
Borchers Andrea Ann (ed.) Handbook of Signs & Symptoms 2015
.pdf
the eye? Does he complain about foreign body sensation or dry, gritty eyes? If so, ask him how severe the problem is and how long he has had it. Then ask about recent sinus infection or vision problems. Take the patient’s vital signs, noting a fever, which may accompany eye infection. Next, evaluate the severity of exophthalmos with an exophthalmometer. (See Detecting Unilateral Exophthalmos.) If the eyes bulge severely, look for cloudiness on the cornea, which may indicate ulcer formation. Describe any eye discharge and observe for ptosis. Then check visual acuity, with and without correction, and evaluate extraocular movements. Palpate the patient’s thyroid for enlargement or goiter.
 EXAMINATION TIP Detecting Unilateral Exophthalmos
EXAMINATION TIP Detecting Unilateral Exophthalmos
If one of the patient’s eyes seems more prominent than the other, examine both eyes from above the patient’s head. Look down across his face, gently draw his lids up, and compare the relationship of the corneas to the lower lids. Abnormal protrusion of one eye suggests unilateral exophthalmos.
Remember: Don’t perform this test if you suspect eye trauma.
Medical Causes
Cavernous sinus thrombosis. Usually, cavernous sinus thrombosis causes the sudden onset of pulsating, unilateral exophthalmos. Accompanying it may be eyelid edema, decreased or absent pupillary reflexes, and impaired extraocular movement and visual acuity. Other features include a high fever with chills, papilledema, a headache, nausea, vomiting, somnolence, and, rarely, seizures.
Dacryoadenitis. Unilateral, slowly progressive exophthalmos is the most common sign of dacryoadenitis. Assessment may also reveal limited extraocular movements (especially on elevation and abduction), ptosis, eyelid edema and erythema, conjunctival injection, eye pain, and diplopia.
Graves’ disease . Exophthalmos occurs in patients with Graves’ disease, an autoimmune disorder that is the most common cause of hyperthyroidism. As the tissues and muscles behind the eye swell, the eyeball is forced forward in the eye socket, causing the eyes to bulge. Other symptoms include increased tearing, sensitivity to light, swelling of the lids, the sensation of grit

in the eyes, and reddened eyes. Other general symptoms include anxiety, fatigue, enlargement of the thyroid gland (goiter), unintended weight loss, increased appetite, heat sensitivity, and tremors.
Hemangioma. Most common in young adults, this orbital tumor produces progressive exophthalmos, which may be mild or severe, unilateral or bilateral. Other signs and symptoms include ptosis, limited extraocular movements, and blurred vision.
Lacrimal gland tumor. Exophthalmos usually develops slowly in one eye, causing its downward displacement toward the nose. The patient may also have ptosis and eye deviation and pain.
Leiomyosarcoma. Most common in people ages 45 and older, leiomyosarcoma is characterized by slowly developing, unilateral exophthalmos. Other effects include diplopia, impaired vision, and intermittent eye pain.
Orbital cellulitis. Commonly the result of sinusitis, this ocular emergency causes the sudden onset of unilateral exophthalmos, which may be mild or severe. Orbital cellulitis may also produce a fever, eye pain, a headache, malaise, conjunctival injection, tearing, eyelid edema and erythema, purulent discharge, and impaired extraocular movements.
Orbital choristoma. A common sign of this benign tumor, progressive exophthalmos may be associated with diplopia and blurred vision.
Orbital emphysema. Air leaking from the sinus into the orbit usually causes unilateral exophthalmos. Palpation of the globe elicits crepitation.
Parasite infestation. Usually, parasite infestation causes painless, progressive exophthalmos in one eye that may spread to the other eye. Associated findings include limited extraocular movement, diplopia, eye pain, and impaired visual acuity.
Scleritis (posterior). The gradual onset of mild to severe unilateral exophthalmos is common with scleritis. Other signs and symptoms include severe eye pain, diplopia, papilledema, limited extraocular movement, and impaired visual acuity.
Thyrotoxicosis. Although a classic sign of thyrotoxicosis, exophthalmos is absent in many patients. When present, it’s usually bilateral, progressive, and severe. Associated ocular features include ptosis, increased tearing, lid lag and edema, photophobia, conjunctival injection, diplopia, and decreased visual acuity. Other findings include an enlarged thyroid, nervousness, heat intolerance, weight loss despite increased appetite, sweating, diarrhea, tremors, palpitations, and tachycardia.
Special Considerations
Exophthalmos usually makes the patient self-conscious, so provide privacy and emotional support. Protect the affected eye from trauma, especially drying of the cornea. However, never place a gauze eye pad or other object over the affected eye; removal could damage the corneal epithelium. If a slitlamp examination is indicated, explain the procedure to the patient. If necessary, refer him to an ophthalmologist for a complete examination. The cause of exophthalmos determines the therapy. Prepare the patient for blood tests, such as a thyroid panel and a white blood cell count.
Patient Counseling
Explain ways to protect the eye from trauma, wind, and dust. Explain the proper application of eye lubricants.
Pediatric Pointers
In children around age 5, a rare tumor called optic nerve glioma may cause exophthalmos. Rhabdomyosarcoma, a more common tumor, usually affects children between ages 4 and 12 and produces the rapid onset of exophthalmos. In Hand-Schüller-Christian syndrome, exophthalmos typically accompanies signs of diabetes insipidus and bone destruction.
REFERENCES
Biswas, J. , Krishnakumar, S., & Ahuja, S. (2010) . Manual of ocular pathology. New Delhi, India: Jaypee–Highlights Medical Publishers, Inc.
Bonavolontà, G. , Strianese, D. , Grassi, P. , Comune, C. , Tranfa, F. , Uccello, G., & Iuliano, A. (2013) . An analysis of 2,480 spaceoccupying lesions of the orbit from 1976 to 2011. Ophthalmology and Plastic Reconstruction Surgery, 29(2), 79–86.
Eagle, R. C. Jr. (2011). Eye pathology: An atlas and text. Philadelphia, PA: Lippincott Williams & Wilkins. Gerstenblith, A. T. & Rabinowitz, M. P. (2012). The wills eye manual. Philadelphia, PA: Lippincott Williams & Wilkins. Roy, F. H. (2012). Ocular differential diagnosis. Clayton, Panama: Jaypee–Highlights Medical Publishers, Inc.
Sheth, V. S. , Marcet, M. M., Chiranand, P., Bhatt, H. K., Lamkin, J. C., & Jager, R. D. (2012). Review manual for ophthalmology. Philadelphia, PA: Lippincott Williams & Wilkins.
Eye Discharge
(See Also Exophthalmus, Eye Pain)
Usually associated with conjunctivitis, eye discharge is the excretion of a substance other than tears. This common sign may occur in one or both eyes, producing scant to copious discharge. The discharge may be purulent, frothy, mucoid, cheesy, serous, or clear, or a stringy white discharge. Sometimes, the discharge can be expressed by applying pressure to the tear sac, punctum, meibomian glands, or canaliculus.
Eye discharge commonly results from inflammatory and infectious eye disorders, but may also occur in certain systemic disorders. (See Sources of Eye Discharge .) Because this sign may accompany a disorder that threatens vision, it must be assessed and treated immediately.
History and Physical Examination
Begin your evaluation by finding out when the discharge began. Does it occur at certain times of the day or in connection with certain activities? If the patient complains of pain, ask him to show you its exact location and to describe its character. Is the pain dull, continuous, sharp, or stabbing? Do his eyes itch or burn? Do they tear excessively? Are they sensitive to light? Does he feel like something is in them?
After taking the patient’s vital signs, carefully inspect the eye discharge. Note its amount, color, and consistency. Then test visual acuity, with and without correction. Examine external eye structures, beginning with the unaffected eye to prevent cross-contamination. Observe for eyelid edema, entropion, crusts, lesions, and trichiasis. Next, ask the patient to blink as you watch for impaired lid movement. If the eyes seem to bulge, measure them with an exophthalmometer. Test the six cardinal fields of gaze. Examine for conjunctival injection and follicles and for corneal cloudiness or white lesions.
Medical Causes
Conjunctivitis. Five types of conjunctivitis may cause an eye discharge with redness, hyperemia, foreign body sensation, periocular edema, and tearing.
With allergic conjunctivitis, a bilateral, white, ropey discharge is accompanied by itching and tearing.
Bacterial conjunctivitis causes a moderate purulent or mucopurulent discharge that may form sticky crusts on the eyelids during sleep. The discharge is commonly greenish or yellowish and usually occurs in one eye. The patient may also experience itching, burning, excessive tearing, and the sensation of a foreign body in the eye. Eye pain indicates corneal involvement. Preauricular adenopathy is uncommon.
Viral conjunctivitis is generally more common than the bacterial form. A serous, clear discharge and preauricular adenopathy are usually present. The history includes a runny nose, an upper respiratory tract infection, or recent contact with a person who had these signs. The onset is usually unilateral.
Fungal conjunctivitis produces a copious, thick, purulent discharge that makes the eyelids crusty and sticky. Also characteristic are eyelid edema, itching, burning, and tearing. Pain and photophobia occur only with corneal involvement.
Inclusion conjunctivitis causes scant mucoid discharge — especially in the morning — in both eyes, accompanied by pseudoptosis and conjunctival follicles.
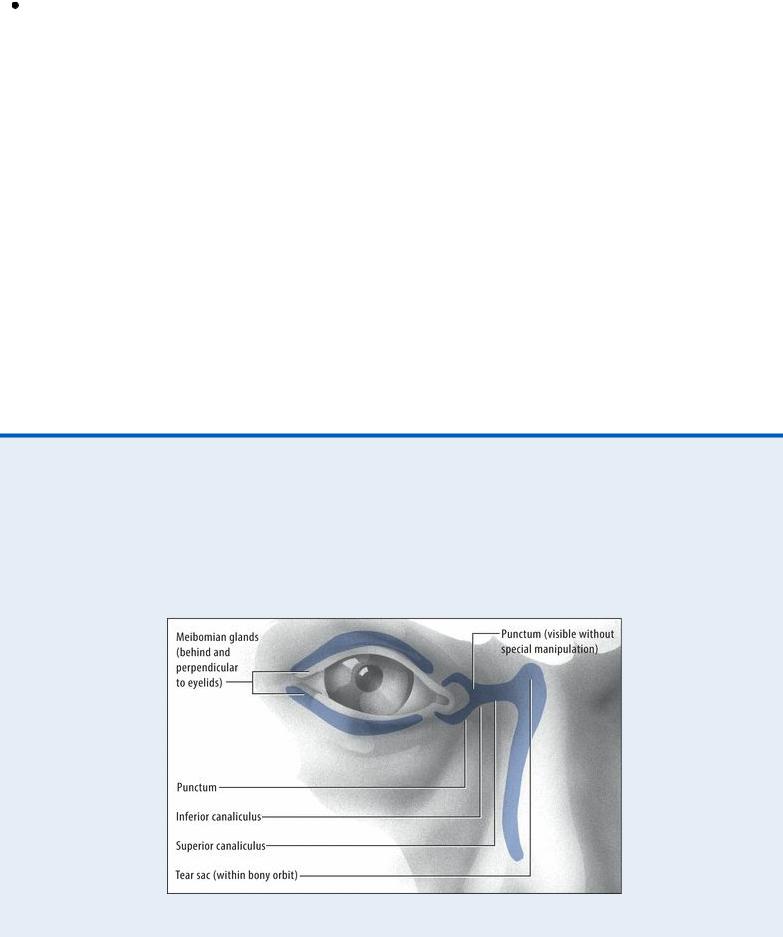
 EXAMINATION TIP Sources of Eye Discharge
EXAMINATION TIP Sources of Eye Discharge
Eye discharge can come from the tear sac, punctum, meibomian glands, or canaliculi. If the patient reports a discharge that isn’t immediately apparent, you can express a sample by pressing your fingertip lightly over these structures. Then characterize the discharge, and note its source.

Corneal ulcers. Bacterial and fungal corneal ulcers produce a copious, purulent unilateral eye discharge. Related findings are crusty, sticky eyelids, and, possibly, severe pain, photophobia, and impaired visual acuity.
Bacterial corneal ulcers are also characterized by an irregular gray-white area on the cornea, blurred vision, unilateral pupil constriction, and conjunctival injection.
Fungal corneal ulcers are also characterized by conjunctival injection and eyelid edema and erythema. A painless, dense, whitish gray central ulcer develops slowly and may be surrounded by progressively clearer rings.
Erythema multiforme major (Stevens-Johnson syndrome). A purulent discharge characterizes Stevens-Johnson syndrome. Other ocular effects may include severe eye pain, entropion, trichiasis, photophobia, and decreased tear formation. Also typical are erythematous, urticarial, bullous lesions that suddenly erupt over the skin.
Herpes zoster ophthalmicus. Herpes zoster ophthalmicus yields a moderate to copious serous eye discharge accompanied by excessive tearing. Examination reveals eyelid edema and erythema, conjunctival injection, and a white, cloudy cornea. The patient also complains of eye pain and severe unilateral facial pain that occurs several days before vesicles erupt.
Keratoconjunctivitis sicca. Better known as dry eye syndrome, keratoconjunctivitis sicca typically causes excessive, continuous mucoid discharge and insufficient tearing. Accompanying signs and symptoms include eye pain, itching, burning, a foreign body sensation, and dramatic conjunctival injection. The patient may also have difficulty closing his eyes.
Meibomianitis. Meibomianitis may produce a continuous frothy eye discharge. Applying pressure on the meibomian glands yields a soft, cheesy yellow discharge. The eyes also appear chronically red, with inflamed lid margins.
Orbital cellulitis. Although exophthalmos is the most obvious sign of this disorder, a unilateral purulent eye discharge may also be present. Related findings include eyelid edema, conjunctival injection, a headache, orbital pain, impaired visual acuity, limited extraocular movement, and a fever.
Psoriasis vulgaris. Usually, psoriasis vulgaris causes a substantial mucus discharge in both eyes, accompanied by redness. The characteristic lesions it produces on the eyelids may extend into the conjunctiva, causing irritation, excessive tearing, and a foreign body sensation.
Trachoma. A bilateral eye discharge occurs in trachoma along with severe pain, excessive tearing, photophobia, eyelid edema, redness, and visible conjunctival follicles.
Special Considerations
Apply warm soaks to soften crusts on the eyelids and lashes. Then gently wipe the eyes with a soft gauze pad. Carefully dispose of all used dressings, tissues, and cotton swabs to prevent the spread of infection. Teach the patient to avoid contaminating the unaffected eye and to refrain from sharing pillows, washcloths, eye drops, or eye makeup with others. Also, be sure to sterilize ophthalmic equipment after use.
Explain ordered diagnostic tests, including culture and sensitivity studies to identify infectious organisms.
Patient Counseling
Explain measures to prevent the spread of infection.
Pediatric Pointers
In infants, prophylactic eye medication (silver nitrate) commonly causes eye irritation and discharge. However, in children, discharges usually result from eye trauma, eye infection, or upper respiratory tract infection.
REFERENCES
Biswas, J. , Krishnakumar, S., & Ahuja, S. (2010) . Manual of ocular pathology. New Delhi, India: Jaypee—Highlights Medical Publishers.
Eagle, R. C. Jr. (2011). Eye pathology: An atlas and text. Philadelphia, PA: Lippincott Williams & Wilkins. Gerstenblith, A. T. & Rabinowitz, M. P. (2012). The wills eye manual. Philadelphia, PA: Lippincott Williams & Wilkins.
Holland, E. J., Mannis, M. J., & Lee, W. B. (2013). Ocular surface disease: Cornea, conjunctiva, and tear film. London: Elsevier Saunders.
Onofrey, B. E., Skorin, Leonid Jr, & Holdeman, N. R. (2011). Ocular therapeutics handbook: A clinical manual. Philadelphia, PA : Lippincott–Raven.
Roy, F. H. (2012). Ocular differential diagnosis. Clayton, Panama: Jaypee–Highlights Medical Publishers, Inc.
Eye Pain
(See Also Exophthalmus, Eye Discharge) [Ophthalmalgia]
Eye pain may be described as a burning, throbbing, aching, or stabbing sensation in or around the eye. It may also be characterized as a foreign body sensation. This sign varies from mild to severe; its duration and exact location provide clues to the causative disorder.
Eye pain often results from corneal abrasion, but it may also be due to glaucoma or other eye disorders, trauma, and neurologic or systemic disorders. Any of these may stimulate nerve endings in the cornea or external eye, producing pain.
 EMERGENCY INTERVENTIONS
EMERGENCY INTERVENTIONS
If the patient’s eye pain results from a chemical burn, remove contact lenses, if present, and irrigate the eye with at least 1 L of normal saline solution over 10 minutes. Evert the lids and wipe the fornices with a cotton-tipped applicator to remove any particles or chemicals. Eye pain from acute angle-closure glaucoma is an ocular emergency requiring immediate intervention to reduce intraocular pressure (IOP). If drug treatment doesn’t reduce IOP, the patient will need laser iridotomy or surgical peripheral iridectomy to save his vision.
History and Physical Examination
If the patient’s eye pain doesn’t result from a chemical burn, take a complete history. Have the patient describe the pain fully. Is it an ache or a sharp pain? How long does it last? Is it accompanied by burning, itching, or discharge? Find out when it began. Is it worse in the morning or late in the evening? Ask about recent trauma or surgery, especially if the patient complains of sudden, severe pain. Does he have headaches? If so, find out how often and at what time of day they occur.
During the physical examination, don’t manipulate the eye if you suspect trauma. Carefully assess

the lids and conjunctiva for redness, inflammation, and swelling. Then examine the eyes for ptosis or exophthalmos. Finally, test visual acuity with and without correction, and assess extraocular movements. Characterize any discharge. (See Examining the External Eye, page 306.)
Medical Causes
Acute angle-closure glaucoma. Blurred vision and sudden, excruciating pain in and around the eye characterize acute angle-closure glaucoma; the pain may be so severe that it causes nausea, vomiting, and abdominal pain. Other findings are halo vision, rapidly decreasing visual acuity, and a fixed, nonreactive, moderately dilated pupil.
 EXAMINATION TIP Examining the External Eye
EXAMINATION TIP Examining the External Eye
For patients with eye pain or other ocular symptoms, examination of the external eye forms an important part of the ocular assessment. Here’s how to examine the external eye.
First, inspect the eyelids for ptosis and incomplete closure. Also, observe the lids for edema, erythema, cyanosis, hematoma, and masses. Evaluate skin lesions, growths, swelling, and tenderness by gross palpation. Are the lids everted or inverted? Do the eyelashes turn inward? Have some of them been lost? Do the lashes adhere to one another or contain a discharge? Next, examine the lid margins, noting especially any debris, scaling, lesions, or unusual secretions. Also, watch for eyelid spasms.
Now gently retract the eyelid with your thumb and forefinger, and assess the conjunctiva for redness, cloudiness, follicles, and blisters or other lesions. Check for chemosis by pressing the lower lid against the eyeball and noting any bulging above this compression point. Observe the sclera, noting any change from its normal white color.
Next, shine a light across the cornea to detect scars, abrasions, or ulcers. Note color changes, dots, or opaque or cloudy areas. Also, assess the anterior eye chamber, which should be clean, deep, shadow-free, and filled with clear aqueous humor.
Inspect the color, shape, texture, and pattern of the iris. Then assess the pupils’ size, shape, and equality. Finally, evaluate their response to light. Are they sluggish, fixed, or unresponsive? Does pupil dilation or constriction occur only on one side?

Blepharitis. Burning pain in both eyelids is accompanied by itching, sticky discharge, and conjunctival injection. Related findings include a foreign body sensation, lid ulcerations, and loss of eyelashes.
Burns. With chemical burns, sudden and severe eye pain may occur with erythema and blistering of the face and lids, photophobia, miosis, conjunctival injection, blurring, and an inability to keep the eyelids open. With ultraviolet radiation burns, moderate to severe pain occurs about 12 hours after exposure along with photophobia and vision changes.
Chalazion. A chalazion causes localized tenderness and swelling on the upper or lower eyelid. Eversion of the lid reveals conjunctival injection and a small red lump.
Conjunctivitis. Some degree of eye pain and excessive tearing occurs with four types of conjunctivitis. Allergic conjunctivitis causes mild, burning, bilateral pain accompanied by itching, conjunctival injection, and a characteristic ropey discharge.
Bacterial conjunctivitis causes pain only when it affects the cornea. Otherwise, it produces burning and a foreign body sensation. A purulent discharge and conjunctival injection are also typical.
If the cornea is affected, fungal conjunctivitis may cause pain and photophobia. Even without corneal involvement, it produces itching, burning eyes; a thick, purulent discharge; and conjunctival injection.
Viral conjunctivitis produces itching, red eyes, a foreign body sensation, visible conjunctival follicles, tearing, and eyelid edema.
Corneal abrasions. With this type of injury, eye pain is characterized by a foreign body sensation. Excessive tearing, photophobia, and conjunctival injection are also common.
Corneal ulcers. Bacterial and fungal corneal ulcers cause severe eye pain. They may also cause a purulent eye discharge, sticky eyelids, photophobia, and impaired visual acuity. In addition, bacterial corneal ulcers produce a grayish white, irregularly shaped ulcer on the cornea; unilateral pupil constriction; and conjunctival injection. Fungal corneal ulcers produce conjunctival injection, eyelid edema and erythema, and a dense, cloudy, central ulcer surrounded by progressively clearer rings.
Dacryocystitis. Pain and tenderness near the tear sac characterize acute dacryocystitis. Additional signs include excessive tearing, a purulent discharge, eyelid erythema, and swelling in the lacrimal punctum area.
Episcleritis. Deep eye pain occurs as tissues over the sclera become inflamed. Related effects include photophobia, excessive tearing, and conjunctival edema.
Erythema multiforme major. Erythema multiforme major commonly produces severe eye pain, entropion, trichiasis, purulent conjunctivitis, photophobia, and decreased tear formation.
Foreign bodies in the cornea and conjunctiva. Sudden severe pain is common, but vision usually remains intact. Other findings include excessive tearing, photophobia, miosis, a foreign body sensation, a dark speck on the cornea, and dramatic conjunctival injection.
Hordeolum (sty). Hordeolum usually produces localized eye pain that increases as the sty grows. Eyelid erythema and edema are also common.
Iritis (acute). Moderate to severe eye pain occurs with severe photophobia, dramatic conjunctival injection, and blurred vision. The constricted pupil may respond poorly to light. Lacrimal gland tumor. A lacrimal gland tumor is a neoplastic lesion that usually produces unilateral eye pain, impaired visual acuity, and some degree of exophthalmos.

Migraine headache. Migraines can produce pain so severe that the eyes also ache. Additionally, nausea, vomiting, blurred vision, and light and noise sensitivity may occur.
Ocular laceration and intraocular foreign bodies. Penetrating eye injuries usually cause mild to severe unilateral eye pain and impaired visual acuity. Eyelid edema, conjunctival injection, and an abnormal pupillary response may also occur.
Optic neuritis. With optic neuritis, pain in and around the eye occurs with eye movement. Severe vision loss and tunnel vision develop but improve in 2 to 3 weeks. Pupils respond sluggishly to direct light but normally to consensual light.
Scleritis. Scleritis produces severe eye pain and tenderness, along with conjunctival injection, a bluish purple sclera and, possibly, photophobia and excessive tearing.
Sclerokeratitis. Inflammation of the sclera and cornea causes pain, burning, irritation, and photophobia.
Subdural hematoma. Following head trauma, a subdural hematoma commonly causes severe eye ache and headache. Related neurologic signs depend on the hematoma’s location and size. Trachoma. Along with pain in the affected eye, trachoma causes excessive tearing, photophobia, eye discharge, eyelid edema and redness, and visible conjunctival follicles. Uveitis. Anterior uveitis causes the sudden onset of severe pain, dramatic conjunctival injection, photophobia, and a small, nonreactive pupil.
Posterior uveitis causes an insidious onset of similar features as well as gradual blurring of vision and distorted pupil shape.
Lens-induced uveitis causes moderate eye pain, conjunctival injection, pupil constriction, and severely impaired visual acuity. In fact, the patient usually can perceive only light.
Other Causes
Treatments. Contact lenses may cause eye pain and a foreign body sensation. Ocular surgery may also produce eye pain, ranging from a mild ache to a severe pounding or stabbing sensation.
Special Considerations
To help ease eye pain, have the patient lie down in a darkened, quiet environment and close his eyes. Prepare him for diagnostic studies, including tonometry and orbital X-rays.
Patient Teaching
Stress the importance of following instructions for drug therapy and give careful instructions about eye protection. Explain that the patient should always seek medical attention for eye pain.
Pediatric Pointers
Trauma and infection are the most common causes of eye pain in children. Be alert for nonverbal clues to pain such as tightly shutting or frequently rubbing the eyes.
Geriatric Pointers
Glaucoma, which can cause eye pain, is usually a disease of older patients, becoming clinically significant after age 40. It usually occurs bilaterally and leads to slowly progressive vision loss,
especially in peripheral visual fields.
REFERENCES
Eagle, R. C. Jr. (2011). Eye pathology: An atlas and text. Philadelphia, PA: Lippincott Williams & Wilkins. Gerstenblith, A. T., & Rabinowitz, M. P. (2012). The wills eye manual. Philadelphia, PA: Lippincott Williams & Wilkins.
Huang, J. J., & Gaudio, P. A. (2010). Ocular inflammatory disease and uveitis manual: Diagnosis and treatment. Philadelphia, PA : Lippincott Williams & Wilkins.
Roy, F. H. (2012). Ocular differential diagnosis. Clayton, Panama: Jaypee–Highlights Medical Publishers, Inc.
