
clavien_atlas_of_upper_gastrointestinal_and_hepato-pancreato-biliary_surgery2007-10-01_3540200045_springer
.pdf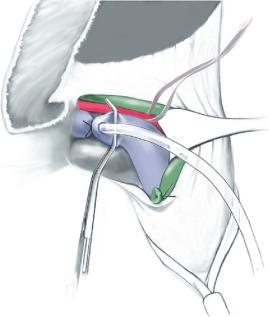
Right Living Donor Hemihepatectomy |
497 |
|
|
|
|
STEP 5 |
Right graft explantation |
|
|
|
When the parenchymal transection is complete, the right graft is separated and only |
|
|
|
|
|
remains attached to the donor by the right hepatic artery, right portal vein, right hepatic |
|
|
vein and possibly accessory veins to the cava. The right hepatic duct is usually divided |
|
|
either just prior to or at the end of the parenchymal division. |
|
|
There are two methods of right liver graft removal: either an “in situ” perfusion with |
|
|
cold preservation solution, or graft removal after placement of vascular clamps and |
|
|
“ex situ” back-table perfusion. In some centers an intravenous bolus of heparin is |
|
|
administered to the donor 5min prior to graft explantation. |
|
|
Ex situ perfusion technique: the right hepatic artery is proximally tied and divided. |
|
|
A vascular clamp is placed on the right portal and hepatic veins, which are also divided |
|
|
respectively. The graft is removed and flushed on the back-table with a cold preservation |
|
|
solution. As for a cadaveric liver transplantation, the bile duct needs to be flushed |
|
|
separately. |
|
|
In situ perfusion technique: cannulation of the right portal is started by placing a |
|
|
vascular clamp closed to the portal vein bifurcation without obstructing the left portal |
|
|
vein. A catheter is introduced into the right portal vein and is fixed with a 2-0 silk liga- |
|
|
ture just distal to the clamp. The right hepatic vein is divided followed by the right |
|
|
hepatic artery while the perfusion of the right hemiliver through the catheter is started. |
|
|
The right graft is then removed and subsequently further perfused with cold preserva- |
|
|
tion solution on the back-table. |

498 |
SECTION 3 |
Liver |
|
|
|
STEP 6 |
Closure of donor vessels and hepatic duct |
|
|
Both the right portal vein and right hepatic vein should be cut at the time of graft |
|
|
|
|
|
explantation with an adequate cuff on the remaining donor vessel. This is especially |
|
|
important in the case of the portal vein, where iatrogenic stricture and twisting should |
|
|
be avoided at all costs. In the case of a portal vein trifurcation, the right anterior and |
|
|
right posterior portal vein branches should be divided separately without attempting to |
|
|
obtain a common cuff to avoid causing a stricture of the remaining donor portal vein. |
|
|
The hepatic vein stump is closed with a continuous 4-0 Prolene suture, and the portal |
|
|
vein stump is oversewn with a continuous 5-0 or 6-0 Prolene suture. |
|
|
The transected border of the left liver is again checked for hemostasis. Potential bile |
|
|
leaks may be identified by placing a wet gauze sponge on the cut surface for 5–10min. |
|
|
Any areas of bile leakage are oversewn with a 5-0 PDS suture and re-checked. The |
|
|
remnant liver is fixed by suturing the attached falciform ligament to the diaphragm. |
|
|
This prevents potential rotation of the left liver and an iatrogenic Budd-Chiari syndrome |
|
|
in the postoperative period. The abdomen is closed without placement of a drain. |
|
Complications
These are the same as for right hemihepatectomy, the most common being:
■ |
Biliary fistula |
■ |
Sustained hepatic dysfunction |
■ |
Biliary strictures |
Tricks of the Senior Surgeon
■In performing the hilar dissection, start on the right lateral aspect when identifying the right portal vein and hepatic artery. This avoids excessive dissection and skeletonization of the right hepatic duct and bile duct.
■Identification of the biliary anatomy by intraoperative cholangiography should be performed early in the operation. A radiopaque metal clip or small bulldog should be used to mark the area of the right hepatic duct during the cholangiogram. An atraumatic bulldog can be placed on the distal bile duct to avoid passage of contrast into the lower bile duct.
■Marking the pathway of the middle hepatic vein by intraoperative ultrasound helps decide the parenchymal transection line, which should be 1cm to the right of the middle hepatic vein.
■Central venous pressure should be maintained low by anesthesia as it helps to reduce blood loss.
■The hanging maneuver makes the parenchymal dissection easier, particularly in the last part.
|
Living Donor Transplantation: |
|
Left Hemiliver Donor Procedure and Implantation |
|
Koichi Tanaka, Hiroto Egawa |
|
For laparoscopic left hemiliver donor procedure see chapter by D. Cherqui. |
|
Open Donor Procedure for Left Living Donor Liver Grafts |
|
|
STEP 1 |
Access and mobilization |
|
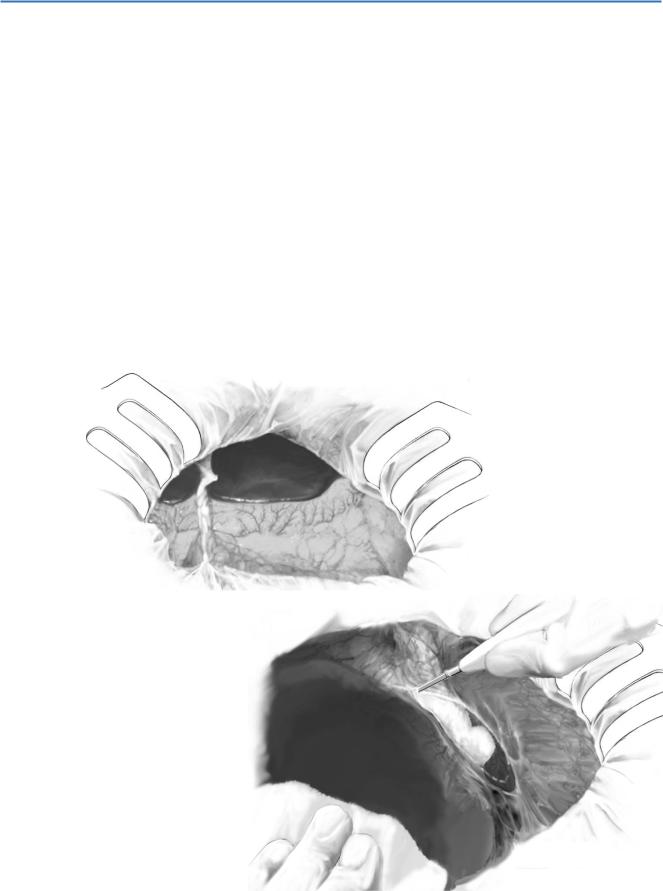
Access is gained through a bilateral subcostal incision with cranial extension. The falci- |
|
|
|
form ligament is divided leaving enough length on the liver side as it needs to be fixed |
|
in the recipient. Finally a retractor (e.g., Takasago retractor) is installed (A). |
|
The lateral segment is lifted up and a towel is placed in front of the spleen for its |
|
protection. A sponge is placed behind the left triangular ligament and the lateral |
|
segment is placed back. The left liver is pulled downward and the left coronary |
|
ligament and the left triangular ligament are divided by a cautery knife (B). |
A
B

500 |
SECTION 3 |
Liver |
|
|
|
STEP 2 |
Approach to the left hepatic vein and the left side of the cava |
|
|
|
|
The lateral segment is rotated to the right, and the ligamentum venosum is encircled, ligated and divided near the inferior vena cava (A). The connective tissue is detached from the superior aspect of the Spigelius lobe to expose the left side of the inferior vena cava as well as the posterior surface of the left hepatic vein (B).

Living Related Liver Transplantation: Left Hemiliver Donor Procedure and Implantation |
501 |
|
|
|
|
STEP 3 |
Dissection of the hepatoduodenal ligament |
|
|
|
|
The serous membrane on the ventral aspect of the hepatoduodenal ligament is detached at the level of the cystic duct and the hepatic arteries are identified. The left and middle hepatic arteries are dissected out at the hepatic hilum up to the bifurcation of the right and left hepatic artery (A). The middle hepatic artery can be cut off when it is clearly smaller than the left hepatic artery.
When the anterior aspect of the hepatoduodenal ligament is separated, the common bile duct can be identified. After the left hepatic duct is identified a small vascular clip is placed to the predetermined cut line on the bile duct. A 24-G puncture needle with
a trocar is inserted into the common bile duct and cholangiography is obtained (B). In some cases, the left hepatic duct may be located inside the hepatic parenchyma
and it is difficult to be identified. In such cases, it can be identified during the dissection of the parenchyma.
The cholangiography provides information of the biliary anatomy and allows to determine the dissection line of the left hepatic duct (C). After the cholangiography, the catheter is removed and the puncture site is closed by a 6-0 Prolene stitch. The left hepatic duct can now be encircled at the point of predetermined cut line (D).
502 |
SECTION 3 |
Liver |
|
|
|
STEP 4 |
Parenchymal dissection |
|
|
For a Left Lateral Segment Graft (Sg2 and 3) |
|
|
|
|
|
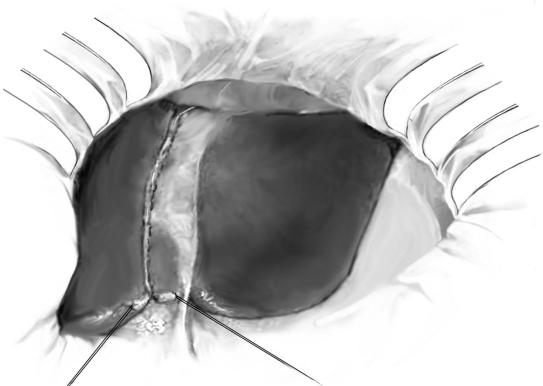
A cutting line is marked on the surface with a cautery knife approximately 1cm to |
|
|
the right of the falciform ligament (A). Without any vascular obstruction during |
|
|
parenchymal dissection, the liver surface is incised with a cautery knife and the |
|
|
parenchyma is dissected with a Cavitron Ultrasonic Surgical Aspirator (CUSA) |
|
|
in combination with a bipolar cautery with irrigation system for hemostasis. |
|
|
Small vessels are dissected with the cautery knife while thicker vessels |
|
|
(i.e., diameter >3mm) are ligated or clipped. Large vessels are clamped, dissected |
|
|
and suture-ligated by 5-0 or 6-0 Prolene stitches. |
|
A

Living Related Liver Transplantation: Left Hemiliver Donor Procedure and Implantation |
503 |
|
|
|
|
STEP 4 (continued) |
Parenchymal dissection |
|
|
For a Left Lateral Segment Graft (Sg2 and 3) |
|
|
|
|
|
The left hepatic duct can be found where the parenchymal dissection line meets the |
|
hepatic hilus region (right side of the left portal branch) (B). The left hepatic duct is cut at the previously determined site. The hilar plate and the stiff fibrous tissue are dissected with a cautery knife. The left hepatic duct is closed with 6-0 Prolene suture on the donor side.
In the left lateral segment graft, reconstruction of the Sg4 hepatic duct is not necessary and it can be closed after confirming the direction. The Sg4 duct can be closed on the donor side too.
It is crucial to free the left portal vein branch completely through ligation and isolation of the caudate branches. They extend from the horizontal part of the origin of the branch.
For the parenchymal dissection, curved DeBakey forceps are used as a guide. The tip of the forceps is inserted between the caudate lobe and the lateral segment
from the head direction of the portal vein. The forceps are lifted and fixed. The cutting line of the parenchyma is made between the marked incision of the surface and the tip of the forceps (C).
B
C
504 |
SECTION 3 |
Liver |
|
|
|
STEP 4 (continued) |
Parenchymal dissection |
|
|
For a Full Left Hemiliver Graft without caudate lobe (Sg2–4) |
|
|
|
|
|
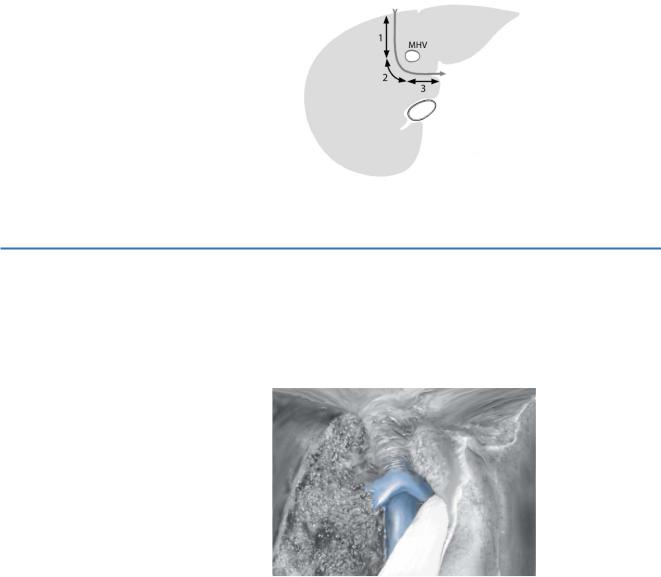
The cutting line for left hemiliver graft is marked on the surface with electrocautery |
|
starting from the right side of the middle hepatic vein to the liver bed of the gallbladder. The location of the middle hepatic vein is confirmed with ultrasonography before parenchymal dissection. The cutting line on the posterior side starts from the liver bed and reaches to the right side of the predetermined cutting point of the left hepatic duct.
The parenchymal dissection follows the sagittal plane from the top surface until the level of the middle hepatic vein (line 1). When the entire middle hepatic vein is included in the graft side, the direction of the dissection is changed in an oblique plane (line 2). To prevent injury of the middle hepatic vein and its small venous branches, some parenchymal tissue should be left on the middle hepatic vein. After dissection of the left hepatic duct, the direction is changed toward the space between the lateral segment and the caudate lobe (line 3). The curved DeBarkey forceps are useful as a guide as in left lateral segmentectomy.
STEP 5 |
Preparation of the hepatic veins |
|
The tissue around the hepatic veins is separated and the confluence of the left hepatic |
|
|
|
vein and the middle hepatic vein is exposed using the CUSA. Small branches around |
|
the confluence should be stitched with 6-0 Prolene suture and divided. Do not use |
|
hemostatic clips as they might interfere with the vascular clamp. |
Living Related Liver Transplantation: Left Hemiliver Donor Procedure and Implantation |
505 |
|
|
|
|
STEP 6 |
Perfusion and removal of the graft |
|
|
|
|
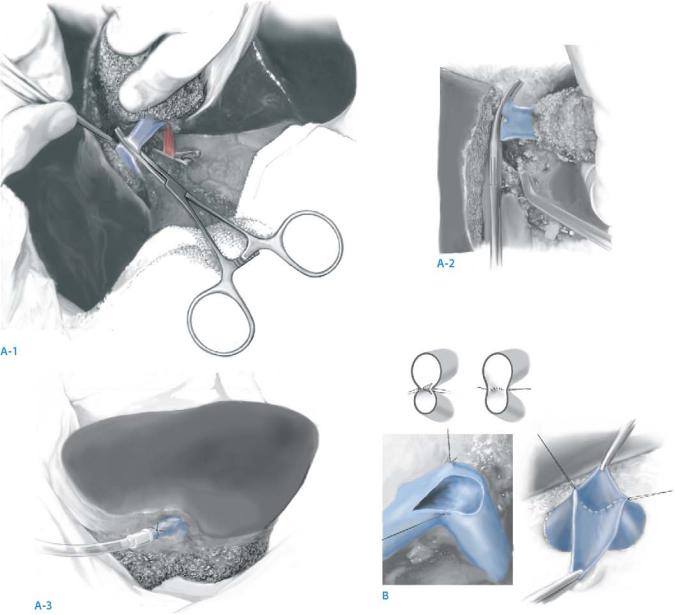
After accomplishing the parenchymal dissection, the donor is systemically administered 1,000units of heparin. The left hepatic artery is clamped with two clips and divided. The anterior wall of the left portal vein is opened and the tip of the catheter for perfusion is inserted into the lumen. Subsequently the left portal vein is divided (A-1). The left hepatic veins is clamped with a spoon clamp and divided. Immediately after dividing the left hepatic vein (A-2), the graft is perfused with preservation solution [histidine-tryptophan-ketoglutarate (HTK) or University of Wisconsin [UW] solution] (A-3). The artery is not rinsed. The hepatic duct is washed with the solution.
The donor hepatic vein is closed with 5-0 Prolene, the donor portal vein with 6-0 Prolene and the donor hepatic artery is closed with 6-0 Prolene suture or 3-0 silk double ligation.
If the left hepatic vein has a septum close to the orifice, it is cut sharply with scissors and sutured to make a single orifice with enough length of the cuff (B).
506 |
SECTION 3 |
Liver |
|
|
|
|
Implantation Procedure for Left Living Donor Liver Grafts |
|
|
|
|
STEP 1 |
Access and hilar dissection |
|
|
A bilateral subcostal incision with an upper midline extension to the xiphoid is the |
|
|
|
|
|
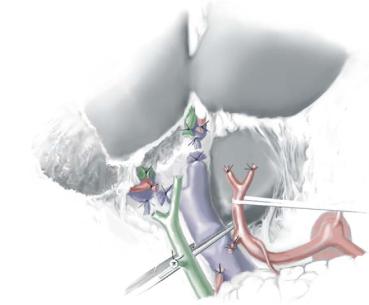
preferred access. The most important point to consider during the hilar dissection in |
|
|
living donor liver transplantation is to leave the pedicle of the vessels and bile duct with |
|
|
the greatest possible length, because they are much shorter than those in a cadaveric |
|
|
liver graft. The hepatic arteries are dissected carefully and transected close to the liver |
|
to provide adequate length and enough options for arterial reconstruction. In children suffering from biliary atresia the hepatic artery frequently has a larger size than expected. In this particular situation, dissection of the hepatic artery inside the liver
of the recipient is required to adjust the size of hepatic artery between the graft and the recipient. Double ties on the proximal side of the hepatic arteries are recommended to prevent injury to the intima. The first ligation is done loosely just to occlude the lumen with 4-0 silk. The second tie is placed tightly just distal to the first.
The portal pedicle is elongated by dissecting the tissue around the portal vein up to the confluence of the superior mesenteric and splenic vein. Removal of the lymph nodes around the portal vein is helpful as it provides the desired smooth curve of the portal vein. The portal flow should be confirmed by unclamping the portal vein. The left gastric vein is divided routinely to increase portal flow.
