
- •Hematuria II: causes and investigation
- •Hematospermia
- •Lower urinary tract symptoms (LUTS)
- •Nocturia and nocturnal polyuria
- •Flank pain
- •Urinary incontinence in adults
- •Genital symptoms
- •Abdominal examination in urological disease
- •Digital rectal examination (DRE)
- •Lumps in the groin
- •Lumps in the scrotum
- •2 Urological investigations
- •Urine examination
- •Urine cytology
- •Radiological imaging of the urinary tract
- •Uses of plain abdominal radiography (KUB X-ray—kidneys, ureters, bladder)
- •Intravenous pyelography (IVP)
- •Other urological contrast studies
- •Computed tomography (CT) and magnetic resonance imaging (MRI)
- •Radioisotope imaging
- •Post-void residual urine volume measurement
- •3 Bladder outlet obstruction
- •Regulation of prostate growth and development of benign prostatic hyperplasia (BPH)
- •Pathophysiology and causes of bladder outlet obstruction (BOO) and BPH
- •Benign prostatic obstruction (BPO): symptoms and signs
- •Diagnostic tests in men with LUTS thought to be due to BPH
- •Why do men seek treatment for their symptoms?
- •Watchful waiting for uncomplicated BPH
- •Medical management of BPH: combination therapy
- •Medical management of BPH: alternative drug therapy
- •Minimally invasive management of BPH: surgical alternatives to TURP
- •Invasive surgical alternatives to TURP
- •TURP and open prostatectomy
- •Indications for and technique of urethral catheterization
- •Indications for and technique of suprapubic catheterization
- •Management of nocturia and nocturnal polyuria
- •High-pressure chronic retention (HPCR)
- •Bladder outlet obstruction and retention in women
- •Urethral stricture disease
- •4 Incontinence
- •Causes and pathophysiology
- •Evaluation
- •Treatment of sphincter weakness incontinence: injection therapy
- •Treatment of sphincter weakness incontinence: retropubic suspension
- •Treatment of sphincter weakness incontinence: pubovaginal slings
- •Overactive bladder: conventional treatment
- •Overactive bladder: options for failed conventional therapy
- •“Mixed” incontinence
- •Post-prostatectomy incontinence
- •Incontinence in the elderly patient
- •Urinary tract infection: microbiology
- •Lower urinary tract infection
- •Recurrent urinary tract infection
- •Urinary tract infection: treatment
- •Acute pyelonephritis
- •Pyonephrosis and perinephric abscess
- •Other forms of pyelonephritis
- •Chronic pyelonephritis
- •Septicemia and urosepsis
- •Fournier gangrene
- •Epididymitis and orchitis
- •Periurethral abscess
- •Prostatitis: presentation, evaluation, and treatment
- •Other prostate infections
- •Interstitial cystitis
- •Tuberculosis
- •Parasitic infections
- •HIV in urological surgery
- •6 Urological neoplasia
- •Pathology and molecular biology
- •Prostate cancer: epidemiology and etiology
- •Prostate cancer: incidence, prevalence, and mortality
- •Prostate cancer pathology: premalignant lesions
- •Counseling before prostate cancer screening
- •Prostate cancer: clinical presentation
- •PSA and prostate cancer
- •PSA derivatives: free-to-total ratio, density, and velocity
- •Prostate cancer: transrectal ultrasonography and biopsies
- •Prostate cancer staging
- •Prostate cancer grading
- •General principles of management of localized prostate cancer
- •Management of localized prostate cancer: watchful waiting and active surveillance
- •Management of localized prostate cancer: radical prostatectomy
- •Postoperative course after radical prostatectomy
- •Prostate cancer control with radical prostatectomy
- •Management of localized prostate cancer: radical external beam radiotherapy (EBRT)
- •Management of localized prostate cancer: brachytherapy (BT)
- •Management of localized and radiorecurrent prostate cancer: cryotherapy and HIFU
- •Management of locally advanced nonmetastatic prostate cancer (T3–4 N0M0)
- •Management of advanced prostate cancer: hormone therapy I
- •Management of advanced prostate cancer: hormone therapy II
- •Management of advanced prostate cancer: hormone therapy III
- •Management of advanced prostate cancer: androgen-independent/ castration-resistant disease
- •Palliative management of prostate cancer
- •Prostate cancer: prevention; complementary and alternative therapies
- •Bladder cancer: epidemiology and etiology
- •Bladder cancer: pathology and staging
- •Bladder cancer: presentation
- •Bladder cancer: diagnosis and staging
- •Muscle-invasive bladder cancer: surgical management of localized (pT2/3a) disease
- •Muscle-invasive bladder cancer: radical and palliative radiotherapy
- •Muscle-invasive bladder cancer: management of locally advanced and metastatic disease
- •Bladder cancer: urinary diversion after cystectomy
- •Transitional cell carcinoma (UC) of the renal pelvis and ureter
- •Radiological assessment of renal masses
- •Benign renal masses
- •Renal cell carcinoma: epidemiology and etiology
- •Renal cell carcinoma: pathology, staging, and prognosis
- •Renal cell carcinoma: presentation and investigations
- •Renal cell carcinoma: active surveillance
- •Renal cell carcinoma: surgical treatment I
- •Renal cell carcinoma: surgical treatment II
- •Renal cell carcinoma: management of metastatic disease
- •Testicular cancer: epidemiology and etiology
- •Testicular cancer: clinical presentation
- •Testicular cancer: serum markers
- •Testicular cancer: pathology and staging
- •Testicular cancer: prognostic staging system for metastatic germ cell cancer
- •Testicular cancer: management of non-seminomatous germ cell tumors (NSGCT)
- •Testicular cancer: management of seminoma, IGCN, and lymphoma
- •Penile neoplasia: benign, viral-related, and premalignant lesions
- •Penile cancer: epidemiology, risk factors, and pathology
- •Squamous cell carcinoma of the penis: clinical management
- •Carcinoma of the scrotum
- •Tumors of the testicular adnexa
- •Urethral cancer
- •Wilms tumor and neuroblastoma
- •7 Miscellaneous urological diseases of the kidney
- •Cystic renal disease: simple cysts
- •Cystic renal disease: calyceal diverticulum
- •Cystic renal disease: medullary sponge kidney (MSK)
- •Acquired renal cystic disease (ARCD)
- •Autosomal dominant (adult) polycystic kidney disease (ADPKD)
- •Ureteropelvic junction (UPJ) obstruction in adults
- •Anomalies of renal ascent and fusion: horseshoe kidney, pelvic kidney, malrotation
- •Renal duplications
- •8 Stone disease
- •Kidney stones: epidemiology
- •Kidney stones: types and predisposing factors
- •Kidney stones: mechanisms of formation
- •Evaluation of the stone former
- •Kidney stones: presentation and diagnosis
- •Kidney stone treatment options: watchful waiting
- •Stone fragmentation techniques: extracorporeal lithotripsy (ESWL)
- •Intracorporeal techniques of stone fragmentation (fragmentation within the body)
- •Kidney stone treatment: percutaneous nephrolithotomy (PCNL)
- •Kidney stones: open stone surgery
- •Kidney stones: medical therapy (dissolution therapy)
- •Ureteric stones: presentation
- •Ureteric stones: diagnostic radiological imaging
- •Ureteric stones: acute management
- •Ureteric stones: indications for intervention to relieve obstruction and/or remove the stone
- •Ureteric stone treatment
- •Treatment options for ureteric stones
- •Prevention of calcium oxalate stone formation
- •Bladder stones
- •Management of ureteric stones in pregnancy
- •Hydronephrosis
- •Management of ureteric strictures (other than UPJ obstruction)
- •Pathophysiology of urinary tract obstruction
- •Ureter innervation
- •10 Trauma to the urinary tract and other urological emergencies
- •Renal trauma: clinical and radiological assessment
- •Renal trauma: treatment
- •Ureteral injuries: mechanisms and diagnosis
- •Ureteral injuries: management
- •Bladder and urethral injuries associated with pelvic fractures
- •Bladder injuries
- •Posterior urethral injuries in males and urethral injuries in females
- •Anterior urethral injuries
- •Testicular injuries
- •Penile injuries
- •Torsion of the testis and testicular appendages
- •Paraphimosis
- •Malignant ureteral obstruction
- •Spinal cord and cauda equina compression
- •11 Infertility
- •Male reproductive physiology
- •Etiology and evaluation of male infertility
- •Lab investigation of male infertility
- •Oligospermia and azoospermia
- •Varicocele
- •Treatment options for male factor infertility
- •12 Disorders of erectile function, ejaculation, and seminal vesicles
- •Physiology of erection and ejaculation
- •Impotence: evaluation
- •Impotence: treatment
- •Retrograde ejaculation
- •Peyronie’s disease
- •Priapism
- •13 Neuropathic bladder
- •Innervation of the lower urinary tract (LUT)
- •Physiology of urine storage and micturition
- •Bladder and sphincter behavior in the patient with neurological disease
- •The neuropathic lower urinary tract: clinical consequences of storage and emptying problems
- •Bladder management techniques for the neuropathic patient
- •Catheters and sheaths and the neuropathic patient
- •Management of incontinence in the neuropathic patient
- •Management of recurrent urinary tract infections (UTIs) in the neuropathic patient
- •Management of hydronephrosis in the neuropathic patient
- •Bladder dysfunction in multiple sclerosis, in Parkinson disease, after stroke, and in other neurological disease
- •Neuromodulation in lower urinary tract dysfunction
- •14 Urological problems in pregnancy
- •Physiological and anatomical changes in the urinary tract
- •Urinary tract infection (UTI)
- •Hydronephrosis
- •15 Pediatric urology
- •Embryology: urinary tract
- •Undescended testes
- •Urinary tract infection (UTI)
- •Ectopic ureter
- •Ureterocele
- •Ureteropelvic junction (UPJ) obstruction
- •Hypospadias
- •Normal sexual differentiation
- •Abnormal sexual differentiation
- •Cystic kidney disease
- •Exstrophy
- •Epispadias
- •Posterior urethral valves
- •Non-neurogenic voiding dysfunction
- •Nocturnal enuresis
- •16 Urological surgery and equipment
- •Preparation of the patient for urological surgery
- •Antibiotic prophylaxis in urological surgery
- •Complications of surgery in general: DVT and PE
- •Fluid balance and management of shock in the surgical patient
- •Patient safety in the operating room
- •Transurethral resection (TUR) syndrome
- •Catheters and drains in urological surgery
- •Guide wires
- •JJ stents
- •Lasers in urological surgery
- •Diathermy
- •Sterilization of urological equipment
- •Telescopes and light sources in urological endoscopy
- •Consent: general principles
- •Cystoscopy
- •Transurethral resection of the prostate (TURP)
- •Transurethral resection of bladder tumor (TURBT)
- •Optical urethrotomy
- •Circumcision
- •Hydrocele and epididymal cyst removal
- •Nesbit procedure
- •Vasectomy and vasovasostomy
- •Orchiectomy
- •Urological incisions
- •JJ stent insertion
- •Nephrectomy and nephroureterectomy
- •Radical prostatectomy
- •Radical cystectomy
- •Ileal conduit
- •Percutaneous nephrolithotomy (PCNL)
- •Ureteroscopes and ureteroscopy
- •Pyeloplasty
- •Laparoscopic surgery
- •Endoscopic cystolitholapaxy and (open) cystolithotomy
- •Scrotal exploration for torsion and orchiopexy
- •17 Basic science of relevance to urological practice
- •Physiology of bladder and urethra
- •Renal anatomy: renal blood flow and renal function
- •Renal physiology: regulation of water balance
- •Renal physiology: regulation of sodium and potassium excretion
- •Renal physiology: acid–base balance
- •18 Urological eponyms
- •Index

406 CHAPTER 9 Upper tract obstruction
Hydronephrosis
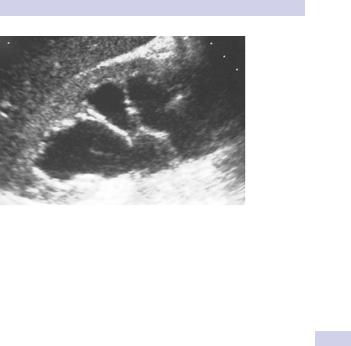
Hydronephrosis is dilatation of the renal pelvis and calyces (Fig. 9.1). When combined with dilatation of the ureters it is known as hydroureteronephrosis.
Obstructive nephropathy is damage to the renal parenchyma resulting from obstruction to the flow of urine anywhere along the urinary tract.
Dilatation of the renal pelvis and calyces can occur without obstruction and thus hydronephrosis should not be taken to necessarily imply the presence of obstructive uropathy.
Ultrasound
•False negative (i.e., obstruction present, no hydronephrosis)—acute onset of obstruction; in the presence of an intrarenal collecting system; with dehydration; misdiagnosis of dilatation of the calyces as renal cortical cysts (in acute ureteric colic, ultrasonography fails to detect hydronephrosis in up to 35% of patients with proven acute obstruction on IVP)
•False positive (i.e., hydronephrosis, no obstruction)—capacious extrarenal pelvis; parapelvic cysts; vesicoureteric reflux; high urine flow
Diagnostic approach to the patient with hydronephrosis
Hydronephrosis may present either as an incidental finding on an ultrasound or CT done because of nonspecific symptoms or it may be identified in a patient with a raised creatinine or presenting with flank pain.
Symptoms, if present, will depend on the rapidity of onset of obstruction of the kidney (if that is the cause of the hydronephrosis); whether obstruction is complete or partial, unilateral or bilateral; and whether the obstruction to the ureter is extrinsic to the ureter or within its lumen.
Causes of hydronephrosis are listed in Box 9.1.
History
•Severe flank pain suggests a more acute onset of obstruction and, if very sudden in onset, a ureteric stone may well be the cause. Pain induced by a diuresis (e.g., following consumption of alcohol) suggests a possible UPJ obstruction (See Chapter 7, p. 346).
•Anuria (the symptom of bilateral ureteric obstruction or complete obstruction of a solitary kidney)
•If renal function is impaired, symptoms of renal failure may be present (e.g., nausea, lethargy, anorexia).
•Extrinsic causes of obstruction (e.g., compression of the ureters by retroperitoneal malignancy) usually have a more insidious onset, whereas intrinsic obstruction (ureteric stone) is often present with severe pain of very sudden onset.
•An increase in urine output may be reported by the patient that is due to poor renal concentrating ability.
•Obstruction in the presence of bacterial urinary tract infection—signs and symptoms of pyelonephritis (flank pain and tenderness, fever) or sepsis
HYDRONEPHROSIS 407
Figure 9.1 Hydronephrosis as seen on renal ultrasonography.
Examination
•Measure blood pressure—elevated in high-pressure chronic retention (HPCR) due to benign prostatic obstruction (caused by fluid overload).
•Bilateral edema (due to fluid overload)
•Abdominal examination—percuss and palpate for an enlarged bladder.
•In men, DRE (?prostate or rectal cancer), and in women, vaginal examination (?cervical cancer)
•Check serum creatinine to determine the functional effect of the hydronephrosis.
•Renal ultrasonography (if not already done)
IVP findings in renal obstruction
•An obstructive (dense) nephrogram
•A delay in filling of the collecting system with contrast material
•Dilatation of the collecting system
•An increase in renal size
•Rupture of fornices (junction between renal papilla and its calyx) with urinary extravasation
•Ureteric dilatation and tortuosity
•A standing column of contrast material in the ureter
Unilateral hydronephrosis
Obtain a KUB X-ray (a ureteric stone may be seen), or CTU (or IVP) if a stone is suspected.
•If no stone is seen, but hydronephrosis is confirmed and ureter is nondilated, the obstruction must be at the UPJ. In the absence of a ureteric stone visible on CTU, the diagnosis must be UPJ obstruction.
•If no stone is seen and the ureter is dilated as well as kidney, ureteric TCC is likely. Arrange for retrograde pyelography to identify site of obstruction, and ureteroscopy/ureteric biopsy.

408 CHAPTER 9 Upper tract obstruction
Bilateral hydronephrosis
•If the patient is in retention or has a substantial post-void residual urine volume, pass a catheter. If the elevated creatinine falls (and the hydronephrosis improves), the diagnosis is bladder outlet obstruction (BOO), due, for example, to BPH, prostate cancer, urethral stricture, or detrusor-sphincter dyssynergia. If the creatinine remains elevated, the obstruction affecting both ureters is higher upstream.
•Obtain TRUS and prostatic biopsy if prostate cancer is suspected on DRE, and a CT scan to look for malignant bilateral ureteric obstruction or abdominal aortic aneurism (AAA).

HYDRONEPHROSIS 409
Box 9.1 Causes of hydronephrosis
Unilateral
•Obstructing ureteric stone
•UPJ obstruction
•Obstructing clot in ureter
•Obstructing ureteric TCC
•Any of the causes listed below when the pathological process has not yet extended to involve both ureters
Bilateral
•Bladder outlet obstruction (BOO)
•BPH
•Prostate cancer
•Urethral stricture
•Detrusor-sphincter dyssynergia (DSD)
•Posterior urethral valve
•Bilateral ureteric obstruction at their level of entry into the bladder
•Locally advanced cervical cancer
•Locally advanced prostate cancer
•Locally advanced rectal cancer
•Poor bladder compliance (often combined with DSD): neuropathic bladder (spinal cord injury, spina bifida); post-pelvic radiotherapy
•Periureteric inflammation
•From adjacent bowel involved with inflammatory bowel disease (e.g., Crohn’s, ulcerative colitis) or diverticular disease
•Retroperitoneal fibrosis
•Idiopathic (diagnosed following exclusion of other causes)
•Periarteritis—aortic aneurysm, iliac artery aneurysm
•Post-irradiation
•Drugs—methysergide, hydralazine, haloperidol, LSD, methyldopa, B-blockers, phenacetin, amphetamines
•Malignant—retroperitoneal malignancy (lymphoma, metastatic disease from e.g., breast cancer), post-chemotherapy
•Chemicals—talcum powder
•Infection—TB, syphilis, gonorrhea, chronic UTI
•Sarcoidosis
•Bilateral UPJ obstruction (uncommon)
•Hydronephrosis of pregnancy (partly due to smooth-muscle relaxant effect of progesterone, partly obstruction of ureters by fetus)
•Hydronephrosis in association with an ileal conduit (a substantial proportion of patients with ileal conduit urinary diversion have bilateral hydronephrosis, in the absence of obstruction)
•Bilateral ureteric stones (rare)
