
- •Hematuria II: causes and investigation
- •Hematospermia
- •Lower urinary tract symptoms (LUTS)
- •Nocturia and nocturnal polyuria
- •Flank pain
- •Urinary incontinence in adults
- •Genital symptoms
- •Abdominal examination in urological disease
- •Digital rectal examination (DRE)
- •Lumps in the groin
- •Lumps in the scrotum
- •2 Urological investigations
- •Urine examination
- •Urine cytology
- •Radiological imaging of the urinary tract
- •Uses of plain abdominal radiography (KUB X-ray—kidneys, ureters, bladder)
- •Intravenous pyelography (IVP)
- •Other urological contrast studies
- •Computed tomography (CT) and magnetic resonance imaging (MRI)
- •Radioisotope imaging
- •Post-void residual urine volume measurement
- •3 Bladder outlet obstruction
- •Regulation of prostate growth and development of benign prostatic hyperplasia (BPH)
- •Pathophysiology and causes of bladder outlet obstruction (BOO) and BPH
- •Benign prostatic obstruction (BPO): symptoms and signs
- •Diagnostic tests in men with LUTS thought to be due to BPH
- •Why do men seek treatment for their symptoms?
- •Watchful waiting for uncomplicated BPH
- •Medical management of BPH: combination therapy
- •Medical management of BPH: alternative drug therapy
- •Minimally invasive management of BPH: surgical alternatives to TURP
- •Invasive surgical alternatives to TURP
- •TURP and open prostatectomy
- •Indications for and technique of urethral catheterization
- •Indications for and technique of suprapubic catheterization
- •Management of nocturia and nocturnal polyuria
- •High-pressure chronic retention (HPCR)
- •Bladder outlet obstruction and retention in women
- •Urethral stricture disease
- •4 Incontinence
- •Causes and pathophysiology
- •Evaluation
- •Treatment of sphincter weakness incontinence: injection therapy
- •Treatment of sphincter weakness incontinence: retropubic suspension
- •Treatment of sphincter weakness incontinence: pubovaginal slings
- •Overactive bladder: conventional treatment
- •Overactive bladder: options for failed conventional therapy
- •“Mixed” incontinence
- •Post-prostatectomy incontinence
- •Incontinence in the elderly patient
- •Urinary tract infection: microbiology
- •Lower urinary tract infection
- •Recurrent urinary tract infection
- •Urinary tract infection: treatment
- •Acute pyelonephritis
- •Pyonephrosis and perinephric abscess
- •Other forms of pyelonephritis
- •Chronic pyelonephritis
- •Septicemia and urosepsis
- •Fournier gangrene
- •Epididymitis and orchitis
- •Periurethral abscess
- •Prostatitis: presentation, evaluation, and treatment
- •Other prostate infections
- •Interstitial cystitis
- •Tuberculosis
- •Parasitic infections
- •HIV in urological surgery
- •6 Urological neoplasia
- •Pathology and molecular biology
- •Prostate cancer: epidemiology and etiology
- •Prostate cancer: incidence, prevalence, and mortality
- •Prostate cancer pathology: premalignant lesions
- •Counseling before prostate cancer screening
- •Prostate cancer: clinical presentation
- •PSA and prostate cancer
- •PSA derivatives: free-to-total ratio, density, and velocity
- •Prostate cancer: transrectal ultrasonography and biopsies
- •Prostate cancer staging
- •Prostate cancer grading
- •General principles of management of localized prostate cancer
- •Management of localized prostate cancer: watchful waiting and active surveillance
- •Management of localized prostate cancer: radical prostatectomy
- •Postoperative course after radical prostatectomy
- •Prostate cancer control with radical prostatectomy
- •Management of localized prostate cancer: radical external beam radiotherapy (EBRT)
- •Management of localized prostate cancer: brachytherapy (BT)
- •Management of localized and radiorecurrent prostate cancer: cryotherapy and HIFU
- •Management of locally advanced nonmetastatic prostate cancer (T3–4 N0M0)
- •Management of advanced prostate cancer: hormone therapy I
- •Management of advanced prostate cancer: hormone therapy II
- •Management of advanced prostate cancer: hormone therapy III
- •Management of advanced prostate cancer: androgen-independent/ castration-resistant disease
- •Palliative management of prostate cancer
- •Prostate cancer: prevention; complementary and alternative therapies
- •Bladder cancer: epidemiology and etiology
- •Bladder cancer: pathology and staging
- •Bladder cancer: presentation
- •Bladder cancer: diagnosis and staging
- •Muscle-invasive bladder cancer: surgical management of localized (pT2/3a) disease
- •Muscle-invasive bladder cancer: radical and palliative radiotherapy
- •Muscle-invasive bladder cancer: management of locally advanced and metastatic disease
- •Bladder cancer: urinary diversion after cystectomy
- •Transitional cell carcinoma (UC) of the renal pelvis and ureter
- •Radiological assessment of renal masses
- •Benign renal masses
- •Renal cell carcinoma: epidemiology and etiology
- •Renal cell carcinoma: pathology, staging, and prognosis
- •Renal cell carcinoma: presentation and investigations
- •Renal cell carcinoma: active surveillance
- •Renal cell carcinoma: surgical treatment I
- •Renal cell carcinoma: surgical treatment II
- •Renal cell carcinoma: management of metastatic disease
- •Testicular cancer: epidemiology and etiology
- •Testicular cancer: clinical presentation
- •Testicular cancer: serum markers
- •Testicular cancer: pathology and staging
- •Testicular cancer: prognostic staging system for metastatic germ cell cancer
- •Testicular cancer: management of non-seminomatous germ cell tumors (NSGCT)
- •Testicular cancer: management of seminoma, IGCN, and lymphoma
- •Penile neoplasia: benign, viral-related, and premalignant lesions
- •Penile cancer: epidemiology, risk factors, and pathology
- •Squamous cell carcinoma of the penis: clinical management
- •Carcinoma of the scrotum
- •Tumors of the testicular adnexa
- •Urethral cancer
- •Wilms tumor and neuroblastoma
- •7 Miscellaneous urological diseases of the kidney
- •Cystic renal disease: simple cysts
- •Cystic renal disease: calyceal diverticulum
- •Cystic renal disease: medullary sponge kidney (MSK)
- •Acquired renal cystic disease (ARCD)
- •Autosomal dominant (adult) polycystic kidney disease (ADPKD)
- •Ureteropelvic junction (UPJ) obstruction in adults
- •Anomalies of renal ascent and fusion: horseshoe kidney, pelvic kidney, malrotation
- •Renal duplications
- •8 Stone disease
- •Kidney stones: epidemiology
- •Kidney stones: types and predisposing factors
- •Kidney stones: mechanisms of formation
- •Evaluation of the stone former
- •Kidney stones: presentation and diagnosis
- •Kidney stone treatment options: watchful waiting
- •Stone fragmentation techniques: extracorporeal lithotripsy (ESWL)
- •Intracorporeal techniques of stone fragmentation (fragmentation within the body)
- •Kidney stone treatment: percutaneous nephrolithotomy (PCNL)
- •Kidney stones: open stone surgery
- •Kidney stones: medical therapy (dissolution therapy)
- •Ureteric stones: presentation
- •Ureteric stones: diagnostic radiological imaging
- •Ureteric stones: acute management
- •Ureteric stones: indications for intervention to relieve obstruction and/or remove the stone
- •Ureteric stone treatment
- •Treatment options for ureteric stones
- •Prevention of calcium oxalate stone formation
- •Bladder stones
- •Management of ureteric stones in pregnancy
- •Hydronephrosis
- •Management of ureteric strictures (other than UPJ obstruction)
- •Pathophysiology of urinary tract obstruction
- •Ureter innervation
- •10 Trauma to the urinary tract and other urological emergencies
- •Renal trauma: clinical and radiological assessment
- •Renal trauma: treatment
- •Ureteral injuries: mechanisms and diagnosis
- •Ureteral injuries: management
- •Bladder and urethral injuries associated with pelvic fractures
- •Bladder injuries
- •Posterior urethral injuries in males and urethral injuries in females
- •Anterior urethral injuries
- •Testicular injuries
- •Penile injuries
- •Torsion of the testis and testicular appendages
- •Paraphimosis
- •Malignant ureteral obstruction
- •Spinal cord and cauda equina compression
- •11 Infertility
- •Male reproductive physiology
- •Etiology and evaluation of male infertility
- •Lab investigation of male infertility
- •Oligospermia and azoospermia
- •Varicocele
- •Treatment options for male factor infertility
- •12 Disorders of erectile function, ejaculation, and seminal vesicles
- •Physiology of erection and ejaculation
- •Impotence: evaluation
- •Impotence: treatment
- •Retrograde ejaculation
- •Peyronie’s disease
- •Priapism
- •13 Neuropathic bladder
- •Innervation of the lower urinary tract (LUT)
- •Physiology of urine storage and micturition
- •Bladder and sphincter behavior in the patient with neurological disease
- •The neuropathic lower urinary tract: clinical consequences of storage and emptying problems
- •Bladder management techniques for the neuropathic patient
- •Catheters and sheaths and the neuropathic patient
- •Management of incontinence in the neuropathic patient
- •Management of recurrent urinary tract infections (UTIs) in the neuropathic patient
- •Management of hydronephrosis in the neuropathic patient
- •Bladder dysfunction in multiple sclerosis, in Parkinson disease, after stroke, and in other neurological disease
- •Neuromodulation in lower urinary tract dysfunction
- •14 Urological problems in pregnancy
- •Physiological and anatomical changes in the urinary tract
- •Urinary tract infection (UTI)
- •Hydronephrosis
- •15 Pediatric urology
- •Embryology: urinary tract
- •Undescended testes
- •Urinary tract infection (UTI)
- •Ectopic ureter
- •Ureterocele
- •Ureteropelvic junction (UPJ) obstruction
- •Hypospadias
- •Normal sexual differentiation
- •Abnormal sexual differentiation
- •Cystic kidney disease
- •Exstrophy
- •Epispadias
- •Posterior urethral valves
- •Non-neurogenic voiding dysfunction
- •Nocturnal enuresis
- •16 Urological surgery and equipment
- •Preparation of the patient for urological surgery
- •Antibiotic prophylaxis in urological surgery
- •Complications of surgery in general: DVT and PE
- •Fluid balance and management of shock in the surgical patient
- •Patient safety in the operating room
- •Transurethral resection (TUR) syndrome
- •Catheters and drains in urological surgery
- •Guide wires
- •JJ stents
- •Lasers in urological surgery
- •Diathermy
- •Sterilization of urological equipment
- •Telescopes and light sources in urological endoscopy
- •Consent: general principles
- •Cystoscopy
- •Transurethral resection of the prostate (TURP)
- •Transurethral resection of bladder tumor (TURBT)
- •Optical urethrotomy
- •Circumcision
- •Hydrocele and epididymal cyst removal
- •Nesbit procedure
- •Vasectomy and vasovasostomy
- •Orchiectomy
- •Urological incisions
- •JJ stent insertion
- •Nephrectomy and nephroureterectomy
- •Radical prostatectomy
- •Radical cystectomy
- •Ileal conduit
- •Percutaneous nephrolithotomy (PCNL)
- •Ureteroscopes and ureteroscopy
- •Pyeloplasty
- •Laparoscopic surgery
- •Endoscopic cystolitholapaxy and (open) cystolithotomy
- •Scrotal exploration for torsion and orchiopexy
- •17 Basic science of relevance to urological practice
- •Physiology of bladder and urethra
- •Renal anatomy: renal blood flow and renal function
- •Renal physiology: regulation of water balance
- •Renal physiology: regulation of sodium and potassium excretion
- •Renal physiology: acid–base balance
- •18 Urological eponyms
- •Index

456 CHAPTER 10 Trauma to the urinary tract
Penile injuries
Penile fracture
This involves rupture of the tunica albuginea of the erect penis (i.e., rupture of one or both corpora cavernosa and/or rupture of the corpus spongiosum and urethra). The tunica albuginea is 2 mm thick in the flaccid penis and thins to 0.25 mm during erection, which makes it vulnerable to rupture if the penis is forcibly bent (e.g., during vigorous sexual intercourse).
In general, the diagnosis of penile fracture is straightforward and based on the presence of classic history and physical findings. Delay in diagnosis is common, as many men are initially too embarrassed, ashamed, or frightened to present immediately for medical attention. Penile imaging is not needed to diagnose penile fracture, although MRI has been reported to be accurate in equivocal cases.
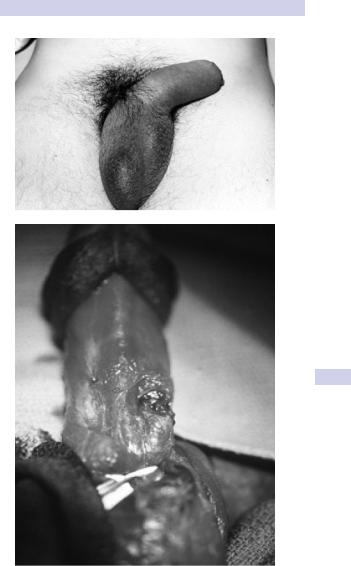
The patient usually reports a sudden “snapping” sound or “popping” sensation, with sudden penile pain and detumescence of the erection. The penis immediately becomes markedly swollen and bruised, a classic appearance known as the “eggplant” deformity (Fig. 10.16).
A tender, palpable defect may be felt over the site of the tear in the tunica albuginea. If Buck fascia has ruptured, bruising extends onto the lower abdominal wall and into the perineum and scrotum; otherwise, the discoloration is contained along the penile shaft.
If the urethra is damaged, there may be blood at the meatus or hematuria (dipstick/microscopic or macroscopic) and pain on voiding or urinary retention. Arrange a retrograde urethrogram or flexible cystoscopy in such cases. Immediate primary urethral repair is warranted for concomitant urethral injuries.
Treatment
Immediate surgical repair has been repeatedly associated with a lower complication rate (e.g., reduced impotence, penile deformity and scar tissue formation, prolonged penile pain) than that of conservative treatment of penile fracture.
The fracture site in the tunica albuginea is exposed via a circumcision incision, the hematoma evacuated, and the defect in the tunica closed with interrupted 2–0 absorbable sutures. Deep stitches in the underlying erectile tissue are unnecessary and possibly harmful; only tunical closure is warranted.
A self-adhesive compressive bandage, application of cold compresses to the penis, analgesics and anti-inflammatory drugs, and abstinence from sexual activity for 6–8 weeks are prudent adjunct measures to promote optimal healing.
Surgical repair of penile fracture
Expose the fracture site by degloving the penis via a circumcising incision around the subcoronal sulcus or by an incision directly over the defect if palpable. A degloving incision allows better exposure of the urethra for associated urethral injuries.
Alternatively, use a midline incision extending distally from the midline raphe of the scrotum, along the shaft of the penis. This latter incision,
PENILE INJURIES 457
A
B
Figure 10.16 A) Typical “eggplant deformity” appearance of fractured penis. B) Intraoperative appearance of penile fracture—a transverse defect in the tunica albuginea in the midshaft.

458 CHAPTER 10 Trauma to the urinary tract
along with a degloving incision, allows excellent exposure of both corpora cavernosa so that an unexpected bilateral injury can be repaired easily, as can a urethral injury should this have occurred.
Close the defect in the tunica albuginea with absorbable 2–0 sutures. Cover the knots with Buck fascia or bury them so that the patient is unable to palpate them. Leave a urethral catheter overnight (voiding can be difficult immediately postoperatively). Repair a urethral rupture, if present, with a spatulated single or two-layer urethral anastomosis, and splint repair with a urethral catheter for 2 weeks.
Amputation
Place the amputated penile remnant, if found, in a wet gauze pad inside a plastic bag, which is then placed inside another bag containing ice (bag in a bag). It can survive for 24 hours.
Blood loss can be severe; resuscitate the shocked patient and crossmatch blood. Consider psychiatric consultation if the wound was selfinflicted.
Knife and gunshot wounds
Associated injuries are common (e.g., scrotum, major vessels of the lower limb). Most corporal injuries, other than minor ones, should undergo primary repair to prevent long-term disturbance of erectile function.
Remove debris from wound (e.g., particles of clothing) and débride necrotic tissue sparingly. Repair as for penile fractures (see Box 10.7).

PENILE INJURIES 459
Box 10.7 Treatment of penile injuries
Surgical reimplantation of amputated penis
Repair the urethra first, over a catheter, to provide a stable base for subsequent neurovascular repair. Concomitant suprapubic urinary diversion is usually recommended. Close the tunica albuginea of the corpora with 2–0 absorbable sutures.
Cavernosal artery repair is not recommended, since it is technically very difficult and does not improve penile viability.
Microsurgical anastomosis (via plastic surgical consultation) is then performed on the dorsal artery of the penis, the dorsal vein to provide venous drainage, and, finally, the dorsal penile nerve and skin. In the absence of microsurgical expertise availability, a “macroreplantation” of the urethra, corpora, and skin is acceptable.
Penile bites and skin loss injuries
Clean the wound copiously. Give broad-spectrum antibiotics (e.g., cephalosporin and amoxycillin). If skin loss has occurred via degloving injury, a loose primary closure with 3–0 chromic is recommended.
Zipper injuries
If the penis is still caught in the zipper, use lubricant jelly and gently attempt to open it. The zipper bar may have to be cut with orthopedic cutters or pried apart with a pair of surgical clamps on either side of the zipper.
