
- •Overview
- •Ethiology
- •Prognosis
- •Cholinesterase Inhibitors Class Summary
- •Donepezil (Aricept, Aricept odt)
- •Rivastigmine (Exelon, Exelon Patch)
- •Galantamine (Razadyne, Razadyne er)
- •N-Methyl-d-Aspartate Antagonists Class Summary
- •Memantine (Namenda, Namenda xr)
- •Nutritional Supplement
- •Summary
- •Краткое изложение
- •Глоссарий
- •Neuropsychological testing - нейропсихологические тесты-
- •References
- •Appendix donepezil (Rx) - Aricept, Aricept odt
- •Rivastigmine (Rx) - Exelon, Exelon Patch
- •Galantamine (Rx) - Razadyne
- •Memantine (Rx) - Namenda xr
Overview
Alzheimer disease (AD) is an acquired disorder of cognitive and behavioral impairment that markedly interferes with social and occupational functioning. It is an incurable disease with a long and progressive course. In AD, plaques develop in the hippocampus, a structure deep in the brain that helps to encode memories, and in other areas of the cerebral cortex that are used in thinking and making decisions. Whether plaques themselves cause AD or whether they are a by-product of the AD process is still unknown. See the image below.
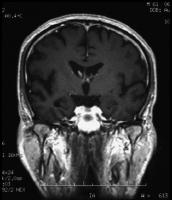
Coronal T1-weighted magnetic resonance imaging (MRI) scan in a patient with moderate Alzheimer disease. Brain image reveals hippocampal atrophy, especially on the right side.
Signs and symptoms
Preclinical Alzheimer disease
A patient with preclinical AD may appear completely normal on physical examination and mental status testing. Specific regions of the brain (eg, entorhinal cortex, hippocampus) probably begin to be affected 10-20 years before any visible symptoms appear.
Mild Alzheimer disease
Signs of mild AD can include the following:
Memory loss
Confusion about the location of familiar places
Taking longer to accomplish normal, daily tasks
Trouble handling money and paying bills
Compromised judgment, often leading to bad decisions
Loss of spontaneity and sense of initiative
Mood and personality changes; increased anxiety
Moderate Alzheimer disease
The symptoms of this stage can include the following:
Increasing memory loss and confusion
Shortened attention span
Problems recognizing friends and family members
Difficulty with language; problems with reading, writing, working with numbers
Difficulty organizing thoughts and thinking logically
Inability to learn new things or to cope with new or unexpected situations
Restlessness, agitation, anxiety, tearfulness, wandering, especially in the late afternoon or at night
Repetitive statements or movement; occasional muscle twitches
Hallucinations, delusions, suspiciousness or paranoia, irritability
Loss of impulse control: Shown through behavior such as undressing at inappropriate times or places or vulgar language
Perceptual-motor problems: Such as trouble getting out of a chair or setting the table
Severe Alzheimer disease
Patients with severe AD cannot recognize family or loved ones and cannot communicate in any way. They are completely dependent on others for care, and all sense of self seems to vanish.
Other symptoms of severe AD can include the following:
Weight loss
Seizures, skin infections, difficulty swallowing
Groaning, moaning, or grunting
Increased sleeping
Lack of bladder and bowel control
In end-stage AD, patients may be in bed much or all of the time. Death is often the result of other illnesses, frequently aspiration pneumonia.
Diagnosis
Means of diagnosing AD include the following:
Clinical examination: The clinical diagnosis of AD is usually made during the mild stage of the disease, using the above-listed signs
Lumbar puncture: levels of tau and phosphorylated tau in the cerebrospinal fluid are often elevated in AD, whereas amyloid levels are usually low; at present, however, routine measurement of CSF tau and amyloid is not recommended except in research settings
Imaging studies: Imaging studies (eg, computed tomography [CT]; magnetic resonance imaging [MRI]; and, in selected cases, single-photon emission CT [SPECT] or positron emission tomography [PET]) and laboratory tests may be used. These tests help exclude other possible causes for dementia (eg, cerebrovascular disease, cobalamin [vitamin B12] deficiency, syphilis, thyroid disease) and rule out potentially treatable causes of progressive cognitive decline, such as chronic subdural hematoma or normal-pressure hydrocephalus
Essential update: Brain protein may be biomarker for Alzheimer's up to ten years before diagnosis
In a cross-sectional study of 48 AD patients without diabetes, 20 cognitively normal diabetic patients, 16 patients with frontotemporal dementia, and 84 cognitively normal controls, researchers found that dysfunctionally phosphorylated insulin receptor substrate-1 (IRS-1), a neuronal protein, is detectable in blood using exosome-based technology and may be able to predict AD up to 10 years before the appearance of symptoms.
Compared with all other groups, patients with AD had several-fold higher p-Ser312-IRS-1 and Ser312/p-panY ratios and lower p-panY-IRS-1. In a longitudinal analysis of 22 of the AD patients who provided blood samples 1 to 10 years before diagnosis, preclinical and clinical levels of all three proteins were indistinguishable, while preclinical levels differed significantly from those of control s (P < .001).
