
clavien_atlas_of_upper_gastrointestinal_and_hepato-pancreato-biliary_surgery2007-10-01_3540200045_springer
.pdf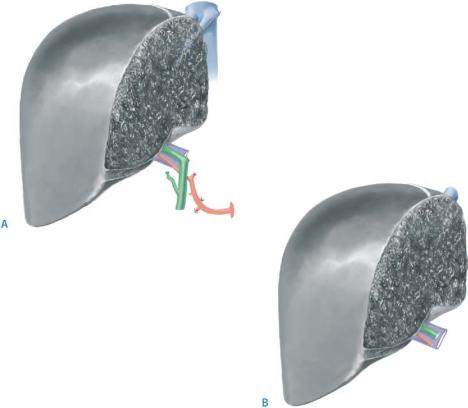
Auxiliary Liver Transplantation |
517 |
|
|
STEP 2 |
Preparation of the right liver graft |
|
|
A right cadaveric graft is ideally split in situ. If performed ex situ the median hepatic vein should be preserved on the graft side in order to avoid congestion and bleeding of the graft cut surface at the time of revascularization. The graft includes (A):
■Segments 5–8
■The right branch of the hepatic artery
■The right branch of the portal vein
■The right hepatic duct(s) along with the confluence and the common hepatic duct
■The right and median hepatic vein both attached to the retrohepatic inferior vena cava. Since the left hepatic vein has been divided by retaining a narrow patch from the common trunk, the defect has to be closed by transverse suture
In a right living donor graft (see also chapter on living donor liver transplantation), the retrohepatic vena cava, median hepatic vein, and extrahepatic biliary tract must stay on the donor side. Consequently, the graft includes (B):
■Segments 5–8
■The right branch(es) of the hepatic artery
■The right branch(es) of the portal vein
■The right hepatic duct(s)
■The right hepatic vein
518 |
SECTION 3 |
Liver |
|
|
|
|
Implantation of a Right Liver Graft from a Cadaveric Donor |
|
|
|
|
STEP 3 |
Caval anastomosis |
|
|
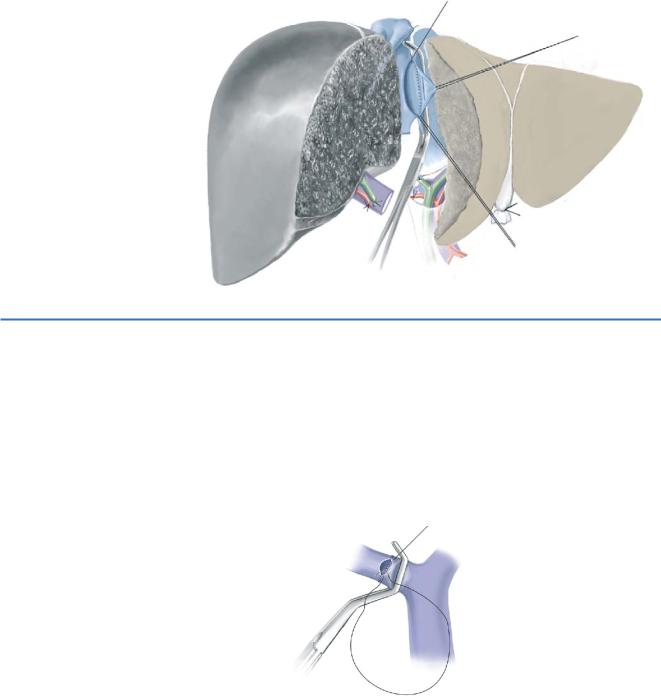
In a cadaveric graft, a caval implantation is performed. The native IVC is clamped later- |
|
|
||
|
ally and opened for about 5cm including the ostium of the right hepatic vein. The left |
|
|
side of the graft IVC is widely opened and a side-to-side cavocavostomy with a contin- |
|
uous 4-0 Prolene suture is performed. While the posterior layer is stitched, the graft is flushed with Ringer’s or 4% albumin solution.
STEP 4 |
Portal vein and arterial anastomosis |
|
The native right portal branch stump is clamped at its origin, and it is widely opened. |
|
|
|
The length of the graft portal vein is accurately adjusted in order to avoid tearing or |
|
kinking. An end-to-end anastomosis is performed between the donor and recipient right |
|
portal branch with a 5-0 or 6-0 Prolene running suture, leaving a growth factor of about |
|
5mm. The graft is then revascularized and careful hemostasis performed. |
|
The standard artery reconstruction is an end-to-end anastomosis between the |
|
donor and recipient right hepatic artery, using separate stitches of 8-0 Prolene. Donor |
|
saphenous vein interposition may be necessary to implant the graft artery more |
|
proximally on the recipient celiac axis. |
Auxiliary Liver Transplantation |
519 |
|
|
STEP 5 |
Reconstruction of the biliary tract |
|
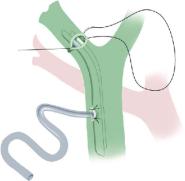
After careful hemosthasis, a standard direct duct-to-duct anastomosis with separate |
|
|
|
PDS 6-0 stitches is performed and a T-drain is inserted. If a standard choledocho- |
|
choledochostomy cannot be performed, a Roux-en-Y hepaticojejunostomy would |
|
be performed. |
Note: Implantation of a Right Liver Graft from a Living Donor
The right liver graft from a living donor differs from the cadaveric graft implantation at step 1 only. Since the IVC has been left to the donor, the graft’s right hepatic vein is implanted in an end-to-side fashion to the recipient IVC
520 |
SECTION 3 |
Liver |
|
|
|
|
|
|
Left Auxiliary Partial Orthotopic Liver Transplantation |
|
|
|
Left APOLT is recommended for children since an adult right liver graft may be too |
|
|
|
large. An adult left lobe or left hemiliver graft is sufficient to provide a graft |
|
|
|
weight/patient weigh ratio above 1%. |
|
|
|
|
|
|
STEP 1 |
Removal of the native left hemiliver and preparation of the graft |
|
|
|
The resection of the native left hemiliver can be performed under selective occlusion |
|
|
|
|
||
|
of the left portal triad (see chapter “Segmentectomies, Sectionectomies and Wedge |
|
|
|
Resections”) and includes resection of segment 1 with preservation of the median |
|
|
|
hepatic vein in the right hemiliver. The left side of the retrohepatic segment of the |
|
|
|
inferior vena cava is widely exposed to facilitate the left hepatic graft implantation. |
|
|
|
|
For the preparation of the graft, resection of Sg1 is recommended, regardless of the |
|
|
type of graft (Sg2 and 3 or left hemiliver) or the type of donor (cadaveric or living). |
|
|
|
|
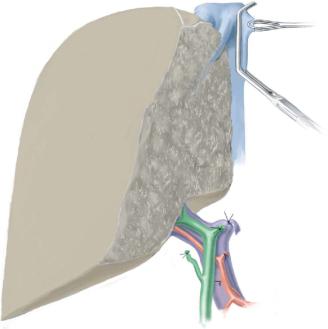
The left grafts include: |
|
|
■ |
The left branch of the hepatic artery (living donor) or the entire hepatic artery |
|
|
|
including the celiac trunk (cadaveric donor) |
|
|
■ |
The left branch of the portal vein |
|
|
■ |
The left hepatic duct |
|
|
■ |
The retrohepatic IVC is never left attached to the left graft |
|
|
■ |
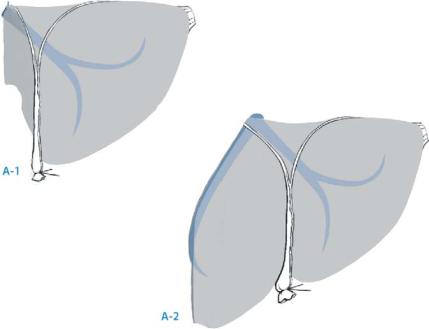
Either segments 2 and 3, drained through the left hepatic vein (left lateral section) |
|
|
■ |
Segments 2, 3 and 4, drained through the left and the median hepatic vein (left |
|
|
|
hemiliver graft) (A-1, A-2) |
|
Auxiliary Liver Transplantation |
521 |
|
|
STEP 2 |
Implantation of left liver grafts |
|
The native IVC is clamped anterolaterally, using the remaining stump of the left hepatic |
|
|
|
vein to expose the vessel. Then, the native IVC is opened vertically on 2cm, beginning at |
|
the ostium of the left hepatic vein. An end-to-side anastomosis is performed using a |
|
continuous 4-0 Prolene suture between the recipient vena cava and the graft left hepatic |
|
vein or common median-left stem. The portal vein is adjusted and implanted with a |
|
growth factor as for the right side. The standard artery reconstruction is an end-to-side |
|
anastomosis between the graft celiac axis and the recipient common hepatic artery or |
|
splenic artery. End-to-end anastomosis between the donor and recipient left hepatic |
|
artery is used in case of a living donor graft. |
|
The standard technique for biliary tract reconstruction is a direct duct-to-duct |
|
anastomosis, with separate PDS 6-0 or 7-0 stitches, and with insertion of a T-drain. |
|
A Roux-en-Y hepaticojejunostomy is performed in case a direct anastomosis cannot |
|
be performed |

522 |
SECTION 3 |
Liver |
|
|
|
|
Tricks of the Senior Surgeon |
|
■Never start the recipient procedure before the split procedure has been shown to be anatomically feasible.
■Two teams need to work simultaneously, headed by two experienced liver surgeons.
■Never start before a biopsy of the recipient liver has been performed. Fibrosis or cirrhosis would lead to perform orthotopic rather than auxiliary liver transplantation.

SECTION 4
Biliary Tract and Gallbladder
Yuman Fong

Introduction
Yuman Fong
Diseases of the biliary tract represent some of the most challenging problems for the surgeon. Gallstone disease is a common ailment, for which surgical treatment has been recorded since ancient times. In the following chapters, authorities in the field will describe the often performed procedures of cholecystectomy and common bile duct exploration. Versions of these procedures performed as open surgery will
be presented as well as the laparoscopic versions, which are arguably one of the major advances in general surgery in the past two decades. Surgery to fix the most feared complication from treatment of gallstone disease, namely bile duct injury, will also be presented.
We will then proceed to discussions of treatments for diseases that are much rarer: congenital malformations of the biliary tree and malignancies of the proximal/mid bile duct and gallbladder. Resections of these conditions are extremely challenging from a technical perspective. The principles, operative conduct, and “tricks of the senior surgeon” are presented by accepted masters of this trade. Distal bile duct problems will be presented in the chapters on pancreatic resection.
Finally, palliative bypasses for obstructions of the biliary tree will be presented. These chapters will describe the general approach to performing a facile biliary-enteric anastamosis, as well as methods of specific bypass procedures such as a choledochoduodenostomy or a hepaticojejunostomy. Even though biliary stent placement by endoscopic or percutaneous routes is widely used for patients who have clearly unresectable malignancies, for patients with benign disease or with disease found unresectable at surgery, such bypasses offer durable palliation with little added morbidity over the surgical exploration.

Laparoscopic Cholecystectomy, Open Cholecystectomy
and Cholecystostomy
George A. Fielding
Laparoscopic Cholecystectomy
Mouret performed the first laparoscopic cholecystectomy in Lyon in 1988, and the first written report was by Dubois in 1989. Reddick popularized the procedure in the United States in 1990.
Indications and Contraindications
Indications |
■ |
Same as for open procedure |
|
■ |
One of the most important indications is that the surgeon be adequately trained |
|
|
to perform the procedure |
|
■ |
All manifestations of symptomatic gallstones – biliary colic, history of jaundice, |
|
|
chronic cholecystitis and acute cholecystitis |
|
■ |
Gallstone pancreatitis |
|
■ |
Acalculous cholecystitis |
|
■ |
Large gallbladder polyps |
|
|
There are no absolute contraindications to laparoscopic cholecystectomy |
Contraindications |
■ |
|
|
■ |
Relative contraindications include cirrhosis and portal hypertension, bleeding |
|
|
diathesis, pregnancy |
|
■ |
Technical modifications can be made to suit these three problems |
Preoperative Investigation and Preparation for the Procedure
Preoperative investigations include liver function tests and typically an ultrasound examination. If the laparoscopic cholecystectomy is being performed for acalculous cholecystitis, patients may have had nuclear studies to assess gallbladder function.
If there is the suspicion of gallbladder cancer or big polyps, a CT scan is required. There is no place for routine preoperative endoscopic retrograde cholangio-
pancreatography (ERCP) in laparoscopic cholecystectomy.
The patient should have prophylactic antibiotics on induction and appropriate anti-thromboembolic measures.
528 |
SECTION 4 |
Biliary Tract and Gallbladder |
|
|
|
|
Procedure |
|
|
|
|
STEP 1 |
Access |
|
|
The procedure should be performed on a table allowing operative cholangiography. |
|
|
||
|
There is no routine need for a nasogastric tube or Foley catheter. |
|
Typically there is no requirement for invasive anesthetic monitoring.
Patients are placed supine, legs together with a slight reverse Trendelenburg position. There is little to gain by using a steep reverse Trendelenburg position.
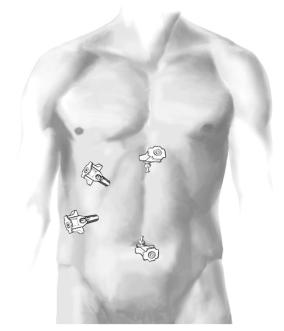
Safe access:
Open insertion of a Hasson cannula through a transumbilical incision. Eversion of the umbilicus creates access via the gap in the linea alba at the base of the umbilicus.
The Hasson cannula can be sat directly in the peritoneal cavity. There is no need for stay sutures nor to suture the port in place. A 30° telescope is used; insufflation pressures are set at 15mmHg. Placement of other access parts is as shown in the figure.
