинтиграфия мелкоузлового цирроза
- •Лапароскопия – крупноузловой цирроз
- •Передняя стенка живота при синдроме портальной гипертензии
- •Компьютерная томография
- •FibroScan®
- •Выраженность фиброза при фибросканировании печени
- •Stages of Liver Disease
- •Progression of Hepatitis B Infection
- •Healthy Liver
- •Healthy Liver
- •Types of Hepatitis
- •Hepatitis B is a Devastating Global Healthcare Issue
- •Hepatitis – Disease Terminology
- •How Hepatitis B is Acquired?
- •How the Infection is Acquired in the West?
- •Hepatitis B – Diagnosis Terminology
- •Diagnosis of Chronic Hepatitis B
- •Signs and Symptoms of HBV Infection
- •Universal Hepatitis B Vaccination
- •Global Control of Hepatitis B
- •Types of viral Hepatitis
- •Healthy Liver
- •Liver biopsy
- •Detection of serologic markers of hepatitis B virus (HBV) infection, as a function
- •Lamivudine is a Potent Inhibitor of HBV Replication
- •Lamivudine has an Excellent Pharmacokinetic Profile
- •Patient Entry Criteria
- •One Year of Lamivudine - Conclusions
- •Resistance to Anti-Viral Drugs
- •Prevention of Hepatitis B
- •Universal Hepatitis B Vaccination
- •Recommendations for Pre-exposure Vaccination
- •Recommendations for Post-exposure Vaccination
- •Global Control of Hepatitis B
- •Concurrent immunologic diseases in type 2 autoimmune hepatitis.
- •Probabilities of clinical, biochemical, and histologic remission during corticosteroid therapy.
- •Clinical features of type 2 autoimmune hepatitis.
- •Liver transplantation for autoimmune hepatitis.
- •Survival expectations and probability of developing cirrhosis during and after corticosteroid treatment.
- •liver biopsy
- •Detection of serologic markers of hepatitis B virus (HBV) infection, as a function
- •The Efficacy and Safety of Lamivudine in HBeAg-positive Chronic Hepatitis B
- •Lamivudine is a Potent Inhibitor of HBV Replication
- •Lamivudine has an Excellent Pharmacokinetic Profile
- •What Patient Populations Have Been Studied
- •Key Lamivudine Clinical Studies (1)
- •Key Lamivudine Clinical Studies (2)
- •Patient Entry Criteria
- •Lamivudine Rapidly Suppresses
- •One Year of Lamivudine - Conclusions
- •Resistance to Anti-Viral Drugs
- •Concurrent immunologic diseases in type 1 autoimmune hepatitis.
- •Probabilities of clinical, biochemical, and histologic remission during corticosteroid therapy.
- •Clinical features of type 2 autoimmune hepatitis.
- •Liver transplantation for autoimmune hepatitis.
- •Survival expectations and probability of developing cirrhosis during and after corticosteroid treatment.
- •ALCOHOLIC LIVER DISEASE
- •Principal alcohol-induced hepatic lesions
- •Alcohol-induced hepatic lesions
- •Pathogenesis of liver injury secondary to chronic ethanol ingestion
- •Equivalents of pure alcohol
- •Alcoholic fatty liver
- •Two-Hit Model of the Progression of Fatty Liver Disease
- •Alcoholic fatty liver
- •Similarities between Alcoholic and Nonalcoholic Fatty Liver Diseases
- •Alcoholic hepatitis
- •This figure depicts a laparoscopic view of a patient with chronic active hepatitis
- •Percutaneous liver biopsy with or without ultrasonic guidance
- •Alcoholic hepatitis: liver biopsy
- •Treatment of severe alcoholic hepatitis
- •Причины смерти при алкогольном гепатите
- •Alcoholic cirrhosis
- •Alcoholic cirrhosis
- •Alcoholic cirrhosis: clinical manifestations

LIVER DISEASES
Symptoms. Signs. Syndroms. Diseases.
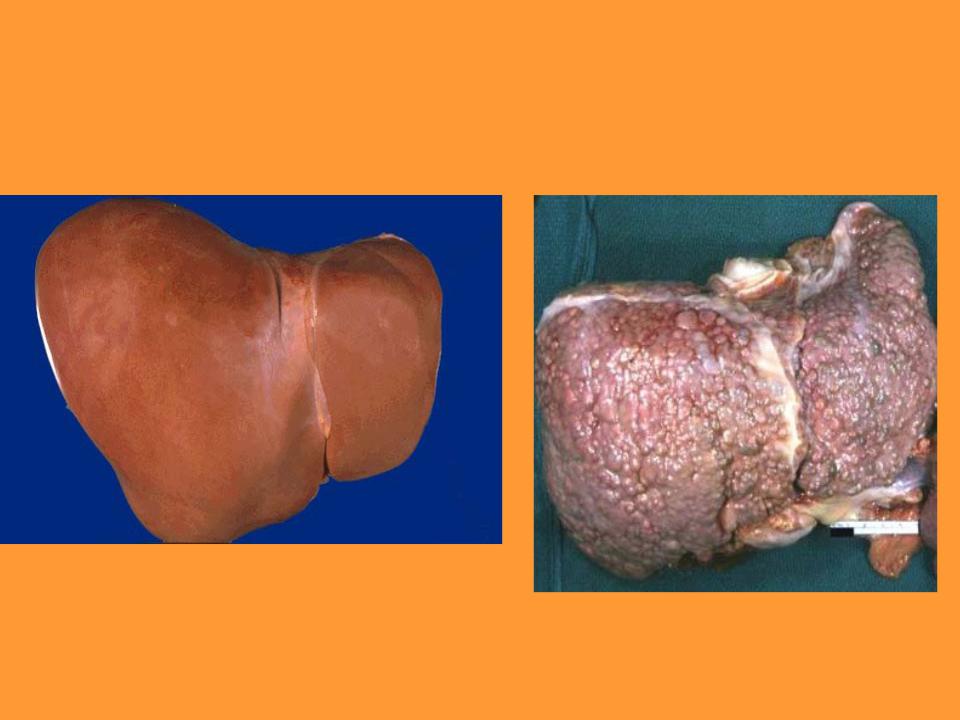
LIVER DISEASES

Do you know that …
•Liver is a depot for 13% of blood in every given moment
•Liver receives blood from 2 vessels
-oxygenated blood from a. hepatica
-blood with nutrients and metabolic products from v. porta
•Venous blood enters through v. porta and leaves liver via v. hepatica
•Liver may lost ¾ of hepatocytes before hepatic failure develops
•Liver is the unique human organ that can regenerate it self
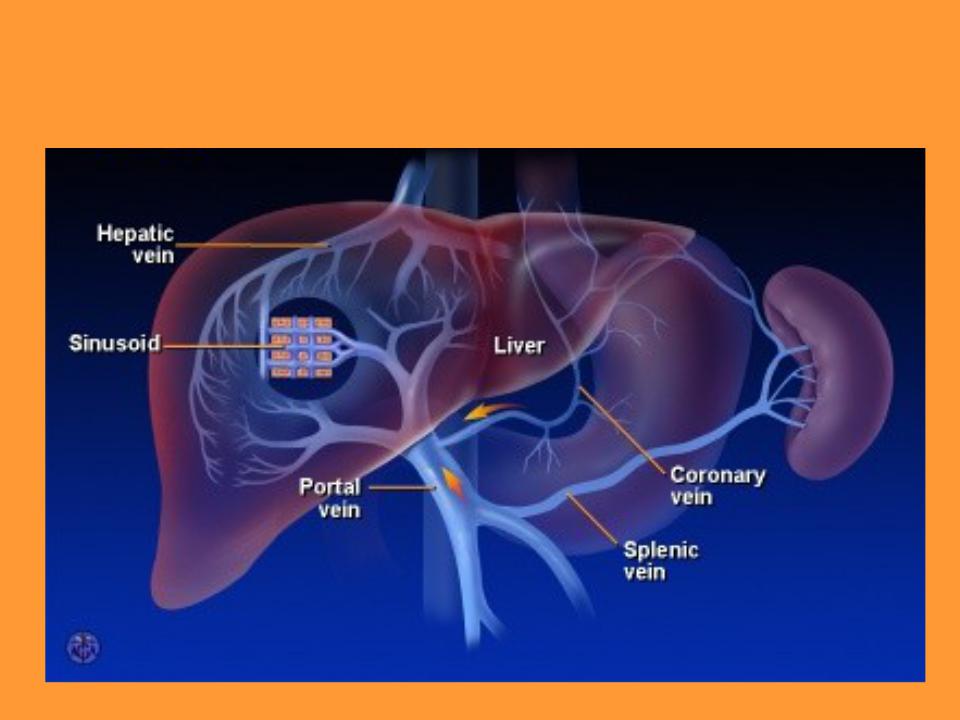
Liver structure v. portae system

Liver
•Stores sugar needed for energy
•Absorbs good nutrients
•Breaks down poisons (toxins) and drugs
•Makes important proteins that help build new tissue and repair broken tissue
•Produces bile, which helps remove waste from the body

Liver functions
•Synthetic
-synthesis of albumin, coagulation factors, fibrinogen, cholesterol, compliment, binding proteins for iron, copper, vit. A and other
•Detoxification and excretion
-products of metabolism (proteins, steroids, prostaglandins, drugs, alcohol, bilirubin, urea, ammonium and so on)
•Accumulation (deposition)
-glycogen, lipids, iron, copper, vitamins А,В12,D,Е,К
•Secretion
-secretion of bile

Major risk factors for liver disease
•alcohol use
•medications (including herbal compounds, birth control pills, and over-the-counter medications)
•personal habits
•sexual activity
•injection drug use
•recent surgery
•remote or recent transfusion with blood and blood products
•occupation
•familial history of liver disease

Symptoms of liver disorders
Constitutional symptoms
•Fatigue*
•Weakness
•Nausea
•Poor appetite
•Malaise
Liver-specific symptoms
•Jaundice*
•Dark urine*
•Light stools*
•Itching
•Ascites*
•Abdominal pain
•Liver pain
•Bloating

Fatigue
•The most common and most characteristic symptom of liver disease.
•It is variously described as lethargy, weakness, listlessness, malaise, need for sleep, lack of stamina, and poor energy.
•Typically arises after activity or exercise

Jaundice
–A yellow discoloration of the skin or sclera is a manifestation of hyperbilirubinemia and can be congenital or acquired.
–It may be also classified as:
•hemolytic (sickle cell anemia)
•hepatocellular (viral hepatitis)
•and obstructive (carcinoma of bile duct or head of the pancreas).
