
clavien_atlas_of_upper_gastrointestinal_and_hepato-pancreato-biliary_surgery2007-10-01_3540200045_springer
.pdf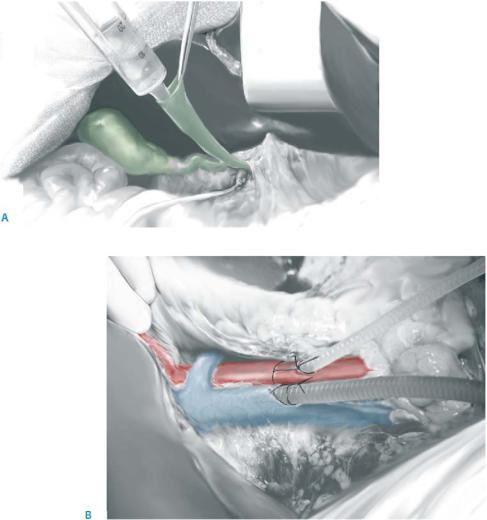
Technique of Multi-Organ Procurement (Liver, Pancreas, and Intestine) |
457 |
|
|
|
|
STEP 4 |
Preparation and perfusion of the abdominal organs |
|
|
|
|
The gallbladder fundus is opened with the electric cautery and gallbladder and bile ducts are flushed out with saline. Manual compression of the distal bile duct allows a better proximal duct cleansing, which should be completed through a small catheter once the bile duct is transected (A).
When the thoracic team is ready for procurement, heparin is given (500units/kg body weight) and the aortic canula is inserted right above the aortic bifurcation. If the thoracic team prefers to clamp the suprahepatic IVC during the procurement, the IVC can be canulated at the same level as the aorta in order to obtain better decompression and clean exsanguination. For both the aorta and the IVC, chest drains can be used (B).
The portal vein does not need to be perfused in situ, but only during the back-table preparation.
The supraceliac aorta is clamped or ligated at the beginning of aortic perfusion with the preservation solution (e.g., 60ml of UW solution/kg body weight) and the intravascular cooling of the abdominal organs is completed by abundant topical irrigation using cold saline.
The bile duct is transected just above the duodenal arch and needs to be rinsed once more with saline through a small catheter.
458 |
SECTION 3 |
Liver |
|
|
|
STEP 5 |
Preparation and procurement of the arterial axis |
|
|
|
|
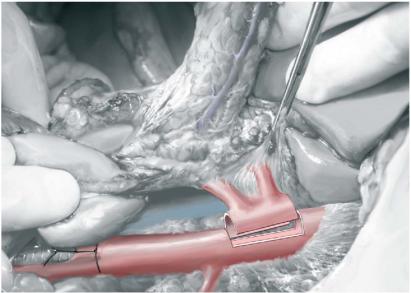
Once the abdominal organs are discolored and the thoracic procurement is completed, the en-bloc liver-pancreas procurement can start. The dissection of the superior mesenteric artery trunk is completed at the anterior side of the abdominal aorta. Retroperitoneal tissue and solar plexus located between IVC and aorta are transected from the left renal vein towards Winslow’s foramen in order to fully expose the right side of the aorta and the superior mesenteric artery. Next, the anterior side of the aorta is incised just distally to the origin of the superior mesenteric artery. After visualization of the orifices of the renal arteries, an arterial aortic Carrel patch encompassing the origin of both superior mesenteric artery and celiac trunk is created. The simultaneous excision of the vascular roots of the tissue bloc is an important step of the en-bloc liver-pancreas procurement.
Afterwards, colon and intestine are repositioned in the abdomen. All branches of the left gastric artery are transected closed to the stomach, allowing the preservation of a possible left hepatic artery (LHA) originating from the left gastric artery.
Technique of Multi-Organ Procurement (Liver, Pancreas, and Intestine) |
459 |
|
|
|
|
STEP 6 |
Preparation of the duodenum and the pancreas |
|
|
|
|
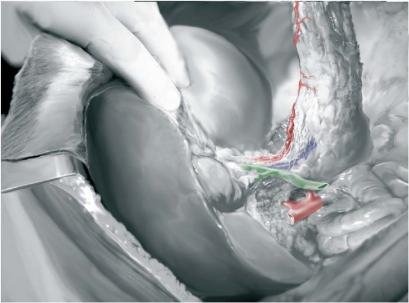
After instillation of a betadine solution through a gastric tube, the duodenum and the jejunum are stapled distal to the pylorus and the ligament of Treitz, respectively.
The mesenteric root is transected distally of the pancreas using the GIA stapling device. The splenocolic ligament is taken down and the spleen and the pancreas are freed retroperitoneally. Finally, the IVC is transected at the level of the right adrenal gland, the liver is mobilized by transection of the falciform ligament and the liver-pancreas bloc is removed containing a large diaphragmatic patch.
The ex-vivo separation of liver and pancreas is done on the back-table after identification of the vascular anatomy (see back-table work).
460 |
SECTION 3 |
Liver |
|
|
|
|
Modifications of the En-Bloc Liver Pancreas Procurement |
|
Pancreas Removal for Islet Transplantation
For islet procurement, the pancreas is removed together with the liver and the duodenum is simply removed from the pancreatic head.
Procurement of Intestine for Transplantation
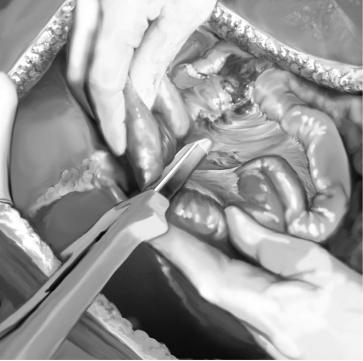
After initial preparation of the superior mesenteric artery and the celiac trunk, the intestine is repositioned adequately in the abdominal cavity. The first jejunal loop is transected about 10cm distal to the ligament of Treitz using a GIA stapler . The transected jejunal loop is pulled up by the assistant in order to better individualize the mesenteric root. A second assistant maintains the intestine in place to avoid traction on the superior and inferior mesenteric veins, as malpositioning causes reduced splanchnic perfusion.
Several small branches of the jejunal mesentery are transected close to the serosa (as is usually done in a duodenopancreatectomy). The proximal part of the mesenteric vessels are freed for about 2cm, so the small pancreatic veins joining the right part of the SMV are ligated, as well as those branches of the SMV draining the pancreatic isthmus. Once the SMV is freed, the abdominal organ perfusion can be started.
As soon as the perfusion is completed, the liver-pancreas-small bowel bloc can be retrieved. In case of an isolated intestinal transplant it can be necessary to extend the superior mesenteric vein and artery using free iliac venous and arterial grafts.
Technique of Multi-Organ Procurement (Liver, Pancreas, and Intestine) |
461 |
|
|
Back-table Work
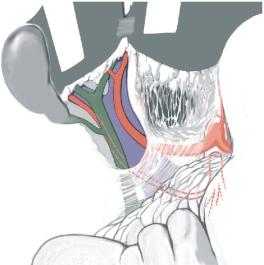
First, the gallbladder and the bile ducts need to be flushed again to avoid mucosal damage by precipitating bile salts. Next, ex-vivo portal flushing is done through a canula introduced in the SMV. The tip of the portal vein catheter is positioned with slight finger compression. The liver-pancreas bloc is positioned as in the abdominal cavity; the aorta patch, containing the celiac trunk and the superior mesenteric artery, is dissected free. Splenic,
celiac, hepatic and left gastric artery should all be individualized; one should look as well for the RHA and the LHA. Bile duct and the portal vein and splenomesenteric venous confluence also need to be dissected. The final repartition of all vascular axes is dictated by their anatomical variability.
A.In the presence of standard arterial anatomy, the celiac trunk should be kept with the whole pancreas transplant. By doing so, a reconstruction with a Y-graft can be avoided as the superior mesenteric artery can be directly connected to the ostium of the common hepatic artery (for illustration see chapter “Orthotopic Liver Transplantation”). The repartition of the venous vessels is usually unproblematic if the recipient portal vein is transected close to the liver parenchyma.
B.If the liver-pancreas bloc contains an LHA originating from the left gastric artery, the celiac trunk should go to the liver graft. In this case, a vascular reconstruction between splenic artery and superior mesenteric artery is necessary using a free iliac arterial graft (see Sect.6, chapter “Pancreas Transplantation”).
C.In the presence of an aberrant RHA with a complete extrapancreatic course, one can decide to divide the superior mesenteric artery between the head of the pancreas and the origin of the aberrant right hepatic artery (see Figure). This allows for three different types of reconstruction (for illustrations see chapter “Orthotopic Liver Transplantation”):
–Anastomosing the stump of the superior mesenteric artery on the ostium of the splenic artery
–Anastomosing the celiac trunk or the common hepatic artery on the proximal ostium of the superior mesenteric artery
–Anastomosing the aberrant right hepatic artery to the gastroduodenal artery

462 SECTION 3 Liver
In the case of an intrapancreatic RHA, division of this artery should only be performed after discussion with the pancreas and liver teams. If this artery is transected proximal to the pancreatic head, it must be possible for the liver surgeon to implant the RHA into the ostium of the gastroduodenal or the splenic artery.
Both recipient teams must finally decide if both organs should be implanted because of technical difficulties.
The only anatomical absolute contraindication to simultaneous whole pancreas and liver transplantation is the presence of an important pancreatico-duodenal artery originating from an aberrant RHA. In this case, vascularization of the pancreatic head can be compromised, as the gastroduodenal artery and thus the superior pancreatico-duodenal artery are kept to retain the common hepatic artery for the liver allograft.
Tricks of the Senior Surgeon
■The correct procurement of iliac, superior mesenteric, carotid and jugular vessels is crucial as complex vascular reconstructions might be required during the implantation. Therefore, the whole iliac axis down to the inguinal ligament must be taken.
■The bile duct should be routinely rinsed by means of a small feeding tube through the cut end, as remaining bile salts precipitate and may damage the biliary epithelium. Flushing the biliary tree through the gallbladder cleans only the distal bile duct and thus is not enough!
■Correct back-table bath temperature must be guaranteed. Warming up of the solution and direct contact with the ice can both be harmful and can easily be avoided by separating the allograft from the crushed ice through a cold saline buffer.

Orthotopic Liver Transplantation
Robert J. Porte, Jan Lerut
Since its introduction into clinical practice in 1963 by Starzl et al., the technique of orthotopic liver transplantation has been refined progressively. The original technique included resection of the recipient inferior vena cava (IVC) and the use of extracorporeal venovenous bypass. More confidence with the technique and the more frequent use of technical variants in pediatric liver transplantation have led to the development of recipient cava-preserving hepatectomy techniques without use of venovenous bypass and with or without use of a temporary portocaval shunt, independently of anatomical and general status of the recipient. Regardless of the exact technique, orthotopic liver transplantation is characterized by three stages: the pre-anhepatic, the anhepatic and the post-anhepatic stage. The technique of orthotopic liver transplantation, either with or without preservation of the recipient IVC, will be described following these three stages.
Indications and Contraindications
Indications |
a) Chronic liver failure (cirrhosis) due to: |
|
|
– |
Chronic hepatitis B, B and D (coinfection), and C |
|
– |
Alcoholic liver disease |
|
– |
Autoimmune hepatitis |
|
– |
Cryptogenic cirrhosis |
|
– |
Congenital liver fibrosis |
|
– Primary and secondary biliary cirrhosis |
|
|
– |
Primary sclerosing cholangitis |
|
– |
Biliary atresia |
Metabolic liver diseases:
–Wilson’s disease
–Alpha1-antitrypsin deficiency
–Hemochromatosis
–Protoporphyria
Vascular diseases
–Budd-Chiari syndrome
b)Acute liver failure
–Viral [hepatitis A, B, D (coinfection), E]
–Intoxications (e.g., acetaminophen, Amanita phalloides)
–Acutely decompensated chronic liver disease (e.g., Wilson’s disease)
–Extensive liver trauma
–Budd-Chiari syndrome
c)Metabolic disorders (e.g., tyrosinemia, familial amyloid polyneuropathy, primary hyperoxaluria)
d)Liver tumors
–Hepatocellular carcinoma: single tumors <5cm, or up to three tumors <3cm (Milan criteria, extended criteria center dependent)
–Metastases of neuroendocrine tumors
–Benign (polycystic liver disease, giant hemangioma, Caroli’s disease)
464 |
SECTION 3 |
Liver |
|
|
|
|
|
|
– |
Untreated systemic infections or sepsis |
|
Contraindications |
|
||
|
– |
Extrahepatic malignant disease |
|
|
– |
Irreversible multiorgan failure |
|
Preoperative Investigation and Preparation for the Procedure
History and physical examination:
Laboratory tests: Liver tests, coagulation studies, kidney function, electrolytes, hepatitis and HIV serology
Doppler ultrasound: Check for patency and flow of liver vessels (portal vein, hepatic artery, and hepatic veins)
Check for tumors, vascular collaterals, aneurysms of the splenic artery or splanchnic thrombosis
May be indicated in primary sclerosing cholangitis
In case of portal vein thrombosis, planned retransplantation, and in case of hepatocellular carcinoma for TACE (trans-arterial chemo-embolization)
According to the Child-Pugh criteria (bilirubin, albumin, prothrombin time/INR, ascites, encephalopathy) and/or according to the Model for End-Stage Liver Disease (MELD) score (serum creatinine, bilirubin, international normalized ratio, INR)
Graft biopsy in case of suspected steatosis

Orthotopic Liver Transplantation |
465 |
|
|
Procedures
|
Orthotopic Liver Transplantation:The Pre-anhepatic Stage |
STEP 1 |
Access, exposure, exploration, and dissection of the hepatoduodenal ligament |
After a bisubcostal incision, the round and falciform ligaments are divided. Care must be taken to avoid injury of large collaterals or a repermeabilized umbilical vein, which may be present in the umbilical ligament due to portal hypertension. A retractor (e.g., Thompson) is installed followed by a careful mobilization of the left and right hemiliver. The left and right triangular and coronary ligaments are divided as for a left and right hemihepatectomy and the hepatogastric ligament is transsected by cautery or after stepwise suture ligation. A possible aberrant or accessory left hepatic artery needs to be identified and ligated. All these steps have to be performed with a particularly careful technique, as portal hypertension and consecutive dilation of the vascular bed leads to more fragile vessels which are prone to bleeding.
Next, the hepatoduodenal ligament needs to be palpated and checked for aberrant arterial anatomy, i.e., an aberrant or accessory right hepatic artery from the superior mesenteric artery, running behind the common bile duct. The peritoneum is opened on the ventral aspect of the ligament and the proper hepatic artery is identified.
A.Dissect the proper hepatic artery towards the liver. Ligate and divide the left and right hepatic artery distal from the bifurcation (A-1).
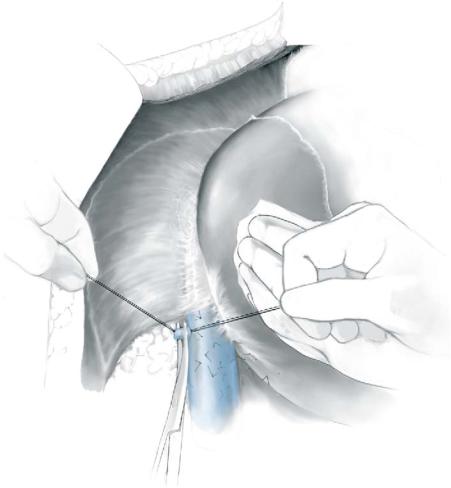
B.Encircle the common bile duct as high as possible (usually at the level of the cystic duct or above) in the porta hepatis, preserving an adequate amount of tissue surrounding it to avoid devascularization. Again, check for a possible aberrant right hepatic artery. Divide the common bile duct and ligate and divide the aberrant right hepatic artery, if present (A-2).
C.Dissect the portal vein completely free from its surroundings along the length of the hepatoduodenal ligament.
466 |
SECTION 3 |
Liver |
|
|
|
STEP 2 |
Mobilization of the infrahepatic inferior vena cava |
|
|
At this stage of the operation, the planes of dissection are different for the classical |
|
|
|
(with resection of the IVC) and the cava-sparing (or piggyback) technique. The latter technique is more demanding but has the advantage of avoiding interruption of the caval venous return and of a shorter warm ischemia time during implantation, because only one instead of two IVC anastomoses have to be performed.
The two techniques will be described separately.
The Classical Technique with Resection of the IVC
The liver is turned to the left and the infrahepatic inferior vena cava is exposed. The right adrenal vein is identified and ligated between ties. The inferior vena cava is mobilized circumferentially by opening the peritoneal reflection along the right side of the cava with cautery. Care must be taken not to injure the right hepatic vein. The same technique is applied on the left side of the cava.
